Mental Health Professionals and Patients Often Disagree on Causes of Symptoms
A new study finds that clinicians’ disregard for mental health patients’ insight into their own condition may be detrimental to treatment.
Dissecting the DSM Debate: Researchers Analyze Critiques Across Audiences
A new study systematically explores critical reactions to the DSM-5 and identifies unifying themes.
Decontextualized Depression and PTSD Diagnoses Fail Indigenous Communities
A case analysis of an American Indian woman illustrates how the DSM diagnostic criteria misrepresent the lives of indigenous people.
Study Reveals Inconsistency in ADHD Diagnostic Determinations
Researchers compare differences between research and clinical diagnoses of ADHD and explore the consistency of clinical determinations over time
The Power Threat Meaning Framework One Year On
The team that developed the Power Threat Meaning framework as a diagnostic alternative reflects on the response to the framework after one year.
The Role of Racial Bias in the Overdiagnosis of Schizophrenia
Researchers detect disparity between white and African American patients diagnosed with schizophrenia when symptoms of a mood disorder are present.
Constructing Alternatives to the DSM: An Interview with Dr. Jonathan Raskin
Dr. Raskin discusses psychotherapists’ dissatisfaction with current psychiatric diagnostic systems and explores alternatives.
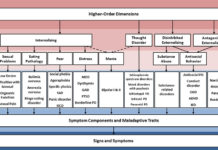
International Research Team Proposes a New Taxonomy of Mental Disorders
New data interpreted to suggest a hierarchical, dimensional system of mental disorders will aid future research efforts and improve mental health care.
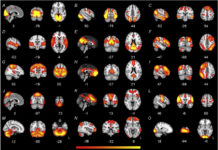
No Brain Connectivity Differences Between Autism, ADHD, and “Typical Development”
Neuroscience researchers find no differences in brain connectivity between children with diagnoses of autism, ADHD, and those with no diagnoses.
Mental Health Concerns Not “Brain Disorders,” Say Researchers
The latest issue of the journal Behavioral and Brain Sciences features several prominent researchers arguing that mental health concerns are not “brain disorders.”
Stigmatizing Effects of the Psychosis-Risk Label
Study examines the effects on participants of being told they are at risk of developing psychosis.
Developing Alternatives to the DSM for Psychotherapists
A new article suggests counselors and psychotherapists are dissatisfied with current diagnostic systems and outlines some potential alternatives.
Philosophers Challenge Psychiatry and its Search for Mechanisms of Disorder
Attempting to locate the mechanisms of psychiatric disorder is a step in the wrong direction and fails to challenge potentially unjust social practices.
How Stigma and Social Factors Drive the Negative Health Outcomes Associated with Autism
A new study explores the interplay between social stress and quality of life for individuals self-identified with high-functioning autism.
International Study Documents Widespread Distress in College Students
An international study of college students reveals ubiquitous social and emotional challenges faced by young adults.
Minimal Evidence for Disruptive Mood Dysregulation Disorder in Childhood
Researchers offer a critical take on the inclusion of the Disruptive Mood Dysregulation Disorder in the DSM-V.
Challenging Resilience as a Buzzword: Toward a Contextualized Resilience Model
Researcher Dr. Silke Schwarz highlights how Western psychology’s construction of individual resilience deflects emphasized individual pathology and deflects efforts at structural change.
The Effect of Psychiatric Diagnosis on Young People’s Sense of Self and Social Identity
A new review highlights the effects that psychiatric diagnosis has on children and adolescents’ social relationships and views of self.
Questioning the Philosophical Assumptions of Neuroscience Research
Are philosophical misunderstandings behind the failure of neuroscience to provide useful clinical research?
Can Precision Medicine Work for Depression?
From STAT: The idea of using precision medicine to treat depression is quickly gaining new ground. But many researchers and experts worry that the idea...
Treatment-Resistant Depression as a Sign of Unconscious Health
In this video, Dr. Elio Frattaroli describes how biological explanations for "treatment-resistant depression" often ignore the meaning and context of a patient's suffering. He...
The Sound of Madness
From Harper's Magazine: People who hear positive, encouraging voices often seen as spiritual guides or messages and people diagnosed with schizophrenia are usually thought of as...
Differing Depression Diagnostic Tools May Influence Research Findings
The type of diagnostic assessment used in research settings, either fully structured or semi-structured interview, may affect which participants in receive a diagnosis of major depression.
Hopeless But Not Broken: From George Carlin to Protest Music
From CounterPunch: Although people are often pathologized and shamed for feeling hopeless, hopelessness is sometimes a natural reaction to an oppressive political climate. George Carlin...
Psychiatric Diagnosis Can Lead to Epistemic Injustice, Researchers Claim
A discussion of the role of epistemic injustice in the experiences of patients diagnosed with psychiatric disorders.