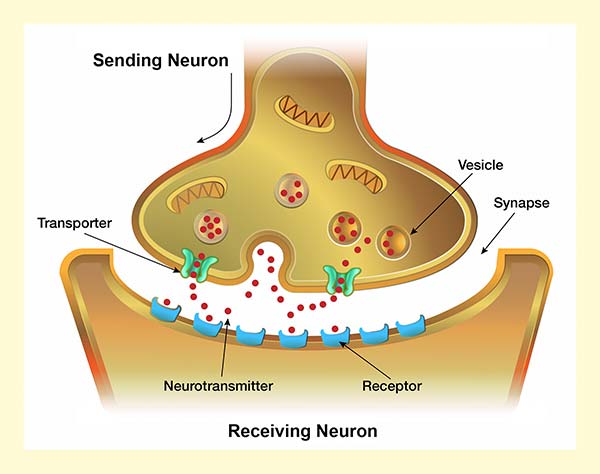
To assess the merits of psychiatric drugs, it is helpful to understand how they “act” on the brain, and how the brain responds to the presence of the drug.
How brain neurons communicate
There are an estimated 100 billion neurons in the brain. Messages are passed along neuronal pathways in the brain via molecules, known as neurotransmitters, that act as “chemical messengers.”
The first (sending) neuron releases a neurotransmitter into the tiny gap between neurons, known as the synaptic cleft, and the neurotransmitter then binds with receptors on the second neuron. The neurotransmitter is said to fit into the receptor like a “key into a lock.”
This binding action either causes the second (receiving) neuron to fire or inhibits its firing. An excitatory response passes the message along the neuronal pathway; an inhibitory response dampens this neuronal activity. To end the message, the chemical messenger is then “transported” back into the first neuron and stored for later re-use.