The long-term outcomes literature for antipsychotics, which has been compiled over a period of nearly 50 years, consistently tells of drugs that increase the likelihood that a person diagnosed with schizophrenia will become chronically ill.
A. The Chronicity Problem Becomes Apparent (1960s-1970s)
It seems paradoxical that drugs that ameliorate acute psychotic symptoms over the short term will increase the likelihood that a person so treated will fare poorly over the long term. But that disturbing fact showed up in the very first outcome studies, and has continued to show up ever since.
1.NIMH’s first follow-up study
a) One Year After Discharge. Schooler, N. American Journal of Psychiatry123 (1967): 986-995.
This NIMH study looked at one-year outcomes for 299 patients who had been treated either with neuroleptics or placebo upon their admission to a hospital. This was the first long-term study conducted by the NIMH, and the researchers found that patients who received placebo “were less likely to be rehospitalized than those who received any of the three active phenothiazines.”
2. NIMH”s first two relapse studies
a) Relapse in Chronic Schizophrenics Following Abrupt Withdrawal of Tranquilizing Medication. Prien, R. British Journal of Psychiatry115 (1968): 679-86.
The critical finding of this NIMH study was that relapse rates rose in direct relation to dosage–the higher the dosage that patients were on before the antipsychotic was withdrawn, the greater the relapse rate. At the start of the study, 18 patients were on placebo, and only one got worse over the next six months (6%). Sixty-five patients were on 300 mg. of chlorpromazine at the start of the study, and 54% of those patients worsened after the drug was withdrawn. One hundred thirteen patients were on more than 300 mg. of chlorpromazine at the start of the study, and 66% of those patients got worse after drug withdrawal. (See table 3, page 684.)
b) Discontinuation of Chemotherapy for Chronic Schizophrenics. Prien, R. Hospital and Community Psychiatry 22 (1971): 20-23.
In this NIMH study, the earlier finding that relapse rates rose in correlation with neuroleptic dosage was confirmed. Only 2 of 30 patients who were on placebo at the start of the study relapsed during the next 24 weeks (7%). Twenty-three percent of the 99 patients who were on less than 300 mg. of chlorpromazine at the start of the study relapsed following drug withdrawal. Fifty-two percent of the 91 patients who were on 300 to 500 mg. of chlorpromazine at the start of the study relapsed following drug withdrawal, and sixty-five percent of the 81 patients who were on more than 500 mg. of chlorpromazine at the start of the study relapsed following drug withdrawal. The researchers concluded: “Relapse was found to be significantly related to the dose of the tranquilizing medication the patient was receiving before he was put on placebo–the higher the dose, the greater the probability of relapse.” (See page 22, 23.)
3. A study comparing five-year outcomes in the pre-Thorazine and post-Thorazine eras
a) Comparison of Two Five-Year Follow-up Studies. Bockoven, J. American Journal of Psychiatry132 (1975): 796-801.
In this study, Boston psychiatrists Sanbourne Bockoven and Harry Solomon compared relapse rates in the pre-drug era to those in the drug era, and found that patients in the pre-drug era had done better. Forty-five percent of the patients treated at Boston Psychopathic Hospital in 1947 had not relapsed in the five years following discharge, and 76% were successfully living in the community at the end of that follow-up period. In contrast, only 31% of patients treated in 1967 with drugs at a Boston community health center remained relapse-free for the next five years, and as a group they were much more “socially dependent”–on welfare, etc.–than those in the 1947 cohort.
Other researchers who reviewed relapse rates for New York psychiatric hospitals in the 1940s and early 1950s reported similar findings: roughly 50% of discharged schizophrenia patients had remained continuously well through lengthy follow-up periods, which was markedly superior to outcomes with neuroleptics. See Nathaniel Lehrman, “A state hospital population five years after admission: a yardstick for evaluative comparison of follow-up studies,” Psychiatric Quarterly, 34 (1960), 658-681; and H.L. Rachlin, “Follow-up study of 317 patients discharged from Hillside Hospital in 1950,” Journal of Hillside Hospital5 (1956), 17-40.
4. Two NIMH studies in the 1970s investigating longer-term outcomes in non-medicated patients
a) The Treatment of Acute Schizophrenia Without Drugs. Carpenter, W. American Journal of Psychiatry 134 (1977): 14-20.
In this 1977 NIMH study, 49 schizophrenia patients, placed into an experimental hospital program that provided them with psychosocial support were randomized into drug and non-drug cohorts. Only 35% of the non-medicated patients relapsed within a year after discharge, compared to 45% of those treated with medication. The medicated patients also suffered more from depression, blunted emotions, and retarded movements.
b. Are There Schizophrenics for Whom Drugs May be Unnecessary or Contraindicated? Rappaport, M. International Pharmacopsychiatry 13 (1978):100-111.
In this 1978 study, Maurice Rappaport and his colleagues at the University of California, San Francisco randomized 80 young male schizophrenics admitted to Agnews State Hospital to drug and non-drug groups. Only 27% of the drug-free patients relapsed in the three years following discharge, compared to 62% of the medicated group. Most notably, only two of 24 patients (8 percent) who weren’t medicated in the hospital and continued to forgo such treatment after discharge subsequently relapsed. At the end of the study, this group of 24 drug-free patients was functioning at a dramatically higher level than drug-treated patients.
5. The Soteria project.
During the 1970s, the head of schizophrenia studies at the NIMH, Loren Mosher, conducted an experiment that compared treatment in a homelike environment (called Soteria), where antipsychotics were minimally used, to conventional treatment in a hospital setting. At the end of two years, the Soteria patients had “lower psychopathology scores, fewer (hospital) readmissions, and better global adjustment” than those treated conventionally with antipsychotics. Only 31% of the patients treated without drugs in in the Soteria House who remained off neuroleptics after leaving the program relapsed over the next two years.
a) A Non-Neuroleptic Treatment for Schizophrenia.Mathews, S. Schizophrenia Bulletin 5 (1979), 322-332.
b) Community Residential Treatment for Schizophrenia.Mosher, L. Hospital and Community Psychiatry 29 (1978), 715-723
c) The Treatment of Acute Psychosis Without Neuroleptics.Mosher, L. International Journal of Social Psychiatry 41 (1995), 157-173.
d) Treatment of Acute Psychosis Without Neuroleptics.Bola, J. The Journal of Nervous and Mental Disease 191 (2003):219-229.
6. Is the cure worse than the disease?
a) Maintenance Antipsychotic Therapy.Cole, J. American Journal of Psychiatry132 (1977): 32-6.
In 1977, Jonathan Cole, the former head of the NIMH Psychopharmacology Service Center, concluded that given the myriad of problems caused by antipsychotics, “every chronic schizophrenic outpatient maintained on an antipsychotic medication should have the benefit of an adequate trial without drugs.” He titled his article, “Is the Cure Worse than the Disease?”
B. A Biological Explanation for Drug-Induced Chronicity
7. Drug-induced supersensitivity psychosis
In the late 1970s, two physicians at McGill University, Guy Chouinard and Barry Jones, identified the biological changes induced in the brain by antipsychotics that led to the high relapse rates for drug-treated patients. Because the drugs dampen dopamine activity, the brain tries to compensate by becoming “supersensitive” to dopamine. In particular, the drugs trigger an increase in the density of dopamine receptors. This perturbation in dopamine function, over the long term, makes the patients more biologically prone to psychosis and to worse relapses upon drug withdrawal. Chouinard and Jones concluded: “Neuroleptics can produce a dopamine supersensitivity that leads to both dyskinetic and psychotic symptoms. An implication is that the tendency toward psychotic relapse in a patient who has developed such a supersensitivity is determined by more than just the normal course of the illness.”
a) Dopaminergic Supersensitivity After Neuroleptics. Muller, P. Psychopharmacology 60 (1978):1-11.
b) Neuroleptic-Induced Supersensitivity Psychosis:Chouinard, G. American Journal of Psychiatry 135 (1978):1409-1410.
c) Neuroleptic-Induced Supersensitivity Psychosis:Chouinard, G. American Journal of Psychiatry137 (1980):16-20.
d) Neuroleptic-induced supersensitivity psychosis, the “hump course” and tardive dyskinesia. Chouinard, G. Journal of Clinical Psychopharmacology 2 (1982):143-4.
C. Twenty-Five Years of Confirming Evidence
Psychiatry has mostly ignored the problem of “neuroleptic-induced supersensitivity psychosis” since the early 1980s. But since that time there have been a number of long-term outcome studies that have confirmed the fact that antipsychotics increase the likelihood a person will become chronically ill.
8. Philip Seeman’s animal model of psychosis.
a) Dopamine Supersensitivity Correlates with D2 HIGH States, Implying Many Paths to Psychosis. Seeman, P. Proceedings of the Nat Acad of Science 102 (2005):3513-18.
b) Breakthrough Dopamine Supersensitivity During Ongoing Antipsychotic Treatment Leads to Treatment Failure Over Time. Samaha, A. J Neuroscience 27 (2007):2979-86.
In these two articles, Philip Seeman from the University of Toronto reported that agents that trigger psychotic-like behavior in animals–amphetamines, angel dust, lesions to the hippocampus, gene-knockout manipulations–all cause an increase in D2 receptors that have a high affinity for dopamine. However, he found that haloperidol and olanzapine both doubled the density of D2 HIGH receptors, and thus cause the very biological abnormality that in animal models had been identified as a final pathway. In a 2007 paper, he concluded that “these results are the first to demonstrate that ‘breakthrough’ supersensitivity during ongoing antipsychotic treatment undermines treatment efficacy.
9. Cross-cultural studies
a) The International Pilot Study of Schizophrenia.Leff, J. Psychological Medicine 22 (1992):131-145.
The first World Health Organization study that compared schizophrenia outcomes in “developed” and “developing” countries was called The International Pilot Study of Schizophrenia. It began in 1968, and involved 1202 patients in nine countries. At both two-year and five-year follow-ups, the patients in the poor countries were doing much better. The researchers concluded that schizophrenia patients in the poor countries “had a considerably better course and outcome than (patients) in developed countries. This remained true whether clinical outcomes, social outcomes, or a combination of the two was considered.” Two-thirds of the patients in India and Nigeria were asymptomatic at the end of five years. The WHO investigators, however, were unable to identify a variable that explained this notable difference in outcomes. See pages 132, 142, 143.
b) Schizophrenia: Manifestations, Incidence and Course in Different Cultures.Jablensky, A. Psychological Medicine, supplement20 (1992):1-95.
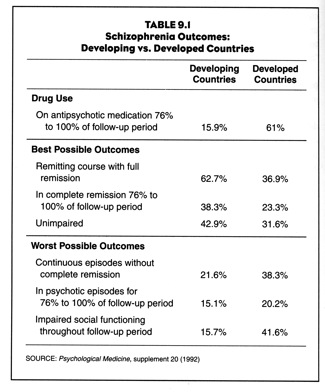
The second WHO study of this type was called the Determinants of Outcome of Severe Mental Disorders. It involved 1379 patients from 10 countries, and was designed as a follow-up study to the International Pilot Study of Schizophrenia. The patients in this study were first-episode patients, and 86% had been ill fewer than 12 months. This study confirmed the findings of the first: two-year outcomes were much better for the patients in the poor countries. In broad terms, 37 percent of the patients in the poor countries (India, Nigeria and Colombia) had a single psychotic episode and then fully recovered; another 26.7% of the patients in the poor countries had two or more psychotic episodes but still were in “complete remission” at the end of the two years. In other words, 63.7% of the patients in the poor countries were doing fairly well at the end of two years. In contrast, only 36.9% of the patients in the U.S. and six other developed countries were doing fairly well at the end of two years. The researchers concluded that “being in a developed country was a strong predictor of not attaining a complete remission.”
Although the WHO researchers didn’t identify a variable that would explain this difference in outcomes, they did note that in the developing countries, only 15.9% of patients were continuously maintained on neuroleptics, compared to 61% of patients in the U.S. and other developed countries.
Who Data Summarized
c) Cross-national Clinical and Functional Remission Rates. Haro, J. Brit J of Psychiatry 199 (2011): 194-201.
In this study funded by Eli Lilly, 11,078 schizophrenia patients in 37 countries were all treated with antipsychotics. The patients in the developing countries–North Africa and the Middle East–had functional outcomes as poor as patients in Europe. Thus, in this study where all patients were medicated, the functional outcomes of patients in the poor countries were much worse than in the earlier WHO studies, and now were no better than functional outcomes in the richer countries.
10. The Vermont Longitudinal Study
In a long-term study of schizophrenia patients released during the late 1950s and early 1960s from the back wards of Vermont State Hospital, Courtenay Harding reported that twenty years later 25% to 50% of the patients were completely off their medications, suffered no further signs and symptoms of schizophrenia, and were functioning well. She concluded that it was a “myth” that schizophrenia patients must be on the drugs all their lives, and the reality was that “it may be a small percentage who need medication indefinitely.”
a) The Vermont Longtitudinal Study of Persons with Severe Mental Illness, II. Harding, C. American Journal of Psychiatry 144 (1987):727-734.
b) Empirical Correction of Seven Myths about Schizophrenia With Implications for Treatment. Harding, C. ACTA Psychiatrica Scandinavica 90, suppl. 384 (1990):140-146.
11. A meta-analysis of the outcomes literature
a) One Hundred Years of Schizophrenia. Hegerty, J. American Journal of Psychiatry 151 (1994):1409-1416.
In 1994, Harvard Medical School researchers reported that outcomes for schizophrenia patients in the U.S. had declined since the 1970s, to the point that they were no better than they had been in 1900. Although the researchers did not blame antipsychotics for the poor outcomes, it is notable that this decline occurred during a period when American psychiatrists began telling the public that people diagnosed with schizophrenia had to stay on the drugs for life. In other words, the decline coincided with the adoption of a paradigm of care that emphasized lifelong drug therapy.
12. MRI Studies (1990s)
During the 1990s, researchers using MRI technology discovered that antipsychotics shrink the frontal lobes and cause an enlargement of the basal ganglia. In the “Follow-up Magnetic Resonance Imaging” study, researchers reported that the enlargement of the basal ganglia was associated with a worsening of both the positive and negative symptoms of schizophrenia. This was powerful evidence of how the drugs cause chronic illness over time.
a) Increase in Caudate Nuclei Volumes of First-Episode Schizophrenia Patients Taking Antipsychotic Drugs. Chakos, M. American Journal of Psychiatry 151 (1994):1430-1436.
b) Neuroleptics in Progressive Structural Brain Abnormalities in Psychiatric Illness. Madsen, A. The Lancet 32 (1998):784-785.
c) Subcortical Volumes in Neuroleptic Naive and Treated Patients with Scizophrenia. Gur, R. American Journal of Psychiatry 155 (1998):1711-1717.
d) A Followup Magnetic Resonance Imaging Study of Schizophrenia. Gur, R. Archives of General Psychiatry 55 (1998):145-152.
13. Nancy Andreasen’s Research on Brain Volumes
Starting in 2003, Nancy Andreasen, the former editor of the American Journal of Psychiatry, began reporting on her large MRI study of schizophrenia patients treated with antipsychotics. She found that the patients progressively lost “frontal white matter volume,” and that this brain shrinkage was associated with a worsening of negative symptoms, increased functional impairment, and, after five years, cognitive decline. In a 2011 article, she reported that this shrinkage was drug-related. Use of the old neuroleptics, the atypical antipsychotics, and clozapine were all “associated with smaller brain tissue volumes,” with decreases in both white and grey matter. The severity of illness and substance abuse had “minimal or no effect” on brain volumes.”
a) Progressive Structural Brain Abnormalities and Their Relationship to Clinical Outcome. Ho, B. Arch Gen Psych 60 (2003):585-94.
b) Long-term Antipsychotic Treatment and Brain Volumes. Ho, B. Arch Gen Psych 68 (2011):128-37.
12. Tardive dyskinesia and global decline
Over the long term, antipsychotics may cause dopaminergic pathways in the brain to become permanently dysfunctional. They may lead to movement disorders (tardive dyskinesia); severe psychotic symptoms (tardive psychosis), and global cognitive decline (tardive dementia.
a) Tardive Dyskinesia in Patients Treated with Major Neuroleptics. Crane, G. American Journal of Psychiatry 124, supplement (1968):40-47.
b) Clinical Psychopharmacology in its 20th Year. Crane, G. Science 181 (1973):124-128.
c) Functional Impairment in Tardive Dyskinesia. Yassa, R. Acta Psychiatrica Scandinavica 80 (1989): 64-67.
d) Central Determinants of Attention and Mood Disorder in Tardive Dyskinesia. Myslobodsky, M. Brain and Cognition 23 (1993):88-101.
e) Cognitive Dysfunction in Schizophrenia. Waddington, J. Brain and Cognition 23 (1993):56-70.
f) The Effect of Atypical versus Typical Antipsychotics on Tardive Dyskinesia. De Leon, J. Eur. Arch. Psychiatry Clinical Neurosciences 257 (2007):169-172.
Twenty percent of patients on atypicals developed tardive dyskinesia in less than five years, a rate similar to that with standard neuroleptics.
g) The Neuropathologic Effects of Antipsychotic Drugs. Harrison, P. Schizophrenia Research 40 (1999):87-99.
13. Martin Harrow’s 15-year outcomes study
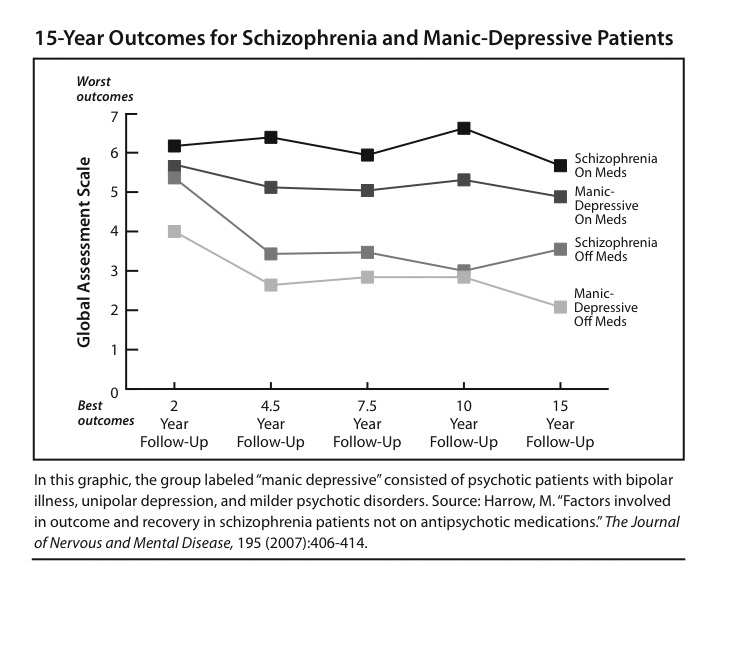
Factors Involved in Outcome and Recovery in Schizophrenia Patients Not on Antipsychotic Medications. Harrow, M. Journal of Nervous and Mental Disease 195 (2007): 407-414.
NIMH-funded researchers followed the long-term outcomes of schizophrenia patients diagnosed at two Chicago-area hospitals in the late 1980s, and they found that at the end of 15 years, 40% of the schizophrenia patients who had stopped taking antipsychotics were recovered, versus 5% of those who had stayed on the drugs. Long-term outcomes for patients with “other psychotic disorders” were also much better for those off antipsychotics than for those who stayed on the medications.
Long Term Schizophrenia Outcomes
Source: Martin Harrow and Thomas Jobe. “Factors involved in Outcome and Recovery in Schizophrenia Patients Not on Antipsychotic Medications: A 15-year Multifollow-up Study.”The Journal of Nervous and Mental Disease, 195 (2007):406-414.












[…] Association] and NIMH [National Institute of Mental Health], is of course completely false. See Robert Whitaker’s research, and also the work of Loren Mosher, as proof. Also, a few recovery stories as living […]
Report comment
[…] CorrespondentsArchivesSource DocumentsAnatomy of an EpidemicAntipsychotics/SchizophreniaBenzodiazepines/AnxietyAntidepressants/DepressionPolypharmacy/Bipolar illnessPsychotropics/Child […]
Report comment
[…] findings about the dangerous effects such drugs can have. (For a database on this subject go to http://www.madinamerica.com/2010/04/schizophrenia/ and http://www.madinamerica.com/2011/11/%ef%bb%bfearly-death-associated-with-antipsychotics/ […]
Report comment
[…] So, check out these studies and let me know what you think. http://www.madinamerica.com/2010/04/schizophrenia/ […]
Report comment
[…] name, neuroleptic, which literally means “brain damage inducing.” Why? Because that is what the research proves, over and over again, they […]
Report comment
[…] name, neuroleptic, which literally means “brain damage inducing.” Why? Because that is what the research proves, over and over again, they […]
Report comment
[…] might have very different experiences. Some of the evidence is described in this long article: Antipsychotics/Schizophrenia (although it's a bit of an anti-drugs rant, and it might not give a balanced view). […]
Report comment
[…] […]
Report comment
[…] someone who desperately didn't want them to having to release data that proved they did: Antipsychotics/Schizophrenia – Mad In America …. [note: Some links download the associated pdf's] 12. MRI Studies (1990s) During the 1990s, […]
Report comment
[…] http://www.madinamerica.com/2010/04/schizophrenia/ […]
Report comment
Removed for moderation.
Report comment