Soteria-style community houses are a proven, viable, cost effective alternative to traditional psychiatric hospitals. They offer a gentler, kinder, supportive environment for people experiencing extreme mental distress or crisis, commonly described as psychosis. In the majority of cases, this event is a psychosocial problem, not a biomedical one. While medical treatment is relevant to people suffering neurological damage from accidents or disease, it can be inappropriate and counterproductive for psychosocial conditions, often resulting in severe side effects, the inability to function in society, and significantly reduced life expectancy.
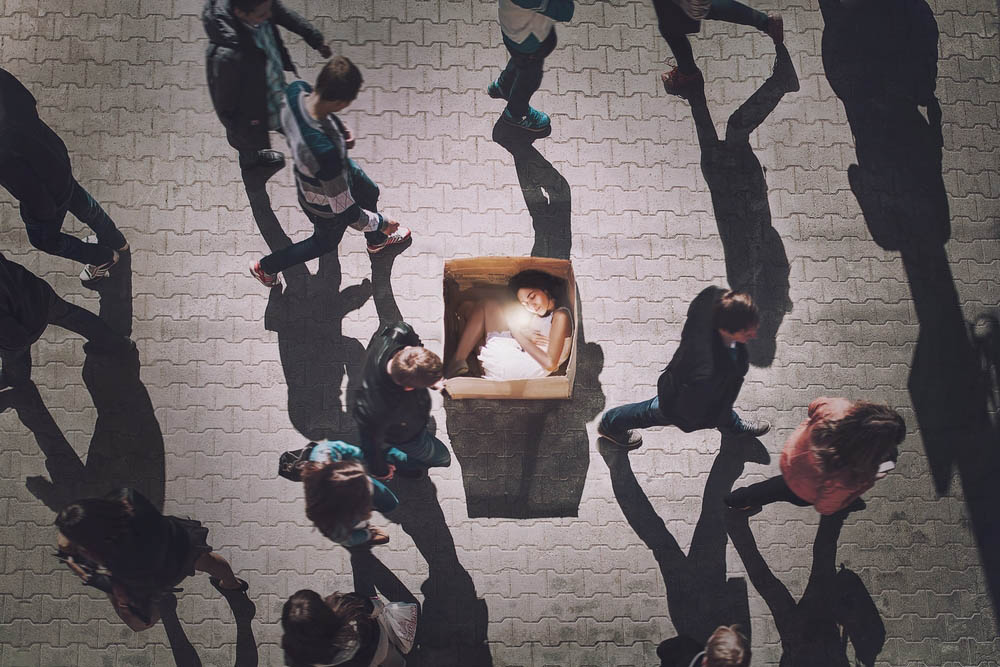 The original Soteria Project was founded by psychiatrist Loren Mosher in San Jose, California in 1971. For over 50 years, Soteria community houses and their variations have demonstrated the potential to produce better long-term results at a reduced cost compared to traditional psychiatric hospital treatment.
The original Soteria Project was founded by psychiatrist Loren Mosher in San Jose, California in 1971. For over 50 years, Soteria community houses and their variations have demonstrated the potential to produce better long-term results at a reduced cost compared to traditional psychiatric hospital treatment.
Traditional psychiatric hospital treatment is normally based on the routine use of psychiatric drugs, electroconvulsive therapy (ECT), and physical restraint. This environment is often perceived as authoritarian, hostile, and violent. The Soteria paradigm, while not adopting a dogmatic anti-medication position, aims to minimise the use of psychotropics and treat medication as something to be taken voluntarily from a position of informed choice, without coercion or compulsion.
The success of Soteria style community houses has often been the cause of their downfall. People with strong ideological motives opposed to non-medical approaches for dealing with psychosis have have often opposed and criticised them as irresponsible, dangerous, and ineffective—without valid evidence to support such claims.
Mosher was dismissed from his senior position at the US National Institute of Mental Health (NIMH) in 1980. In 1998, he also resigned from the American Psychiatric Association in protest. Despite these setbacks, Soteria houses have sprung up all around the world. Some have struggled to survive financially and have been forced to close due to blocking or withdrawal of funds, often for very questionable “political” reasons.
The key philosophical difference of Soteria communities compared to the traditional psychiatric approach is the idea of “being with” someone experiencing psychological distress as opposed to “doing something to” that person.
Soteria’s core principles have been defined as follows:
- Provision of a small therapeutic community with a high level of lay-person staffing.
- Efforts to preserve personal power, social networks and group responsibilities.
- A phenomenological approach, aiming to understand and give meaning to the subjective experience of psychosis.
- Minimal use of antipsychotic drugs, with any drugs taken being by fully informed choice rather than coercion or deception.
There is widespread, though not universal, disappointment with traditional psychiatric services. There have been many critics, some including medical practitioners like psychiatrist and neuroscientist Thomas Insel, former director of the world’s largest funder of psychiatric research, the NIMH, who said:
“Whatever we’ve been doing for five decades, it ain’t working. When I look at the numbers —the number of suicides, the number of disabilities, the mortality data—it’s abysmal, and it’s not getting any better.”
In a later interview, Insel conceded:
“While I think I succeeded at getting lots of really cool papers published by cool scientists at fairly large costs, I think $20 billion, I don’t think we moved the needle in reducing suicide, reducing hospitalisations, improving recovery for the tens of millions of people who have mental illness.”
Community–based mental health services
Most of Australia’s public psychiatric hospitals were closed by the 1990s. It was intended that they would be replaced with community-based services that would provide more personalised and community-centred care; however, the reality has been more complex. After more than 30 years, there remain significant gaps in the system. Some of the reasons cited include inadequate funding, a shortage of qualified mental health professionals, and a lack of community support due to stigma and discrimination, particularly around serious mental health.
There has been some progress towards community-based approaches, including the recognition and importance of peer support from people with lived mental health experience. This has led to the development of new models of care that prioritise consumer and carer involvement so approaches like Soteria are now more viable.
Soteria and Psychosis
In order to understand how Soteria-style community houses work and the potential role they can play in society, it is necessary to understand something about the nature of psychosis.
It is disappointing that many Australian government websites display inaccurate and misleading information about psychosis. One frequently seen and obviously absurd statement is that there is little or no understanding of what psychosis is or what causes it, but nevertheless the experts know how to treat it. This statement alone should ring loud alarm bells.
The experience of psychosis has been understood and interpreted in diverse ways in various cultures throughout history. It was and still is regarded in some parts of the world as a spiritual or mystical phenomena that is beneficial to a culture. While this idea often enrages the radical rationalist, their attitude is unfortunate. There are good, rational reasons for such beliefs in these often ancient practices. Early psychosis can reasonably be understood as the start of a transformative journey of mental development.
Pathologising or labelling psychosis as an illness only began in Western society with the the rise of rationalism around the 19th century, together with modern medicine and the scientific method.
As people began to place increased value on reason, logic, and individual autonomy, behaviours and experiences that appeared to be irrational were increasingly regarded as morally or socially deviant.
This type of thinking lead to deeply entrenched beliefs, which in turn have resulted in the strong stigmatisation of mental illness, together with the marginalisation of affected individuals. At its worst, this lead to an estimated 250,000 deaths at the beginning of World War II in Nazi Germany in a completely unsuccessful attempt to eradicate mental illness from that society. Cruel, inhuman treatments and practices that evolved during this eugenics era continue to this day, resulting in frequent, significant atrocities in many developed countries, including Australia.
There has been considerable worldwide research into psychosis over the last 30 years or so. Unfortunately a great deal of information from readily available high-quality research has failed to find its way into the public arena. The biomedical approach to mental health remains widely accepted, but is strongly criticised for reducing complex experiences and behaviours to a catalogued set of symptoms and for overlooking the social and cultural factors that contribute to these behaviours.
Psychosis is far more prevalent in our society than commonly realised. Studies suggest that around 60% to 70% of psychosis is never diagnosed or treated. Reasons given include stigma, lack of available services, and fear of the dehumanising treatment that is often imposed on those seeking help. Many, however, do not find psychotic experiences like hearing voices all that much of a problem. Some even find them useful. It is the unmanaged or unmanageable experiences together with social disapproval and vilification that are likely to result in significant distress.
Philosophy has a long history of exploring the nature of reality, both objective and subjective. Objective reality is often associated with scientific knowledge and empirical evidence. Language and logic play an important part. Subjective reality, on the other hand, refers to personal experience. It is shaped by perceptions, beliefs, and values as well as emotions, imagination, and creativity.
Psychosis can be understood in terms of these two functions. People normally have the ability to switch back and forth between these two realities, but this skill varies. Difficult or stressful life circumstances, including memories from past trauma, can easily result in a person finding themselves in the deep, muddy waters of subjective reality without the skills necessary to manage it.
It is no coincidence that many young people have their first psychotic episode in late adolescence when they are being called upon to make difficult and complex life decisions. The part of the brain that regulates between subjective and objective reality, known as the prefrontal cortex (PFC) and sometimes called the “Executive,” is still not fully developed.
These problems often have their origin in early childhood. Today’s emphasis on scientific rationalism has contributed to an educational and cultural bias towards valuing cognitive intelligence over emotional intelligence. This appears to have had a significant impact on the quality of life in our Western cultures together with a steady increase in mental health problems.
Emotional intelligence, like most things, is easiest and best learnt when young, but it can be learned at any stage in life. This is where Soteria-style communities can help. Those willing to make the effort learn how to manage their emotions and thereby their psychotic episodes. This ongoing process is facilitated through non-judgemental support, promoting self-determination, encouraging socialisation, providing holistic care, and giving priority to a recovery-oriented agenda instead of one that advocates an incurable, life-long illness.
If a person is homeless, jobless, lonely, and marginalised, or just extremely tired, stressed, and worried, it is likely that their experience of objective reality will not be a happy one. If such a person has the capacity to do so, escaping from an untenable objective reality to embrace subjective reality makes rational sense. Hoping to find a better life experience, even an imaginative one, is not irrational.
Claims are often made that people experiencing psychosis don’t make sense or can’t be understood. In the vast majority of cases these claims are untrue. With a bit of effort and skill, sometimes referred to as empathy, it is possible to step into someone’s psychotic space and communicate with them, even if you don’t accept the objective reality of their perceptions. It may also help to realise that a person in a psychotic state is often talking in metaphoric terms. Metaphor is a long way from meaningless.
Costs and Other Practical Considerations
Psychosis is a very expensive business. According to the Australian government, approximately 125,000 Australians are currently treated each year for psychosis. That is about 1 person out of every 40 who have some form of mental illness. This small number of people, however, consumes nearly half of the $11.5 billion of public money spent each year on mental health services. That is around $43,000 for each psychotic person.
Psychiatric hospital wards are also expensive. The average cost to stay in a public psychiatric ward in Australia is around $1500/day. The average stay is about 12 days, so the average cost of a stay in a public psychiatric hospital is around $18,000. Many people have multiple admissions in any given year.
Soteria–style community house expected costs
Based on experience in the US and other countries, Soteria style community houses cost about a fifth of traditional psychiatric hospital wards. We could therefore expect the running cost to be about $300/day.
This is possible because most costs are for staffing and Soteria houses are run by experienced lay people, often with their own lived mental health experience. Volunteers and the clients themselves also contribute to the running of the house, each according to their capacity. For a start, all household tasks such as cooking, cleaning, laundry, gardening, and, as far as possible, maintenance are carried out by the community.
Soteria length of stay and costs
In the original Soteria houses, residents could stay for as long as they liked. The average stay was about six months, but for some, with no restrictions, it probably became a home away from home.
Based on an expected cost of $300/day, a stay of six months would cost $54,000, which is more than the average annual expenditure for a diagnosed psychotic person. Some countries, notably Israel, have tailored their length of stay in Soteria facilities to match available funding from health insurers. This is an option to consider.
There are also various ways of extending the community experience at little or no additional expense. For example, if affordable shared rental accommodation is available in the near vicinity, stabilised residents who have at least entry-level employment could be encouraged to move out but still maintain close contact with the community, thereby both receiving and providing support as evolving volunteers. It should also be noted that the community automatically self-trains potential future staff. This on the job training could be supplemented with some formal training such as an appropriate non-degree technical and further education (TAFE) course.
Long-term costs
Research has suggested that the long-term costs of the Soteria approach are substantially less than the traditional medical approach. This evidence makes sense considering that institutional support with medication treatment can be lifelong and far from 100% effective. Soteria style support aims to empower people to self-manage their psychotic experiences toward recovery.
Community
Soteria-style houses are community-driven rather than institutionally driven. They are based on the idea that people experiencing psychosis will be subject to less trauma than traditional medical treatment in a supportive peer-to-peer family style environment that is part of a local community. It is also believed that this type of environment is more conducive to developing the skills for successfully managing their condition as well reducing stigma and improving self esteem.
Institutional models, on the other hand, are based on the idea that professional services and facilities are necessary for individuals experiencing psychosis. Institutional models typically prioritise the use of medications and other medical interventions, and normally have a more hierarchical and bureaucratic structure and clinical environment.
Looking Forward
One of the perplexing realities of mental health interventions is that nothing works for everybody and almost anything will work for somebody.
About 25% of people with a psychotic diagnosis seem to have acceptable experiences with the traditional psychiatric hospital ward approach together with the use of long-term antipsychotic medication.
About 40% have bad to very bad experiences. People in this group complain of debilitating side effects. Because they complain or don’t want to take the medication because of these side effects, many are then forced or coerced into accepting involuntary long-term treatment under administrative supervision. These experiences have been described as living a “zombie-like” existence. Another common and sometimes irreversible problem caused by antipsychotic medication is known as tardive dyskinesia. It can be extremely painful and has often been described as torture.
The other 35% of people traditionally treated for psychosis presumably have varying degrees of satisfaction or dissatisfaction between these two extremes.
It is the inhumane practices, experienced by at least 40% of those treated, that have come under heavy criticism from the World Health Organisation and the United Nations Human Rights commission. Australia is one of the world’s worst offenders of these forced or coercive practices, and the state of Victoria is the worst Australian state. Ironically, Victoria also has the highest treatment cost per person for psychosis.
I am not suggesting Soteria-style community houses as total replacement for all psychiatric hospital wards, although there certainly appear to be lessons that traditional mental health institutions could learn. Instead, they are envisaged as an alternative option for many who are unhappy with the traditional approach. This particularly applies to those facing or currently subject to involuntary treatment orders or wishing to withdraw from antipsychotic medication and finding few if any affordable facilities to assist them to do so.
The Soteria approach, however, requires prolonged effort. This can be challenging and not everybody is willing or comfortable undertaking such challenges.
In our instant, press-button, pill-popping world, there are many who just want a quick and easy solution, regardless of the consequences. While antipsychotic medication has more than its fair share of limitations and problems, if people are made fully aware of the consequences and wish to use medication to suppress their psychotic symptoms there seems to be no rational reason why they should be denied this choice.
On the same basis, given all the problems and limitations of antipsychotic medication, there seems to be no valid, rational reason why people who don’t want to be medicated should be forced to do so.
It is common knowledge that mental health in most developed countries is in a mess that is out of control and getting worse. While the number of people affected by psychosis is relatively small, the problem, both in terms of public monetary cost and human suffering, is anything but trivial. Many blame the pharmaceutical companies and the medical profession for the problem. They have undoubtedly played their part, but this article offers a deeper, more insightful understanding based on long term evolving social values together with the experiences of those who have lived through recurrent psychotic episodes.
This article summarises a recent feasibility study for introducing Soteria style facilities into Australia. Those readers who have an interest in moving this idea forward are invited to join the movement and support a proposal to the Australian government for funding. Some of this information may also be useful for anyone looking at Soteria houses and communities in other countries.
In many people’s minds, it offers a better option than forcibly requiring the use of heavy doses of antipsychotic medication for the rest of a person’s life. We need these sort of facilities in Australia and the time is right do something.












I’d rather go to Earth House if I needed residential attention. It was started by a New Jersey ex-patient, I recall, and may be still around.
Report comment
My belief is that everyone should, as far as possible, have freedom of choice in their mental health treatment. The current situation differs in different parts of the world. In Australia most people have no choice and are often subjected to involuntary confinement with little or no treatment other than anti pyschotic medication and sometimes Electro Convulsive Treatment (ECT). This approach is often worse than no treatment at all an leaves many MH suffers with additional trauma from the treatment experience. You may have noticed that the article talks about Soteria TYPE community houses which would allow for variations on the theme of a gentler, kinder, supportive environment with minimal use of medication by choice not by force.
Report comment
Thank you for the well written description of the wonderful possibilities demonstrated in the Soteria model. Good luck in Australia -Loren would be proud.
Report comment
Some “family” members like and enjoy the idea of forced involuntary “care” and want to ensure that the person with psychosis is “locked away”.
At the end of the day, unless making money is the bottom line, no one really cares. Remember that it is not “costing” Governments anything. Simply put, Goverments would rather spend tax payers’ dollars elsewhere, and preferably in a way that benefits them the most, as the priority.
Group Homes are for maximum profit ventures. Care is based on bare minimum standards and the appearance, illusion of proper and fitting attentions.
It seems as though people are living under rocks and in caves when they believe that the Governments et al. are interested in anything other than reputation and money.
Report comment
Tim, I very much like your article. It is very balanced. I love how your Soteria “accepts” people as if they are each rare and have “different” choices of how they want to be treated.
On a sunny bus today I was a bit hyper and I philosophically ruminated on activism. I was recalling my own penchant for activism in years past, particularly.
I shall go on now in this comment to use the word “you” in its broad, general form, so not at all referring to you personally.
On the bus I thought this and scribbled it down on the back of an envelope…
A kind of tyranny becomes the insatiable urge to “make a difference” to “the world”. The compulsion to “make a difference” has, underlying it, a curious non-acceptance of your own unique “differentness”. A uniqueness within you that is so miraculous it cannot be comprehended by others, who are also “different”. If you are so unique, a rare one off, then what are you doing all day in endlessly trying be part of a collective of sames, or a group full of same consensus opinion? This goes against your rareness. It is like a squirrel trying to belong in a den of foxes.
What is often behind the thrilling yet awful burdensome, drive to “make a difference” to “the world” is a failure. It is your own failure to realise that because you are so “different” as an individual, you may never be capable of uniting with the group or the wider group of “the world”. Your own acceptance of your “differentness” is what you shy away from in order to appeal to a collective who cannot accept your “differentness”. So why bother? As soon as you understand how rare you are this feeds the calm that becomes the real “difference” to “the world”. Gone is your urge to “change” the outer sphere, as if ever doing so would get you closer to your own acceptance of your “differentness”. And because you befriend your “differentness” with a passion you no longer are succeptible to being “policed” by the consensus opinion groups.
Instead what happens though is an alluring restlessness, an urge to “settle” the “disagreeableness” of the outer sphere, as if it is your only home. And this causes a need to get others collectively to “accept” your “differentness” or it is as if “the world” is tyrannically unaccepting of you. You may bond with others in a group who are all doing the exact same thing as you. Rather than them simply “accept their rareness” they try to “fix the world”, as you too do. And this effort, effort, effort every day to make a difference in “the world” holds a promise of you feeling the lovely healing that comes of “acceptance”, the “acceptance” of your miracle rareness that you could easily give to your own self from your own self instead. For who else can give you that acceptance if they cannot possibly truly “know” you, since you are so rare?
I see that everyone on the planet is clamouring for acceptance via “changing the world”, but because we are all utterly unique and rare, we all have “different” notions of how to accomplish this impossible, exhausting, never ending, feat. This then sets up factions and polar opposites and schizms and “disagreeableness” escalates. Everyone then says “the world” is in an appalling mess and all the disharmonious disagreeing proves it, and until “the world” is changed, by persuasion, or brute force, or war, or apocalypse, then it is never going to feel “accepting” of our rareness.
So in order to get “the world” to accept your “differentness” you think you have to radically forcefully destroy it, if push comes to shove. My how calm “the world” looks then! When it is covered with ashy fallout.
So is activism about “changing the world” or is activism about not changing anything? Even not trying to change the way someone else might not agree with you or like you. And is activism about trying to get “the world” to hurry up and “accept your difference and specialness” or is activism about “you giving you” that acknowledgement…that realization that never in human history has there ever been another person exactly like you.
When we die and our spirit goes to our sense of a hereafter there may be a life review but seldom do people want to come back. The rock stars do not want to come back and be rock stars. The medics do not want to come back and be medics. The learned professors at universities do not want to come back. None of them give a stuff about “their life’s work”. It is as if in dying we suddenly find the monumental healing we were searching for in our lifelong frenetic work of trying to “make a difference”. Invariably most of us are too small to make even a dent on human progress, or the lack of it. And angel realms do not seem interested in what rock album we did. I suspect none of us are meant to even begin to try to “change the world”. Doing so becomes at best a competition sport or energizing game but at worst becomes a “reason” for us not to smile kindly at an old woman who has been lonely for months. Whilst being so dementedly busy trying to “save the world”, the real world flies out of our busy hands unsavoured.
On the internet are a trillion videos uploaded every day that have the shriek of consternation, consternation, flabberghasted consternation….all voices saying “the world needs saved and changed or it will not accept us…so those people must be silenced…and these people must be silenced…”
But that consternation that tries to rally you to find your acceptance by joining forces, with the left or the right or with the believers or the heretics and so on deafens you to the voice of your own need for your own acceptance, and it rouses you to do your duty and work at being a saviour. Which really means being a destroyer of anyone too “different” to be saved. A kind of hysteria is sweeping world, about “the world”. The real world won’t last if everyone is trying to “fix” it.
You don’t have to save “the world”. All the animals are not saving “the world”. All the animals are finding their personal balance within it, through self acceptance, within it.
You are your own cure when you realise that what you have been looking for in exhaustingly trying to save “the world”…is you.
And when you do cure you, by accepting that nobody else will accept you because you are so incomprehesibly rare, you feel nurtured and serenity comes within and such calm has a ripple effect in other people, who you do not “try to change”, and that “acceptance” from you that they then feel, allows their self acceptance to blossom, and cumulatively, when eight billion people feel such calm, this collective wellbeing does “save the world”, by sort of resiting the allure of “changing everyone in it”.
Report comment
Thanks for the meaningful essay you wrote (as a comment). Good writing filled with meaning deserves a wide audience.
Report comment
My heart is touched that you responded so generously to me, Ron. I could hug you.
Report comment
Thank you Diaphanous Weeping for your interesting discourse on activism, your thoughts about the motivation that drives people to engage in these activities and possible consequences in doing so. Not all of us however are so altruistic.
My teenage years in the 1960’s saw a period of immense social upheaval with international events like the anti-Vietnam war movement, the women’s liberation movement and many counter culture activities including hippies, psychedelic drugs and the British invasion of rock music by the Beatles etc. In the world of mental health interesting things were also happening with counter culture psychiatry and psychology. Ken Kesey’s book One Flew Over the Cuckoos’ nest had a significant impact on psychiatric hospital culture.
All this pretty much went over my head. My interests were cars, girls and sport in about that order.
Then in the early 70’s my world changed dramatically and permanently. I foolishly confided with someone that I “heard voices” and soon after was involuntarily hospitalized and diagnosed with schizophrenia. When I emerged from hospital some months later I was a very different person.
I was unable to get a job, probably due to a loss of confidence from the hospital experience. Eventually I picked up some low paid contract assembly work that I was able to do from home. My first business evolved from there. I never did get a “real job” after that. I managed to earn a reasonable living for the rest of my working life as an entrepreneur, businessman and consultant.
Owning a business when you have psychotic tendencies is a significant advantage. Nobody can sack you if you take a week or three off to go to hospital and since there are plenty of mad businessmen around, mad behavior is likely to be deemed eccentric rather than psychotic. Eccentric is far more socially acceptable. That is not to say things were easy. Looking back it is amazing that I came through some of the bad periods intact.
Eventfully I retired and was happy to potter around with my hobbies and other interest but the local state mental health authorities had other ideas. In the years after I was first hospitalized, nobody cared whether you took your medication or not. Because of the side effects of these early ap’s I had no choice but to try and get through life with the minimum amount of medication which turned out to be a blessing. All that has changed now, at least in Australia, where the “thought police” come after you with legally enforceable involuntary treatment orders. They force their way into your home, hold you down, pull down your pants and inject you with long term depot anti psychotics. I have been fighting these people off for the last few years, even though I no longer use any psychiatric medication. They claim that since, in their view, schizophrenia is an incurable disease, what I am doing is impossible. By disagreeing with them about the need for me to take large amounts of antipsychotic medication I am, according to them, proving that I am unaware that I have a very serious illness which makes me a danger to myself and society. Since there is no viable legal redress in Australia for this kind of institutional insanity, I started clubbing together with others facing similar problems as a means of self defence.
The real crunch however came last year when my 19 year old granddaughter left home to live with her boyfriend. The relationship broke down and around the same time she lost her job. Understandably she was upset. She must have gone to the Commonwealth Employment Center (CES) to try and find another job and shown some signs of distress because the next thing we know the “thought police” have grabbed her, diagnosed her with bipolar disorder and put her on anti-psychotics. We got her a private psychologist to try and get her out of the hands of the state system but he turned out to be a dud as many of them are.
When someone or their family is threatened, the motivation to deal with it is usually survival, not a desire to change the world.
I first heard about Soteria houses on MIA. It interested me enough to read a book by the two guys who founded the first Soteria houses in the US in the early 1970’s. After reading this book I couldn’t help but think how much better my life might have turned out if I had had access to something like that back when I was first hospitalized. My grandaughter certainly needs something like that right now.
How does one go about establishing something like Soteria houses in Australia or for that matter anywhere? I pulled out my old entrepreneur’s hat, sat down with a blank piece of paper and a pencil and started work. What emerged could perhaps be described as a first draft of a business plan.
Earlier this year with the help of a few of my mad friends we set up a web site. I then wrote a couple of things including this article that MIA kindly published.
And that is how I became an activist.
Report comment
Yes, my friend. This is what I mean…
WE ARE “DIFFERENT” INDIVIDUALS.
Report comment
Yes, I agree my personal experience is that Australia psychiatric situation mirrors most of the Western world and some Eastern world countries.
Orthodox psychiatry has ensure that the population is not aware of the serious consequences to be treated with psychiatric drugs by not allowing scientific studies by researchers that shows clearly the disabling brain damage of those drugs, and by nullifying the experiences of the patients. Psychiatrist covers up the side effects from those drugs as if the person is increasing his her altered state of mind situation and by this increasing the drugs which makes a never ending cycle of “chronic illness”. I congratulate you Tim for the clarity of your proposal and for the will to go ahead with this, definitely your capacity of communication and analysis makes you a person to be respected and followed. My personal situation is complicated, nevertheless I hope I can be of any help with my humble abilities to promote Australia Soteria project that will empower young and old, men and women to see their altered state of minds as an opportunity to grow and discover ways to overcome that moments with the support of others and later help others to recover as you have explained so well in your text. Differential diagnosis seems are forgotten nowadays by GP! Nutrition and environmental factors are elements to bear in mind…. Sadly I do not see any good point in psychiatric drugging and I am very upset with orthodox psychiatry and governments supporting them, diplomacy is not my strength and I know is needed in this scenario to give that little step forward that can later on become a giant advance benefiting our families, friends and community G_d bless you Tim! ❤️
Report comment
Tim I am sorry to hear about your experience, specially when touches our love ones.
Your family is very fortunate with you, many families have no idea of what is going on in psychiatry until is too late and they cannot oppose it.
Yes, is important to do our best in overturn any abuse in society because any of us can be the next!
That is why I think is very important to spread as well the knowledge on what psychiatry is and psychiatric drugs do that is the secret to our freedom, is the ignorance in the main population that allows them to be controlled by the wrong leaders and pharma for their greedy intentions..
Specially judges in mental health tribunals need to have a training to understand the consequences of psychiatric drugging.
Report comment
I agree, Soteria houses worldwide, in combination with Hearing Voices groups and Open Dialogue type services, should be the replacement for psychiatry.
“understand[ing] and giv[ing] meaning to the subjective experience of psychosis,” is important.
The important word being “subjective,” as one who had a dream query about what a dream about being “moved by the Holy Spirit” meant, being misdiagnosed as “psychosis.” Not only do I have blasphemy of the Holy Spirit written right into my medical records, which is the only unforgivable sin in the Holy Bible. And it was absurd that my “mental health professionals” believed that all who dream are “psychotic.” Not to mention my former psychologist fraudulently claimed all societal distress, caused by 9/11/2001, was due to a “chemical imbalance” in my brain alone, which was an insane claim. By that child abuse covering up, former psychologist, when I was picking up her medical records.
“Minimal use of antipsychotic drugs, with any drugs taken being by fully informed choice rather than coercion or deception,” is wise and legal advise for all doctors.
I completely agree, informed consent is the law, and that law should be abided by, by all doctors and “mental health professionals.” But, for the past several decades, too many of the “mental health professionals” are now claiming ignorance of the common adverse and withdrawal effects of their psych drugs.
https://www.researchgate.net/publication/247806326_'Brain_shivers'_From_chat_room_to_clinic
Informed consent should include the truth that the antidepressants and ADHD drugs can create the “bipolar” symptoms.
https://www.amazon.com/Anatomy-Epidemic-Bullets-Psychiatric-Astonishing-ebook/dp/B0036S4EGE
And informed consent should include the truth that both the antidepressants and antipsychotics – which are both anticholinergic drugs – can create “psychosis,” via anticholinergic toxidrome.
https://en.wikipedia.org/wiki/Toxidrome
Which all mainstream doctors – including the psychiatrists – are taught in med school.
And it should also be pointed out that the antipsychotics / neuroleptics can create the “negative symptoms” of “schizophrenia,” via neuroleptic induced deficit syndrome.
https://en.wikipedia.org/wiki/Neuroleptic-induced_deficit_syndrome
“One frequently seen and obviously absurd statement is that there is little or no understanding of what psychosis is or what causes it, but nevertheless the experts know how to treat it. This statement alone should ring loud alarm bells.”
Especially since us psychopharmacological researchers, who’ve done our homework, already know that both the antidepressants and antipsychotics can create “psychosis,” via anticholinergic toxidrome.
As one who knows, “psychosis can reasonably be understood as the start of a transformative journey of mental development.” And I hope and pray all who deal with a “psychosis” largely do benefit from such “a transformative journey of mental development.”
“This [scientific fraud based DSM] type of thinking [held by the psychological and psychiatric industries has] lead to deeply entrenched beliefs, which in turn have resulted in the strong stigmatisation of mental illness, together with the marginalisation of affected individuals. At its worst, this lead to an estimated 250,000 deaths at the beginning of World War II in Nazi Germany in a completely unsuccessful attempt to eradicate mental illness from that society.”
But these “scientifically invalid DSM” psychological and psychiatric “genetics” based delusions are actually much worse than even during the Nazi psychiatric holocaust of the Jews. Since the current psychiatric and psychological industries of today are actually mass murdering over 7 or 8 million innocent Americans today, every year. Although I’m not able right now to find the confession of such by the America NIMH, since the current US government has taken such nationally paid for research, that all Americans should have a right to site, off the internet.
“if people are made fully aware of the consequences and wish to use medication to suppress their psychotic symptoms there seems to be no rational reason why they should be denied this choice.”
I agree. But I highly believe no one actually given truthful informed consent, would ever agree to treatment with the iatrogenic illness creating psychiatric drugs.
“On the same basis, given all the problems and limitations of antipsychotic medication, there seems to be no valid, rational reason why people who don’t want to be medicated should be forced to do so.”
I also totally agree, so forced and coerced treatment with the psych drugs should be made illegal.
“Many blame the pharmaceutical companies and the medical profession for the problem. They have undoubtedly played their part.”
I totally agree, as one who dealt with medical doctors who covered up, not only easily recognized malpractice on me, but also the medical evidence of the rape of my very young child, for my ex-religion.
https://books.google.com/books?id=xI01AlxH1uAC&printsec=frontcover&source=gbs_ge_summary
_r&cad=0#v=onepage&q&f=false
I stand adamantly against all “medical professionals,” or anyone else, who wants to psychiatrically and/or psychologically defame my children or myself, to cover up the rape and child abuse of my children, for my former religion.
Shame on the ELCA, and all other paternalistic religions, that bought into the scientific fraud of the psychological and psychiatric industries’ DSM “bible.” Maybe it’s just time to get rid of the last vestiges of the paternalistically created “western civilization.” And admit that the women have value and brains too?
Report comment
Hi there Someone Else
You said:
“I highly believe no one actually given truthful informed consent, would ever agree to treatment with the iatrogenic illness creating psychiatric drugs”
While your beliefs do seem reasonable, my experience is that this unfortunately is not the case. I have personally spoken to a number of people on antipsychotic medication who are terrified at any thought of giving them up. They also feel threatened by any moves such as legal challenges that think might interfere with their access to medication. Some of these people are well educated, highly intelligent and well aware of the consequences including significantly reduced life expectancy. I believe that the problem is the fear of facing the underlying issues that they would be exposed to if they gave up their medication together with possible memories of trauma from previous psychiatric treatment. To the best of my knowledge there are no figures on how many people fit into this category but the figures quoted in my article would suggest that it is possibly of the order of 20%-30% of antipsychotic medication users.
You said
“forced and coerced treatment with the psych drugs should be made illegal”
I agree with you in principle but what most of us are looking for is to have laws that distinctly allow involuntary treatment and confinement removed from mental health acts.
There are many people around the world including some top legal minds working on this problem but at this stage, powerful vested interests like the multinational pharmaceutical companies and medical fraternities appear to have the upper hand. Australia where I live and our near neighbour New Zealand currently have one of the highest involuntary treatment and involuntary confinement rates per head of population in the world. Also many ordinary people from all walks of life support the use of involuntary constraint and medication. Many want to see these restrictions increased. The underlying issue appears to be a combination of ignorance and fear that any easing of involuntary restrictions will result in a flood of psychopathic murderers roaming the streets. Two of our colleagues, consultant psychiatrist and assoc professor Giles Newton-Howes and legal activist and assoc professor Dr Sarah Gordon took the New Zealand government to court earlier this year (2023) to challenge existing laws. They are still waiting on a judgment four months later. This judgment which ever way it goes seems likely to have world wide repercussions.
We are also becoming increasingly aware of many people working in the mental health system who are distressed and frustrated by what they see going on. They too feel powerless to change things and feel that they have no option but to comply with the demands and practices of a system that they often disagree with. Their only other option is to walk away from jobs that they have often spent years studying and training for.
You said “psychosis can reasonably be understood as the start of a transformative journey of mental development.” And I hope and pray all who deal with a “psychosis” largely do benefit from such “a transformative journey of mental development.”
In my opinion you have touched on a very important subject which I would like to see discussed on this and other forums a lot more. At the moment it still seems to be a taboo subject with many people. It deals with some important and quite ancient ideas that were being discussed extensively from about the 1950’s to the 1970’s by people like Carl Jung and quite a few others. By the 1980’s the medical model with its brain chemistry imbalance story had pretty well taken over. Any ideas about transformative journeys were being dismissed as nonsense. The pendulum seems to be swinging back the other way again. While this aspect of psychology still remains very much on the fringe, there are certainly some practitioners around around who have an interest in it. It is worth noting that most people interested in this topic, myself included, believe that the use of antipsychotic medication suppresses any transformative activity. There are sound reasons for this hypothesis.
One interesting aspect of this movement is that the Australian government will make previously illegal psychedelic drugs legal for research purposes from the 1st July 2023.
Report comment
Here is a poster people can put on their wall if they want to. It is a bit like the alcoholic’s anonymous prayer, or other supportive affirmations.
“When someone, anyone, is trying to persuade you to be thinking in a particular way, say this…
You want me to be agreeing with you, you in your differentness, to leave my own differentness to become more like you, side with you, be another you. But supposing I do this? What real difference to the way you are so wonderfully different will it make? My being a clone or identical copy or twin of you, wearing the same shoes, buying the same socks, liking the same music, reading the same authors, at best is only going to convey a sense of shared interests. This cameraderie viewed as only coming from indentical choices may help you feel more “right” about your own choices, as if my apparent allegiance to your choices shows enthusiasm. As if my colluding with your choices within your differentness reassures you that you are on “the right path” and are “going in the right direction”.
You may be displeased if I want to go with my own differentness and not yours. You might say I am “wrong”, or you might say I am “going in the wrong direction”.
This attitude of “you are wrong to be you” or “you are right to be me” forms a bickering over the way we are all, all eight billion individuals, completely rare. So who is broadcasting the standard and categorizing of all of these eight billion individuals and declaring them to have a “right differentness” or a “wrong differentness”?
If ALL ARE EQUAL then WHO is telling each of eight billion that they really must be like everyone else, right down to their choice of shoes or socks or music or beliefs or thoughts or feelings? It is as if a morality is trying to stop bullying in the world but is imagining this is done by making all eight billion people identical and not different and not rare. But is bullying the same thing as differentness in choice of shoes or socks or music or belief or thought or feeling? Are all those differences bullying? Such that a policing morality needs to persuade us all to be clones? Imagine the world as full of identical copies of you. Everyone in the street are wearing your same kind of shoes, socks, listening to your music, praying in your beliefs, thinking your thougts, feeling your feelings? You might want to surprise someone with how daring you are to have lapsed in your belief, only to find all eight billion identical copies of you have already learned that about you since they sort of are you, so you will never be able to shock them, amuse them, worry them, rival them, support them, discover new things about them, nor they you. It would soon become horribly lonely. You are defined by not you. A pear is defined by not being a banana. Your boundary that contains your you needs others not being you to form what is beyond the boundary.
But is there another push to wanting me to agree to be more like you in your different choices? The drive to assert being “right” can sometimes come from having absorbed and bought the notion you are “wrong”. That becomes a deep wound. To heal that bullied wound you try to declare that you are not wrong at all but are right. You declare you are right to be you and rare and completely different. Indeed this is true. But to declare your rightness may mean telling another individual that that they are all wrong for being their choice of differentness. To heal you from having absorbed nonsense that you are wrong means wounding an individual for their being different in their own rare choices. Your boundary becomes less about defining you as different from someone else, or a pear or a banana, and becomes more about defining that your differentness is the right one and their way of being in the world is wrong.
When we are schooled into liking being told we are right, being right brings a warm feeling of security and goodness. So being declared bad brings a dreadful feeling. Extending that, when we call someone elses differentness wrong, because they have wrong shoes or socks or music or beliefs or thoughts or feelings, we call the sum total of that individual bad. Not only do they get told they must drop their different rareness and become you but they are told they are wrong and bad if they do not become you. This happened in the Spanish Inquisition.
Prove it, prove it, prove it, becomes the message. An individual gets told to prove why their different socks or shoes are the right choice, why their beliefs and thoughts and intimate feelings are the right feelings. If they cannot offer an extreemly rational explanation then they and their differentness is deemed a problem for the making of a right world, that only has the right kind of different people in it, all identical, all wearing the same socks and shoes. All of that need to prove your own differentness right is done because of a failure in you to really believe your differentness is indeed right or rather so rare it cannot be reduced to judgey categories or standards that way….and so are all eight billion other peoples differentnesses right or rare and special to them. Now, you may not like their different choices. You really do not have to.
Some people might say…make me like you by being pleasing to me, by disowning your differentness.
All you have to reply is…you do not have to like me.
How can you be wrong? You are too rare and unique to fit into consensus opinion. What any individual can be is abusive or bullying and cruel. That is not so much a choice as a sickness connected to making healthy choices. That sort of bad behavìour may be different also but it is also a form of oppression towards other peoples freedom to choose to be their own different. As such you may call abuse and bullying and cruelty WRONG.
But all other million trillion choices and differentnesses are harmless. And getting people to change those robs them of their sense of who they really are, and that is part of what makes the wound that later wants to tell you that you are wrong for merely being the rare being that you are.
You may say that I should drop my differentness to support you, as if my rareness holds you back, or as if you need me to empathize with the way you are getting bullied. This is magical and good. It is wonderful when people unite against bad despotic leaders, but being against bullying does not mean having to change your shoes and socks and music and thoughts and feelings. And because a bully becomes that way by in childhood never being allowed to be their own sweet rare self, the work of reducing bullying in the world involves leaving people alone to be exactly who they prefer to be. The acceptance of difference, not the acceptance of bullying, is curative.
Report comment
I’d love to see all that condensed down to one succinct sentence.
Report comment
Would you? If you read my longer comments spanning two years you would find me extolling the importance of Soteria houses. I recall saying that there should be a Soteria House in every localiy globally. I did not confine those comments to a single sentence. And I am glad you did not either.
I have a kind of schizophrenia that causes me to do scriptomania, I feel compelled to write all day every day. It is a symptom. I cannot help it. I hope that if I go to Soteria House this difference of mine will be okay there.
If I might be so bold I seem to have left you maybe concluding that my not responding to your very real traumas in your life has been a sign of disregard. This is simply not true. I read all of your comment with sadness. You have had ghastly experiences of torture. I could share some of my own but that would be to crowd out your own harrowing story. I wanted you to have your own arena to make it stand out and be heard.
It is also a tendency of mine to pick up on what a commenter said and go into a private philosophical space in my own mind and study many aspects in a philosphical way. In my own opinion many schizophrenics who are friends of mine are like this. You say the colour crimson and away they retreat, only to come back with screeds of theories on the nature of human existence. Some schizophrenics I know take such theorizing in a poetic or visionary direction, others take it in a political direction.
Perhaps you want political change. I am more dreamy. I often regard political hopes as not being realistic about the limitations of human integrity.
I am like the lone kid in the school yard who talks to herself. Everyone else wonders why I am not on their side. I have no answer as to why I feel compelled to be apart. But that does not mean I am not love.
Report comment
Hi Diaphanous Weeping,
You said- I recall saying that there should be a Soteria House in every locally globally
Agreed. They need to be spread throughout every community. For us in Australia that probably means about 1 to 2 Soteria houses for every local council municipality.
You said- I have a kind of schizophrenia that causes me to do scriptomania
I get it. Write away. I can’t see that doing you or anybody else any harm.
You said- If I might be so bold I seem to have left you maybe concluding that my not responding to your very real traumas in your life has been a sign of disregard.
The thought didn’t even cross my mind. My own traumas are no different to those of a few million others.
You said – It is also a tendency of mine to pick up on what a commenter said and go into a private philosophical space in my own mind.
I do the same thing myself. Sometimes I drive myself mad but then I am already mad. Oh well.
You said – Perhaps you want political change.
No I want change to the mental health system in Australia. I would like to see that change throughout the world but that extends the scope beyond what I think we can achieve from here. The change however has to be political because that is the way that health including disability and mental health works in Australia. Things are different in other parts of the world. If we are successful and I am optimistic that we will be, I would hope that it will have some follow on effects in other parts of the world.
You said -I am like the lone kid in the school yard who talks to herself etc
I can relate to that
Take care
Tim
Report comment
Hi Diaphanous Weeping
I had a thought that evolved from one of your earlier posts.
When someone, anyone, is trying to persuade you to be thinking in a particular way, smile at them and say….
“No Thanks”
Report comment
Tim, thankyou for talking to me on these notions. I am glad of your reaching out to me.
May your life and my life know the accomplishment of our good dreams.
Report comment
Hello Diaphanous Weeping, here Orli, pleasure to meet you, after reading a few of your posts have you thought about self publishing your insides?
Is almost free is clear you have blood of a writer!
Nothing to loose to try if you think you can enjoy it…
Let me know if you would like some practical information, I have some experience on that.
I do not think schizophrenia is a “mental illness” or any other label, they exist in order to drug people legally, without a diagnosis you cannot prescribe. No I am denying your “special mind function”, I am of the opinion that DSM should be banned…
Report comment
Hi Tim
Good luck with your efforts to get Soteria houses up and running in Australia, and hopefully, New Zealand. A little history. If you go back and look at Tuke and what he was doing at York with the Quakers, he was far closer to Soteria. If you look at Pinel, you can clearly see the use of leverage or force as the principle means of treatment. For example, his superintendent Pussin used to rattle chains before entering cells, under the misguided philosophy of the 18th century priest Condillac that fright would put the animal soul in conflict with the rational soul, and the rational soul might prevail. Reading Pinel you could be forgiven for thinking you were reading a missing chapter from Haley’s Strategic therapy. He was keen on finding medicine’s that might leverage change also – the first vaccinations in Paris were given in Pinel’s clinic. By contrast Tuke was not attempting to leverage change. His case examples show this. They had a sick house cow, and they turned to one of their residents, a farmer, and consulted him as to what they should do. The cow got better, as did the farmer, as his prestige rose in the community. I think that Foucault treats Pinel and Tuke equally as foundational stones for the medical model, but a close reading shows this difference. Many of the early asylums preferred Tuke’s approach; but I think the kicker came about mid-19th century that favoured Pinel’s approach. This was what to do with the “mad” and dangerous. This was the laws that allowed the locking up of some “mad” – magistrates thought they could rely on medical doctors to apply those laws humanely; and non-medics were an unknown commodity. So more and more asylums needed the head man to be a medic, and Tuke’s model was sidelined…
Report comment
Hi Nick,
I have read a bit of history about mental health facilities and treatment over the last 300 years or so. The Quakers both in the UK and the US seem to have set some good examples and precedents which unfortunately never gained much traction in the wider community. What I also find interesting is the way that treatment has moved back and forth between psychological/spiritual approaches and medical approaches, neither which appear to me to have been particularly scientific.
Report comment
Tom,
There’s a movie by Daniel Mackler on YouTube called, “Open Dialogue: an alternative Finnish approach to healing psychosis”. He has other films on the same subject.
I wish you the best of luck in your activism,
Birdsong
Report comment
You said:
There’s a movie by Daniel Mackler on YouTube called, “Open Dialogue: an alternative Finnish approach to healing psychosis”
Thanks. I will have a look at that when I find some time.
Someone pointed me to this one also.
https://www.eventbrite.com/e/listening-to-voices-tickets-628272438777?fbclid=IwAR0KucjrEtt-mb-XujnMNSCEEM6-hGkHhU40UJb8vnu5zgyeosW0clw7E_
I haven’t had a chance to look at this one yet either. This MIA article resulted in a flourish of enquires which is good of course but it is keeping me pretty busy.
Regards
Tim
Report comment
https://t.me/OrliBerm/3765
I have posted your article in my humble Telegram
Thank you
Report comment