A new study of the effects of the Physician Payments Sunshine Act, a policy passed in 2014 as part of the Affordable Care Act, finds that the mandated financial disclosures have not prevented physicians from being influenced by pharmaceutical industry money.
The Sunshine Act requires that pharmaceutical and medical device companies report gifts to physicians. Leading experts on financial conflicts of interest, Joel Lexchin and Adrian Fugh-Berman, investigated the policy’s impact over the seven years it has been in effect. They found no evidence that physician behavior regarding financial conflicts of interest has changed in that time. Further, there was no evidence that employers, meeting organizers, or medical journals have excluded physicians based on their personal conflicts of interest. They argue that something more is needed to redress the damages wrought by financial conflicts of interest in the medical industry:
“Disclosure is necessary but not sufficient to address the damage that industry relationships cause to medical knowledge and public health.”
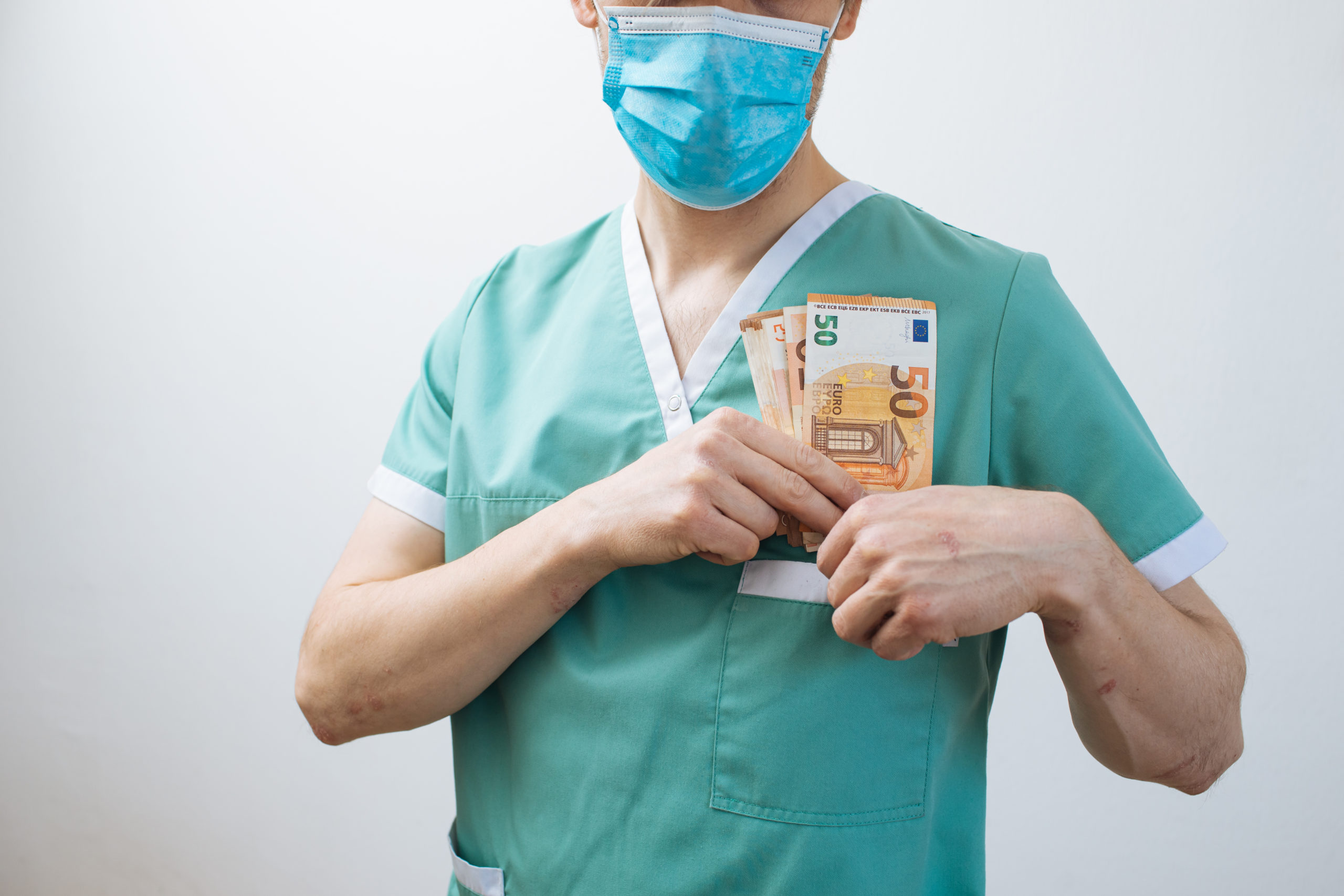 The problem of conflicts of interest in the medical field has been widely reported, despite industry efforts to downplay, rename, or hide the evidence. The field of psychiatry is no exception. At its extreme limit, financial conflicts of interest may result in inappropriate prescribing of medications and the creation of diagnostic constructs to develop markets for new drugs. Conflicts of interest (COIs) are also prevalent in psychotherapy research, where disclosure is far less common than in other fields.
The problem of conflicts of interest in the medical field has been widely reported, despite industry efforts to downplay, rename, or hide the evidence. The field of psychiatry is no exception. At its extreme limit, financial conflicts of interest may result in inappropriate prescribing of medications and the creation of diagnostic constructs to develop markets for new drugs. Conflicts of interest (COIs) are also prevalent in psychotherapy research, where disclosure is far less common than in other fields.
Lexchin and Fugh-Berman’s new article notes that the Sunshine Act has provided lots of information for researchers examining conflicts of interest via the payment database Open Payments. In a large study of over 150,000 physicians, for example, researchers found that those who received gifts from drug-device manufacturers prescribed a higher percentage of branded drugs and devices overall than physicians who received no gifts. Physician payments are also linked to increased prescribing of expensive branded drugs with uncertain medical benefits.
But just like on Wall Street, where mandated disclosure of conflicts of interest failed to alter the course of insider behavior that had already produced a long history of market scandals, the Sunshine Act caused no change in behavior in the medical profession.
“Despite robust, consistent results showing that payments to physicians degrade rational prescribing, there is no evidence that physician behavior regarding conflicts of interest has changed,” Lexchin and Fugh-Berman write.
“No effective policies have been enacted to restrict financial COI. Medical journals do not use Open Payments to vet authors or reviewers, and universities do not sanction physicians for COI.”
Further, there has been no change in consumer and patient behavior. Consumers rarely seek information about physicians, even when such information is crucial to their health, and generally show a forgiving attitude about the effects of financial COI. Somewhat perversely, the disclosure of COI may actually increase trust. Transparency, while necessary, is thus not a sufficient solution to the problem of physician-industry COI.
What is needed, the authors suggest, is a serious effort to eliminate financial COI. Some measures have already proven successful at decreasing COIs, such as limiting interactions between students and trainees and pharmaceutical companies. Other authors have suggested reforms to eliminate all gifts, free meals, and travel payments.
In 2011 the US Institute of Medicine also recommended limitations on the activities of physicians with COIs and the divestiture of financial investments for members of medical guideline development groups. Several medical associations have declined to accept funding from for-profit companies for research or educational projects.
“All of these changes,” Lexchin and Fugh-Berman write, “need to be accompanied by a strong and ongoing endorsement from the leadership in the medical community” to protect the influence of money on physicians’ ability to deliver quality care to patients.
****
Lexchin, J. and Fugh-Berman, A. (2021). “A Ray of Sunshine: Transparency in Physician-Industry Relationships is Not Enough.” Journal of General Internal Medicine, published online 10 March 2021. (Link)














Actually I’m not surprised at these findings. How many patients know how to research their doctor’s conflict of interest or understand its importance? Medical journals accept pharmaceutical money and universities have their own conflicts of interest. So their indifference is to be expected. And how many physicians, especially psychiatrists, have an incentive to support tougher laws when they’re benefitting from pharmaceutical grants and gifts?
Report comment
I have always considered “transparency” a joke. “I’m taking bribes from Big Pharma to promote their drugs. Here are the companies paying me off.” And then the get to go ahead and make “recommendations” based on who is paying them, and no one stops them. How about disqualifying anyone on the take from participating in making practice recommendations? How about forbidding researchers at colleges and universities from taking any funds from industry directly, as used to be the case when I was a kid? As soon as you can use your research grant to get a patent and make a ton of money, your scientific objectivity is shot to hell, I don’t care who you are. Publishing one’s conflicts of interest is a useless and ridiculous measure. Preventing conflicts of interest is what we need to be doing.
Report comment
“At its extreme limit, financial conflicts of interest may result in inappropriate prescribing of medications and the creation of diagnostic constructs to develop markets for new drugs”.
No, not ‘…extreme limit(s)’….it’s SOP.
Following the DSM-IV’s wide expansion of symptoms for bipolar disorder that tripled the number of adult diagnoses in the U.S. and X40 for pediatric diagnoses (!) conveniently coinciding with new drug approval and ‘rebranding’ of old ones….I made an appointment with a psychiatrist during this ‘gold rush’ for the industry.
I had just closed a business, had a new job (with good insurance), my bills were current but teetering….causing stress & insomnia.
15 minutes into my appointment I was pronounced bipolar 1 and drugged with Astra Zeneca’s Seroquel, an antipsychotic (+ other drugs, of course) resulting in a Neuroleptic Malignant Syndrome ADR requiring an all-night monitoring of my vital signs in hospital.
And there she was in 2014… listed in Pro Publica’s ” Dollars for Docs” user-friendly tool to identify graft. Her largest donor…Astra Zeneca, makers of Seroquel who contributed towards her $65,000 annual haul from pharma….a nice, new E-class Benz every year.
I became bankrupt and homeless as a result of the ongoing side effects of a relentless cascade of drugs, from private to state-funded prescribers, coast to coast, for 11 harrowing years…a compliant revenue stream & job creator.
The inscription over the gates to this psychiatric netherworld, paid for by pharmacy & their field-reps, the APA….
“Once drugged, always drugged”.
The periodic hand-wringing articles and lip-service that pop up from members lamenting the continuing APPEARANCE of corruption are an exercise in disingenuous cynicism and fool no one.
Ms. Logan’s article isn’t nearly angry enough.
Report comment
Well said, Krista!
Report comment
Of Course Not! As long as you have propaganda and the promotion of these drugs through advertising and mass media and other influences which make them look attractive, rather than the dangerous, deadly drugs they are. Thank you.
Report comment
The last line really caught my attention: “All of these changes,” Lexchin and Fugh-Berman write, “need to be accompanied by a strong and ongoing endorsement from the leadership in the medical community”.
That is the problem right there. The higher up you go in medicine, the greater the chance of corruption. Why would the leadership want to change a system that gives them so much money?
Even after the prescription opioid epidemic nothing has changed. There is a recognition that corruption can be a big problem in the political and justice systems, and there are measures in place to prevent corruption. (You can argue that these measures are inadequate, but there is at least an acknowledgement of how harmful corruption can be.)
In medicine, however, everyone seems to think that Doctors have some sort of moral super-power that no-one else in society has. Many of these problems exist because there is nothing in place to prevent it. Doctors and the Drug companies get away with it simply because they can!
Report comment