A new pro-recovery manualized intervention – called the REFOCUS intervention – has been developed and will now be evaluated in a multisite randomized control trials. The strengths-based intervention, which focuses on promoting relationships, is outlined in the latest issue of the British Journal of Psychiatry.

The REFOCUS intervention was developed by a group of researchers led by Professor Mike Slade at King’s College London. The team aims to influence both policy and practice “to help make mental health services in England more recovery-orientated and better able to promote wellbeing.”
The researchers began the development of REFOCUS from three main principles: (1) Prioritize involvement of people with lived experiences in the program, (2) Place an emphasis on supporting recovery for ethnic minority groups, and (3) Decrease the emphasis on diagnosis as a determinant of care.
To attempt to establish a model for personal recovery the research team then carried out a systematic review of recovery narratives, but because there was a lack of published recovery narratives involving people of ethnic minority groups, they also conducted a qualitative study of minorities using mental health services across England. Drawing on this evidence, the researchers collaborated with patients, providers, and experts to develop the REFOCUS manual.
They identified five key recovery principles, labeled the CHIME framework, including “Connectedness, Hope and optimism, Identity, Meaning and purpose, and Empowerment” as well as four recovery-oriented practices. These included “promoting citizenship (e.g. challenging stigma), organizational commitment (e.g. workforce planning), supporting personally defined recovery (e.g. treatments) and working relationship (e.g. interpersonal style).”
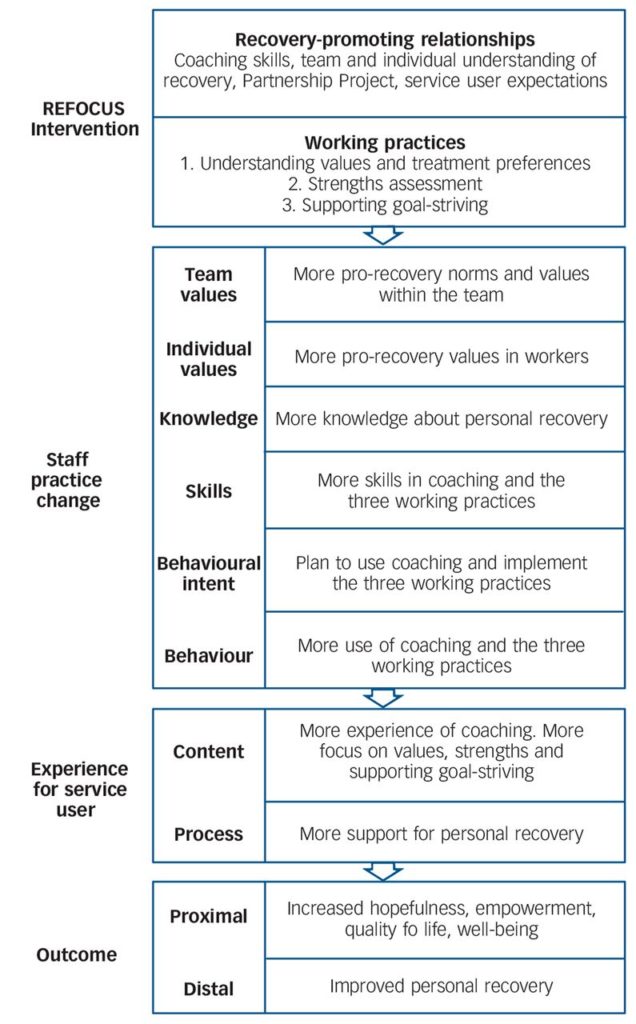
“The resulting REFOCUS intervention is intended to increase the support for recovery provided by community mental health teams,” they write. “The intervention is transdiagnostic and transprofessional, so in principle it may have relevance (following modification and evaluation) in other settings, such as in-patient, private practice, peer-run services or other clinical populations.”
Now that the program has been developed, the researchers have begun large multisite randomized control trials to evaluate the efficacy of the program.
*
Slade, M., Bird, V., Le Boutillier, C., Farkas, M., Grey, B., Larsen, J., … & Williams, J. (2015). Development of the REFOCUS intervention to increase mental health team support for personal recovery. The British Journal of Psychiatry, 207(6), 544-550.(Abstract)















Mike Slade is a good writer who is almost antipsychiatry in his attitudes by American standards. Here is a good paper by Slade and Eleanor Longden; The Empirical Evidence about Mental Health and Recovery: How Likely, How Long, What Helps?
http://www.mifellowship.org/sites/default/files/MIFellowship_Slade_Longden_Empirical%20evidence%20about%20mental%20illness_WEB_5_8_2015.pdf
The links at the bottom to the clinical trial sites don’t work. They’re behind some kind of log-in barrier.
I hope these trials show that relational non-diagnosis focused interventions for psychosis are better than torture as normal. As they should.
Report comment
Hi bpd, I agree.
I think the best starting position would be outlaw Diagnoses (like “Schizophrenia”/”Bipolar” or anything else) as these can be used as excuses to abuse and control and exclude people for the rest of their lives. These diagnoses are insults to human beings.
Psychosis can mean anything (I suppose), but I think the model should be one of recovery and independence, not longterm psychiatric illness and exclusion.
Report comment
Fiachra, I agree! Or rather, any way we identify people should make it clear that we’re not assuming they have a biologically based illness in the absence of such evidence. I think it’s much better to focus on reported experience (often misnamed “symptoms”) or what the person individually identifies as their problems than to give a label and think that explains anything. That approach is just so pathetic (the one that says “you’re schizophrenic and that explains these symptoms. Um No….”)
The model should be one that says that with sufficient help, people going through whatever can do what they want and become as healthy as so-called “normal” people, whatever they are. There’s a diagnosis we can use – “normal”, “healthy”.
Report comment
“Connectedness, Hope and optimism, Identity, Meaning and purpose, and Empowerment”
This is basically the opposite of today’s US psychiatric practice, based upon my experience.
“Connectedness,” I was told by my psychologist to “quit all your activities and concentrate on the meds.” I didn’t heed that bad advice, thank God.
“Hope and optimism,” I was hopeful and optimistic throughout my so called “treatment,” but my psychiatrist claimed I was “irrelevant to reality” and wrote in his medical records that he thought I was “w/o work, content, and talent.” Since, in reality, I had a wonderful group of friends, fine family, and was a very active volunteer who many appreciated and counted upon, I chose to continue to believe in myself, rather than believe my psychiatrist’s pessimistic and unhopeful delusions. In the end, he ended up declaring my entire life, all his delusions about me, a “credible fictional story.” Can “fictional” people blog?
“Identity,” I also didn’t bother buying into my psychologist’s and psychiatrist’s “lifelong, incurable, genetic mental illness,” identity belief system. In reality, my “mental health professionals” were just gas lighting me. And since none of the DSM disorders have any scientific validity or reliability all “mental health professionals” are actually nothing but gas lighters trying to convince people they have the made up DSM “mental illnesses.”
“Meaning and purpose,” I had meaning and purpose in my life, but found “mental health professionals” drugging me into oblivion in order to cover up the sexual abuse of my child for the ELCA religion and a “bad fix” on a broken bone at which my PCP’s husband was the “attending physician” to lack credible meaning and legal purpose in their lives.
“Empowerment,” I chose to leave my “mental health professionals” because their goal was to disempower me, for unethical child molesters and incompetent medical professionals. “I’m taking control,” and will write my own life’s story instead.
Let’s hope our society can rid itself of our current gas lighting industry, what is euphemistically called our “mental health” industry.
Report comment
Exactly, via diagnosing and overdrugging, most psychiatrists and psych hospitals today promote the following, despite misleading euphemisms to the contrary: Isolation, Despair, Identity Diffusion, Meaninglessness, Nothingness, Powerlessness.
As Dante wrote, “Abandon All Hope Ye Who Enter Here.” This message should be posted prominently above all but a handful of American psychiatric hospitals.
Report comment
And it was Dante who claimed the hypocrites would be the ones landing in the lowest depths of hell. By God, I believe we’ve found them!
Report comment
I had no idea there would be an entire industry that wants to be defamed with made up “mental illnesses” and tortured forever, however. I had thought we, as a society, all knew such behavior was wrong after the Holocaust.
As my son noticed when he was just a little boy, “the golden rule has a trick to it.” Treat others as you’d like to be treated, because you will be judged, based upon the way you treated others.
I’m quite certain this is why almost all real religions include this wise theology within their belief systems – not to mention it makes coexisting on the planet much easier. But the psychiatrists’ theology is that it is the right of a small group of people to defame and torture all the other people for the entirety of their lives.
Report comment