Researchers at New York University (NYU) developed a simulated training experience for primary care residents to learn more about the unique health needs of transgender patients. Findings, published in the Journal of Graduate Medical Education, highlight training outcomes and the value in learning through transgender community partnerships.
“Qualitative feedback from learners indicated that even those who had baseline knowledge of the basics of care for transgender patients found that the opportunity to interact with a patient in a low-stakes setting increased learners’ comfort during future real-world encounters.”
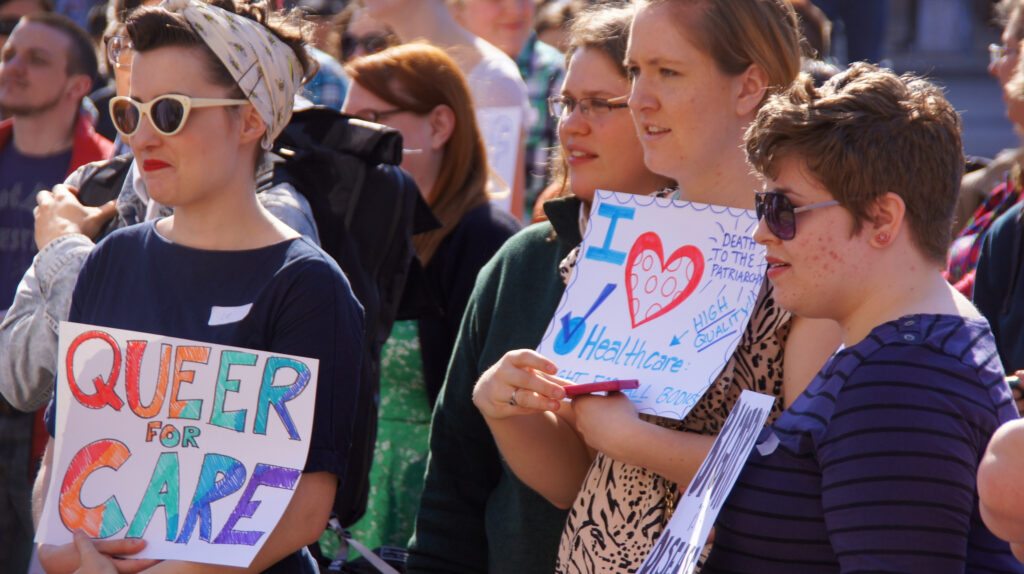
Richard Greene and his team of researchers call attention to commonly reported experiences of transgender patients who confront discrimination and substandard care when seeking medical services. Some propose that these blunders are a result of providers lacking adequate knowledge, training, and experience. The intervention designed by Greene and colleagues seeks to address this directly by providing a simulated experience in which residents interact with a transgender patient.
The team hired transgender actors who presented as women with high blood pressure and high blood potassium, and who were interested in undergoing an orchiectomy, the surgical removal of one or both testicles. In this case, the patient was presented as taking medication to treat high blood pressure, and estradiol, a form of estrogen.
After meeting with the patient, the primary care residents were tasked with developing a treatment plan for managing her high blood pressure and high blood potassium in a way that was collaborative and respectful to her values surrounding hormone treatment. Following the training, they were asked to complete a survey assessing their preparedness, perceived performance, and challenges.
The transgender actor and a faculty member also rated and provided feedback on the performance of each of the 23 residents who underwent the training. Criteria for their performance were developed from transgender health guidelines and specifics pertinent to this case but focused particularly on core communication skills, patient satisfaction, and case-specific skills.
“Learning objectives included asking patients their name, pronouns, and gender identity; discussing sexuality, sexual activity, and associated risks; and avoiding assumptions about hormone use or surgical treatments.”
When communication score and patient satisfaction score were compared to those in nine control cases, results demonstrated no significant difference between them. However, frequencies of specific treatment examples and qualitative data illuminate noteworthy findings. Despite not attaining statistical significance, both communication score and patient satisfaction score were higher after the training.
“Feedback helped residents identify learning needs, including how to ask directly about transition, appropriate terminology, how to admit lack of knowledge to a patient, and putting aside preconceptions about a patient’s identity.”
Additional outcomes indicated that 61% of residents made the patient feel comfortable and directly asked about her gender identity. While 58% of residents correctly identified the high blood pressure medication as causing dangerously high potassium levels, only 25% engaged in a discussion on possible remedies for high potassium. About 58% of the residents collected details on medically relevant information surrounding the patient’s transition. Finally, only 39% of residents offered the patient treatment for high blood pressure.
The residents’ performances demonstrated that good communication skills may serve as a method to overcome errors in clinical judgment surrounding transgender-specific cases. Yet, the authors note that the importance of implementing training programs such as this one is underscored by the fact that most residents did not directly inquire about the patient’s gender identity or long term goals of care.
Their observations lead the authors to encourage the development and implementation of training programs similar to this one, emphasizing the value in having representation from transgender individuals.
“We advocate for the use of transgender actors to play transgender roles, as their insights about patient experience are imperative to provide appropriate feedback.”
****
Greene, R. E., Hanley, K., Cook, T. E., Gillespie, C., & Zabar, S. (2017). Meeting the Primary Care Needs of Transgender Patients Through Simulation. Journal of Graduate Medical Education, 9(3), 380-381. (Link)















“Learning objectives included asking patients their name, pronouns, and gender identity; discussing sexuality, sexual activity, and associated risks; and avoiding assumptions about hormone use or surgical treatments.”
Hmm. I’m not seeing what this has to do with high blood pressure and high potassium.
Report comment
I think that the ultimate concern of this activity or training exercise was to give the residents a chance to interact with a transgendered person under the guise of blood pressure and high potassium. Many people are uncomfortable when transgendered people show up. Sometimes this stems from prejudice but a lot of times it stems from just being uncomfortable with something that you are not familiar with. Transgendered people are not going to go away and they are not going to hide so doctors need to learn how to deal with their own uncomfortable feelings in order that the feelings do not get in the way of providing the best medical care possible.
An equally interesting training exercise would be if they used “mental patients” as the subjects. As most of us know, many doctors treat us terribly if they find out that we have a lived history.
These programs not only teach young doctors and medical students how to look for and treat specific health problems, they also try to help the trainees grow as human beings who are more open to the modern world.
Report comment
Yes, I understand the motivation behind the training, and I think it makes a lot of sense. But how often do you go to a doctor specifically for high blood pressure and have them bring up your “sexuality, sexual activity, and associated risks”? It’s inappropriate.
Report comment
The effects of hormones can be responsible for a number of physical symptoms from what I understand, so that could be one reason for bringing up sexuality.
Report comment
Hormones may be relevant, but the person’s sex life isn’t.
Report comment
Not sure of your point, or implication.
Report comment
This was a very interesting training exercise. The high blood pressure and high potassium were just additional factors for the doctors in training. A transgender patient is a whole new ballgame.
Report comment
These kinds of training programs are quite interesting if you are the actor playing the role of a certain kind of patient. I’ve done this with second year medical students at the university medical center in the city where I live. You as the actor critique the medical student or doctor’s performance so it gives them a chance to see the areas where they need to improve the way that they interact with patients.
I remember one time where I was an actor playing a patient. These actors have a particular name but I don’t remember it now. Anyway, I was playing a farmer in his 50’s who was becoming very accident prone. My “sprained ankle” that I got from jumping off a running tractor was the third accident in two months. One of the objectives was to get the student to talk with me about prevention and being more careful and aware of what I was doing. Things went just fine for ten students and then with the eleventh I ran into a terrible snag. The young medical student listened to my explanation for why I got injured and then broke down crying. He began pleading with me to be more careful as he cried his eyes out. Then he explained to me that his beloved grandfather was killed in an accident with farm equipment. It was obvious that he was still grieving. As the actor you can’t go out of character at any time, no matter what the student says. Finally I said screw it and proceeded to remind the young man that this was only a training but this it obviously stirred up a lot of grief for him. And being the chaplain that I was I worked him through things so that he pulled himself together and we went on. I was not asked to be an actor again after that but as far as I’m concerned people come before all other things.
Report comment