A recent multinational study, led by researcher Hannah Jongsma, found that the treated incidence of psychosis is higher among racial/ethnic minorities, men, younger people, and in areas with lower levels of owner-occupied housing. This study highlights the pronounced variation of experiences of “schizophrenia” across the globe.
“The incidence of psychotic disorders varied by person and place, indicating that both individual and catchment area–level risk factors are important in predicting incidence.”
Previous research detailing the incidence of “psychosis” globally, has been assumed that the experiences referred to as “psychosis” are similar across contexts. However, subsequent studies, conducted in the U.S. and Europe, have documented considerable differences across experiences that coincide with factors such as age, race and ethnicity, neighborhood, and other environmental attributes. In these studies, men, younger adults, individuals from racial or ethnic minority groups, and people born and raised in urban settings were found to be more likely to experience symptoms associated with psychosis.
Apart from the one international study conducted by the World Health Organization, researchers have not investigated the incidence of “psychosis” world-wide, nor has it been explored in relation to these contextual factors.
In this study, the incidence of “psychosis,” as defined by the ICD-10 diagnostic criteria, was examined across multiple countries to investigate genetic and environmental determinants. More specifically, how age, sex, racial/ethnic minority status, latitude, population density, unemployment, and whether owner-occupied housing or single-personal household environments related to the incidence of “psychosis.”
Jongsma and researchers collaborated with centers in England (n = 2), France (n = 3), the Netherlands (n = 2), Italy (n = 3), Spain (n = 6), and Brazil (n = 1). Participants included 2,774 individuals (F =1196, M =1578; median age = 30.5 years) identified as experiencing their first episode of “psychosis.” The study was conducted between May 1, 2010 and April 1, 2015.
A total of 2,183 (78.7%) individuals were identified as having a nonaffective “psychotic disorder.” These results demonstrated an 8-fold variation in incidences of all “psychotic disorders,” ranging from 6 per 100,000 person-years in Santiago, Spain, to 46.1 per 100,000 person-years in Paris, France. This 8-fold variation was calculated with standardization for age, sex, and racial/ethnic minority category.
Rates were highest among racial and ethnic minority groups and men, specifically 18 to 24 years of age. Incidences of “psychosis” were lower in areas with more owner-occupied homes. For individuals identified as having nonaffective “psychotic disorder,” rates were similar, and for people identified with affective “psychosis,” lower rates were associated with high area-level unemployment, an unexpected finding.
The results of this study also identified a higher risk of “psychosis” for women older than 45 years-old. The authors additionally noted that this study’s findings “add further evidence to the observation that early intervention services with an upper age limit of 35 years (or lower) may lead to sex-related mental health inequalities: only 50.8% of women (605 of 1190) with psychosis were identified before 35 years of age in our settings, compared with 67.9% of men (1070 of 1577).”
“This study confirmed marked heterogeneity in risk for psychotic disorders by person and place, including higher rates in younger men, racial/ethnic minorities, and areas characterized by a lower percentage of owner-occupied houses,” report the authors.
The researchers discuss how first episode psychosis (FEP) also varied according to environmental factors:
“Incidence of FEP varied not only by person, but importantly, by place, suggesting that the social environment may shape incidence patterns of FEP.”
****
Jongsma, H. E., Gayer-Anderson, C., Lasalvia, A., Quattrone, D., Mulè, A., Szöke, A., … & Berardi, D. (2017). Treated incidence of psychotic disorders in the multinational EU-GEI study. JAMA Psychiatry. (Link)















“psychosis,” as defined by the ICD-10 diagnostic criteria,
I wish there was a real test for psychosis.
George Carlin said he was angry , the rich and the elite call the poor persons anger “psychosis” for not accepting the shick they are forced to eat, smell and handle. Not following orders? you are psychotic.
Higher the human density, the higher the rate of anger? You are driving me crazy!
“The owners of this country don’t want that. They don’t want a population of citizens capable of critical thinking. They don’t want well informed well educated people capable of critical thinking. That doesn’t help them. What they want are “Obedient Workers” People who are just smart enough to run the machines and do the paper work and just dumb enough to passively accept the low paying chitter jobs with the reduced pension and reduced benefits.” ADULT LANGUAGE https://www.youtube.com/watch?v=3RhIxxvYtRE
Report comment
There does need to be a non-subjective “real test” for “psychosis.” In the USA, the psychologists and psychiatrists, at least the ones that I dealt with, believe all thoughts, dreams, and gut instincts are “psychosis,” according to their medical records. That is a way-too-all-inclusive definition of “psychosis” because their definition of “psychosis” basically means everyone is “psychotic,” since we all dream.
I guess it’s good the “bio-bio-bio” DSM deluded psychologists and psychiatrists are now doing research into the potential “Environmental Factors Associated with Psychosis,” to try to imply their professions didn’t go off on a “mindless” insanity fest of belief and fraudulent claims to all of humanity that their scientifically invalid DSM disorders are all real “genetic” illnesses.
But that is exactly what they actually did, and they do owe the entire world an apology for deceiving the world with their scientific fraud, especially all those they’ve harmed. Particularly since they’re also raping our entire economy with their absurdly high prices, and fraud based research into their eugenics theories, rationalized by their claims their malpractice insurance is a high cost necessity that must be worked into the overall cost of all people’s health care.
If you doubt there is known medical scientific fraud behind the “psychosis” diagnoses. Here’s your medical proof that it has been medically known for a long time that the “antipsychotics” can create “psychosis,” via “antipsychotic” induced anticholinergic toxidrome poisoning.
https://en.wikipedia.org/wiki/Toxidrome
Repentance, real change, including proper amends to those they’ve harmed, is what’s needed by today’s DSM deluded psychologists and psychiatrists.
The majority won’t benefit from your fluff research pieces intended to continue to hide from the masses, the staggering in scope crimes being committed against humanity by today’s “mental health professionals.” Like the fact the number one actual function of today’s “mental health professionals” is, in fact, covering up child abuse on a massive scale, by turning millions of abused children into the “mentally ill” with the psychiatric drugs.
Today, “the prevalence of childhood trauma exposure within borderline personality disorder patients has been evidenced to be as high as 92% (Yen et al., 2002). Within individuals diagnosed with psychotic or affective disorders, it reaches 82% (Larsson et al., 2012).”
And, of course, the DSM treatment recommendations for these “disorders” do include the “psychosis” inducing “antipsychotics.” Oops, the medical community went off worshipping “Rockefeller medicine.” And the Rockefeller’s are an historically notorious, fraud based, war mongering and profiteering, fiscally irresponsible, we all now know ‘in need of a bailout,’ globalist bankster family.
Report comment
Some sure signs of Psychosis:
Imagination
Spirituality
Sensitivity
Sense of Humor
Playfulness
Love of beauty
Creative Output (shrinks can’t make/understand art, so artists must all be loons)
Depth of Character
Conscience
Insight (into people’s character; not gullibility)
Individuality
Need for Compassion
Disagreeing with Shrink
Failure to Worship Shrink
Complex Idealogy
Liking Cats Too Much
Lol! 😛
Report comment
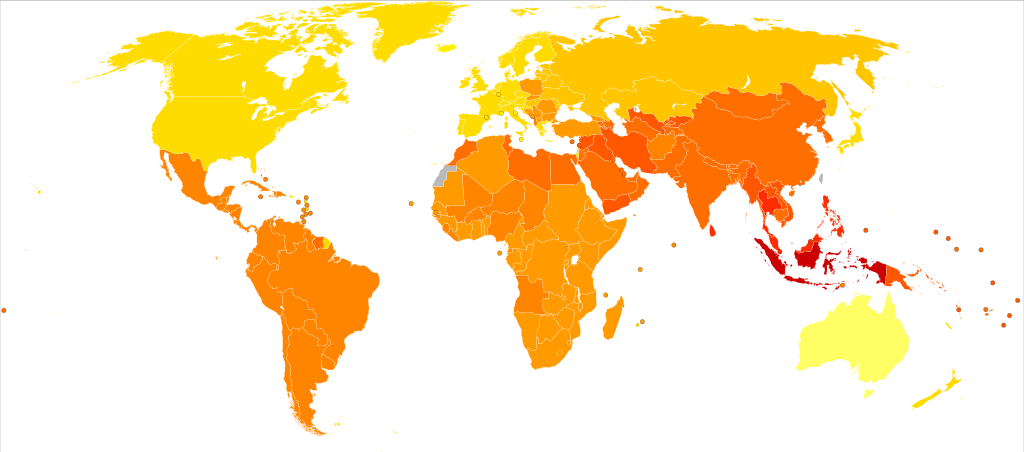
And the global map is screwy because north of the Canadian-American border there are fewer cities and fewer people which would make “psychosis” zero persons per square mile.
Report comment
mainstream US psychiatry will -not- acknowledge this, in all likelihood. They are still selling the myth that “Schizophrenia” can strike anyone, anywhere, at any time. I guess they want us to believe that people can be a-OK, and then one day, their brain malfunctions.
Even if one questions the validity of the diagnosis, it is worth noting that some areas are more “crazy-making,” for a lot of people, than others. Low status, poor social integration, poverty, isolation…these are the factors that go into creating “Schizophrenics.”
Again, I doubt most US mental health people will even give this information a cursory glance. This data does not fit their dogma, so they will choose to ignore it (my best guess, anyway). Hopefully, the mental health people in other areas are (or will be…) less dogmatic and take a moment to reflect upon their profession, how they treat people, etc.
Report comment
I wish people would learn to respond to all attempts at psychiatric and psychological testing with the middle finger.
Report comment
Just putting quotes around “psychosis” is meaningless if “it” is nonetheless accepted and treated as genuine.
Report comment