The involuntary commitment of persons with psychosocial issues links our healthcare and public health systems to the prison industrial complex. Disability justice advocates have critiqued the coercive practices endemic to civil commitment and forced hospitalization that remain legal in the United States, arguing that abolition must include psychiatry.
New work published in the Journal of Law, Medicine, and Ethics by Rafik Wabli and Leo Beletsky argues that the legal framework that sustains involuntary treatment and civil commitment cannot and must not be held out as a viable alternative to the criminal legal responses to behavioral and mental health challenges.
Instead, the authors advocate for “true alternatives to incarceration that are centered on liberation that seeks to shrink the carceral system’s grasp on individuals’ and communities’ lives.”
 Police are often the first and only agency to respond to a mental health crisis, which can lead to crisis escalation, hospitalization, incarceration, or the use of lethal force. Police involvement in involuntary psychiatric commitments has been steadily increasing, and Black people are more likely to become involved with mental health services through law enforcement and involuntary commitment.
Police are often the first and only agency to respond to a mental health crisis, which can lead to crisis escalation, hospitalization, incarceration, or the use of lethal force. Police involvement in involuntary psychiatric commitments has been steadily increasing, and Black people are more likely to become involved with mental health services through law enforcement and involuntary commitment.
Disability justice activists have also made the case that abolitionists must work to dismantle “alternatives to incarceration” such as community-assisted ‘treatment’ programs.
Drawing inspiration from street-level praxis and action, including grassroots organizations and community organizers across the country, the authors advocate for a Public Health Abolition framework that understands the relationship between public health and abolition as both longstanding and strategic. Quoting scholar/activist Mariame Kaba, the authors note:
“[Abolition is] much more than just eliminating laws such as involuntary commitment, or getting rid of armed officers that respond to mental health crises. It is about preventing further harm and violence from happening, and when it does occur, to not respond with more violence.”
A public health abolition praxis must thus follow the “positive project” of abolition: not merely eliminating harmful systems but creating new systems of care for those who use drugs or experience mental health crises.
One example of such a positive project is JusticeLA, a community-based organization founded in 2017 to shift the city’s dollars and investment away from police and prisons and into community-based systems of care. Since then, JusticeLA has led Los Angeles in transforming the city’s system of organized care. In November of 2020, for example, Los Angeles County voters approved the historic Measure J, which dedicated 10% of the County’s budget to fund alternatives to incarceration.
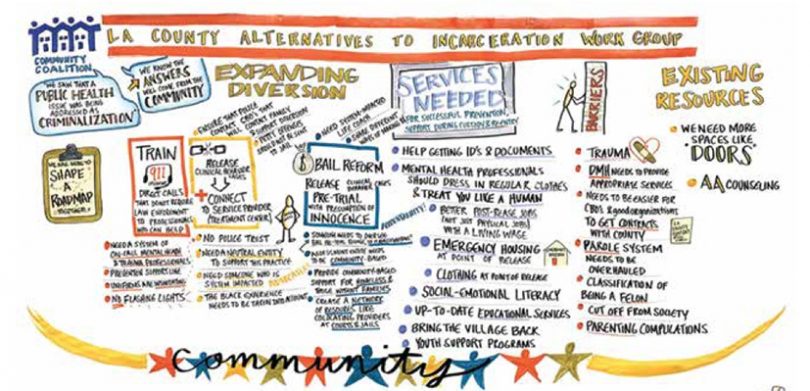
Another organization, the LA County Alternatives to Incarceration (ATI) Workgroup, helped create a roadmap for the county to transition to funding services and programs that better respond to substance use or mental health-related crises. The authors write:
“The recommendations in the ATI report include increasing non-carceral crisis mobile response teams, creating an alternate crisis response system (988 number), funding harm reduction services, supervised consumption sites, expanding access to medication for addiction treatment, and much more.”
The transformations underway in Los Angeles thanks to the work of organizations like JusticeLA give us hopeful examples of what the positive project of abolition looks like.
These efforts show “that an abolitionist public health framework works to dismantle systems and sites of oppression, and instead builds and reinforces systems and sites of care that address the root causes of violence and harm.”
****
Wahbi, R., and Beletsky, L. (2022). Involuntary Commitment as “Carceral-Health Service”: From Healthcare-to-prison pipeline to a public health abolition praxis. Journal of Law, Medicine & Ethics, 50(2022): 23-30. (Link)















Thank you Jenny,
I shall miss your articles. I must go.
I have a very old book that has lengthy epistles of a legal sort from another centrury, about abolition. The language of that era is extraordinarily convoluted, as is the linguistic grovelling deferring to powers in order to buy emancipation of some poor Jsmaican plantation captive’s liberty. A bit like saying to a jury, of a trafficked minor…
“Ladies and Gentlemen, we can see how rough and uncouth and bad mannered this child prostitute is, how dishevelled and unkempt she looks, and we can shudder lest she contaminate our noble higher thinking faculties which are God given, and yet does this bedraggled troublemaker not deserve new slippers?”.
It is grotesque. Such servile language. But servants of all sorts will be made of human beings who have the misfortune to live in an epoch of servile convoluted finicky verbosity of speech. Rationalism adores its words, not the emotions of the poor people tasked with keeping up with such words. A very word-centric world view tends not to be a heart-centric view of the individual with bruises.
I am disappointed that poor slipper limping Amber Heard has been thrashed by a million juries.
My own angels have it that she is an angel among us. Her job is to be thrashed by the masses because this leverage will begin the descent. A fall of Man. A fall into utter disgrace. A bit like how it took the grainy footage of callous ovens at a death camp to finally, finally, shine a light on despicable harrowing dismissal of culpability. By this I mean that women are going to be like the new trafficked. Spat at and reviled and pilloried. But women have souls who have sort of agreed to help the light be shone on endemic human shamefull cruelty. In order for the light to reveal the growing darkness in human hostility, human lovelessness, women are going to bear the unbearable as things get much worse.
Reading the pages of the old book I mentioned you just want to reach back in time and yell…
“Stop the hyperbole and just scream that intolerance is WICKED!!!”
Humanity is going to have to visit its penchant for torturing other innocent creatures in order to be able to take a good long look at itself. This is where women come in as ambassadors of peace in this process. But as is often the case with the “rational” mindset they cannot get beyond “word-centric bickering” and arrive at “heart-centric valuing” of other individuals emotions. They cannot see the bruises. There are more ways of leaving a room than by the door. There are more ways of leaving the body than by a bruise. And there are more ways to bruise someone than inflicting a spefic shade of lilac or prussian blue.
My schizophrenia at times has been so tormenting that I hit my head on any convenient hard surface. I can categorically state that it always astonished me that the hardness of a hit does not mean a deeper bruise. Often the weakest hit leaves the most profuse bouquet on the forehead. A dreadful 4am spree of using a wall to try to save myself by knocking out my hallucinations from my brow gave me six months of brain fog concussion but NO bruise.
I used to marvel at why people during the Spanish Inquisition found it acceptable to spectate, often packing a picnic and beverages, an act of unbridled atrocity in a town square. Did nobody want to throw up?
I now believe that what occurs is a mass hypnosis in the human herd that has them all pursuing a sense of virtue through grisly acts of nightmare violence. The virtue is coming from “decency”. A sense of entitled outraged rational self righteousness at the expense of any gut intuition that atrocity is the opposite of virtue. If your gut feeling is located in your body and your sense of reason is located in your intellect then it is the tearing apart of these, en mass, as intellect stretches away from its obligation to “have a heart”. Intellect often fears “feeling” since emotions are uncontrollable by “certitude”. Feelings just are what they are. They are not analysable, not that this stops the braying chanting mobs. The medieval mobs, all united in chorus as one herd, one engine, one rational man made machine. The picnic picky nitpickers camping on the court room lawn. The heartless puppets with ironic heart emojis on placcards, loud speakers of intellectual, cause and effect, fetishing, media indoctrination. The media is “right” so the bruises must be the “wrong” hue to be “real”.
Miss Heard is the first to the media death camp. A million bewildered angels will follow. Gentle hearted women. And caring heartfelt fathers, brothers and sons. The Anti Christ is coming. And all of the bile about narcissistic mothers and sisters and daughters is but a preparatory step in that journey to collective human depravity. The worm has turned.
The lambasting of the female of the human species IS the lambasting of “heart-centred” ways. The defilement and degradation of “feelings”. A woman cannot cry without it being regarded as the victim ploy of a demon narcissist and deserving of a global response of snickering and violence. It matters not one jot that being a narcissist in the true pathological sense is rare and that even then the narcissist is often more like a boring burden wearing an empath down, whittling away at the empath’s sychophantic people pleasing neurosis, which may not be a bad result. These days the narcissist is deemed unfit for human society. But being as narcissism is on a spectrum of normal this means everyone who cries into their nightgown and says they feel like a victim can also be declared a demon.
The black person in my old book was declared a weeper who did not have the pristine words or intellectual prowess to know the error of their way of weeping.
This is where we are at….Again.
A professor in my Divinity degree once said that it is never the suffering in society who we must concern ourselves with, if we know about them then they are not the ones who truly are suffering. The people who are the real victims are the ones not identified as victims but as problems. See it like strata. The surface layer may have one community, the next layer another community, the next layer another community. It is those way beneath the deepest known layer whose suffering apparently does not exist. And the worst is that it is this layer who do not even know it themselves that they are suffering oppression and persecution and damnation and atrocity. They just smile dry eyed as they sweep the streets or pour tea or mend the shirts of the jury.
Report comment
If your gut feeling is located in your body and your sense of reason is located in your intellect then it is the tearing apart of these, en mass, as intellect stretches away from its obligation to “have a heart”
Outstanding.
The certitude of rationalism is false anyway, though we kid ourselves that the ‘tearing apart’ allows us to understand complexity more clearly. It just the bolsters the illusion of understanding and allows us to stand apart. This standing apart is dangerous. We understand less while imagining the opposite, and can enact cruelty while patting ourselves on the back.
We need the wisdom of the heart.
Report comment
https://youtube.com/shorts/gPObIhdnxB8?feature=share
In addition to my previous comment Jenny, this video could have come straight out of the pages of that old book that has hideous court room charicatures of African slaves. The book is a snapshot of the gentrification of intelligence. Seeing intelligence as morally superior to crying. Such narcissism videos are doing what I long predicted. They are sliding collective awareness of the “I” and demonization of the emotions that come from the innocent “I” over onto women.
You cannot know your authentic feelings unless you are in touch with your “I”, as in “I feel sad” or “I feel afraid”. So you “I” is like a notice board where you stick your real feelings. What is gradually going to occur in global civilization is the disparagement of an individual’s basic human right to voice from their “I” any of their feelings “if” those don’t pass muster with metaphorical judges. A million people have become armchair judges and rather than use terms like sin, or sloth, or lust, or laziness, to counterpoint moral rectitude, certitude, and self righteous deceny, as was seen in the slave trade, instead the new condemnatory “word-centric” words are greedy narcissist, cunning borderline, manipulative victim and liar. These words come straight out of the annals of psych disciplines. Psych has given everyone permission to lambast everyone with these terms.
You may be wondering why I am in no hurry to ditch my schizophrenia diagnosis. My contention is that we need to turn our world what I call…
Baby caring.
By this I mean that it should not matter at all whether you call yourself a Jew or a Christain or an atheist or a woman or a man or an LGBTQ plus person or a mad person or a normal person or an addict or an alcoholic or s homeless person or a narcissist or a logical science buff or a fool or a schizophrenic or a gilded Mackaw with crystal feathers of deepest azure blue. If we ALL baby each other, which means treating each other as if..
ALL ARE EQUAL
then NOBODY should be badly heckled or lambasted or punished or abused or turned into servile forelock tugging puppets on strings. If today Jenny you want to call yourself a “remarkable interstellar nebula floating in a glass of spring water” and tomorrow you want to call yourself a “vessel of divine knowledge” and the next day you choose to call yourself “bipolar” and the next day “never been bipolar” and the next day “a world saving woman of compassion” none of these descriptors you choose for yourself should make you a biffed baby heckled by a million juries.
A MOTHER is symbolically a person who says “yes” to her baby all day long. The rare occasions of saying “no” are saying “yes” to life saving protection, such as “no” do not run accross the flat surface since it is really a highway with juggernauts on it. Mostly a MOTHER says “yes” to any eccentric or potty or bizarre or playful notions the baby dreams up because there is an awareness that love of life needs the marriage between “I” and “feelings” in order to make enjoyable and unique “free choices” that will grow a sense of wellbeing about being in the world. And when a billion “babies” feel such wellbeing the feeling spreads and soon the whole world becomes WELL.
But in this era, because the world is not well, humans need to re-understand the importance of being “baby caring” towards each other. This involves being at times MOTHERLY towards the eccentric or odd or different or bizarre or playful. It involves leaving people’s individual “feelings” and “free choices” and their “I” in peace to be whatever these wish to be. It also involves being MOTHER to your own needs for “baby caring” acceptance of what you like and need.
When a woman so symbolic of “emotions” is shunned in a court room what is being shunned is the human cry for “baby caring”.
Instead “baby caring” is lambasted as conniving, duplicitous, crafty, witch crafty, guilt tripping, vile, lying, lazy, greedy, bitchy.
This is what will continue in city after city, town after town, village after village, until all the actual real babies are called bitches.
When the horizon darkens with that pall of smoke and real babies are given no protection because their real mothers are scolded from attending to their babies “feelings” then the world will be awash in its own depravity and sickness. But one day a light will shine on this. A beacon. An a million mirrors that hold the reflection of judgemental hostile ugliness will brighten with human forgiveness.
I find there is nothing forgiving in this above video, on narcissism, that I link at the start.
More and more videos are coming like gushers from the Hoover Dam. Videos parrotting the merciless Anti Christ blueprint of the entitled.
When the Hoover Dam falls know this to be true.
People think the collapse of a dam or a global flood means a wet doormat and rabbit hutch. A massive flood means the spoiling of a billion ready meals in markets as refrigeration switches off. It means no street lights. It means black outs. It means gang warfare. It means the army being drafted in. It means no access to meds so a million jurers have to drop into a chasm of instant withdrawal. It means mass trauma, relocation, loss and grief on a vast scale and the one psychologist’s appointment diary booked up for a decade. Puppets on strings will seize the day.
But it is meant to go this way. Humanity is having its deck of preferences shuffled so that in future it plays a fairer game.
So there is nothing one can do to stop it. The angels are leading the way through the dark impenetrable forest, helping each human follow the distant light of the beacon.
Many will stumble into hostility, rage, violence, as they are taught to think the demon is their unknown neighbour. When there are no neighbours left but ghosts lifting veils behind smashed windows humans will pause and realise the silence contains no babbling of babies.
Report comment
https://youtu.be/ozjWLo-vdsU
I want to lastly share that I DO NOT think a big flood will happen any time soon. It may not occur for many years or a decade or more and so there is no point in dwelling on it beyond retaining its “possibility” like a pebble in a pocket, to feel once in a while. It is quite possible I am bonkers in this regard and nothing will occur…NOT ever. And I may have gotten it incorrect about food shortages and meds shortages. I do know the future that is coming is a nice one. So whatever natural disasters occur on this planet, which they regularly do, plucky humans ALWAYS find a way to recover. So please only read my mad utterances as if fairy tales, if you like. I might only be an old hag on a moor hissing into the lake and seeing portents in the ripple effect. So please ignore my jottings if you find them psychotically idiotic. I did predict covid fifteen years ago. So that was a long long long wait. And if I had fretted over it that first week I would not have been able to just go with the flow of life and be ordinary and that is what I believe life is for, the comfort of the ordinary and unsurprising. This video is of lovely divine beings, namely the beautifully ordinary Kirsten and Joerg. They have not a care in the world. They just never seem to think the worst will ever happen. They breeze through life and this is how I feel wellness comes. They are like a mom and dad who are always smiling and delighted. We have the choice to cultivate that interior parenting to our stressed inner baby. Life is already startling so the onus ought to be on calming right down and being a bit more like a passive, unflusterd animal. Just browse leaves all day. Animals never think the worst will happen either, nor do children. The live in the realm of “feelings, feelings, feelings”. They shut down “what if” thinking.
Even when or if the flood arises, in any disaster the best way to cope is to regard it all as a mirage and kind of pleasantly phase out being focused on it. Instead it would be better to be cultivating the art of being more dreamily Kirsten and Jeorg. I could say this is how to maintain balance. But it is not everyone’s choice. Lots of people are ponderers of philosophy or science or religion. All of that helps balance too, if it is “your” choice. There is no one way. It is all a case of seeing life and the world however you like to and pleasing yourself in it.
Sticky jam scone anyone?
Report comment