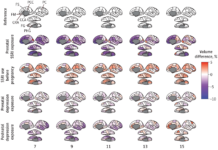
In a new study in pregnant mice, researchers found that an SSRI antidepressant, in combination with the immune response that happens after viral infection, may be dangerous to the fetus.
The researchers studied the effects of maternal inflammation (which is induced as an immune response to viruses) as well as the impact of the SSRI fluoxetine (Prozac). They found that the combination of fluoxetine and inflammation resulted in almost all pregnancies being lost.
“While most control, polyI:C [inflammation alone], and fluoxetine pregnancies successfully produced live pups, we found that a large fraction of fluoxetine pregnancies were lost following the [immune response],” the researchers write. “Moreover, only a few fluoxetine [plus inflammation] pups made it to weaning age while most pups from the other treatment groups were viable.”
Male mice born to mothers who had inflammation also exhibited autistic-like behaviors, including repetitive actions and impaired communication and sociability.
In the press release, senior researcher Jon Lukens said:
“Our results might help to explain the rise in autism prevalence over the last 20 years, as this time coincides with the rollout of widespread SSRI usage in the developing world.”
The study, published in Brain, Behavior, and Immunity, was led by Lukens and Kristine Zengeler at the University of Virginia.
 The researchers examined the biology of the maternal-fetal interface (MFI), which includes the placenta and other structures. This is the source of serotonin for the fetus—and serotonin is a vital brain chemical for developing various systems in the baby.
The researchers examined the biology of the maternal-fetal interface (MFI), which includes the placenta and other structures. This is the source of serotonin for the fetus—and serotonin is a vital brain chemical for developing various systems in the baby.
They write, “Given that the placenta is the sole source of serotonin for the developing embryo early in pregnancy, paired with the importance of serotonin for brain development, prenatal disruption of maternal serotonin levels could presumably alter offspring neurodevelopment.”
They also did behavioral tests to compare mice born to mothers with inflammation with those born to healthy mothers.
Experiment 1
The first experiment compared two groups: in one group, pregnant mice had an inflammation (immune response) provoked; pregnant mice in the other group did not. This response was meant to mimic the effects of a viral infection.
They found that the MFI for the mice with inflammation had extremely high serotonin levels, twice the usual amount.
Once the mice were born, the researchers did three behavioral tests:
- Ultrasonic vocalization recording: a measure of how often mice made sounds after being separated from their mother;
- Marble burying assay: a measure of repetitive behavior that involves seeing how many marbles the mice bury over a time period;
- Social preference test: a measure of whether mice interact with a mouse they’ve never met before or with an object they’ve never seen before.
The researchers found that male mice born to mothers with an immune response during pregnancy exhibited repetitive behaviors and impaired communication and sociability, which they write is suggestive of autism. However, female mice, and mice whose mothers were in the control group (no immune response), had “normal” behavior and sociability.
Experiment 2
The second experiment combined this with the SSRI antidepressant fluoxetine (Prozac), which the researchers write is one of the top 20 drugs most commonly prescribed to pregnant women. There were four groups:
- Mice dosed with fluoxetine then had inflammation;
- No fluoxetine, but inflammation;
- Fluoxetine, no inflammation;
- No fluoxetine, no inflammation.
In contrast to mice who had inflammation, where the MFI serotonin levels doubled, mice who received fluoxetine had extremely low serotonin levels in the MFI, which were “nearly undetectable,” the researchers write.
The researchers did not do the behavioral tests with these mice, but one thing they did discover was that the babies of the first group—whose mothers were mice dosed with fluoxetine who also had inflammation—were unlikely to survive. Many pregnancies were lost after the immune response during pregnancy, and even those born rarely survived long enough to be weaned.
The researchers found that, in mice, the combination of SSRI antidepressants and an immune response during pregnancy was almost always fatal to the fetus.
The researchers note that the biological changes in the MFI were different in each group—meaning that the SSRI had a complex interaction with the inflammatory immune response. Moreover, even without inflammation, they write, “SSRI exposure alone can modulate the expression of genes involved in immune and serotonin signaling at the maternal-fetal interface.”
The researchers write that SSRIs have both pro- and anti-inflammatory properties and so have a complex effect that reinforces some inflammation while dampening other inflammatory responses while possibly leaving some processes untouched.
In conclusion, they write, “Our study suggests that SSRI intake during pregnancy could potentially have lasting consequences on offspring neurobiology.”
However, they add that “SSRI use provides necessary reprieve from detrimental mental health states” (although their study did not provide data on this).
This study comes on the heels of a recent study in rats that found those exposed to the popular antidepressant citalopram (Celexa) in utero had an impaired ability to nurture their children in later life.
In a study from 2016, female mice exposed to fluoxetine (Prozac) in utero also exhibited impaired maternal behavior, while male mice exposed to the same drug in utero exhibited increased aggression.
It is important to note that a study in animals may not always give good information about how a phenomenon manifests in humans. However, mice and rats have long been considered a good proxy for studying biological effects that would be considered unethical in humans.
Additionally, non-randomized studies in humans have consistently found antidepressant use in pregnancy to be associated with myriad risks to neonatal health, including neonatal withdrawal syndrome, preterm birth, congenital disabilities, developmental problems, cardiopulmonary problems, and even death.
In a 2021 study, researchers argued that antidepressants should be discontinued during pregnancy because of the risk of neonatal withdrawal syndrome. They identified symptoms of hypoglycemia, tremors, hypotonia, hypertonia, tachycardia, rapid breathing, and respiratory distress in babies born to mothers who used antidepressants.
Other research has found that antidepressant use during pregnancy alters brain development in the fetus. For example, a study in JAMA Psychiatry found that antidepressant use during pregnancy increased the risk of infants with speech disorders, while a study in the American Journal of Psychiatry found that antidepressant use during pregnancy increased the risk of impaired neurological functioning in infants.
****
Zengeler, K. E., Shapiro, D. A., Bruch, K. R., Lammert, C. R., Ennerfelt, H., & Lukens, J. R. (2023). SSRI treatment modifies the effects of maternal inflammation on in-utero physiology and offspring neurobiology. Brain, Behavior, and Immunity, 108, 80-97. https://doi.org/10.1016/j.bbi.2022.10.024 (Link)