Tag: anti-depressant
Joanna Moncrieff: Psychiatric Drug Mechanisms of Action
We discuss Doctor Moncrieff’s work to address the realities of psychiatric drugs and the groundbreaking RADAR study which focuses on antipsychotic drugs.
Study 329 Taper Phase
Most doctors still affect surprise at the idea SSRIs might come with withdrawal problems. Regulators knew very clearly since 2002 about the problems, but have decided to leave any communication of these issues in company hands.
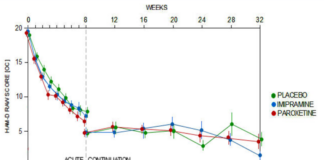
Study 329 Continuation Phase
All the fuss about Study 329 centers on its 8-week acute phase. But this study had a 24-week Continuation Phase that has never been published. Until Now.
Sadness: The Problem and The Solution
There is an ever-narrowing bandwidth of behavior that supports the dominant narrative in our culture today. We all need to act a certain way to protect the foundational beliefs of our time – that “science” has it all figured out, that rules keep us safe, and that it’s us vs. them (insert germs, terrorists, pests, and other “enemies”). But what are the consequences of this? What is this sadness and where does it go if we bandage our consciousness with business, medication, substances, or general avoidance of our real human experience?
Violence Caused by Antidepressants: An Update after Munich
The media is now reporting details about the 18-year-old who shot and killed nine and wounded many others before killing himself on July 22 in Munich. My clinical and forensic experience leads to a distinction among people who murder under the influence of psychiatric drugs. Those who kill only one or two people, or close family members, often have little or no history of mental disturbance and violent tendencies. The drug itself seems like the sole cause of the violent outburst. On the other hand, most of those who commit mass violence while taking psychiatric drugs often have a long history of mental disturbance and sometimes violence. For these people, the mental health system seems to have provoked increasing violence without recognizing the danger.
Who Will Guard the Guardians of Psychiatry?
The assertion that the so-called antidepressants are being over-prescribed implies that there is a correct and appropriate level of prescribing and that depression is a chronic illness (just like diabetes). It has been an integral part of psychiatry's message that although depression might have been triggered by an external event, it is essentially an illness residing within the person's neurochemistry. The issue is not whether people should or shouldn't take pills. The issue is psychiatry pushing these dangerous serotonin-disruptive chemicals on people, under the pretense that they have an illness.
Restoring Study 329: Letter to BMJ
When we set out to restore GSK’s misreported Study 329 of paroxetine for adolescent depression under the RIAT initiative, we had no idea of the magnitude of the task we were undertaking. After almost a year, we were relieved to finally complete a draft and submit it to the BMJ, who had earlier indicated an interest in publishing our restoration. But that was the beginning of another year of peer review that we believed went beyond enhancing our paper and became rather an interrogation of our honesty and integrity. Frankly, we were offended that our work was subject to such checks when papers submitted by pharmaceutical companies with fraud convictions are not.
The Psychiatry Sandcastle Continues to Crumble
Psychiatry would long since have gone the way of phrenology and mesmerism but for the financial support it receives from the pharmaceutical industry. But the truth has a way of trickling out. Here are five recent stories that buck the psychiatry-friendly stance that has characterized the mainstream media for at least the past 50 years.
Study 329: 50 Shades of Gray
Access to data is more important than access to information about conflicts of interest. It is only when there is access to the data that we can see if interests are conflicting and take that into account. Problems don’t get solved unless someone is motivated for some reason. We need the bias that pharmaceutical companies bring to bear in their defense of a product, along with the bias of those who might have been injured by a treatment. Both of these biases can distort the picture but it’s when people with differing points of view agree on what is right in front of their noses that we can begin to have some confidence about what we have.
Study 329 in Japan
By 2002 GlaxoSmithKline had done 3 studies in children who were depressed and described all three to FDA as negative. As an old post on Bob Fiddaman’s blog reproduced here outlines, several years later they undertook another study in children in Japan. (Editor's note: This is a re-print, by David Healy, of a post by Bob Fiddaman)
On the Link Between Psychiatric Drugs and Violence
One of psychiatry's most obvious vulnerabilities is the fact that various so-called antidepressant drugs induce homicidal and suicidal feelings and actions in some people, especially late adolescents and young adults. This fact is not in dispute, but psychiatry routinely downplays the risk, and insists that the benefits of these drugs outweigh any risks of actual violence that might exist.
Study 329: The Data Wars Cross the Rubicon
It can be difficult to pinpoint transitions. The Rubicon that led from a Medical Republic to a Pharmaceutical Empire was crossed in 1962 with the passage of the Amendments to the Food and Drugs Act. This act put in place an apparatus of controlled trials, prescription-only status and disease indications that laid the basis for a global pharmaceutical hegemony, although the drift to Empire could still have been stopped at this point.
Study 329: MK, HK, SK and GSK
It is appropriate to hold a company or doctors who may be aiming to make money out of vulnerable people to a high standard when it comes to efficacy, but for those interested to advance the treatment of patients with any medical condition it is not appropriate to deny the likely existence of harms on the basis of a failure to reach a significance threshold that the very process of conducting an RCT will mean cannot be met, as investigators' attention is systematically diverted elsewhere.
Psychiatry’s Thalidomide Moment
The authors of Study 329 began recruiting adolescents for a comparative study of Paxil, imipramine and placebo in 1994 and finished their investigations in 1997. They dropped a large number of their original cohort, so the randomness element in the study must be open to question. Late in 1998, SmithKline Beecham, the marketers of Paxil, acknowledged in an internal document that the study had shown that Paxil didn’t work for adolescents in terms of the two primary and six secondary outcomes they had established at the start of the study. In a nutshell, Study 329 was negative for efficacy and positive for harm, contrary to their succinct upbeat conclusion.
The Troubled Life of Study 329: Consequences of Failure to Retract
If someone were to ask the surviving authors of Study 329 the question: “Knowing what you know now, if you had to do it over, would you agree to participate in that study again?”, many would probably say no. Study 329’s problems started to surface right after it was published. Several doctors wrote letters to the JAACAP Editor with probing questions, mostly centred on the psychiatric side effects of paroxetine, and the measures used to claim its efficacy in treating adolescents. The authors responded and the questioners did not pursue their concerns further. Except one.
Next week, fourteen years and two months after it was published, it is about to take yet another hit, when the Restored version is published.
Study 329: The Timelines
In addition to hosting the Panorama programs and The Famous Grouse history of Study 329, Study329.org has a comprehensive timeline on the origins of concerns about the SSRIs and the risk of suicide, initially with Prozac and subsequently with Paxil/Seroxat. The hope is to provide a comprehensive repository for anyone who wants to study SSRIs, RCTs, and Study 329 in particular.
Psych Meds Put 49 Million Americans at Risk for Cancer
With 1 in 5 Americans taking a psychiatric medication, most of whom, long term, we should probably start to learn a bit more about them. In fact, it would have been in the service of true informed consent to have investigated long-term risks before the deluge of these meds seized our population over the past thirty years.
A Reply to Peter Kramer: Do Serotonin Imbalances Cause Depression?
A recent article on the website i09 titled, ‘The Most popular Antidepressants are Based on an Outdated Theory” has again raised the issue of Chemical Imbalances. It is interesting that the author of the i09 piece cites Dr. Peter Kramer and states, “Some psychiatrists vehemently disagree with the way journalists and other psychiatrists have pushed back against the chemical imbalance theory….” In both cases he cited what he considered the best evidence in support of the theory, but he did not discuss the research in any depth. Back in 2008, we took an in-depth look at the evidence that Dr. Kramer used to support the chemical imbalance theory. When one takes a closer look at that research we do not think it supports the theory. For this reason, we are reposting our 2008 essay about this.
A Story About NMDA Receptor Subunits, and Why SSRIs Impair Cognitive...
The impact of long-term SSRIs on memory-related nerve cell receptors does have functional consequences. Research shows that SSRIs impair the acquisition of fear memories. (Perhaps a positive outcome.) But unlearning fear memories involves new learning as well, and according to a study by LeDoux and colleagues, long-term exposure to SSRIs makes it harder to unlearn fear memories.
Pilots Crashing on Antidepressants: A (Not So) Brief History
With the current focus on the possible contribution of psychoactive drugs to the crash of GermanWings flight A320 on Tuesday, March 24, it is useful to identify potential links between the effect of the antidepressants and the events. In all 47 cases listed on SSRIstories, the pilots were taking antidepressant medications, mostly SSRIs, often in combination with other medications and sometimes with alcohol.
Winging it: Antidepressants and Plane Crashes
The crash last week of the Germanwings plane has shocked many. In view of the apparent mental health record of the co-pilot Andreas Lubitz, questions have been asked about the screening policies of airlines. The focus has generally been on the conditions pilots may have or the arguments they might be having with partners or other situational factors that might make them unstable. Even when the issue of the medication a pilot may be taking is raised, it is in the context of policies that permit pilots to continue on drugs like antidepressants to ensure any underlying conditions are effectively treated. But fewer treatments in medicine are effective in this sense than people might think and even when effective they come with effects that need to be balanced against the likely effects of the underlying condition.
Things Your Doctor Should Tell You About Antidepressants
The conventional wisdom is that antidepressant medications are effective and safe. However, the scientific literature shows that the conventional wisdom is flawed. While all prescription medications have side effects, antidepressant medications appear to do more harm than good as treatments for depression.