A recent study published in this month’s issue of Psychiatry Research attempted to examine the impact of an anti-stigma public media campaign in Germany. They focused on changes in public attitudes toward people affected by symptoms associated with depression and schizophrenia as a result of the psychenet- Hamburg Network Mental Health awareness campaign.
“Overall, this study showed that the information and awareness campaign had almost no significant effects on the general public’s attitudes toward people affected by either schizophrenia or depression,” the researchers, led by German medical sociologist Anna Makowski, wrote. “One could assume that deeply rooted convictions cannot be modified by rather time-limited and general activities targeted at the public.”
 The researchers recognize that stigma against people who have been diagnosed with mental disorders “is a prevalent phenomenon which imposes a high burden on those affected.” Past studies have found that negative attitudes and social rejection of those with mental health problems have remained stable over the past several decades, primarily fueled by a lack of knowledge about possible causes, treatments, and a lack of personal contact with people who are openly struggling with these issues.
The researchers recognize that stigma against people who have been diagnosed with mental disorders “is a prevalent phenomenon which imposes a high burden on those affected.” Past studies have found that negative attitudes and social rejection of those with mental health problems have remained stable over the past several decades, primarily fueled by a lack of knowledge about possible causes, treatments, and a lack of personal contact with people who are openly struggling with these issues.
Stigma is defined in this study as the “co-occurrence of labeling, stereotyping, separating and discrimination,” and the researchers make use of measures of social distancing to quantify these attitudes. The reluctance to engage with those diagnosed with mental disorders has been tied to older age, lower levels of education, and “biogenetic causal attributions such as somatic or hereditary factors.”
According to a study published just last month in the British Journal of Psychiatry, the biomedical model of mental illness, prevalent in industrial societies, “results in stigmatization and rejection from the outside, and self-attribution and self-blame from the inside.” In November, a large-scale international survey of attitudes about mental health also found that biological explanations of mental disorders had negative effects on public attitudes. The survey found that people in developed countries are more likely to assume that ‘mental illnesses’ are similar to physical illnesses and biological or genetic in origin, but they are also much less likely to think that individuals can overcome these challenges and make a full recovery. (See MIA’s coverage of these studies here and here, respectively)
Social distancing and stigma can severely exacerbate the circumstances of those suffering. Consequences ranging from a lack of employment opportunities to a lack of community inclusion block avenues to recovery and make it more likely that people will suffer over the long term.
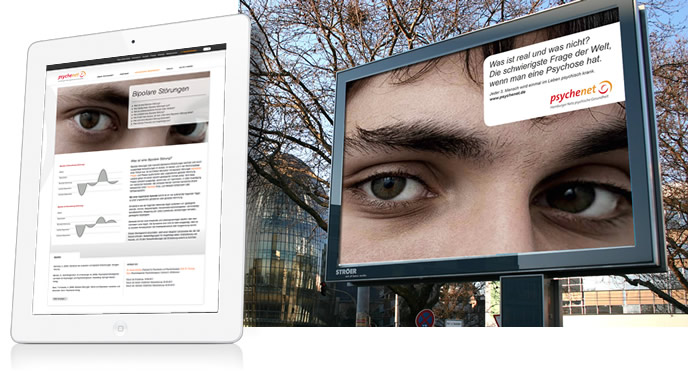
In the present study, researchers investigated a recent campaign aimed to increase information and awareness of mental health issues from 2011 to 2014 in Hamburg, Germany. The psychenet media campaign, as it was called, developed a website, print advertising, and short movies that were shown in cinemas about 40,000 times over the three-year period.
“In the movies, patients with mental illness served as actors,” the researchers explain. “They shared their genuine and very personal stories with the aim to achieve awareness, encourage sensitivity and break down prejudices to- ward those affected by mental illness and their relatives.”
The researchers evaluated how the psychenet media campaign affected desire for social distance and emotional reactions toward people who have been diagnosed with depression and schizophrenia. They found that only 7.3% of the respondents were familiar with the campaign. While those who were familiar did show lower levels of desire for social distance, these results did not reach statistical significance.
“It can be expected that such attitudes are primarily affected by political, social and economic circumstances. Furthermore, this is backed up by the way mental disorders and patients are represented in the media and how the public debates on mental illness proceed,” the researchers wrote in their concluding statements.
“Tailored measures that target specific groups seem better suited compared to broad-based interventions such as the psychenet campaign.”
*
Makowski, A.C., et al., Changes in beliefs and attitudes toward people with depression and schizophrenia – results of a public campaign in Germany. Psychiatry Research (2016), http://dx.doi.org/10.1016/j.psychres.2016.01.029i















The only “stigma” of mental illness is the one they create to push pills.
Your brain is broken, you need drugs.
My brain is broken ? Can I get a test using medical science to prove that ?
Report comment
If it were broken, a neuropsychological interview would provide you with hints as to where (as a patient, you may have experienced the beginnings of one where they asked you simple bio stuff plus (of course) the identity of the President and other such hot items).
If it were merely bent, quantitative tests (NOT personality tests) like the Hoffer-Osmond Diagnostic(HOD) or the Experiential World Inventory could give you a good idea. I have a HOD, which I use to check myself should I suddenly find myself getting strange.
Report comment
You wouldn’t have to worry about stigma if you had effective treatments for serious mental illnesses. At present, you have two schools: the pseudo medical, which creates the Zombies, and with new anti-psychotic drugs, that Fat People; and secondly, the social influence, which leads to long periods of convalescence from repeated flare-ups of symptoms- great for romantic novels, but exceedingly poor for maintaining a steady work record. Neither of these is particularly helpful at reducing the stigma of impaired “personhood”.
Report comment
Where is your data for the “social influence
leading to “long periods of convalescence” and “being
poor for maintaining a steady work record”. This is nonsense… intensive psychotherapy and family approaches have helped many/most people who engage in them return to productive engagement with work and school. Take a look at Open Dialogue, the 388 program, RAISE, PREP, EASA, the metaanalyses by Knekt and Leichsenring and Gottdiener on long-term psychotherapy.
Report comment
The answers are easy, but oh so difficult:
– Stop diagnosing people.
– Stop conceptualizing of life problems as illnesses.
– Stop denying the effects of poverty, inequality, abuse, neglect, trauma on our fellow human beings.
– Do unto others as we would have them do unto us.
This stigma campaign was doomed because it’s medical model lite, it still labels the people as having mental illnesses (at least I assume that). Therefore people will still view them as “other” as fundamentally different or broken.
What people need to accept is that anyone can become depressed or psychotic given enough stress. Depressed and psychotic people are not fundamentally different in their potentials and capacities than the rest of us.
Report comment
You have got the real ad campaign down! Let’s make some videos!
Report comment
I agree we should make some videos. I hear that is what MIA is going to start doing this year! Then one of us should win the lottery and fund a super PAC to get all my points above advertised on TV and radio hourly.
Report comment
Stigma comes only from the labels that the psychiatrists give the patients – if the doctors simply addressed the specific symptoms of the patients (worked on the symptoms to alleviate them using various interventions), there cannot be any stigma. It seems for all categories of DSM diagnoses, symptoms listed in their criterion sets are normally distributed in the general population (see: http://www.ncbi.nlm.nih.gov/pubmed/17716032).
Report comment
Nancy, this looks like a very interesting paper. Have you read the full version? If so, can you please contact me? I’m at bpdtransformation (at) gmail (dot) com
Edward
Report comment
As anyone with half a brain, or perhaps half a heart, would know, stigmatization results from grouping people as “different” from the mainstream. That energy of “differentness” comes directly from the mental health industry, which is profiting from convincing everyone that they need “treatment” for the emotional experiences that come with being alive.
A real anti-stigma campaign would not say, “You shouldn’t be prejudiced against these people just because their brains are fucked up.” It should be saying, “There is nothing different about the ‘mentally ill’. These folks are just the same as you. Many of them have had tough lives and have had to fight to survive. Love and care about each other and ‘mental illnesses’ will drift away.” In fact, even identifying “them” as people with “mental illnesses” is still stigmatizing! How about, “All of us suffer from the struggles of life sometimes. Anxiety, depression, anger, and hopelessness are all a normal part of life’s many challenges. Help each other when you see someone else is struggling – tomorrow it may be you who needs their support!”
So much of the “stigma” is caused by the system itself, it just makes me gag every time they develop a new “anti-stigma” campaign that just rubs more salt in the wound. It makes as much sense as saying, “Don’t be prejudiced against Spanish-speakers, even though they aren’t really Americans.” It would be better for them to say nothing than to explain why “mental illness” is just like physical illness, and you shouldn’t be prejudiced against people just because their brains don’t work right.
—- Steve
Report comment
Don’t be prejudiced against those dangerous nut jobs! They aren’t truly dangerous as long as we keep them properly drugged!
This provides the useful function of stereotyping us as a bunch of rampaging mad dogs. But, not to worry, they have a wide assortment of safe and effective muzzles!
Still, who wants to be around a rabid dog even if it is wearing a muzzle? Thanks for nothing, mental illness experts.
I only wish I had the choice between wearing a muzzle and letting them rape my poor brain.
Report comment
I think the problem is…addressing the real causes of “mental illness” on a large scale would mean admitting that 21st century societies tend to be sick, and that these sick societies create sick people. It would also mean looking at family dynamics after decades of NAMI-style dogma that absolves all families of any responsibility for the “mental illness” of its members.
Blaming the brain, pushing pills…its not just that psychiatry is now ideologically dedicated to somatic treatments. Society as a whole, right now, seems interested in maintaining the illusion that society is a-OK and those who fail to function as expected are “losers,” unless of course they have a label, in which case they are subject to the “cruel compassion” of being a mental defective.
I think this may explain why many European countries and the UK are more willing to try psychosocial treatments and at least allow people to discuss different ways of understanding and approaching “mental illness.” I think the great myths of American culture–anyone can succeed, pick yourself up by your bootstraps, “personal accountability,” etc.–when combined, create an unwillingness to reflect upon the world around us.
Report comment
You speak wisely. Psychiatry has thrived here partly because of our unwillingness to allow that our culture is flawed and damaging to its members in many small and large ways. It’s much easier for those in power to blame the victims of an unfair or oppressive system rather than trying to listen and change it, and unfortunately, psychiatry’s need for power and funding plays right into the hands of those inclined to that kind of thinking.
Report comment