New research finds that patients in public healthcare settings find relationally oriented treatments, such as psychodynamic psychotherapy, helpful to them in a variety of ways. Clinician-researchers led by Dr. Hannah Richardson from the Cambridge Health Alliance, a public medical system associated with Harvard Medical School, recently published results from their study in The Journal of Mental Health Training, Education, and Practice to understand what patients receiving psychodynamic psychotherapy found helpful in their treatment.
While they found that most patients thought their treatment was helpful, they often mentioned their therapist as an essential element of helpful treatment. Such findings highlight the value of interpersonal connections as a part of treatment and that patients outside the traditional psychotherapy practice setting value treatments that focus on this connection (i.e., psychodynamic therapy). The authors reviewed some of the current research on patients’ perspectives of good therapy, noting that they are not very common and that:
“Although interventions such as single-session therapy may rely less on the therapeutic relationship, it is unclear whether they can be helpful to patients with complex problems… The therapeutic relationship emerges repeatedly in the literature as helpful regardless of the study design or population. Other factors perceived as helpful by patients across modalities include personal contact, awareness/ insight/understanding, behavioral change/problem solution, empowerment, exploring feelings/emotional experiencing, relief, feeling understood, patient involvement, reassurance/support/safety, and ‘voicing.’”
 The authors wanted to understand what patients found helpful in psychodynamic psychotherapy, which hasn’t received much attention in patient-centered research. They also wanted to understand whether patients’ reporting of what they found helpful in psychodynamic psychotherapy changed with 100 patients three months into treatment and 88 patients after ending therapy.
The authors wanted to understand what patients found helpful in psychodynamic psychotherapy, which hasn’t received much attention in patient-centered research. They also wanted to understand whether patients’ reporting of what they found helpful in psychodynamic psychotherapy changed with 100 patients three months into treatment and 88 patients after ending therapy.
Patients who agreed to receive follow-up questionnaires from the researchers were asked one open-ended question about what they found most helpful about the treatment they received at the clinic, along with the patients’ numerical rating of how beneficial the therapy had been. Patients in the study had an average length of therapy of 10.5 months or approximately 44 mostly weekly sessions. In addition to receiving psychodynamic psychotherapy, about half of the patients also reported receiving psychiatric medication as part of their treatment.
The authors analyzed patients’ feedback on their treatment experiences by categorizing and organizing their responses into themes based on perceived patterns while prioritizing code development that emphasized inter-rater agreement and consistency among researchers. From these initial analyses of responses from patients three months into treatment, the authors created a codebook of 16 categories to deductively code patients’ responses after completing treatment. This led to the analysis of the themes that connected the codes.
From this analysis, the authors found that the most common codes found in patients’ responses of what they found therapeutic in treatment were having someone to talk to, having structure in treatment (a consistent and frequent therapeutic ‘frame’), and symptom relief/improved functioning.
 Patients, whether they had explicitly mentioned it or not, had identified the therapist’s presence as important to what they found helpful about treatment, indicating that what is considered therapeutic by patients happens in the context of a relationship with the therapist. It was even observed that categories related to the therapy relationship increased at the end of therapy, indicating that therapists become more critical to patients’ views of what is therapeutic as treatment progresses.
Patients, whether they had explicitly mentioned it or not, had identified the therapist’s presence as important to what they found helpful about treatment, indicating that what is considered therapeutic by patients happens in the context of a relationship with the therapist. It was even observed that categories related to the therapy relationship increased at the end of therapy, indicating that therapists become more critical to patients’ views of what is therapeutic as treatment progresses.
The authors also identified four categories representing different levels of insight expressed by patients. From the first level, describing “venting/ranting” as therapeutic, then “talking/someone to talk with,” followed by therapy “directing attention at experience,” culminating with “insight” as being identified as therapeutic. The authors note the following results:
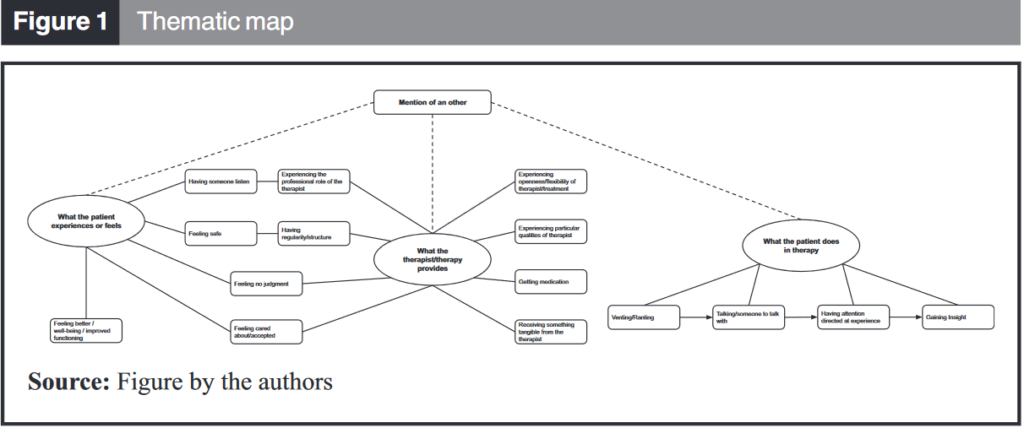
“We identified three themes that emerged from our coded data: The first theme, what the patient experiences or feels, incorporates categories such as improved functioning, feeling safe, and feeling cared about. Many of the categories within this theme connect with the different perspectives captured by the second theme, what the therapist/therapy provides. The third theme, what the patient does in therapy, incorporates the four levels of insight described above. All three themes have “mention of an other” embedded within them. The three themes can be thought of as giving different views or perspectives on the therapy process.”
Focusing on inter-rater reliability between researchers and quantifying patient responses, a positivist perspective in qualitative research may be perpetuated, which prioritizes statistical power in the results to make inferences about population variations from sample observations. This approach may lead to the assumption that the most common responses represent validity without fully embracing the researchers’ interpretations.
By implementing such reductions, the methodological integrity of the findings could potentially be compromised, overlooking the invaluable perspective provided by qualitative research, which can lead to a comprehensive and contextually grounded understanding of patients’ experiences in psychodynamic therapy.
Psychodynamic psychotherapy is a depth-oriented, emotion-focused, and relational approach to mental health treatment that goes beyond symptom reduction, prioritizing building self-understanding and fulfilling interpersonal relationships. It has often been marginalized in favor of approaches such as cognitive behavioral therapies (CBT), despite continued research in that psychodynamic therapies show strong evidence for their efficacy in treating common mental disorders, such as depression, anxiety, personality, and somatic disorders, as well as bipolar and trauma disorders in LGBTQ patients.
This research shows that psychodynamic therapies are often equivalent to CBT, challenging the notion that CBT is the gold standard treatment approach to be used across the board. Some research suggests that psychodynamic therapy is more effective at improving reflective functioning in some patients with borderline personality disorder than CBTs, and when integrated with CBT, it can improve therapy outcomes.
As psychodynamic therapy continues to gain attention in the mental health field, the research of Richardson and colleagues is innovative in focusing on patients’ perspectives on the elements of treatment that are therapeutic. Combined with the naturalistic setting of a public mental health clinic, this research also emphasizes the applicability of such therapeutic approaches to often-underserved populations.
While it is helpful to know more about what patients find helpful in therapy, future research directions include understanding more about what patients say is unhelpful in their treatment. Nonetheless, these study findings demonstrate the need for healthcare organizations to value the therapeutic relationship as a central component of treatment, as well as focus on outcomes beyond symptom reduction.
****
Richardson, H., Ernst, J., Drill, R., Gill, A., Hunnicutt, P., Silver, Z., Coger, M., & Beinashowitz, J. (2023). In the patient’s own words: A qualitative study of what patients find helpful in psychodynamic psychotherapy. The Journal of Mental Health Training, Education and Practice. https://doi.org/10.1108/JMHTEP-06-2022-0041















As someone who has been harmed by therapy and blamed myself for many, many years, I believe that finding what is unhelpful (to harmful) in therapy deserves more than a brief mention.
People have been researching what is helpful to a statistically significant number of participants for years, while the harms have been ignored. The “relationship” in psychodynamic therapy is a particular risk for many clients who have a background of relational trauma and find it hard to recognize when the therapy isn’t working or is indeed bad for them. I know this from my own experience and from qualitative observations in online support forums. There is some research on harmful therapy but I’m nor sure it would be helpful to list studies here. Nevertheless, what is “helpful” about therapy without attempting to qualify what may be harmful is dangerous to some clients. I am one of them.
Report comment
‘The “relationship” in psychodynamic therapy is a particular risk for many clients who have a background of relational trauma and find it hard to recognize when the therapy isn’t working or is indeed bad for them.’ That is an insightfull really good point. And an understatement…
There is a theater play by Sabina Berman, as beautifull as Bergman, I don’t think has been translated, based on the case of Dora, treated by Mr. Freud that gives historical context to your narrative.
Saddly, I never got to see the play. Probably I never will, but I got the book!. At less than 1 dollar per page, or was it a peso?. New, not secondhand.
Oddly, the theater play, humm, was promoted as a “mistake” by Mr. Freud. But to me, it was typical fraudian…
There are several cases where abuse was continued and Fraudulently justified by the father of psychoanalysis.
So, psychodynamics keeps giving, and not in a good way…
Report comment
We really need to stop the naval-gazing and the repeated talking points like, “They often mentioned their therapist as an essential element of helpful treatment.” By saying this, the perspective is from the therapists, not from the clients or patients of the past. It is not the therapist that essential to the healing; it is the client’s internal workings. If it were the therapist, then why do we need so many therapists with different methods? Why can’t we train based on the research? What makes a good therapist? These are narratives that have been repeated since Freud, which no one challenges, and they are what keeps clients in therapy for a ridiculous amount of time and money.
So, what’s my concern? What may help people heal? It’s accepting that they are like everyone else because trauma is a unique experience that increases our uniqueness, and this is the major difference. Clients find that they are different from their therapists and no longer agree with them (even a bad therapist may help sometimes), which is a process of human development that is often overlooked and undermined — individuation and differentiation by Margaret Mahler. Even long-term relationships go through this phase after they pass and survive the power struggle phase. One realizes that they are both like everybody else and different from everybody else. This is an internal process that has nothing to do with the therapist person per se (or directly), who should be an instrumental tool, not central to anyone’s recovery. Making the therapist central to recovery is like making a psychiatry to human healing!
The reason for the saying “The therapist is essential to recovery” is that, similar to religion and internalizing Jesus or God or any deity, the process of therapy involves internalizing the therapist and this is where a lot of people struggle because it is not explained appropriately in the consent informing process. IMHO, this is the biggest scam ever perpetuated in modern society. Internalizing an adult whom you know nothing about is what causes and perpetuates madness, much like believing in God or a deity or a fascist!
Therapy acts very similar in the making of trauma – such as having a person observe you, interpret your experience by validating or sometimes correcting, and molding one’s thoughts without you, the client, not doing the same; and they have the audacity to say they are essential. A heart surgeon can heal you on the table but if you do not change your life, you will be back on the table!
A therapist is an instrument to healing but not to essential!
Report comment
Like really folks. There is a reason you have to work so hard to sell the concept of paying to be mostly pleasant for $200 at least once a week for years AND that there a people desperate enough to do it.
Just seeing all of these positive psychotherapy research hot takes by psychology grad students about banal study results as if they are powerful, persuasive, or newsworthy is redic.
No, psychotherapy is not liberationist because no society of free people with their needs met would have much use for the clinic, either as patient or therapist. Psychodynamic therapy actually serves to limit the imagination of people who know things need to change to only focus on themselves.
Lonely people would not be appreciative of exploitative encounter with a one-sided paid professional if their lives had room for genuine community and the ability and time to nurture relationships.
I don’t trust therapists to do meaningful research or reporting on harms of psychotherapy and find their exaltations of anything positive to show as simply self-justifying.
Psychotherapy isn’t exempt from the problems of Psychiatry because it doesn’t come in pill form. It is still plenty rife for abuse and long-term harm. All of the research and training spent to justify and liscene new therapy and therapists is better spent making people’s lives both materially less precarious and emotionally enriching by not training/coercing/policing affect states as a requirement to access basic need of lice. We don’t need private confidants to help us understand the horrendous nonsense we are forced to learn in order to live in a bad society to just continue to live in it. we need a decent society so that we don’t require or teach that nonsense in the first place.
Report comment
That’s so beautifully eloquently put.
Report comment
Agree 100%. Goddamn stupid “study” from a goddamn stupid “profession”.
Report comment
Nathan speaks THE TRUTH.
Report comment
Research on therapy tends towards large-scale study designs, which is quite limited, I think. Naturally, every person experiencing therapy is significantly distinct from all other such persons; The effectiveness of therapy is defined by the interaction of that person’s particularities and the therapy. However, group studies tend to smooth over such distinctions to reach general conclusions, meaning they are of little use in studying those interactions. Studies that focus on individuals are also needed to properly inform clinical practice. I would also second Mella’s thoughts on the need to study potential harms.
Report comment
But unfortunately such fine grained empirical, let alone scientifical testing grounds are not achievable without knowing how the thing of therapy works. Enough to come with specific individually testable hypothesis.
That was the flaw and allure of psychoanalysis and psychodynamics:
Claim benefit to the client, patient, individual, individually based, he/she said so itself!: I feel better now.
Regardless of the impracticability, even impossibility of testing it in the aggregate and the specific individual.
Not unlike the horoscope: it can get so fined grained mathematically and astronomically, and yet, it lacks causality.
Report comment
Well psychoanalysis, and its psychodynamics alternate ego, it’s doppelganger conjoint twin brother, was even recognized by Lacan, both a psychoanalyst and a top dog of 20th century epistemics as PSEUDOSCIENTIFIC.
In the sense, interpolating, that black box inferences about the inner workings of the black box, the human mind, were and still are scientifically untestable. Let alone by or with the circular reasoning impervious to criticism of psychodynamics.
And I would not be caught trying pseudoscientific therapies, treatments, remedies, let alone desperate ones.
The scientific ones are already on the aggregate already poor and expensive enough.
Suit yourselves believers, beware that it has not really improved much, as psychiatry hasn’t in over 100yrs. Not really tried and tested though.
Report comment
It’s asinine “research” like this that make me wonder why I bother with MIA at all, as sometimes it seems like one masturbatory propaganda piece after another for the “mental health” industry. AND WHO IN THIS WORLD needs a “study” to tell them that people feel better after talking with someone???
Report comment
I know, it’s like when they “discover” that hiking in the woods makes people feel calmer, and instead of saying, “hey, try hiking!” they decide to call it “Nature Therapy!”
Report comment
Glad you agree. The whole “mental health” racket is nothing but a bunch of intellectual flatulence.
Report comment
…and after calling it “Nature Therapy” they then charge people a hefty fee!!!
Report comment
Exactly! They hire “nature therapists” and pay them to go hiking with you!
Report comment
Fucking unbelievable. Especially when the best part of being in nature is BEING ALONE in nature.
Report comment
Bird watching therapy.
Watching birds fly has a positive affect effect too, and somewhat strong IIRC.
Report comment
True! You should get funding for a study!
I used to go to the hummingbird house at the Philadelphia Zoo during the week when nobody was there. I would sit for 10 minutes making no noise, and soon I was surrounded by birds doing their thing. It was very soothing, and I didn’t need someone to tell me it “worked!”
Report comment
Well…
I did used to be tacken to the zoo often enough. Just, after my young age realization that elephants were forced to “do” performances, it lost it’s charms. Young elephants too.
Guess which one was my favorite animal back then?.
Decades past for me to go, with open heart…
But, for birds. seen a peruvian Condor, I think, fly in a large cage, small for “it”, was devastating… double reason not to go again, back then. I could see some “squaring” on it’s flight, like, weird, like seeing a bird videogame, on early 80s graphics.
Still, I can see eagles fly now, sometimes, here!, in my current home town!. And some peregrin falcons, whom deceived me: I thought they were the same!.
Nope, each one was unique and different, they were just migrating. Different spots, expectations.
🙂
Silly me, I thought they were pets!. So, assumed, all nearby.
And even a crazy eagle crapped the bejeezus out of me!, trying to catch something on the ground: like zzzsut!, a shadow went to the ground.
And one was just perching, there, in the accros fence!, like our national symbol, just no snake in beak.
So, yeah, it does have a positive effect on me. Rare as it might be.
🙂
Report comment
The hummingbird house was a new experiment at the time with an open environment rather than cages. It felt like they were pretty good with the environment or it would not have felt good to be there. I felt like I was in their world.
Report comment
I wonder if at some point swinger therapy will be a thing?.
hahaha…
Report comment
Haven’t even read the article but I just felt like commenting on this theme, research has shown since the 1950’s that the only predictor of therapeutic success is the relationship and it has nothing to do with the technology. So any therapeutic approach that promotes its technology as the reason for any success it has is deluding itself.
Report comment
Psychodynamics has to theoretical, scientific basis.
And it is not fasifiable, meaning it is not empirical, and no experiments can prove it has any grip on reality.
And therefore no claim it has beneffits is a valid one: experiments can’t prove that, can’t disprove that, and lacking theory, as beyond doubt, not one single experiment can be done to prove it. It is unfalsifiable.
There being no theory, no generalizable empirically predictable facts beyond doubt on relationships, ANY CLAIMS OF therapist to client/patient relationships are as pseudoscientific as psychoanalysis/psychodymanics.
It’s just moving the flag post from whatever that was, to I am better!, I have better relationships with my clients!, yipeee!.
Where is the causality on that to do experiments to test the theory, the methodology and the hypothesis that any therapists is better than average?.
And on averages: half the people are below average, and half above. And the aggregate, the sum of all participants in the psychodynamic market can’t do NEITHER BETTER NOR WORSE, than average.
By, maths and definitions.
Report comment
Unfalsifiable hypotheses, incorrectly called theories are zombie theories:
They refuse to go away, and always, a positive study can give them new life.
Disproving them are outside science, since no mechanism is sure, beyond doubt to exist, that allows them to be tested scientifically. No positive or negative finding can prove them right or wrong.
Just like love, God, the Holly spirit, angels and demons, and Faith: they are outside science, and therefore outside experiments.
Simple first half 20th century epistemics.
And that is something even skeptics, sometimes/most of the times won’t admit: experiments can’t disprove the paranormal. For that, they would have to have a theory for the paranormal. (!?)
Which explains why I felt an unwelcomed skeptic in skeptic communities.
I had an otherwise unacknowledged, really, over the early telecomunications web back at the end of the 90s with a top one, a really top one. Whom I had, and still do much respect and appreciation for.
But he targeted me when the psychiatric/victims of psychiatry were targeting me, and apparently, that passed as me doing “magical” therapy.
Nope, I was trying for “them” to leave me alone. It sounds weird, it was weird, but it ended with a: “You are harrasing me!”, from me, in public, but he did not know that. That bad it was.
Guess, what this top skeptic asked me if I was going to do?.
If I was going to sue him. Yep, instead of asking for an apology, he asked me if I was going to sue him. Despite I was a victim of harrasement who had to do a very public scandal…
Saddly, he relatively recently passed away, after apparently stopping fighting against the paranormal. Like he lost the prize to keep fighting. But, still, I do respect and appreciate his work, not his charge against me, although it was and is understandable for me. Just, innapropiate, and probably back then illegal.*
🙂
Muahahahaha!. Black cape, bunny sign to me forehead!. You can’t touch me!. Zizzling cat sounds…
*True story. I never wrote or spoke about it with anyone. Guess where the witness of that!, worked at some point?. A major tech company in the US, before it became the behemot now is. True story. As far as I can tell, except, we shared an interest in deceiving for fun, his outlasted mine. And no, I don’t believe in the paranormal, I am a skeptic, but I can see, there are limits, unlike him…
Report comment