Informed Consent for Benzodiazepines: A Personal Account
I began to have transient moments where I would feel oddly disconnected from my environment or wake up and feel like I was coming out of my skin. I did not know it at the time, but I was experiencing interdose benzodiazepine withdrawal and it would end up leading me down a path of polypharmacy.
Benzos Increase Risk of Fractures
A meta-analysis of all relevant studies on MEDLINE, EMBASE, OVID and ScienceDirect published through January 2013 finds that the use of benzodiazepines, especially short-acting,...
A Rorschach Test for Psych Drugs
On October 23, the New York Times ran a very nice feature story about a Los Angeles woman, Keris Myrick, who, even though she...
Nonclinical Factors are Associated with Long-Term Benzodiazepine Use in Older Adults
White race and size of initial prescription, along with poor sleep quality, are associated with long-term benzodiazepine use in older adults.
Psychologist Rethinks Psychotropic Medications, Calls for Renewed Dialogue
Psychologist and Professor Amber Gum has published the story of her personal journey of rethinking psychotropic medication in a special issue on "The Politics of Mental Health" in The Journal of Medicine and the Person. Influenced by Mad in America and the work of Robert Whitaker, Gum became aware of evidence that “suggests that psychotropic medications are less effective and more harmful than most believe” and now hopes to encourage other mental health professionals and researchers to engage in open-minded, critical self-assessment of standard practices.
Culturally Numb
Experiencing emotional pain is a necessary part of life. Emotional pain often contains valuable lessons to help us on our journeys. We need to make sure we are not numbing our hearts to those that are hurting. We need to de-stigmatize the struggles, joys and pains that come with being human. We need to not just mindlessly pursue happiness - though we might think of that as an inalienable right - and avoid pain. We need to do the only thing that brings true joy: embrace all of life and each other, as we experience together all that makes us human.
Benzodiazepine Use Linked to Dementia and Memory Loss
A recent review of the research found that benzodiazepine use may have long-term effects on memory and increase the risk for dementia. The study,...
More on Benzos and Cognitive Damage
There is mounting evidence that benzodiazepines are causing Alzheimer's Disease. I cannot imagine any genuine medical specialty ignoring or downplaying information of this sort. But psychiatry, with the perennial defensiveness of those with something to hide, promotes the idea that they are safe when used for short periods, knowing full well that a huge percentage of users become "hooked" after a week or two, and stay on the drugs indefinitely.
We Have Seen the Evidence Base, and it is Us
Anyone who has used benzodiazepines and sleeping pills knows how difficult it is to get off them (worse than heroin!) and how much time it takes to recover. Although there is a lot more helpful information on the web these days, a lot of it is based on anecdotal accounts, personal stories and theories rather than “real” evidence.
Announcing an International Symposium and Institute on Psychiatric Drug Risks and Withdrawal
I have given up on psychiatry as a system capable of “being there” for people who are dealing with life and death issues. Psychiatry as a system of care lacks validity. Every day — unfortunately — we learn of new examples proving this statement. But here's the good news: every day we meet people who show us that the predictions of psychiatry are not true; that there are “cures,” that it is possible to reduce or withdraw psychiatric drugs.
Differentiation of SSRI and Benzo Dependence/Withdrawal “Not Rational”
Researchers from the Cochrane Center and University of Copenhagen in Denmark, publishing in the May issue of Addiction, "explore the rationale for claiming that...
Benzo Drugs, UK Fudge, Cover Up and Consequences
In 1980, the British Medical Journal published a “Systematic Review of the Benzodiazepines” by the Committee on the Review of Medicines. The committee denied the addictive potential of Benzodiazepines and limited their suggestions to short term use. The results have been devastating.
The Rotted Fruit
In the law if one falsehood is uncovered in sworn testimony, all of the statements made and the actions that follow are suspect. If...
Benzodiazepine Use and Risk of Alzheimer’s Disease
If a person in mid-life is feeling anxious, or depressed, or can't sleep? No problem. No need to figure out the source of these concerns. No need to work towards solutions in the old time-honored way of our ancestors. Today, psychiatrists have pills. Pop a benzo! And by the way, you'll have a 40% increased risk of Alzheimer's Disease in your late sixties.
Cracked Open – Installment 3
I’ve been working steadily on Cracked Open, a book that chronicles my experience being a mother suffering terrible insomnia to a mother desperately dependent on benzodiazepines. I am not alone. I live in a state that ranks at the top for anti-depressant and anti-anxiety meds and we love to give them to women. But I’m not writing this book simply for mothers or for women. I’m writing it for anyone who has gone into a doctor’s office, desperate and sick, and come out with a prescription that led them down a path to illness and/or disability. It happens so often.
Hypnotic Medications Linked to Suicide Risk
A recent review found that hypnotic medications are associated with risks of suicide and suicidal ideation.
Long-Term Benzos Worsen Anxiety
Long-term use of benzodiazepines for anxiety remains a widespread, despite guidelines that recommend against it, according to a roundtable discussion at the annual conference of...
Slew of New Studies Spot Links Between Psychiatric Medications and Bone Loss, Fractures
Four different studies conducted in different ways examining different groups have linked use of certain psychiatric drugs to bone fracture risks and negative impacts on human bone development.
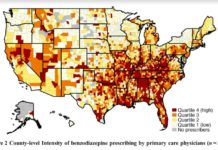
Benzodiazepine Prescriptions in Older Adults Used in Rural and Low Income Areas
Benzodiazepine prescription practices may be in response to an epidemic of distress, rather than being used to treat specific mental health diagnoses.
Benzodiazepines Linked to Increased Risk of Alzheimer’s: Causation or Not?
According to a study in the British Medical Journal, benzodiazepine use is associated with a significantly increased risk of developing Alzheimer’s disease. Some experts...
Researchers Identify Patterns in Antidepressant and Long-Term Benzodiazepine Use
The researchers found that, of those who were initially prescribed both antidepressants and benzodiazepines, approximately 12% went on to engage in long-term benzodiazepine use.
Benzodiazepine & SSRI Addiction and Withdrawal
The May issue of Addiction includes a review of pharmacological and phenomenological issues around benzodiazepine (BZD) and SSRI discontinuation. Definitions, perceptions and management of the...
Long-term Painkiller Use on Rise, 1/3rd Dangerously Mix with Anti-anxiety Meds
About 9% fewer Americans are using prescription opioids than were five years ago, but those people are taking more of the drugs for longer periods of time, according to a study by pharmacy benefits manager Express Scripts reported in FiercePharma. And nearly one-third are being put in serious risk of overdose death by taking the opioids alongside prescriptions for benzodiazepine sedatives, stated the New York Times.
Is a Little Stigma Better Than None?
An anti-anti-stigma campaign
The whole anti-stigma campaign is something of a joke. Google the word “stigma,” see for yourself. Mental health labels are inherently stigmatizing,...
New Clinical Guidelines on Deprescribing Benzodiazepines
New guidelines recommend deprescribing benzodiazepine receptor agonists for adults.