In a new study in Translational Psychiatry, researchers write that they have developed a blood test that can identify those who will die by suicide, and even tell the difference between them and others with a major depressive disorder diagnosis.
The researchers write, “Our results strongly suggest that blood gene expression is highly informative to understand molecular changes in suicide. Developing a suicide biomarker signature in blood could help health care professionals to identify subjects at high risk for suicide.”
If their data supports this claim, this would be a striking breakthrough—a true blood test that could accurately identify who’s most at risk. No need to do a psychological assessment for all of the factors linked to suicide—feeling lonely, burdensome, recent loss of a job or a loved one, etc. Instead, a simple blood test that can tell if you’re going to die by suicide soon.
In addition to just being able to tell who will die soon, the researchers also claim their results could lead to drugs that prevent suicide—no need to help people reconnect with others, improve their self-esteem, or get meaningful employment:
They write, “Genes identified as dysregulated in suicide could be potential targets for future pharmacological interventions to prevent suicide in MDD patients.”
The data, though, presents a much more murky picture. For one thing, it’s quite a small study: in total, they were able to analyze the blood from 19 people who died by suicide, 18 with MDD who died from other causes, and 16 without a psychiatric diagnosis who died from other causes. The researchers also acknowledge that their results are “preliminary” and that they used “exploratory” statistics—more liberal definitions of significance than usual. Thus, they write, their findings require replication by other researchers before they are actually considered usable.
So, what did they find?
There were 11 biomarkers that differed between the groups at a statistically significant level. However, statistical significance does not indicate clinical significance. Here are the results for those 11 biomarkers:
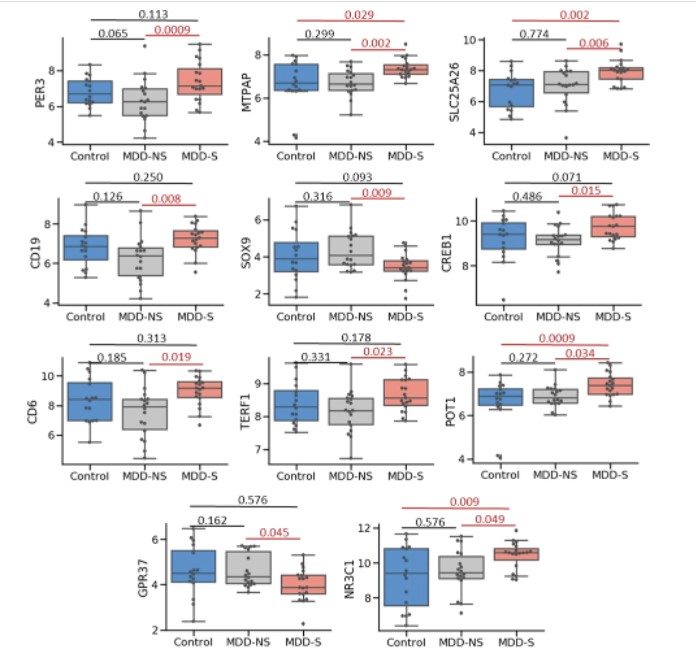
The important aspect to pay attention to in this graphic is the black dots, each of which represents one person. What these graphs demonstrate is that although the findings may be statistically different, in every group, almost every single biomarker overlaps with that of someone from a different group.
Let’s take a closer look at one biomarker, chosen at random:
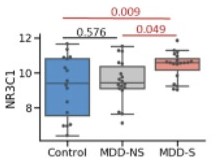
What we see here is that the “healthy” controls (on the left) had a wide variety of scores on this biomarker (hence the longer vertical black bar), while people with the MDD diagnosis who did not die by suicide (the middle) had a slightly tighter grouping of scores. People with the MDD diagnosis who died by suicide (on the right) had the tightest grouping of scores. These scores, on average, were statistically different, because those who died by suicide were slightly more grouped up at higher scores. But each individual score of those in the rightmost group overlaps with an individual score from one of the other groups.
That is, if you measured this biomarker for someone, it would tell you very little—usually nothing—about which group they were in.
(The exception is a few extremely low scores in the control group—but again, with so few participants, it’s unclear how seriously to take those three low scorers on this particular biomarker. They could easily be statistical outliers.)
But even if these findings were to be taken seriously, what they come down to is a finding that those who died by suicide were under extreme stress, which should not be surprising. The biomarkers that were elevated were mostly related to stress:
The researchers write, “Specifically, stress response changes, including polyamine metabolism, circadian rhythm, immune dysregulation, and telomere maintenance are shared among suicides in blood.”
This implies that people who are under extreme stress are more likely to die by suicide. One obvious solution, then, might be to alleviate the stressors people are experiencing.
However, the researchers suggest something else: that the biological systems responsible for conveying stress are to blame. Thus, more research should be devoted to these biological pathways:
“Future studies in large clinical populations investigating these systems might help in the identification of acutely suicidal MDD patients.”
****
Mamdani, F., Weber, M. D., Bunney, B., Burke, K., Cartagena, P., Walsh, D., . . . & Sequeira, A. (2022). Identification of potential blood biomarkers associated with suicide in major depressive disorder. Transl Psychiatry, 12, 159. https://doi.org/10.1038/s41398-022-01918-w (Full text)















To even entertain an idea is to legitimate the bio-neuro pseudo science. Should be better things to write about, like how people are organizing to eradicate the mental health system.
Joshua
Report comment
If this were true, it would be the first ever bio-marker “disorder” in the history of psychiatry, although there have been a few dsm categories, e.g., Rhett Syndrome, and genes was found to be the culprit, but then it was pulled out of dsm and given to real doctors. Says something about dsm and pathologizing human suffering – pretty much all negative.
Report comment
Oops
Report comment
Thank You Peter,
https://blogs.bmj.com/bmj/2021/07/05/time-to-assume-that-health-research-is-fraudulent-until-proved-otherwise/
Report comment
Based on this and lots of other failed bio-psychiatry studies, I can confirm that psychiatry is just trying its best to stay relevant at this point.
Report comment
Seriously, a blood test for suicide? Who is dumb enough to believe this kind of nonsense?
Report comment
The people who’ve been brainwashed into believing the cult called psychiatry that’s who.
Report comment
I wonder if there is a blood test for gullibility, or dishonesty?
Report comment
Peter, thank you for this excellent article. Very interesting and informative. Given the small sample size, statistical fishing expedition methodology, poor sensitivity and specify of test results rendering them clinically useless, and over-the-top claims in the abstract, this article is a prototypical psychiatric infomercial masquerading as science. But informercial for what product? I checked out the conflicts of interest section of the article which says there are none. None, with Alan Schatzberg as an author? No way this article isn’t part of an effort to develop an “anti-suicide” pill or patent a “suicide test” by the authors. My prediction is that another heavily manipulated and scientifically flawed study will soon be forthcoming followed by one or both of the aforementioned products, thereby enriching the authors. We know the playbook by now. The major problem with this study is the possibility that someone might take it seriously.
Report comment
Yeah. So now they can kill – “There’s was a death in his blood anyway…”. It is almost tribal manipulation done by a hostile shamans sponsored by evil kingdom. This is not medicine, this is a branch of barbarity.
———————————————————————————
James Hillman “Re – visioning psychology”
Report comment
And why would anyone submit to such a blood test? Someone should write an article about that.
Report comment