A new study in Psychological Medicine finds that babies born to mothers taking antidepressants were more than six times as likely to have neonatal withdrawal syndrome—including breathing problems, irritability/agitation, tremors, feeding problems, and seizures—than those born to mothers taking other types of drugs. More than 80% of the reported symptoms were classified as serious.
The researchers also did a second analysis by comparing antidepressants to methadone—a drug known to cause neonatal withdrawal syndrome. Their analysis found that antidepressants were just as likely as methadone to induce the effect.
“Our findings are of importance both for clinicians treating pregnant women and for neonatologists. When balancing potential benefits and risks for the prescription of antidepressants during pregnancy clinicians should not underestimate the risk of neonatal withdrawal syndrome with any type of antidepressant,” the researchers write.
The term “neonatal withdrawal syndrome” was preferred by the researchers. Other terms for the same syndrome include neonatal abstinence syndrome and poor neonatal adaptation syndrome.
 Previous Research
Previous Research
Studies have consistently found antidepressant use in pregnancy to be associated with myriad risks to neonatal health, including neonatal withdrawal syndrome, preterm birth, birth defects, developmental problems, cardiopulmonary problems, and even death.
In a 2021 study, researchers argued that antidepressants should be discontinued in pregnancy because of the risk of neonatal withdrawal syndrome. They identified symptoms of hypoglycemia, tremors, hypotonia, hypertonia, tachycardia, rapid breathing, and respiratory distress in babies born to mothers who used antidepressants.
In another study, researchers found that 30% of babies born to mothers who used antidepressants experienced neonatal withdrawal syndrome. None of the babies whose mothers did not use antidepressants had this complication.
According to Massachusetts General Hospital/Harvard Medical School, between 25 to 30% of babies exposed to SSRIs will experience this syndrome. Another study found that over half (56%) of babies exposed to SSRIs had this problem.
Yet another study accounted for preexisting factors like depression severity by comparing women who continued using antidepressants during pregnancy with women who had the same indication and did use antidepressants initially—but stopped after becoming pregnant. That study found that those who continued to use antidepressants increased the risk of neonatal health complications, including preterm birth, low birth weight, and hospitalizations, in their newborns.
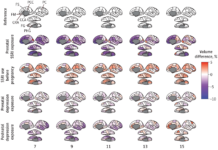
Other research has found that antidepressant use during pregnancy alters brain development in the fetus. These findings have appeared in top-tier journals, too: for instance, a study in JAMA Psychiatry found that antidepressant use during pregnancy increased the risk of infants with speech disorders, while a study in the American Journal of Psychiatry found that antidepressant use during pregnancy increased the risk of impaired neurological functioning in infants.
A Deeper Dive into the Current Study
In the current study, the researchers used VigiBase, the World Health Organization’s database for reporting suspected adverse drug effects. They compared the rate of neonatal withdrawal syndrome reports for antidepressant use versus the rate for all other drugs combined. Antidepressants were associated with a 6.18 times increased risk compared with the average of all other drugs.
The older tricyclic antidepressants were the worst offenders, with a 10-fold increased risk. SSRIs had the lowest rate of all antidepressants, but still increased the risk by 4.68 times compared with other drugs. Other antidepressants fell in between these two ranges.
The one exception appeared to be bupropion, which was not associated with an increased risk of neonatal withdrawal syndrome in this study.
Eighty-four percent of the neonatal withdrawal syndrome reports were classified as serious.
The study could not compare rates of neonatal withdrawal syndrome for antidepressants against those who took no drugs, since it was based on a drug adverse effect database. Presumably, this type of comparison would increase the relative risk for antidepressants even further.
Likewise, a study of this nature cannot prove causality. The prevalence of reported adverse effects in a pharmacovigilance system like VigiBase can be impacted by other factors, such as when a drug receives notoriety for having that effect.
However, the comparison with methadone accounts for this potential confounding factor. The researchers note that methadone’s connection to neonatal withdrawal was well-known. Thus, if notoriety was the reason for increased reports, antidepressants should have done better when compared to methadone.
The VigiBase adverse effect reporting database has over 28 million individual reports of adverse effects from drugs used around the world.
The research team was an international collaboration led by C. Gastaldon at the WHO Collaborating Centre for Research and Training in Mental Health and Service Evaluation, Department of Neuroscience, Biomedicine and Movement Sciences, Section of Psychiatry, University of Verona, Verona, Italy.
****
Gastaldon, C., Arzenton, E., Raschi, E., Spigset, O., Papola, D., Ostuzzi, G., . . . & Schoretsanitis, G. (2022). Neonatal withdrawal syndrome following in utero exposure to antidepressants: A disproportionality analysis of VigiBase, the WHO spontaneous reporting database. Psychological Medicine, 1-9. https://doi.org/10.1017/S0033291722002859 (Full text)














Yes, I flagged this up myself a while ago. This is a really important and good article.
Being born an addict with withdrawal cravings might set those children up for yearning for the back to womby bliss from street drugs. Then they get pregnant while on drugs and the cycle repeats. I do think some mom’s choose sophoriphics if they are weary from arguing all day with bickering partners. But those elixirs of calm should only be from safe herbalism specialists and only in a crisis. Your valerians and passifloras. Ancient respected remedies plucked by apothecaries from verdant hedges.
In Prozac’s hey day even babies in the womb were probably imbibing Prozac and finding their developing brain’s serotonin peaks and troughs inconsolable.
A crying baby can become a neglected baby if young parents have exhaustedly knocked on the doctor’s door and “tried everything” to soothe the baby. Mothers used to be blamed for being uptight. Told their “energy” or “worry” or “neuroticism” was to blame for a yelping pitiful bundle of joylessness. It would be slipped in their records that they were possibly not looking after their baby. Some babies may even have been taken away into foster care.
But I do hope this understanding won’t lead to grown up kids blaming their duped mothers for generational iatrogenic harm. Like passive smoking was sometimes blamed for some non smoker growing a tumour. The pills thing is an international and intergenerational TRAGEDY. Mothers would not have taken such pharmaceuticals had they had better knowledge of the consequences. We must move away from reactions that are parent blaming and instead create ways to repair the unintended awful results.
Report comment
These study results are devastating. It also leads me to wonder how to deal with it: Suppose a woman is taking antidepressant drugs and discovers she is pregnant. To protect the baby, she can taper off, but how will her withdrawal effects affect the developing fetus? This needs more research.
Also, it suggests it would be wise to taper off before becoming pregnant, which requires time and support, especially for those who have been taking AD for a long time. Both scenarios reinforce the need for more research and more supports for the under-studied and under-appreciated issue of psychiatric drug withdrawal.
Report comment
I don’t like to say “I told you so,” but…
https://canadafreepress.com/article/please-dont-forget-about-me-antidepressants-and-birth-defects
Report comment
Great that this info is out, but we now exist in a country that mandates full-term pregnancies while denying bodily autonomy to anyone with mental illness.
I’m pro-patient autonomy. I also know that many pregnant women are bullied or forced into remaining on SSRIs .The MH enforcers tend to increase brutality when their patient becomes pregnant and the ‘bad apple’ psychiatrists lead those efforts in degradation. The psych field is unsafe to women (and to NB, trans pregnancies) and needs scrutiny. Though, I do think this article will be validating to the many mothers who fought back against SSRI drugging while they were pregnant..Everyone else deserves restoration
Lawsuits needed on behalf of the mothers who were pushed, forced, or mislead to stay on these pills.
Report comment