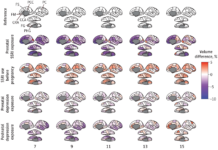
Antipsychotics Lead to Worse Outcomes in First-Episode Psychosis
Those who did not get antipsychotics in the first month were almost twice as likely to be in recovery after five years.
Stop Using Antidepressants Except for “the Most Severe Depression,” Experts Say
Experts advocate limiting antidepressant use to only the most severe cases of depression, emphasizing the need for social and psychological interventions.
ADHD Drugs Linked to Cardiovascular Disease
Service users taking drugs to treat ADHD may be at increased risk for hypertension and arterial disease
Adding Antipsychotics Worsens Outcomes in Psychotic Depression
Outcomes were worse for all, with young people on combination therapy twice as likely to experience rehospitalization or death by suicide than those on antidepressants alone.
Only One of Five Key Xanax Trials Deemed Positive by F.D.A.
The published literature is misleading, as the negative Xanax trials either went unpublished or were spun to appear positive.
Animal Study Shows Impact of Prozac in Pregnancy on the Child
Researchers found that rats born to mothers given the antidepressant Prozac during pregnancy or breastfeeding exhibited varied behavioral and developmental effects, with implications for the understanding of antidepressant impacts during human pregnancies.
Mental Health Staff Reluctant to Support Service Users in Tapering Antipsychotics, Study Finds
Study reveals schizophrenia patients find little support from mental health staff in reducing side effects-heavy drugs.
SSRI Use During Pregnancy Alters the Child’s Brain Development
Reduced brain volumes due to SSRI exposure in pregnancy was not explained by maternal depression alone.
Psychiatric Journals’ Pro-Pharma Publication Bias Hides Suicide Risk of Antidepressants
Selective publication bias in top psychiatry journals was not explained by the quality of the studies, but by financial ties to pharma.
Antidepressants Increase Suicide Attempts in Youth; No Preventative Effect
Researchers find that SSRIs increase suicide attempts up to age 24, and have no preventative effect at any age, even for those at high risk of suicide.
No Benefit for Adding Antidepressants to CBT in Severe Depression
For those with severe depression, inpatient CBT was effective but the adding antidepressants did not improve treatment outcomes.
New Data Reveal the Full Extent of STAR*D Failure
The initial study, which has been used to promote antidepressants, employed outcome switching to hide poor results.
Lexapro for Children: Drug With No Meaningful Benefit and Increased Suicidality Gets FDA Approval
Response and remission rates were the same in the drug versus placebo groups, and Lexapro increased suicidality sixfold.
Patients Express Anger at Doctors’ Ignorance About Antidepressant Withdrawal Effects
Antidepressant users share their frustrations towards a healthcare system that overprescribes but is ill-equipped to support with discontinuation and withdrawal symptoms.
Prolonged Negative Impacts of Benzodiazepine Use Revealed in New Study
Researchers find that adverse effects often last over a year, with many users experiencing substantial life changes.
Antidepressants, Antipsychotics, and Benzos All Increase Suicide Attempts in New Study
In a study of people with borderline personality disorder, only ADHD stimulants were associated with a decrease in suicide.
Pharma CEO, Others Attempt Contradictory Critiques of Serotonin-Debunking Study
Moncrieff et al. respond to the contradictory and, in some cases, false concerns raised by these critics of their serotonin review.
Cancer Risk Higher for Those on Clozapine
The antipsychotic clozapine, considered the “gold-standard” treatment for psychosis, was found to increase the risk of blood and lymph system cancers.
No Difference in Antidepressant Effectiveness After Genetic Testing
Genetic testing may help reduce the length of time people experience the harmful effects of antidepressant drugs, but it is not helpful for predicting efficacy.
Do Not Prescribe Antidepressants for Mild to Moderate Depression or at First Visit
World Psychiatry article challenges conventional antidepressant prescription practices.
Study Highlights Lack of Evidence for Antidepressants in Treatment of Chronic Pain
A new Cochrane review details the lack of evidence for antidepressants in the treatment of chronic pain.
Hyperbolic Tapering off Antidepressants Limits Withdrawal
New research by Jim van Os and Peter Groot finds that using hyperbolic tapering to discontinue antidepressants reduces withdrawal effects.
What Is the Risk of Permanent Sexual Dysfunction from Antidepressants?
Males taking antidepressants were at 100 times the risk of erectile dysfunction compared with the healthy population and more than three times the risk even after controlling for other variables.
Breaking Blind: Antipsychotic Drug Efficacy May Be Overestimated
Only 4 of 188 antipsychotic trials assessed blinding, and in all 4 cases, the blind was broken, potentially leading to an overestimation of the drug effect.
Prescribers Often Fail to Support Patients Discontinuing Antidepressants, Study Finds
Study reveals most patients are dissatisfied with prescribers' support when discontinuing antidepressants.