My name is Daniel and I am 25 years old. I hold a Bachelor of Science degree (pre-health professions/Kinesiology) and am in my last term of a Master’s of Science in secondary education/science program. Because of mental health issues, I currently take 20 mg of Prozac (fluoxetine) and 2.5 mg. of Zyprexa (olanzapine). For the past several months, I have suffered from what I believe is a reaction to the drugs I’m on: mouth ulceration. I have had mouth ulcers in the past, but not like this. Since 2020 began, I have had a minimum of two to five ulcers in my mouth most of the time, with a grand total of about 40 ulcers during this period. At some points, I’ve had five to seven ulcers at once. I am not 100% certain if this is due to my medications, but I strongly believe there is a relationship, and that motivated me to tell my story.
My Backstory
When I was coming home from school one day when I was in the eighth grade, I was attacked by a gang of about a dozen middle-school kids. The gang beat me up pretty badly, and I was left with a huge lump on my head and quite a few large bruises. My parents took me to the emergency room and the hospital filed a police report. No one was ever apprehended. Since then, I have suffered from emotional distress.
Although I’ve had migraines since I was about nine years old, by age 15, they were coming regularly—one to three a month. After being attacked, I began to suffer from extreme migraine episodes when, in addition to getting a terrific headache, I developed gastric stasis problems. Also, the left or right side of my face plus my hand and leg on that side would often get extremely numb. The numbness persisted over the years and gradually got worse. I finally visited a neurologist when I was in tenth grade. I had a headache the day before my appointment (it was not as severe as at other times and I didn’t think it was a migraine). The neurologist administered an EEG in his office, and we learned that my headache had been a hemiplegic migraine, which mimics a stroke.
I became terrified of what was happening to me and how numb parts of my body would become. Sometimes I would wake up with numbness down half my body and heave over the toilet many times until I finally vomited. During high school, I felt like I was a burden to the nurse’s office because my frequent illness made it look like I was gaming the system to get out of class. I assure you, I was not.
In high school, I struggled with emotional problems. When I went inpatient during my junior year, I was put on the neuroleptic Risperdal. I was told little about the drug or its potential effects, so I researched them myself. I believe every patient must be knowledgeable of the side effects related to his or her medications, since in my experience psychiatrists generally are not forthcoming with this information. Meanwhile, the migraines continued, growing more and more severe over the years.
As I approached 24 years of age, I started to wonder if maybe I didn’t need to be on the Risperdal any longer. No mental health diagnosis had been provided to me when I was discharged from the hospital at 17, so I wasn’t really sure why I was taking it. I had been seeing the same psychiatrist since I was hospitalized. However, the hospital where he worked had been sold and no longer took my insurance, so he advised me he was dropping me as a patient. He explained that he handled children and, since I was no longer a child, he suggested finding another psychiatrist nearer to where I lived.
Eventually, I was accepted into a behavioral health group and provided with a new psychiatrist. As it turned out, she had a preconceived notion of what was going on and did not want to listen to me. Without even taking a look at my medical records, she told me she wanted to put me on a particular medication. Period. Because of her attitude, I didn’t see her again, but one good thing did come of that visit: She ordered blood tests. When the results came back, they showed that after about seven years on Risperdal, the drug had backfired, dangerously raising the prolactin levels in my endocrine system. That meant I had to come off of it. Incidentally, the psychiatrist never actually mentioned this fact. Luckily, I had obtained a copy of my labs and brought the results to the attention of my primary care physician.
While discussing the prolactin level issue with her, I brought up the fact that I wanted to withdraw from the Risperdal and mentioned my lack of success in getting an empathetic psychiatrist to help me. She said she would work with me, not realizing how far in over her head she would get.
Risperdal Withdrawal
Risperdal withdrawal was the most powerful, daunting experience of my life. During that process, I often felt intense numbness and severe muscle pains in my arms and legs that would wake me up at night. At the time, my primary care physician suggested getting an electromyograph (EMG) to help find the cause. When I eventually had one, the physician administering the test asked me if I had been in a car accident. I was surprised, but expected something to be wrong because of how numb I was getting. He later told me the EMG results showed that I had cubital tunnel syndrome (a problem with a nerve in the elbow) and a compressed peroneus muscle (in my lower leg and ankle).
Meanwhile, I dropped down on the Risperdal by about .5 mg every month. By the time I got down to .5 mg of Risperdal daily, my behavior had become obnoxious. I was nasty to my family. I didn’t want to eat with anyone. I would go for drives and just park and sit and not come home until after sundown. Even my primary care physician observed that I was hyper-fixated on things and talking incessantly. Acknowledging she could not continue to work with me on my withdrawal, she recommended I get an appointment with a psychiatrist, which I did—surprisingly quickly this time.
This psychiatrist just wanted to tell me what he saw and wanted to do. He would ask me a series of questions to which I was to give “yes” or “no” answers only. He decided to keep me on the .5 mg of Risperdal and added 20 mg of Prozac daily. As the Prozac kicked in, I felt as if I had woken up from a dull perception of life and returned to my childhood self. But those euphoric feelings were short-lasting. Once the psychiatrist raised me to 40 mg of Prozac, I began to perspire incessantly and my mouth became extremely ulcerated. So he dropped the dose back to 20 mg.
After a short period, my behavior degenerated again. I became severely agitated toward my family and, for the first time ever, I had suicidal ideation. On a day that I was scheduled for a therapy session, I began to rant and rave, so my psychiatrist called an ambulance that took me to a crisis-response center. From there, I was transported to a mental hospital. Sadly, I had rescinded my authorization for doctors to share medical information with my family, so when I didn’t come home that day, my mother and sister had no idea of my whereabouts. Fortunately for me, the admissions nurse eventually convinced me to give permission for my mother to be notified.
In the hospital, I was prescribed 2.5 mg of Zyprexa, along with the usual Prozac plus 50 mg of the antihistamine hydroxyzine to help with stress reduction. I was in the hospital for a grand total of five days. This was at the beginning of the pandemic; I’d only agreed to a five-day stay, and when another patient in the facility was taken to a medical hospital with a suspected COVID-19 infection, I demanded to be released. With my mother asking that I be released as well, they let me go home. I later learned that the mental hospital had originally planned for my stay to last 20 days.
Soon after my discharge from the hospital, my psychiatrist decided I should try Tegretol (an anticonvulsant) instead of Zyprexa. Unfortunately, within a couple of days of starting the Tegretol, I exhibited a rash on my foot, which I learned is a pretty serious side effect. So, I went back to the Zyprexa, Prozac, and hydroxyzine cocktail.
Painful Mouth Ulcers
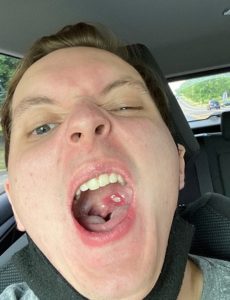
Once home, I began to feel like my old self. But the mouth ulcer problem persisted. From about February until April of this year, I lost a tremendous amount of weight (I am 6’3,” but was down from about 200 lbs. to about 145 lbs.). Part of my weight loss was attributable to the mouth ulceration, as the ulcers made eating excruciating. The problem persists, and sometimes it is pure agony.
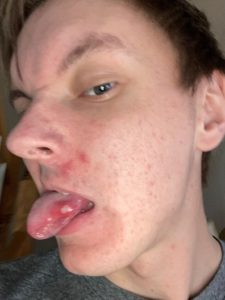
I consulted with my primary care physician about the ulcers. She suggested that they were caused by the hydroxyzine, so I stopped taking it. I experienced a very brief reprieve, but then the ulcers returned with a vengeance. As you can see from these photos, they are large, inflamed, and nasty and sometimes occur three to four at a time.
Because I’d never received informat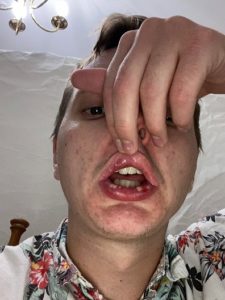 ion about possible drug side effects, I began researching the topic online. I found a case study that documented ulceration in an adolescent who was taking fluoxetine (Prozac). Additionally, I found research showing some associations between ulceration and the use of Prozac and Zyprexa.
ion about possible drug side effects, I began researching the topic online. I found a case study that documented ulceration in an adolescent who was taking fluoxetine (Prozac). Additionally, I found research showing some associations between ulceration and the use of Prozac and Zyprexa.
Seeking Validation
I feel that this country invalidates the experience and insights of those who are maladjusted. Based on my experiences, I’d advise any patient, particularly someone who struggles with physical distress either from an ailment and/or as a result of medication side effects, to investigate their body and what they are putting into it. For me, one of the best things I did was to take start taking Vitamin B-12 supplements after researching online what might be causing my numbness episodes and migraines. Not only did my episodes lessen, but I haven’t had a migraine now in months. My neurologist later gave me a pat on the back for doing that and attributes the diminishment of my headaches to the B-12 alone. And now that I am off the Risperdal, the brain MRI I had this past summer showed no indication of the nerve issues seen in the EMG during my withdrawal from that drug.
Even though some of my medical issues have resolved, I now believe the universal law for a mental health patient is similar to Murphy’s Law—whatever can go wrong, will go wrong. One extreme, bad situation is transformed into another. So, if you have numbness and tingling from drug A, and switch to drug B, drug B might cause extreme mouth-related ulceration. Some of these side effects can lead to depression. For me, the ulceration is too intense to bear and very demoralizing.
Professionals’ attitudes toward my suffering and its causes are also demoralizing. I can complain about side effects, but because of psychiatry’s belief in anosognosia, a patient’s unawareness of their mental illness, something can actually be wrong but people will react negatively to my pointing it out, or respond in a stigmatizing way. In Stephen Soderberg’s 2018 movie Unsane, the main character is stalked by an individual from earlier in her life. This person just so happens to be a mental health nurse at a facility where she had been an inpatient. When the main character complains about the stalker, the psychiatrist concludes that she is paranoid and needs “more lithium!”
I feel much the same way about my own concerns. I have shown photos of my ulceration to my health care providers and, except for taking me off of hydroxyzine, they didn’t really do anything to accommodate my need for relief from the ulcers and the concomitant pain. Since when do someone’s side effects invalidate his or her human rights? I’m not a doctor, so how can I know what to look for if I have a bad reaction to a medication? It’s almost as if modern medicine couldn’t care less.















I would purge, water fast, get back to “zero” basically. I would throw “life” to the side to just get through this, and then be damn bitter about it 😉
(It should go without saying, the purge/fast means no drugs)
Report comment
“Sadly, I had rescinded my authorization for doctors to share medical information with my family,”
Boans sits and ponders living in a place where such rights are respected. My medical records were “edited” and then distributed without my consent and as a means to slander someone they knew had been subjected to an act of torture and kidnapped. The ‘weapons’ available to these people to conceal their misconduct are quite possibly an explanation for the large number of suicides their ‘services’ are correlated with.
“Since when do someone’s side effects invalidate his or her human rights?”
Since the moment you enter into a doctor patient relationship, and provided ‘implied consent’? (you asked for ‘help’, sorry if your of the opinion this isn’t helpful. Your opinion simply doesn’t count) You just lost your right to consent and are unlikely to notice until you use the word “no”. Then your about to get a lesson in the psychological trauma of ‘coercion’ (drugged without your knowledge [with date rape drugs] and threatened with weapons until you say yes). Of course it’s not torture because of the “inherent in or incidental to lawful sanction” loophole in the Convention against the use of Torture. As a “patient” what would be considered torture becomes an act of kindness to you. Not unlike cutting your chest open to do an operation on your heart, but without the lawful need for consent because the patient is unconscious. To a psychiatrist we are all non compus mentis with our eyes open.
Now consider the effect this could have if you had the ability to make a citizen into a “patient” AFTER you have subjected them to acts of torture? It conceals the torture and allows you to slander the victims as anosognosic ‘mental patients’. And we all know from the Minister that no matter how much they complain, “you can’t listen to them, they’re mental patients”.
So in my State when the police use torture, they simply ‘flag’ anyone who complains for immediate referral to mental health services for ‘refoulment’ with an unintended negative outcome. We provide services to people from other countries who have been traumatised by acts of torture, and provide a label and copious amounts of drugs to anyone we subject to acts of torture and call them “patients” to conceal our human rights abuses. It creates the appearance that ‘they’ torture and ‘we’ don’t. Well we do, but under normal circumstances the victims don’t ever get the chance to be heard. In many cases they can be Stockholmed and will assist in their destruction by taking the drugs willingly.
Consider your use of the term “side effect” for example. It’s a verbal trap. Your assuming something to be using that term, that the unwanted effect was not doctors intention. How would you prove it if a doctor was injecting you with a cocktail that was intended to make your skin feel like it was burning and they claimed it was a side effect? And you had no choice but to take the drugs? And he/she simply smiled at you when you suggested to them that they were deliberately harming you? Police don’t even bother asking because they know they would need a confession that the intent was to harm, which they would not obtain. In fact your complaint would be considered grounds for referral to mental health services for ‘treatment’ And I met one young man who resorted to putting a pistol in his mouth and pulling the trigger, taking a big piece of his face in the process, just to have the forced drugging stopped.
Things haven’t been this good since the Inquisition lol Even Mengele had a burden of proof placed on him by the National Socialists (hence the need for “editing” the documents with a match when someone from outside wanted to look). In my State they simply “edit” the documents after the fact and make the complainant a “patient” requiring ‘treatment’. Cover ups provide the State with the ability to violate human rights and turn away anyone who dares question their authority.
You have the right to remain silent, but quite possibly not he ability to when being subjected to ‘treatment’ for exercising that right. The ‘side effects’ will stop when you answer the questions, maybe.
Report comment
What kind of treatment is that that worsens the quality of life?
Another story about the revolting ignorance of doctors
Report comment
And tends to kill you younger if you follow your “treatment plan.”
Report comment
Yes, I had ulcers in my mouth. too. I almost asked the prescriber about them; but, soon after that, I totally quit the drugs and they were mostly gone. However, when stressed, one or two may flair up for a while and then go away. Of course, like you, that’s not the only issues I dealt with while on the drugs and then there was the withdrawal. sadly, even after the withdrawal, there are still issues in which to contend. However, since none of the drug-makers or the psychiatrists, etc. want to admit all this; it is very difficult to know how long any of this will last. But, since the brain is definitely involved, it may be lifelong. Thank you.
Report comment
Thanks for your story Daniel. I also had a whole heap of ghastly effects when the Zyprexa/Prozac combo was inflicted on me, including but not limited to migraines, mouth ulcers and nerve issues…oh and lets not forget the serious suicidal ideation, akathisia and eating problems!
It’s not supposed to happen to adults (I was in my 50’s) but those effects were very real, and I was very lightly dismissed by shrinks as being medication non-compliant, and having the dreaded anosognosia. So nothing was done to assist…they merely doubled down.
I agree that it is horribly demoralising, and akin to torture…a total breach of human rights.
I too found B12 helpful, but coming off the drugs was ultimately what helped most. I am sure you realise how carefully dose reduction must be done – it’s not pleasant and don’t rush it!
Since coming off them, my migraines have dropped right back to pre-drug levels and other symptoms have gradually abated. There is hope.
The trick I found was to slowly and quietly walk away from psychiatry – it is irredeemable. I’m afraid my experiences confirmed that complaining only increases the intensity of its attacks.
You’ll find lots of useful info on this site and others….all the best with your escape and recovery from any damage those charlatans may have done!
Report comment
Great comment and I hope Daniel finds it validating and reassuring.
Report comment
Have you seen an oral pathologist yet? They deal with diseases of the mouth and would probably be more helpful than a family doctor.
Also, have you been tested for H. pylori?
I’ve been experiencing problems in my mouth, throat and stomach too. I think some of it may be due to the anticholinergic effects of the psych drugs. They dry you out, for one thing. I hate the way I feel on them and wish I could go off eventually, but so far have failed in my attempts.
Report comment
Daniel.
Tank you for sharing your tough journey. I cannot imagine the men and women
who ignored your plight to even be pet owners.
But you know I see so much strength in you writing your account and guaranteed
it will reach others to validate their suspicions.
We really have to do this ourselves. The education and the walking away.
There are many resources out there, connect with that which resonates with you.
If something feels not right for you, it’s not right. Period.
Report comment
Daniel was maimed – elevated prolactin, ulcers, migraines – almost exactly as I had been, on psychiatric narcotics which had also been prescribed to me, in response to stressors I had also experienced (toxic schools, no escape, unaccountable law enforcement), and under circumstances (“Suburban Lifestyle Dream”, conscientious parents who were duped by quacks, same age) identical to mine.
We aren’t an outrageous coincidence or two disgruntled losers who simply need “more Lithium”. Psychiatry failed us; it nearly killed us, and vocal ex-patients are a small minority of psychiatry’s abject failure.
Report comment
“Psychiatry failed us; it nearly killed us, and vocal ex-patients are a small minority of psychiatry’s abject failure.”
Yes, most of the unintended negative outcomes no longer have a voice……. or a heart beat for that matter. And whilst means and opportunity may be easily identified, any copper will tell you that you’ll never establish motive (particularly when police will retrieve any documented proof of a motive. Documented torture and kidnapping? We’ll have them back thanks) unless they confess. And with that “sophisticated knowledge of the law” that isn’t going to happen. And even when it has, prosecution of someone who does confess to ending the life of a “patient” is “not in the public interest” (see the case of Dr Alida Lancee). Sad that a citizen can be made into a “patient” with “edited” documents post hoc, well it is for the “edited patient” not the doctor, and police will actively assist in the process of ensuring no action is taken. Amazing what can be done by a doctor (nay, even a Community Nurse) who calls police and requests assistance with their “patient” who just happens to have collapsed as a result of being ‘spiked’ with date rape drugs, and had a knife planted on them for police to find. Set Ups being authorised by the Minister in the name of getting citizens the ‘help’ they don’t need for ‘illnesses’ they don’t have. And we have allowed these people to pass legislation allowing them to administer lethal injections? Combine that with the ability to “edit” documents post hoc (Just a not, “editing” legal narrative to conceal crimes is not really by definition “editing” but these are people who prefer euphemisms such as unintended negative outcomes rather than they killed the person by snapping their neck during a ‘restraint’.)
Report comment
Thanks for sharing your story, Daniel. It’s just appalling the damage psychiatrists do to their patients, then deny. I’m so sorry you’ve been so harmed.
I, too, am a survivor of extreme antidepressant and antipsychotic induced anticholinergic poisonings. I did not personally suffer from oral infections, but did run into a couple other, likely psych drug induced immune system compromised, infections when being neurotoxic poisoned.
I hope and pray you are able to heal from the traumas, including the psychiatric induced traumas, to which you’ve unjustly been subjected.
Report comment
Thank you for your story Daniel. For you mouth ulcers, you might want to check your toothpaste. I used to get horrible mouth ulcers too. Most toothpastes contain an ingredient called Sodium Lauryl Sulfate. That ingredient has been know to cause mouth ulcers and now that I avoid toothpaste containing it, I rarely get them.
I am a psychiatric survivor. I was given quite a cocktail of psychiatric drugs. I was started on an SSRI when I was 20, for off-label use. I had TMJ issues. Shortly after started the SSRIs I developed terrible GI issues. I had diarrhea and during the small bowel follow through the barium was in my stomach for 4 hours. I should have been diagnosed with gastroparesis (delayed gastric emptying) then but nothing was wrong with me. The antidepressants were depressing and lead to a psychiatric misdiagnosis. I was given more and more drugs. By the end of my 14 years on psychiatric meds, I was on the maximum dose of zyprexa, the maximum dose of Lamictal, and Zoloft. I was walking into walls. Sleeping 12 hours straight through 3 alarm clocks. I was regurgitating food. I had severe tremors. And there are no such thing as side effects only direct effects of the drugs that doctors and pharmaceutical companies like to ignore. I am completely off all psychiatric drugs. I educated myself on how to taper myself off and I received very little help. I was told something bad might happen. At the point I decided to go off my drugs my body was already shutting down. My weight was in an all out free fall. According to my doctors I wasn’t losing weight. How they missed the 100 lbs weight lost is beyond me. Were they blind?
Today, I get most of my nutrition through an IV. My GI tract is nonfunctional. I have dysautonomia which is a fancy term for the dysfunction of the autonomic nervous system. All those things you don’t think about but your body is supposed to do automatically. One gastroenterologist admitted that it was probably the psychiatric drugs that caused my medical issues. Gastroparesis used to be limited to just people with diabetes, but not any more. The vast majority of people with gastroparesis and GI dysmotility are idiopathic, a fancy medical word for they don’t know. Being in the gastroparesis support groups I have noticed a high correlation of the people with gastroparesis and dysautonomia are currently taking or haven taken psychiatric medications.
I now live with a plethora of symptoms. Regular healthcare is just as bad as mental health care. Consent…What exactly is that? I was given a “Nutrition Support Partnership Agreement” and partnership is a real stretch of the imagination. To sum up the contract it says that if you don’t do everything your doctors ask we will kill you. Actually they phrase it a little nicer. If you don’t follow every recommendation we make then we will throw you out of the program. For those of us that need nutrition support being throw out of the program means dehydration, malnutrition and potential death if you can not find another doctor to take over in time and very few doctors are willing to prescribe nutrition support.
Doctors and nurses regularly lie in my medical chart. If they don’t like you, they have no problem causing defamation of character. I dislike all the doctor and nurse worship that goes on in this country. The truth is I am regular abused and then blamed for that abuse. That abuse is not limited in psychiatric wards. It is systemic throughout the hospital systems. I have nightmares about people that work in healthcare. The “Care” in the word Healthcare is a real stretch of the imagination. They have no empathy and no compassion for the people they are treating and “treating” is also a stretch of the imagination. They try to give you another cocktail of drugs to cover up some of the symptoms. Most doctors tell me it is not there job to diagnose or treat. Most of my appointments look exactly the same. Yes, still have the same symptoms and see you in 3 months, with some verbal abuse thrown my way. Maybe insulting me is the only way they know how to interact with another human. I don’t have a primary care doctor. They are the worst with the insults. Also they don’t accept patients like me, they like healthy patients. A gastroenterologist was trying to do a study with primary care physicians to see if they could get to the patients diagnoses faster but her studied failed because as soon as the PCP found out their patients had dysautonomia and gastroparesis they abandoned their patients. PCPs are the worst for patient abandonment. They claim they don’t feel qualified to treat us. The truth no one is qualified. I am on my own. I am left to fly solo and navigate a scary world completely and utterly alone. Most patients give up. Only the strong fight. It is an unrelenting battle. A battle to get them to do their jobs just to stay alive another day. I would have lost that battle a long time ago if I had stayed on the psychiatric medication. I have been on Parenteral Nutrition/IV Nutrition for 4 years now with almost no hope of ever getting off.
My recommendations are stay away from psychiatric drugs.
Report comment
Hi toostubborn.
I encountered the “healthcare” system and I know what you are saying is absolutely
true.
It came about because of the rudimentary science, a pretense that doctors are discoverers of
issues and that there are actual treatments.
IF you cannot successfully be treated, and you dare to complain, the slander starts.
A LOT of the chronic illness “programs” are laced with demeaning language.
They are smokescreens to make it seem that people are treated. These programs are run by young healthy people with lots of brainwashing.
They don’t want to deal with chronic stuff, they hate it. And the minimizing or innuendos by staff are all done to discourage empathy, and to discourage the patient from returning.
I get it. I get that the nurse or doctor cannot fix the suffering that goes on at home.
But if they could stop with the abuse, the lies, own their ignorance.
The public was misled by “science”. When people want to convince you of how wonderful all those advances are, they cite their own experience, or uncle Joe’s heart surgery.
They have no inkling of how ugly it can get.
Report comment
Hello,
I think your migraines and mood/mental issues might be caused by Disseminated Histoplasmosis.
Report comment
I cannot thank you enough for posting this. I thought I was going crazy. For the past week I’ve dealt with an ulcer on the inside of my lip, which then I had one literally in my throat and just this week on the side of my tongue. Your pictures were spot on.
I had done a search for hydroxyzine and side effects and then I specifically searched ulcers and came across your article
I too am in disbelief that it is not a side effect that is listed!
Report comment
Thank you so much for this article. I was recently brought into the ER because I was having a severe panic attack and they put me on hydroxyzine. I quickly started to develop these ulcers and painful mouth swelling. I came back the next day because I also had a fever and the doctor just looked at me (didn’t run any tests and by look I mean just literally looked at me) and said I had cold sores or herpes 1(labialis). I was so confused because I had spent the entire weekend home and I never share drinks with anyone. It didn’t make any sense to me. Then I started doing my research as the more I took hydroxyzine the worse I got. I had never taken this medication before and never suffered from “cold sores” and it’s spread to my throat as well. Thank you for this.
Report comment
Hi All,.
Some 10 weeks ago I finished Escitalopram which i was on this year from Feubruary until August and in 2023 i was on it for 2 months. In 2023 i had no ulcers only swollen taste buds here and there. But this year since start of february when i started escitalopram i have the issue. Neverthelless, even now when discontinued the drug 10 weeks ago i get aptheous ulcer usually 1 on weekly frequency. It gets healed within 2 days normally, while when i was using escitalopram it took full week to get healed.
Anyone having same kind of issue?
Report comment