From EMPOWER to Exercise: What Actually Helps Older Adults Quit Benzos?
Despite clear risks, benzos and z-drugs remain widely prescribed to the elderly. New research explores what helps—and what doesn’t—when trying to stop.
Benzodiazepines Linked to Suicide, Study Finds
A new study finds that benzodiazepines—alprazolam (Xanax), lorazepam (Ativan), and diazepam (Valium)—are associated with an increased risk of suicidal events.
Psych Drugs May Increase Likelihood of Death in Schizophrenia
The drugs, especially benzos and high doses of antipsychotics, led to an increased risk of death within five years. Antidepressants also did not reduce mortality.
Long-Term Benzo Use Linked to Increased Disability
Despite guidance that the drugs should only be used short-term, about a third of patients indicated long-term benzo use.
Only One of Five Key Xanax Trials Deemed Positive by F.D.A.
The published literature is misleading, as the negative Xanax trials either went unpublished or were spun to appear positive.
Prolonged Negative Impacts of Benzodiazepine Use Revealed in New Study
Researchers find that adverse effects often last over a year, with many users experiencing substantial life changes.
Research Explores the Experience of Benzodiazepine Withdrawal
A new study reveals many benzodiazepine users are misinformed about the risks of withdrawal and experience devastating consequences.
What Helps Long-Term Users of Benzodiazepines and Z-Drugs Discontinue?
Current long-term users of benzodiazepines and Z-drugs identify barriers and facilitators for discontinuation.
New FDA Study Shows Benzodiazepines Can Cause Long-Term Injury
The FDA has finally acknowledged the adverse effects of benzodiazepines, the dangers of withdrawal, and that the current packaging does not sufficiently warn of these harms.
World Benzodiazepine Awareness Day 2020
This week on MIA Radio, we present the second part of our podcast to join in the events for World Benzodiazepine Awareness Day 2020...
Benzodiazepines Linked to More Emergency Department Visits
Recent research implicates benzodiazepines as being involved in a high rate of emergency department visits in the US.
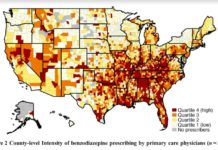
Benzodiazepine Prescriptions in Older Adults Used in Rural and Low Income Areas
Benzodiazepine prescription practices may be in response to an epidemic of distress, rather than being used to treat specific mental health diagnoses.
Nonclinical Factors are Associated with Long-Term Benzodiazepine Use in Older Adults
White race and size of initial prescription, along with poor sleep quality, are associated with long-term benzodiazepine use in older adults.
Psychiatrists Warn Policymakers Benzodiazepine Overuse Could Lead to Next Epidemic
Although opioid addiction and overuse have garnered significant national attention, similar trends in benzodiazepine overprescription and overuse continue to go unnoticed.
Cognitive Impairment from Long-Term Benzodiazepine Use Remains Even After Drug Withdrawal
Long-term benzodiazepine use shown to effect cognitive function during current use and for years after drug discontinuation.
Preventing Long-term Benzodiazepine Use
Researchers Identify risk factors for long-term benzodiazepine use to prevent harmful effects.
Researchers Identify Patterns in Antidepressant and Long-Term Benzodiazepine Use
The researchers found that, of those who were initially prescribed both antidepressants and benzodiazepines, approximately 12% went on to engage in long-term benzodiazepine use.
Prescribing Benzodiazepines As-Needed Leads to Abuse
A new study reported on in Medscape, examined risk factors for misuse of benzodiazepines (drugs such as Xanax, Ativan, and Klonopin). The researchers found that patients who had been prescribed the medication on an as-needed basis were more likely to end up abusing it than those who had been prescribed a standing dose.
Hypnotic Medications Linked to Suicide Risk
A recent review found that hypnotic medications are associated with risks of suicide and suicidal ideation.