Tag: antidepressant efficacy
Half of Those Who Take Antidepressants Are Labeled “Treatment Resistant”
Millions of people are trying multiple antidepressant drugs without success, and psychiatry labels them “treatment resistant.”
Antidepressant Trials Last Eight Weeks, So Why Do We Take Them...
The studies are of short duration and are riddled with methodological issues like unblinding and failure to assess withdrawal.
Placebo Effect—Not Antidepressants—Responsible for Depression Improvement
In adolescent depression treatment, those who received a placebo but thought they received Prozac improved more than those who received the drug and knew it.
Stop Using Antidepressants Except for “the Most Severe Depression,” Experts Say
Experts advocate limiting antidepressant use to only the most severe cases of depression, emphasizing the need for social and psychological interventions.
Psychiatric Journals’ Pro-Pharma Publication Bias Hides Suicide Risk of Antidepressants
Selective publication bias in top psychiatry journals was not explained by the quality of the studies, but by financial ties to pharma.
Antidepressants Increase Suicide Attempts in Youth; No Preventative Effect
Researchers find that SSRIs increase suicide attempts up to age 24, and have no preventative effect at any age, even for those at high risk of suicide.
No Benefit for Adding Antidepressants to CBT in Severe Depression
For those with severe depression, inpatient CBT was effective but the adding antidepressants did not improve treatment outcomes.
New Data Reveal the Full Extent of STAR*D Failure
The initial study, which has been used to promote antidepressants, employed outcome switching to hide poor results.
Do Not Prescribe Antidepressants for Mild to Moderate Depression or at...
World Psychiatry article challenges conventional antidepressant prescription practices.
Regulators Are Approving Drugs Without Clear Evidence That They Work
Drug regulators frequently approve drugs despite contradictory clinical trial results and without evidence of clinical benefits.
Garbage in, Garbage out: The Newest Cochrane Meta-Analysis of Depression Pills...
In May 2021, Cochrane published a network meta-analysis of depression pills for children. The abstract is misleading and reads like drug company marketing.
Researchers: Antidepressant Use in Children Increases Suicide, No Evidence of Benefit
Noted antidepressant researcher, Michael Hengartner, summarizes the latest research on the use of antidepressants in children and adolescents.
Unblinding in Antidepressant Trials Biases Results
Studies that compare the effectiveness of different antidepressant drugs are unreliable, according to new research in BMC Psychiatry.
Results of World’s Largest Antidepressant Study Look Dismal
The STAR-D study is by far the largest and most expensive study of antidepressants ever conducted, and it suggests that in real life situations, people taking antidepressants do not do very well. This may be the reason why the results of the main outcome of the STAR-D study have remained buried for so long.
Joanna Moncrieff and Carmine Pariante Debate Antidepressants
On June 19th, Joanna Moncrieff and Carmine Pariante held an online antidepressant Q&A session with host Danny Whittaker. There was an initial debate, followed...
Review Finds Lack of Evidence for Antidepressants in Treatment of Insomnia
Results from a Cochrane meta-analysis find that the common practice of prescribing antidepressants to treat insomnia is not supported by current evidence.
Dr. Joanna Moncrieff: Challenging the New Hype About Antidepressants
An interview with psychiatrist, academic and author Dr Joanna Moncrieff, one of the founding members of the Critical Psychiatry Network. We talk about the recent meta-analysis of the efficacy and tolerability of 21 antidepressant drugs, widely reported in the UK news media on February 22nd.
Pharma Responds: Antidepressants Really Work. Really?
A recent meta-analysis published in Molecular Psychiatry claims to have settled the debate on whether the slight superiority of antidepressants in trials is due to side effects breaking blind. The principle author was quoted as saying: "once and for all, we've answered the SSRI question." Have they?
Study 329 Taper Phase
Most doctors still affect surprise at the idea SSRIs might come with withdrawal problems. Regulators knew very clearly since 2002 about the problems, but have decided to leave any communication of these issues in company hands.
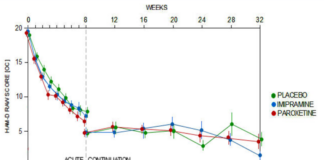
Study 329 Continuation Phase
All the fuss about Study 329 centers on its 8-week acute phase. But this study had a 24-week Continuation Phase that has never been published. Until Now.
Rising Rates of Suicide: Are Pills the Problem?
If you’ve read recent reports that state “US suicide rates surge to a 30 year high,” you might first justify the reality with the fact that things feel very wrong in our world today. On a personal, national, and planetary level, people are suffering to survive and the distress is coming from all sides – medical to economic to existential. But you probably also wonder why more people are choosing this permanent and self-destructive path, and feel compelled to submit to seemingly logical appeals to provide these individuals more help and greater access to treatment. Surprise: that may be the last thing our population of hopeless and helpless needs. Life’s inevitable challenges are not the problem. It’s the drugs we use that are fueling suicide.
Who Will Guard the Guardians of Psychiatry?
The assertion that the so-called antidepressants are being over-prescribed implies that there is a correct and appropriate level of prescribing and that depression is a chronic illness (just like diabetes). It has been an integral part of psychiatry's message that although depression might have been triggered by an external event, it is essentially an illness residing within the person's neurochemistry. The issue is not whether people should or shouldn't take pills. The issue is psychiatry pushing these dangerous serotonin-disruptive chemicals on people, under the pretense that they have an illness.
Restoring Study 329: Letter to BMJ
When we set out to restore GSK’s misreported Study 329 of paroxetine for adolescent depression under the RIAT initiative, we had no idea of the magnitude of the task we were undertaking. After almost a year, we were relieved to finally complete a draft and submit it to the BMJ, who had earlier indicated an interest in publishing our restoration. But that was the beginning of another year of peer review that we believed went beyond enhancing our paper and became rather an interrogation of our honesty and integrity. Frankly, we were offended that our work was subject to such checks when papers submitted by pharmaceutical companies with fraud convictions are not.
“Why You Should Stop Taking Your Antidepressants”
The New York Post reprints an excerpt on antidepressants from the latest book by MIA contributor, Kelly Brogan, MD, “A Mind of Your Own:...
“The Mystery of When to Stop Antidepressants”
Researchers are studying whether psychological treatments can prevent relapse after patients go off antidepressant medication, reports the Wall Street Journal, noting that "SSRIs have long been...