Tag: evidence-based medicine
Jon Jureidini–Evidence-Based Medicine in a Post-Truth World
In this interview, Jon Jureidini talks about the issues with evidence-based medicine and describes what led to the debasement of a system originally conceived to challenge extravagant claims and poor science.
The Cochrane Tapes Reveal a Horrendous Show Trial Against a Critic...
Why did Cochrane expel one of its best known scientists, who had helped get Cochrane started and bolstered its reputation? What happened that day?
Assessing Outcomes at the Alternative to Meds Center: Survey Results Prove...
I am often contacted by organizations seeking help with documenting how their efforts make a statistically significant difference when it comes to their clients’ success. Let’s take a look at some of the essential aspects that must be considered for those seeking documentation of evidence-based treatment.
Treatment Guidelines Should Not Be Written by Professional Societies and Insiders
John Ioannidis, a leading expert on research methods, takes a critical look at the way professional societies write treatment guidelines.
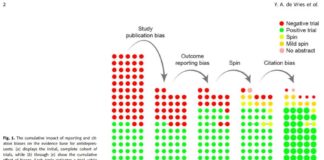
Publication Bias Inflates Perceived Efficacy of Depression Treatments, Study Finds
Researchers report the cumulative effects of major biases on the apparent efficacy of antidepressant and psychotherapy treatments.
Sami Timimi and John Read: Royal College of Psychiatrists, Latest Update
An interview with Professor Sami Timimi and Professor John Read who provide an update on a complaint made to the UK Royal College of Psychiatrists by a group of thirty academics, psychiatrists and people with lived experience.
“Evidence-Based Medicine”: Corporate Medicine’s Instrument
From Medium: The notion of "evidence-based medicine" is that a particular treatment is considered effective if research finds it safe and efficacious in the majority...
Has Psychiatry Gone Uniquely Astray?
Science is supposed to be evidence-respecting and thereby open-minded; psychiatry is presently not. But is psychiatry really unique in this respect? Is it the only field of medicine where dogmatically held theories contrary to evidence have held sway for long periods?
A Memoir of Chronic Fatigue Illustrates the Failures of Research
From The New Yorker: In her new book Through the Shadowlands, Julie Rehmeyer chronicles her struggles with chronic fatigue syndrome, or systemic exertion intolerance disease (S.E.I.D.),...
Is Evidence Based Medicine a Form of Microfascism?
In this post for BMJ Opinion, Richard Smith critiques a 2006 paper condemning evidence based medicine as an exclusionary, colonizing form of microfascism that promotes a...
Undisclosed Financial Conflicts Endemic in Clinical Practice Guidelines
While there has been a recent push to account for financial conflicts of interest in medical research, less attention has been paid to organizations...
Interview: Researchers Deconstruct Ghostwritten Industry Trial for Antidepressant
Researchers, Jon Jureidini, Jay Amsterdam and Leemon McHenry, have taken a closer look at the data from a randomized control trial of citalopram (Celexa) that was ghostwritten and then used by the manufacturers to support claims of the drug’s efficacy and safety in the treatment of child and adolescent depression. To get the background on this story, we connected with Dr. Leemon McHenry, an investigator in this study and a lecturer in philosophy at California State University, Northridge.
Lancet Editorial Points to “Trouble with Psychiatry Trials”
While clinical trials make up the “bedrock of evidence-based medicine” in other specialties, psychiatry faces a number of both ethical and scientific problems related to its use of randomized control trials. According to a new editorial in The Lancet Psychiatry, the field of psychiatry research has particular problems with ethical issues in recruitment, inaccurate classification systems, and controversial placebo comparisons, and then, once the studies are finished, it often remains unclear what the “outcomes actually mean for people’s lives.”
Epidemiologists Decry Major Problems in US Psychiatric Practice
In an exchange published in the Journal of Clinical Epidemiology, researchers take turns highlighting major problems in the way psychiatry is currently practiced in the United States. In response to an article by Vinay Prasad calling for an insistence on randomized control trials in “evidence-based” medicine, Jose de Leon, from the Mental Health Research Center at the University of Kentucky begins the back-and-forth by pointing out that this type of evidence has been detrimental to the field of mental health.
Has Evidence Based Medicine Been Hijacked?
John Ioannidis claims that the idea of evidence based medicine has been “hijacked to serve agendas different from what it was originally aimed for,” in a newly published critical essay in the Journal of Clinical Epidemiology. Ioannidis frames the essay as a continuation of a conversation with David Sackett, widely considered the founder of evidence based medicine.
Life, Unarmed
When I was born, everyone was expecting me to have arms. The doctor's mind raced; how am I going to tell this mother and the father that their son has hands but not arms? If he's missing so much in his extremities, mustn’t he also be missing a mind? My mom looked into my eyes and knew - in a way that only mothers know - that I had a mind, and spirit.
New Research into Antipsychotic Discontinuation And Reduction: the RADAR programme
For a long time I have felt that there just isn’t a good enough and long enough study on the pros and cons of long-term antipsychotic treatment versus reduction and discontinuation in people who have psychotic disorders, including those who are classified as having schizophrenia. Moreover, there are increasing reasons to be worried about the effects of long-term treatment with antipsychotics. I put this case to the UK’s National Institute of Health Research recently, and proposed that they fund a trial to assess the long-term outcomes of a gradual programme of antipsychotic reduction compared with standard ‘maintenance treatment.’ The NIHR agreed that this was an important issue, and that a new trial was urgently needed. The RADAR (Research into Antipsychotic Discontinuation And Reduction) study officially started in January 2016.
Overtreatment, Bereavement, and Antidepressants
A recent paper argues that prescribing antidepressants shortly after the death of a loved one is problematic . . . and a few days later, a Harvard academic publicly suggests prescribing antidepressants FOR bereavement. Wait, what?
What a new role for psychiatrists might look like
People have been wondering on this site lately if there is still a role for psychiatrists. The short answer is maybe, if they can...
The American Psychiatric Association’s Response to 60 Minutes: Where is the...
The American Psychiatric Association (APA) has posted a response to the 60 minutes segment on Irving Kirsch and the placebo effect in antidepressant research. But is their response based on scientific data?
Revising the History of the Serotonin Theory of Depression?
Did scientists recently discover that the Serotonin Theory of Depression is false? Or has this been known for decades? We investigate.