I have written the names Martin Harrow and Thomas Jobe so many times that I had almost come to view them as an indivisible pair. Which is why, when Jobe’s partner Anna Weaver texted me a week ago Wednesday telling of his death, I had a difficult time believing it could be true.
Harrow and Jobe’s study of the long-term outcomes of psychotic patients, a research effort that began in the 1970s, when Thomas Jobe was a newly minted psychiatrist, is, in my opinion, the most important research that has been conducted since the arrival of chlorpromazine in asylum medicine in 1955. It belies the conventional narrative that has driven societal care since that time and demands that we rethink everything that psychiatry has told us about its drugs.
Jobe’s death on March 16 came suddenly. A bout of Covid (he was “triple vaxxed”), then the eruption of shingles, followed by abdominal complications—apparently a case of enteric zoster which went undiagnosed. A few weeks earlier, he had still been meeting regularly with Harrow, discussing their ongoing publication of results from their longitudinal study. Every other Sunday, they met at 4 p.m. on Zoom to discuss their research, together with a third person—Cherise Rosen—who had joined their effort in recent times. They had three papers under review, and as always, there were ongoing matters to discuss related to the resistance to their work, particularly when it encroached on pharmaceutical interests.
“We haven’t given up. We keep going. We are still going,” Harrow said. Tom’s death “is a loss for all of us.”
A loss for all of us . . . that is how I feel. My life for the past 15 years would have been dramatically different if it weren’t for their work, and, it’s fair to say, without their work Mad in America may have never sprung into being.
In 2007, they published an article on the 15-year outcomes of the 145 patients in their longitudinal study, and they reported that among the 64 diagnosed with schizophrenia, the recovery rate was eight times higher for those off antipsychotic medication than for those on such medication. I had been contemplating doing a book that investigated the long-term outcomes of patients diagnosed with various major mental disorders, and it was that study that prompted me to believe this would be a worthwhile project, which led to my book Anatomy of an Epidemic. And that in turn led to the creation of this website, which we founded in part to promote findings such as theirs that were never covered in the mainstream media.
Since that 2007 report, they have published a number of papers that have deepened our societal understanding of how the long-term fate of those off medication diverged from those on medication, and their findings—while regularly discounted and dismissed by those intent on maintaining conventional beliefs—told of hopeful new possibilities for those who suffered a psychotic break and were eventually diagnosed with “schizophrenia.” Their findings told of many who had a “time of schizophrenia” and, after getting off antipsychotic medication, eventually recovered and returned to work, enjoying a decent social life too.
“We interviewed patients for up to 20 years, and we found that in a year, a year and a half, or two years after they get out of the hospital, those not on phenothiazines (antipsychotics) start to do better than those who are on them,” Harrow said.
Their work has been a gift to all of us. Their research told of different possibilities, of hopeful possibilities if the mainstream would just grab onto them, and that is the trail of evidence that their 40-year collaboration wrought.
A Student of Szasz
Thomas Jobe, who was born in 1943, majored in philosophy and biology as an undergraduate at Vanderbilt University, and he retained a love of both subjects throughout his life. While earning his medical degree at the University of Chicago Pritzker School of Medicine, he decided to focus on neurology and psychiatry as the specialties he would pursue, the latter because of his interest in philosophy and the nature of the human mind.
His father was a surgeon in the Navy, and he “told him if you want to go into psychiatry, you have to go study with Tom Szasz,” Weaver recalled.
Today—and this has been true ever since American psychiatry adopted its disease model when it published DSM III—Szasz is dismissed by most as a wrong-headed figure, but in the 1960s his book The Myth of Mental Illness was praised in such mainstream publications as Atlantic and Science. The latter publication touted his treatise as “enormously courageous and informative . . . bold and often brilliant.”
Jobe completed his psychiatric residency at SUNY Upstate Medical Center in Syracuse, NY in 1973. What he gained from Szasz, Weaver said, was a passion for “critical thinking. He challenged accepted wisdom.”

After finishing his residency, Jobe spent two years as a Navy psychiatrist. He then returned to Chicago, where he did postgraduate work in the history of science and medicine at the Morris Fishbein Center at the University of Chicago, the subject a love of his, he once wrote, “since high school.” He had a joint faculty appointment in the history and psychiatry departments at the Fishbein Center, where he had the joy of teaching the “history of neuroscience.” In 1978, he moved to the University of Illinois at Chicago, where he co-founded a neuropsychiatry program. There he regularly observed and treated patients in an inpatient unit with psychiatric symptoms following neurosurgery and patients with neurodegenerative diseases who were experiencing psychosis and other psychiatric difficulties.
As his enduring interest in neurology revealed, while he may have developed his “critical thinking” skills at SUNY Upstate, he retained a focus on the “biology” of the mind. During his career he authored more than 180 articles and four books on such topics as brain imaging, brain modeling, traumatic brain injury, stroke and neurodegenerative disease. He edited a book titled Clinical Neuropsychiatry.
He also co-authored books related to the lives of two presidents, Lyndon Johnson and John F. Kennedy. Meanwhile, his studies in philosophy, neurology and psychology ultimately led him, as an online bio states, to develop “a theory of brain plasticity, termed synaptopoiesis, that relies on the transfer of mRNA polyribosomes from the postsynaptic spine of the dendrite into the presynaptic bouton of the connecting axon.” He also “applied fuzzy logic to a theory of cortical engram representation and cortical computation.”
Those who knew him—Harrow and others—describe him as “extremely brilliant,” and yet, at the same time, “super modest.”
“He had such an appetite for knowledge,” said his son Will. “He was always so excited to delve into something new. Books, fuzzy logic, Plato and his cave, virtual representations (of the self), the Matrix . . . if you got him started talking on a topic, he was so gifted. He could explain anything to anybody. He had a Socratic method of talking with you.”
The Chicago Follow-up Study
By the time Jobe landed in Chicago, Martin Harrow had already obtained an NIMH grant for an ambitious longitudinal study, primarily of psychiatric patients treated at Michael Reese Medical Center in Chicago. Harrow, who had received his Ph.D. in psychology from Indiana University in 1961, had grown up in New York City, and his particular brilliance had shown up earlier in chess tournaments. He placed in the top seven at the U.S. Open Chess Championship three times, and he twice drew in tournament games against Bobby Fischer, who was destined to claim the title of world chess champion when he defeated Boris Spassky in 1972.

After graduating from Indiana University, Harrow spent 11 years on the Yale faculty before moving to Chicago in 1973 to take a position as a Professor at the University of Chicago and as the director of the psychology program at Michael Reese. Jobe knew of his research, and after they met, he joined Harrow’s research project, a collaboration that endured more than 40 years and was still flourishing up until his death.
“Tom was extremely literate and knew the literature well,” Harrow said. “He was an extremely brilliant man, and we had a common interest. A lot of what I wrote, he contributed to, and vice versa. We got along very well.”
As for their longitudinal study, Harrow added, Jobe “brought a modern aspect to our thinking on medication.”
During the 1970s, when Harrow obtained NIMH funding for his longitudinal study, the question of the long-term merits of antipsychotics was still a hot issue. The NIMH funded four other studies during that decade on this topic, and each reported findings that were consistent with the conclusion that, on the whole, the drugs worsened long-term outcomes for those diagnosed with schizophrenia and other psychotic disorders. To wit:
- In a retrospective study of the five-year outcomes of first-episode psychotic patients treated at Boston Psychopathic Hospital, Sanbourne Bockoven found that those treated with neuroleptics had a higher rate of relapse and were more socially dependent than a similar cohort of patients treated prior to the arrival of neuroleptics.
- In a randomized study of 80 young male schizophrenia patients admitted to Agnews State Hospital in California, Maurice Rappaport found that at the end of three years those who had been treated in the hospital without neuroleptics and stayed off the drugs following discharge—24 of 41 patients randomized to the non-drug group in the hospital—had dramatically better outcomes than those who were treated with neuroleptics in the hospital and remained on the drugs. The never-medicated group were much less likely to have relapsed and had remarkably better functional outcomes.
- The head of schizophrenia studies at the NIMH during this period, Loren Mosher, ran his well-known Soteria Project, which compared conventional drug treatment in a hospital with treatment in a homelike setting where antipsychotics were used in a selective, minimalist fashion. He reported better two-year outcomes for the Soteria patients.
- The fourth study of schizophrenia patients was led by William Carpenter. It was conducted at the NIMH’s clinical research facility in Bethesda, Maryland. Those treated without drugs were discharged sooner, they had a lower relapse rate at the end of one year, and they also suffered less from depression, blunted emotions and retarded movements. The findings led Carpenter to raise a haunting question: Was the use of neuroleptics making patients “more vulnerable to future relapse than would be the case in the natural course of the illness?”
The study launched by Harrow was, in many ways, the Granddaddy of this research effort. He and Jobe enrolled 200 psychotic patients into their prospective study, recruiting them from two Chicago area hospitals, one private and one public (Michael Reese Hospital). Theirs was a young cohort, with a median age of less than 23 years, and they were following them from an early point in their illness: 67% were in the hospital for the first or second time. Harrow and Jobe followed them for the next 20 years, periodically assessing their status and use of antipsychotics (at 2, 4.5, 7.5, 10, 15 and 20 years).
This type of longitudinal research had a valued—and even hallowed place—in the history of medical research. In the 1890s, German psychiatrist Emil Kraepelin had systematically tracked the outcomes of patients at an asylum in Estonia, and it led him to conclude that psychotic patients who presented with a lack of emotion regularly deteriorated into dementia, an illness he described as dementia praecox, while those who presented with affect (mania, depression, or both) had fairly good long-term outcomes. Usually, “all morbid manifestations completely disappear” he wrote, with this group said to suffer from “manic-depressive” illness.
Harrow and Jobe’s longitudinal study was cast in that same mold, and given that modern psychiatry regularly cites Kraepelin for his groundbreaking findings, their results could be expected to provide an understanding that couldn’t be gleaned from short-term randomized trials. Harrow and Jobe weren’t focused solely on the effects of antipsychotics, but rather were intent on describing the long-term course of psychotic patients in modern times and identifying factors that affected that course. Given that antipsychotics are expected to alter outcomes over the long-term, they could expect to find a difference in those who regularly took the medications compared to those who did not.
If the conventional wisdom held true, those who regularly took the medications would fare much better over time. Yet, if the NIMH-funded research during the 1970s held true (e.g. the findings from the studies mentioned above), then those who continually took the medications could be expected to have higher relapse rates and much worse social functioning.
Their findings would fit into that larger research context. If the fate of those off medication and on medication noticeably diverged, their findings would provide a definitive answer to the haunting question raised by those four NIMH-funded studies, all of which suggested that antipsychotics, in the aggregate, worsened long-term outcomes.
Their Findings
Even in short term trials of antipsychotics, researchers struggle to keep their schizophrenia patients in the studies until their end. Patients often drop out within a few weeks, such that researchers regularly use a method called “last observation carried forward” (LOCF) to assess whether a patient, when last seen, had improved on the study drug compared to placebo. The LOCF findings are then incorporated into the analysis of a drug’s efficacy.
In contrast, Harrow and Jobe still had 145 of their 200 patients in their study at the end of 15 years, a retention rate of 77%. They had managed this exceptional result by regularly staying in touch with the study participants even after they had dropped out of psychiatric care, and that was key to their findings. Psychiatrists rarely see this group of patients when they do well, and thus their long-term outcomes remain hidden from public sight. What Harrow and Jobe discovered was that those who got off medication—and this was true even for those who stopped taking medication while actively psychotic—were much more likely than those who stayed on the drugs to recover, which included remaining stable and returning to work.
In 2007, they published a comprehensive report on the 15-year outcomes of the 145 patients still in their study, 64 of whom had a diagnosis of schizophrenia and 81 who had initially been diagnosed with milder psychotic disorders. At the end of two years, the group not on antipsychotics were doing slightly better on a global assessment scale than the group on the medications. Then, over the next 30 months, their collective fates dramatically diverged.
At the 4.5-year mark, 39% of those off medication were in recovery, and more than 60 percent were working. In contrast, outcomes for those on medication worsened during this period. At the 4.5-year follow-up, only 6% were in recovery and few were working. Those divergent outcomes remained for the next ten years. At the 15-year assessment, 40% of those off medication were in recovery, more than half were working, and only 28% suffered from psychotic symptoms. As for those on antipsychotic medication, only 5% were in recovery, and 64% were actively psychotic.
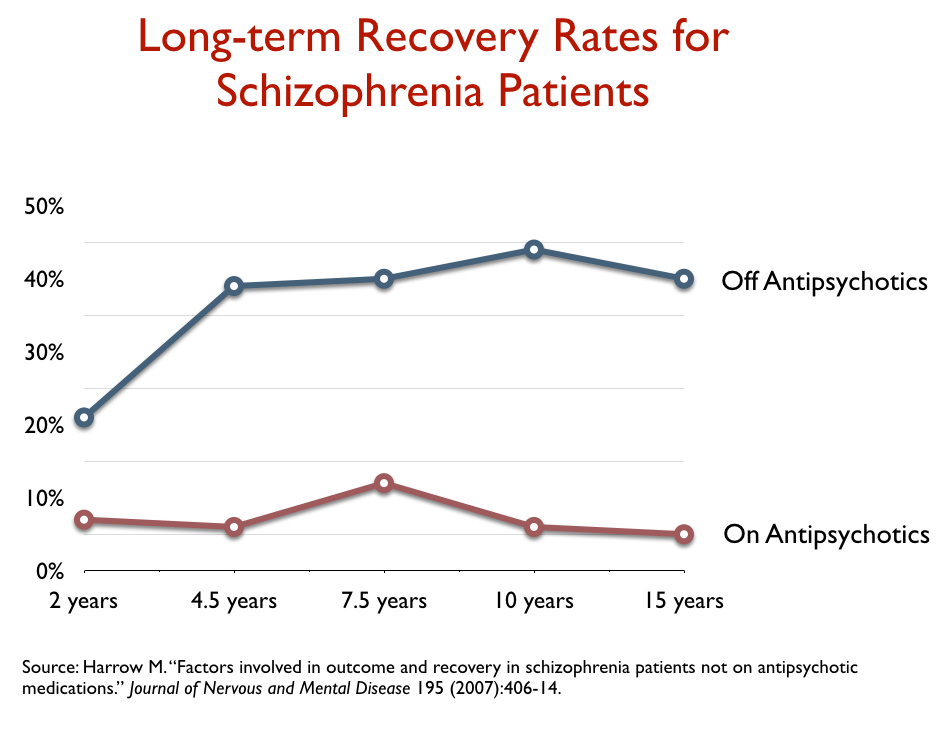 Outcomes for the 81 patients initially diagnosed with a milder diagnosis were of a similar sort: those who got off medication were much better than those who stayed on the drugs. In fact, the 15-year outcomes for schizophrenia patients who got off antipsychotics were better, on a global assessment scale, than those with a milder diagnosis who stayed on the drugs. This was clear evidence that long-term use of antipsychotics had a deleterious effect.
Outcomes for the 81 patients initially diagnosed with a milder diagnosis were of a similar sort: those who got off medication were much better than those who stayed on the drugs. In fact, the 15-year outcomes for schizophrenia patients who got off antipsychotics were better, on a global assessment scale, than those with a milder diagnosis who stayed on the drugs. This was clear evidence that long-term use of antipsychotics had a deleterious effect.
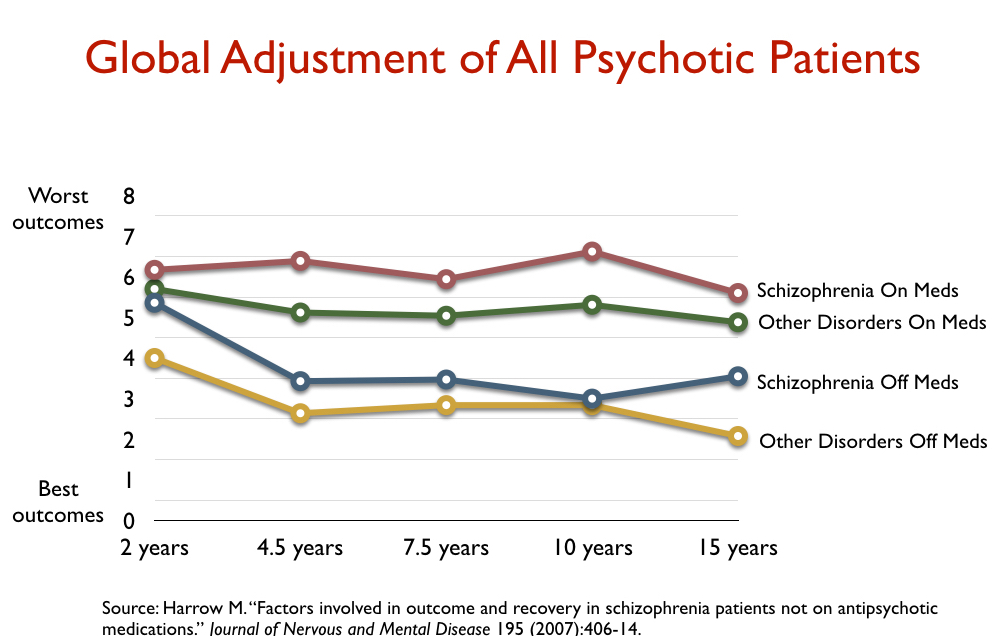
Their results, while telling of great harm done with current protocols for prescribing antipsychotics, had nevertheless illuminated a hopeful possibility for those who suffered a first episode of schizophrenia or psychosis. Those who had gone off antipsychotics and done well had disappeared from societal view, but Harrow and Jobe, by keeping in touch with them, revealed that a “good outcome” was much more common than anyone knew.
A few in the schizophrenia cohort even had high-level jobs—one became a college professor and another a lawyer—and several others had “mid-level” jobs. As Harrow told me when I was researching Anatomy of an Epidemic, “We [clinicians] get our experience from those who leave us and then come back because they relapse. We don’t see the ones who don’t relapse. They don’t come back. They are quite happy.”
In their 2007 article, Harrow and Jobe did not attribute the worse outcomes for the medicated patients to the medication. Instead, they wrote that their study was evidence that there was a significant percentage of schizophrenia patients—those with a good initial prognosis—who could get off the drugs and fare fairly well over the long-term without them. Their 2007 finding argued for selective use of the medications, but even this dent in the conventional wisdom was not well received by most of Jobe’s peers in psychiatry.
“Tom observed that that their research was basically unwelcome,” Weaver recalled. “What I always admired about both of them (Martin and Tom) was that they persisted in the face of this criticism.”
Fleshing out their Results
After publishing their 15-year results, Harrow and Jobe obtained funding from the Foundation for Excellence in Mental Health Care to continue their analysis of data from their longitudinal study. They subsequently published a number of articles that explicitly focused on the long-term effects of antipsychotics.
In their reports, they revisited the dopamine supersensitivity theory as an explanation for why antipsychotics, over the long term, increase the risk that patients will suffer repeated relapses and become chronically psychotic. That theory was first proposed in the late 1970s as an explanation for research findings that told of higher relapse rates for medicated patients. For Jobe, drug-induced dopamine supersensitivity provided a biological explanation for why psychotic patients would be more vulnerable to relapse over the long-term.
In their various publications, Harrow and Jobe compared outcomes for those who got off antipsychotics by year two and stayed off them throughout the study to those who were medication compliant throughout the study. This comparison helped further isolate the long-term effects of antipsychotics, and the difference in their fates was dramatic on every domain measured.
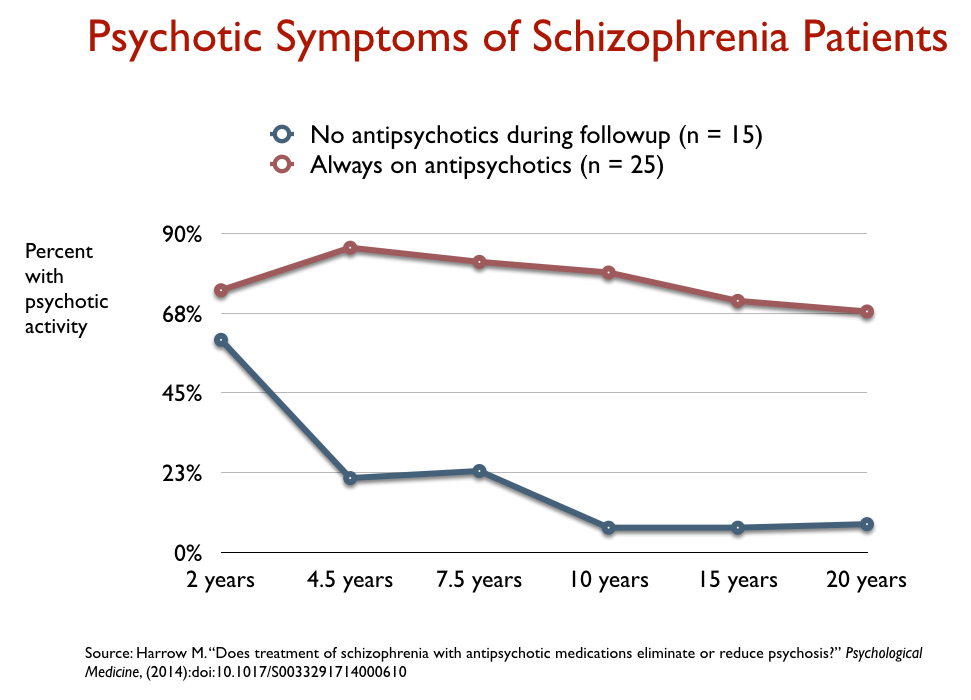
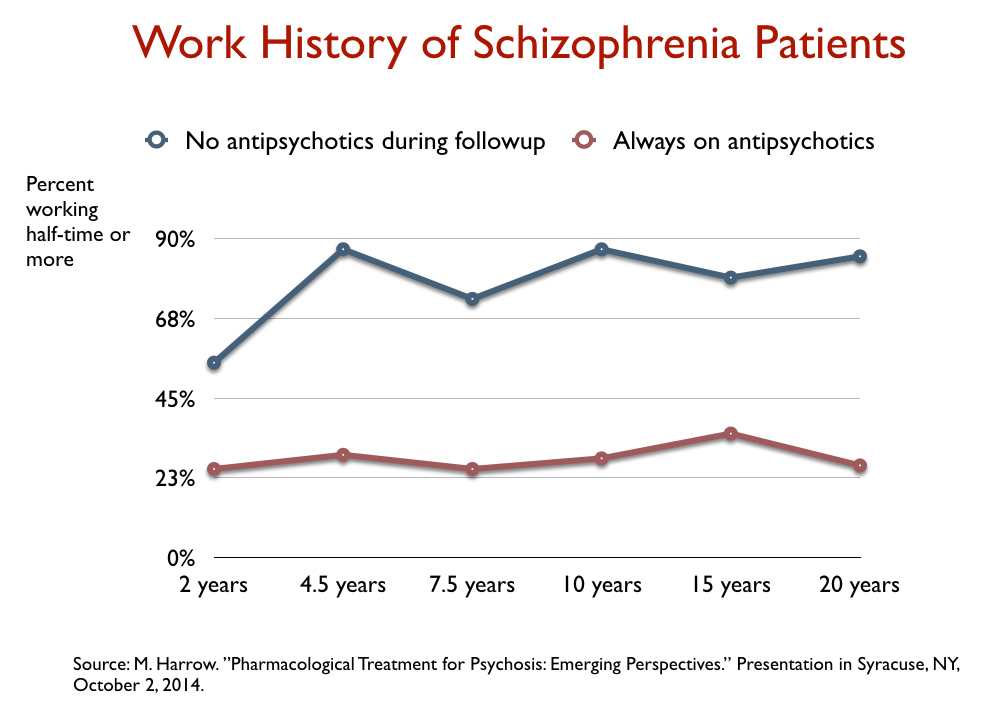 They also looked at whether a difference in initial prognosis could explain the divergent outcomes, and found that in every group—those with a good initial prognosis, those with a bad initial prognosis, and those with a milder diagnosis at baseline—the off-medication group had better long-term outcomes. In a 2021 paper, they determined that after such factors were accounted for, those off medication—at every assessment—were six times more likely to be in recovery than those on medication.
They also looked at whether a difference in initial prognosis could explain the divergent outcomes, and found that in every group—those with a good initial prognosis, those with a bad initial prognosis, and those with a milder diagnosis at baseline—the off-medication group had better long-term outcomes. In a 2021 paper, they determined that after such factors were accounted for, those off medication—at every assessment—were six times more likely to be in recovery than those on medication.
While their papers did get published and stirred further discussions in the research literature, their findings were mostly dismissed, and kept out of public view and out of psychiatric textbooks.
“We have the data, and the data is solid,” Harrow said. “There are a lot of publications. But they are not highlighted (in textbooks); they are not advertised (to the public.) Most people ignore it, it doesn’t fit the times. They don’t see the data, and most who do shrug it off, say it’s just chance or whatever.”
Psychiatry, he added, “has an enterprise that is good for them, and if you think making money is important to a group, to an enterprise, then [maintenance drug therapy] works for them. And when you use phenothiazines in the acute stage, they partly work, but after a while, patients on phenothiazines eventually relapse. But [clinicians] just see it as part of schizophrenia (as opposed to being an effect of the drugs.)”
The influence of drug companies is also a factor, he said. “Drug companies of course don’t want to think that their drugs aren’t helpful after two years. This threatens their money supply and this is the one class of drugs thought to work, and they are very profitable. Let’s not kid ourselves. The phenothiazines are very financially successful medications.”
The Legacy of Their Research
If Harrow and Jobe had come up with the opposite results, with a recovery rate eight times higher for those on antipsychotics than for those who stopped taking the drugs, the American Psychiatric Association, the “thought leaders” in the field, and the drug companies would have trumpeted the results and the quality of their study. The public would have learned how important longitudinal studies are for understanding long-term outcomes and how extraordinary it was that Harrow and Jobe still had 77% of their patients in their study at the end of 15 years. Here was definitive proof that maintenance use of antipsychotics is a very helpful—and necessary—practice.
But since the results upended conventional wisdom, the defenders of the faith have instead found refuge in criticisms that could best be described as dismissing the findings with a figurative wave of the hand. This wasn’t a randomized trial; the difference in outcomes could have been due to chance; this is a study that tells of correlation and not causation; and so forth. The criticisms tell of a guild’s allegiance to maintaining current beliefs and practices, and an inability to respond, with an open mind, to findings that would require changing those practices.
Harrow and Jobe’s research arose during a time when other NIMH studies were raising questions about the long-term effects of antipsychotics, and today, their findings fit into a larger collection of research published since that time. To wit:
- World Health Organization studies determined that longer-term outcomes were much better in two “developing countries,” India and Nigeria, where few people diagnosed with schizophrenia were maintained on antipsychotics, than in the U.S. and other developed countries where maintenance use was the common practice.
- MRI studies of brain volumes determined that antipsychotics shrink brain volumes, and this shrinkage is associated with functional impairments and an increase in negative symptoms.
- Longer term studies in Finland, Germany, Denmark and Australia have all reported higher recovery rates for schizophrenia/psychotic patients who get off antipsychotic medication.
Indeed, in a 2018 paper, Harrow and Jobe identified eight studies that assessed whether “schizophrenia patients improve when treated longer than two or three years with antipsychotic medication,” and “none of them showed positive long-term results.”
In sum, their study is not an outlier in the research literature. Instead, it occupies the featured place in a larger body of research, stretching across five decades, all telling the same story: over the long-term, antipsychotics increase relapse rates and worsen functional outcomes, at least in the aggregate.
Yet, in the conventional narrative, these are the class of drugs said to have made it possible to empty the asylums and to have initiated a “revolution” in the care of the seriously mentally ill. This is why their longitudinal study is the most important research conducted in the psychopharmacology era. It tells of how that narrative of progress is a societal and professional delusion, and how the field, if it is going to do right by its patients, needs to fundamentally rethink that narrative.
That is the extraordinary legacy of their work.
Although their findings have mostly been kept out of public sight, their work has spurred, at least in a few corners of the research literature, a discussion of the long-term effects of antipsychotics, and there has been an acknowledgement that there is a lack of evidence that antipsychotics improve long-term outcomes. The needle has shifted to that degree.
Moreover, in a few select countries, their research has helped stir real-world change. In Israel, Soteria homes are springing up, and one reason is that Harrow and Jobe’s research has shown, at the very least, that some people diagnosed with psychotic disorders can do well off the medication. Soteria provides a possibility for that outcome. In Norway, user groups lobbied the Health Ministry to create medication-free treatment in the country’s four hospital districts, and they put forth Harrow’s and Jobe’s finding as an evidence-based reason to do so.
Then there was the power of a simple graphic. Ole Andreas Underland, a psychiatric nurse, was at a conference where a user group presented the graphic showing an eight-fold higher recovery rate for those off medication, and that stirred him to create what he describes as a “medication-free” treatment center outside Oslo (although much of the effort is devoted to helping chronic patients taper from their drugs.)
Harrow, who is 88, said he worries about “fading away” now that Tom is gone. But shortly after I spoke with him on Sunday, he was getting ready to meet with Cherise Rosen. They have longitudinal data on 400 patients treated at Michael Reese Hospital, and they see further revelations that can come from that resource.
A Life Well Lived
Jobe retired from an active practice in 2006. His wife Patricia died in 2011, and after he and Anna Weaver found each other—she was “a dear friend,” he once wrote—she encouraged him to remain engaged with the longitudinal research.
Tom, she emphasized, had always sought to provide care to poorer populations in Chicago. He should be remembered for that too, she said. Even after he retired, people and families struggling with mental health difficulties would reach out to him for help and guidance. One father of a 20-year-old son wrote to her after learning of this death, telling of how “the support that [Tom] provided to our family with deep knowledge, empathy and perspective was uniquely helpful. He was a beacon of understanding and hope when we couldn’t understand what was happening to us.”
In the last decade, Jobe had continued his philosophical and neurological explorations of the human mind, of modeling consciousness, and in the last few years, he had begun writing a biography of Szasz.
“Szasz was important to him, but there were a lot of people important to him,” Harrow said. “He really was a brilliant guy, who was open to new ideas.”
That is a sentiment—of being open to new ideas—that would seem a fitting gravestone epitaph for a scientist who, in his collaboration with Harrow, upended a psychopharmacology narrative that has governed societal thinking for more than six decades.
***
MIA Reports and essays are supported, in part, by a grant from the Open Society Foundations.


A fitting tribute.
Of course the money side is important but that gets over emphasised at the expense of the real reason that the damaging drugs are still used … “I wanted to become part of a collective voice demanding change in a world that often made no sense to me, a corrupt and crazy world, which frequently exploits the vulnerable and protects the powerful. I saw that there are many complex forces at play and that the mental- health system is part of a larger system of denial operating within our society.” – Dr Jacqui Dillon head of the Hearing Voices Network in De-medicalising Misery. The social causes; poverty, discrimination, abuse and many others are ignored and replaced with “illness” for the very reason that that is what covers up what these rich, industrialised “rational” societies can’t face and what perpetrators want covered up. There are serious problems with organised crime and corruption and lack of humanity, empathy and compassion. It’s just too scary to face so it’s easier to convert it into that term “MH” and throw out the context. Mary Boyle wrote very eloquently about this in “Making the world go away”. But the one who really cracked it was the Italian psychiatrist Franco Basaglia. Society, but also many campaigners, need to divest themselves of the idea that its only all about money.
Report comment
Bob, Michael and those who are reading the column: Thank you for writing the testimonial about Jobe. And also to reference the story of how he developed and the impact that challenged you to act! The rich expressions and responses to a reality that carries with it a measure of hope is remarkable. The Long Term is a natural stance in which to understand change. As Harrow surmised, Jobe apparently had a gift of staying in the space akin to the gap, while trying to understand the architecture as well as the source of the spark.
Not only Thomas Jobe’s Legacy but yours and many who afford witness and a method by which to further the discourse.
Report comment
Hi Bob,
I’m very sorry to hear about Thomas Jobes passing. He certainly contributed to the prospect of genuine recovery and a full return to normal life.
I have have never heard ‘voices’ myself, even though these symptoms were represented as evidence against me. Nor I believe, could I be judged to be delusional by doctors who didn’t even get the countries I had been in right.
But after taking “Strong Psychiatric Medications” for a number of years I found it near enough impossible to stop taking the “medìcations” when I was given permission to stop.
So regardless of “Original Schizophrenia” – Psychiatric Drugs in my estimation, do cause “Schizophrenia”. In the same way maybe, that valium causes long term valium dependency. The other thing is that Strong Psychiatric Drugs (of a type used in “Schizophrenia”) are profoundly disabling.
To cope with my Withdrawal High Anxiety I used a technique similar to below:
DISSOLVING THE PAIN-BODY: An excerpt from THE POWER OF NOW by Eckhart Tolle
(This technique works, costs nothing, can be easily understood, and does not require a therapist – just the ability to persist again and again).
Report comment
Thank you for this beautiful tribute to Thomas Jobe. He did important and valuable work and it stands as a testament to his commitment to helping people and to finding the truth through thoughtful investigation. We all benefit from the work of Jobe and Harrow. My condolences to his wife, friends, and family.
Report comment
I dont believe in death.
Anyone I have lost to them passing away is more with me than they could be in earth life. But I do believe in loss.
Mother Theresa said “We ourselves feel that whatever we are doing is just a drop in the ocean, but the ocean would be less because of that missing drop”.
Robert, the sea level rise is one drop less.
I came across link this in my algorhythm last week. It is no secret that I have different ideas from most here about what is causing my own schizophrenia. I feel that the antipsychotics I had poisioned me but I do not blame anyone for that. I do not blame anyone for teaching me chain smoke when I used to do that. But I am keen on correction of industrial errors. I do think antipsychotics should be radically curtailed to the point of hardly being prescribed. That said, I know a few people who went rapidly downhill when they tried to quit. The withdrawals probably cause that, but its a moot point what causes it if you cannot come off it. In my opinion the pills should never be prescribed except in dangerous circumstance. And only short term.
But I do not believe my schizophrenia was caused by medication. And I am not making it up. It is a very real torment on a daily basis.
My last MRI showed leisons that I do believe came from the years of antipsychotics. I live daily with the iatrogenic damage. But for ten years prior to my medication my schizophrenia was the same as it was on medication, and finally it has been the same after quitting. So although I have many additional effects from the lasting damage of my poisons, those symptoms are not my schizophrenia.
MRIs are pointing out brain shrinkage and an increase in all kinds of neurological states. But these are not schizophrenia, in my opinion. My schizophrenia is wholly “other”.
My illness is, I believe, from a disrupted brain, given that your article mentions how easily the brain can be given to negative symptoms, for instance on drugs. So, we know the brain is as delicate as a sea anemone, one touch and it quakes and spasms.
Science likes to hunt for causes to find cures. This leads it to promote a false “certainty” that keeps inventing new trash treatments. Seldom do scientists ever listen to the actual schizophrenic. It is as if the pursuit of the “logical” cure, that requires not listening to their illogical personal miseries becomes the deafening cure. Deaf ears.
I am so very sick of “certainty”. So now I just invent my own. Or rather I swap “certainty” in preference for “whimsy”. It is much safer. If doctors would be more “whimsical” instead of “logical” and “certain”, nobody would imbibe them pills. But I get it. Psychosis is a desperate thing. And nobody can handle the bawling desperate. A rag in the mouth now comes in a blister strip full of “certainty”.
So, I am not going to be “all certain” of where my schizophrenia comes from. I sense it as a subtle glitch in the meeting between by neurochemicals and my consciousness and my electrical brain waves. A domino effects of one subtle physical cause impacting another. I think brain waves are key. I recently found Tesla’s experiments on frequencies and vibraitions to be most illuminating. I listened to the 111 hertz fequency and it had a powerful effect on my brain. I felt like I was wearing a massive turban. I felt calmer. Maybe some brains are more succeptible to unravelling at discordant sounds in the environment. Or maybe stress activates brain wave malfunctions or electrical epilespy like distortions that cause the hallucinations of schizophrenia.
I have reason to think people may not agree. Some people I know want their brain to be uncorruptable and pristine and identical, as if blueprint good brain from a factory. But the rest of our bodies are not having to be flawless. My problem with the notion of the pristine brain is it draws on the idea of a tough, solid, lump of a brain that can never ever be succeptible. I just do not think that is true. The brain is supremely delicate, as fragile as a glass sponge. Which is why it has such dreadful damage from iatrogenic harm. It seems to me one cannot have it both ways, a tough robust organ that would work fine if left alone, and yet a frail disintegrating mess if given iatrogenic harm. It would be like saying your bladder is tough and strong until it gets swamped by chemicals. Sure the chemicals cause wreck and ruin, but that does not mean the bladder cannot be weak, in some people. Bladder/brain. Not everyone’s brain or body follows an ideal pattern or blueprint. My brain may be a rare never occured before anomaly.
I am all for ceasing any iatrogenic damage. I know antipsychotics are the work of the devil. I know people need better treatment, or better no treatment at all. Soteria seems wonderfully “wistful”. And I am not into everyone being so “certain” of everyone else’s brain. How absurd!
But I am firm in my knowing that what I have is schizophrenia. And I know it is not from medication, and it is not from any lurking trauma. Why it can irk me to hear people insist it must be from these contenders is it is like some stranger telling an asthmatic that their gasping for air is caused by not having friends.
On the subject of friends I caught a you tube video of Jordan Peterson interviewing a man of the mulsim faith. It was a beautiful testimony to how two “sides” that hotly disagree can share the identical joyful passion of what they feel “whimsical” about.
See if you can maybe catch it. I have been no devotee of Jordan Peterson’s landmark speeches, but I have to say this rowdy yet quiet and respectful interview was compellingly evocative of naked humanity.
Here is the link to the brain waves video.
https://youtu.be/T7v9InRW9wk
Report comment
Robert, here is the Jordan Peterson interview I mentioned. Ive been working on my theories on “certainty” for years, so it is was nice to hear it mentioned by JP.
And here is a different link. A friend with schizophrenia wrote to me about it.
It is called The Barber Shop. It is in surround sound 8D. It turns out to be a useful example of what living with hallucinations “feels” like.
Ordinarily a listener would sit in a low lit room and close their eyes and enjoy this farce on headphones and that be all.
But if you are willing to explore this may I suggest that you do the above but as you listen try to imagine you are suddenly psychotic and these “voices” are in the actual room with you, not in your head. And as you try to get into the role of stunned psychotic person, bring your awareness to the “movement” of the voices, more than just the voices. Be fixating on “anticipating” where they are in relation to your physical body. Imagine that the distance between you and a “voice” is on a long stretch of elastic. And the second “voice” is on a different long stretch of elastic. Why this matters to notice is because often for (my) schizophrenia it is not so much the “voices” that stir panic but it is more that the elasticity of their ever moving, bombarding, approaching, vanishing, leaping out, surprise attack quality that is the worst part of the psychotic hallucinations. The kinetic violation to one’s “body space”, an intimidating intrusion you are helpless to stop, that is what escalates the nightmare.
A sculptor once told me to make a clay sculpture of a plant. He said to look at the spaces inbetween the stems and include the spaces as if only doing a sculpture of the spaces. I was very young and silly and mocked him but in life I have found this unexpectedly useful. And in this moment, I suggest that whilst listening to the Barber Shop sound video that you try to become nervously hyper vigilant about the empty spaces where the “voices” are not, as much as the places where they are. This gives an idea of feeling dismay and loss of control of your immediate environment. You dont know what is going to leap out at you or “where”.
Imagine these “voices” harassing you at four am, or in a shop, or at the dentist, or kissing your friend goodbye at the airport, imagine the “voices” are there 24/7, month after month, year after year, decade after decade. Imagine the “voices” are not as cheerful as they are in this video, but are demanding you do things you dont want to do. And because they say they will give you a rest if you do such things, out of abject despair you do what they order you to. Until every day you are bombarded and doing what you do not want to do and trying to write a little comment here is having hallucinations swarm all over you, as “real” as the “voices” feel in this video link.
Then imagine someone else tell you they are “certain” you only hear “voices” because you have a wheat allergy like they do.
There is alot more to my schizophrenia symptoms, awful things too private to say. So I will leave it at this.
I just end on agreeing though that your dear friend was/is right! Antipsychotics help nobody.
(The Barber Shop)
https://youtu.be/oSgSEjoOMUE
(Jordan Peterson and Mohammed Hijab)
https://youtu.be/qgYMuRqXPr0
Report comment
Thank you, Robert, for this tribute to Thomas Jobe, which highlights the importance of his and Martin Harrow’s research findings.
For those of us who were lied to, coerced, and forced to take antipsychotics, then left to search for medical proof of how those drugs made us ungodly sick. Since the psychiatrists, and too many of the mainstream doctors, are unwilling to admit to what they were all taught in med school. Which is that the anticholinergic drugs – including the antidepressants and antipsychotics – can create “psychosis,” via anticholinergic toxidrome, in the short term.
I believe it is of paramount importance to continue to highlight Harrow and Jobe’s findings on the long run adverse effects of the antipsychotics. Since no one should ever be coerced or forced to take drugs that are medically known to make a person “psychotic,” and cause lots of long run harm, as well – and all under the disingenuous guise of “help.”
My condolences to Thomas Jobe’s wife, family, and friends. And, please know, Thomas’ work was, and is, very important to those of us who were harmed by psychiatry.
Report comment
After my two prior comments, this fleshes out the link between brainwaves causing illness/healing and how the vibration in sounds like Teslas 111 hertz frequency may be able to correct imbalances. I know some people fear the word “imbalance” because it can be used as an excuse for disciple or torture, but when I am feeling really ill myself from any virus or infection or illness “imbalance” is for me a useful acceptance that I am out of sorts. I can then try to do things in my environment to find whatever feels balancing TO ME. So, I like the notion Tesla had of vibration being effective at restoring balance. Sound is going to be significant. The negative effects of sound are being weaponized and things like infra sound and Havanah syndrome seem real enough. Dr Susan Greenfield is a neuro scientist who studied the link between emotions and brainwaves. She observed sonething unusual about schizophrenic people. Some, not all, had brain waves similar to children, in terms of being geniusly dynamic and super aware. The brainwave pattens were unable to “ignore” distractions bombarding them.
I know that may sound contentious since many who have schizophrenia do not want it and do not want the diagnosis and do not want themselves to be regarded as having drifted off from their “normal”, bevause for them being thought not normal is a whole other added suffering born of social inquisition. And of course everyone must cry out against the brain ever being seen as so un normal it needs “treated” by bogus lethal quackery. So we must protect the brain from all derogatory social judgement AND protect it from rotten cures. So we must have a…
“Hands Off Our Brains” placcard.
And yet…for me, and probably it is only me, I do not today feel my best “normal” for me. I am imbalanced to the extent I keep calling helplines. Some may say well I just need “kindness” as a treatment. I get kindness from loads of people all already. Some may say I just need therapy. I have spent most of my life getting therapy. I even become one. Some may say I need better medication. Im sorry but medication nearly exploded my heart.
So, I am imbalanced and not my “normal” and I suffer hourly and I want that to stop. I am not sure if (lets not call it treating my brain, but rather impressing my brain) if if if impressing my brainwaves with 111 hertz sound frequencies will improve my lot. But I am willing to gently and voluntarily experiment on myself. As one might experiment on ceasing blue light in the evenings. Doing nothing is not an option.
Here be a Tesla link.
https://youtu.be/4QB_ti8hLo8
And next is sound medicine.
https://youtu.be/rkG6duNAPic .
Report comment
Bob, thank you for making the effort to write this thoughtful, informative piece. Much appreciated!
Report comment