Is Xanax Really the Bad Guy?
While any effort to generate awareness and potentially curb the benzodiazepine epidemic is commendable, we have to ask ourselves, is Xanax just the scapegoat in this situation? Will legislative action and media attention for only one benzodiazepine out of so many make any difference?
Over 1,000 Antidepressant Users Describe how Their Personal Life has Been Affected
Survey examines adverse personal and interpersonal effects of antidepressants and the impact of polypharmacy
Danish Study Finds Better 10-year Outcomes in Patients Off Antipsychotics
Study finds that 74% of patients with a psychotic disorder off antipsychotics at end of 10 years are in remission.
The Monster in Our House: What Psychiatric Medication Did to My Father
When we eliminated his last psychotropic prescription, it was as if my father came back from the dead. All of the monster-like qualities that we thought were severe symptoms of his dementia have practically disappeared. We’ve found ourselves questioning whether he has dementia at all.
New Review Highlights Dangers of Electroconvulsive Therapy
Data shows that over a third of users experience permanent memory loss and that approximately half report not receiving adequate information about the risks from their doctors.
Use of Antidepressants Linked to Diabetes
Selective serotonin reuptake inhibitors (such as Prozac and Zoloft) are the most commonly prescribed medication for depression. SSRIs have long been associated with an...
Vitamin B6 Effective in Reducing Antipsychotic Induced Akathisia
A recent RCT showed that vitamin B6 is as effective as propranolol for the treatment of akathisia.
Victim Blaming: Childhood Trauma, Mental Illness & Diagnostic Distractions?
Why, despite the fact that the vast majority of people diagnosed with a mental illness have suffered from some form of childhood trauma, is it still so difficult to talk about? Why, despite the enormous amount of research about the impact of trauma on the brain and subsequent effect on behaviour, does there seem to be such an extraordinary refusal for the implication of this research to change attitudes towards those who are mentally ill? Why, when our program and others like it have shown people can heal from the effects of trauma, are so many people left with the self-blame and the feeling they will never get better that my colleague writes about below?
Mental Health Services Turned My Daughter’s Crisis into a Way of Life
My world turned upside down when my daughter nearly died from a serious suicide attempt. After several years as her caretaker I began to wonder: What can we do to change the way our mental health services are organized so they won't turn a crisis into a way of life for already distressed and vulnerable people?
Mad In America’s Chapters
Preface
The World Health Organization has repeatedly found that people diagnosed with schizophrenia in the U.S. and other developed countries fare much worse than schizophrenia...
Thou Shall Not Criticize Our Drugs
A medical journal is expected to promote an open-minded discussion of treatments, even if findings—or criticisms—threaten conventional beliefs. But the American Journal of Psychiatry will not find space for criticism even if it comes from one of the best-known psychiatrists in the world.
SMILES Study: Depression and Nutrition
The question this study asked was: In adults with depression who eat a poor diet, does teaching them about nutrition have an impact on their mental health? At the end of the 12-week intervention, the answer was: Yes.
Study of Online Antidepressant Forums Reveals Long Lasting Withdrawal Effects
Effects of discontinuing SSRIs and SNRIs reported on an online forum indicate significant and long-lasting withdrawal symptoms.
Dialectical Behavior Therapy Reduces Self-Harm and Suicide Attempts
A new meta-analysis finds that DBT reduces self-harm, suicide attempts, and reduces the frequency of psychiatric crisis service utilization.
Benzodiazepines Linked to Treatment Resistant Depression
Prior use of benzodiazepines, such as Xanax, Librium, or Ativan, may increase the risk of treatment-resistant depression (TRD), according to a new study published in The Journal of Nervous and Mental Disease.
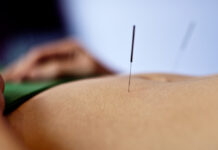
New Data Supports Acupuncture as a Treatment for Depression
Researchers found acupuncture effective in the treatment of chronic pain and depression
Reexamining Schizophrenia as a Brain Disease
Schizophrenia has occupied, and continues to occupy, a position of great import in psychiatry, and it is frequently used to assert the supposed biological nature of the field. What evidence is there to suggest that what we call schizophrenia is a disease of the brain? Surprisingly, very little.
Overcoming the Stigma of Depression
One of the roadblocks to recovery for those who suffer from depression is our culture's tendency to stigmatize depression and other mental health disorders. After my first hospitalization, I remember the dilemma I faced in trying to explain my three-day absence to my employer. If I told the truth—that I was being treated for anxiety and depression—I stood a good chance of losing my job. Instead, I reported that I had been treated for insomnia at a sleep clinic. In another instance, a client of mine who worked as a nurse was petrified of telling her colleagues that she dealt with depression, but when she shared her diagnosis of cancer, they showered her with with love and support.
Promoting Healing After Psychosis
It makes sense to be cautious about any kind of exploratory practice that might send someone who has been "psychotic" into another period of being lost and confused. But we should also beware the risk of trying to be too stable and "normal" after psychosis — the risk of avoiding the transformative work that might need to happen for that person.
New Study Examines User Experience of Discontinuing Psychiatric Medications
Researchers find that support and self-care were helpful for users during discontinuation, but that mental health professionals were not very helpful.
Experiences of Depression Connected to Declining Sense of Purpose
In-depth interviews find that those who screened positive for depression did not explain their experience in terms of diagnostic symptoms.
3 Facts All Parents Should Know About ADHD Stimulant Drugs
Medicating children for a host of mental disorders has become very popular in some parts of the USA. More than 8 million kids from 6 months to 17 years of age are on pharmaceutical drugs in this wonderful country. We lead the world in drugging youth for behavioral, cognitive and attention issues. We are once again #1. But I would like to share with parents as well as adults working with children a few not so readily available facts related to medicating kids for behavior issues.
The Orwellian New Digital Abilify Will Subjugate Vulnerable People Across the US
The FDA approved the prescribing and sale of a new hi-tech compliance-monitoring “antipsychotic” drug this week. A new chapter in human darkness has descended — one that is applauded by the alliance of control addicts that made it happen.
The Good, the Bad, and the Ugly: An Infographic on Bipolar Drugs
Bipolar drug therapy is a balancing act of benefits vs. harms. Odds of attributable benefit cluster in a 15-25% band, so 75%-85% don’t see substantial benefit. Stated differently, if five people take a bipolar drug, only one is likely to see substantial improvement due to it, but all five will have side effects.
Tapering Strips Help People Discontinue Antidepressants
A new study by Peter Groot and Jim van Os has found that tapering strips help people successfully discontinue antidepressant medications.