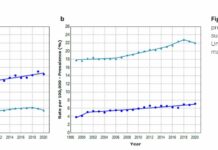
Long-Term Benzo Use Linked to Increased Disability
Despite guidance that the drugs should only be used short-term, about a third of patients indicated long-term benzo use.
When Medication Changes More Than Symptoms: Antipsychotics’ Effect on Identity
Recent research reveals how antipsychotic medications can significantly impact users' identity and self-image, challenging existing clinical approaches.
Antidepressant Trials “Hijacked for Marketing Purposes,” Researchers Say
About half of the large antidepressant trials are biased enough to be considered “seeding trials,” according to the researchers.
Study Links Prenatal Antipsychotic Exposure to Developmental Delays and ADHD
A comprehensive review indicates that children exposed to antipsychotics in the womb face an increased risk of ADHD and developmental delays.
Long-term Outcomes Better for Those Who Stop Taking Antipsychotics
Research undermines the prolonged use of antipsychotics in schizophrenia treatment, suggesting improved social functioning and quality of life with discontinuation.
Antidepressant Use in Pregnancy Harms Child Development, Untreated Maternal Depression Shows Benefit
In this new study, exposure to maternal anxiety in utero also harmed child development.
Study Highlights Difficulty of Antipsychotic Withdrawal
New research finds insomnia, anxiety, and depression are common symptoms of antipsychotic withdrawal, highlighting difficulties of discontinuation.
Common Side Effects Leading to Antidepressant Discontinuation
New research finds the negative drug effects most commonly associated with initiating antidepressant discontinuation are anxiety, suicidal thoughts, vomiting, and rashes.
Antidepressant Use Linked to Sexual Dysfunction, Why Aren’t Prescribers Discussing It?
Research sheds light on the impact of antidepressants on sexual dysfunction, emphasizing the need for patient-physician communication.
Antidepressant Use Tightly Correlates with Increased Suicide Rates
While the study can’t confirm causality, it does contradict the notion that antidepressants reduce suicide at the population level.
Despite Safety Risks, Prescribers Receive Little Guidance of Monitoring Antipsychotic Clozapine
A new review finds a lack of available guidance on how to effectively monitor adverse effects of antipsychotic drug clozapine.
Two Out of Three Find Antidepressant Effects Not Worth Burdens
New study reveals: 2 in 3 people need more than the current antidepressant benefits to consider them worthwhile.
SSRI Withdrawal has Social, Cognitive, and Emotional Consequences
New research finds that the non-physical aspects of withdrawal from SSRIs are often overlooked.
Antidepressant Exposure In Utero May Negatively Impact Motor Skills in 2-Year-Old Children
A new study in Frontiers of Pharmacology finds that antidepressant use during pregnancy is linked to reduced motor skills in children at 2 years...
Placebo Effect—Not Antidepressants—Responsible for Depression Improvement
In adolescent depression treatment, those who received a placebo but thought they received Prozac improved more than those who received the drug and knew it.
Antipsychotics Lead to Worse Outcomes in First-Episode Psychosis
Those who did not get antipsychotics in the first month were almost twice as likely to be in recovery after five years.
Stop Using Antidepressants Except for “the Most Severe Depression,” Experts Say
Experts advocate limiting antidepressant use to only the most severe cases of depression, emphasizing the need for social and psychological interventions.
ADHD Drugs Linked to Cardiovascular Disease
Service users taking drugs to treat ADHD may be at increased risk for hypertension and arterial disease
Adding Antipsychotics Worsens Outcomes in Psychotic Depression
Outcomes were worse for all, with young people on combination therapy twice as likely to experience rehospitalization or death by suicide than those on antidepressants alone.
Only One of Five Key Xanax Trials Deemed Positive by F.D.A.
The published literature is misleading, as the negative Xanax trials either went unpublished or were spun to appear positive.
Animal Study Shows Impact of Prozac in Pregnancy on the Child
Researchers found that rats born to mothers given the antidepressant Prozac during pregnancy or breastfeeding exhibited varied behavioral and developmental effects, with implications for the understanding of antidepressant impacts during human pregnancies.
Mental Health Staff Reluctant to Support Service Users in Tapering Antipsychotics, Study Finds
Study reveals schizophrenia patients find little support from mental health staff in reducing side effects-heavy drugs.
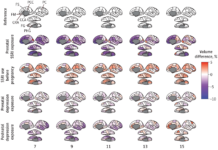
SSRI Use During Pregnancy Alters the Child’s Brain Development
Reduced brain volumes due to SSRI exposure in pregnancy was not explained by maternal depression alone.
Psychiatric Journals’ Pro-Pharma Publication Bias Hides Suicide Risk of Antidepressants
Selective publication bias in top psychiatry journals was not explained by the quality of the studies, but by financial ties to pharma.
Antidepressants Increase Suicide Attempts in Youth; No Preventative Effect
Researchers find that SSRIs increase suicide attempts up to age 24, and have no preventative effect at any age, even for those at high risk of suicide.