Study Deems Support, Not Drugs, Best for Youth at Risk of Psychosis
Research by five U.K. universities across multiple sites for up to two years divided 288 young adults (14-35 years) deemed at risk for psychosis...
Berlin Manifesto for Humane Psychiatry Released
Changing the mental health and psychosocial support system in Germany requires public debate about the ways our society should help and support people in mental crisis and with chronic mental health problems. We believe the driving force behind all help and support should be humanitarianism and respect for inalienable human rights.
Study Finds Hearing Voices Groups Improve Social and Emotional Wellbeing
Hearing Voices Network self-help groups are an important resource for coping with voice hearing, study finds.
Victim Blaming: Childhood Trauma, Mental Illness & Diagnostic Distractions?
Why, despite the fact that the vast majority of people diagnosed with a mental illness have suffered from some form of childhood trauma, is it still so difficult to talk about? Why, despite the enormous amount of research about the impact of trauma on the brain and subsequent effect on behaviour, does there seem to be such an extraordinary refusal for the implication of this research to change attitudes towards those who are mentally ill? Why, when our program and others like it have shown people can heal from the effects of trauma, are so many people left with the self-blame and the feeling they will never get better that my colleague writes about below?
Are Students Benefiting From the Growth Mindset Model?
Results from two meta-analyses reveal shortcomings with the growth mindset theory as applied in schools.
Psychologist Debunks Common Misconceptions of Maslow’s Hierarchy
Utilizing Maslow’s published books and essays, psychologist William Compton delineates common myths and attempts to respond to them.
Responding to Madness With Loving Receptivity: a Practical Guide
In my last three blogs I posed the question- "If madness isn't what psychiatry says it is, then what is it?" Now I'm asking-...
Study Investigates Long-Term Effects of Social and Emotional Learning Programs
Social and Emotional Learning (SEL) programs have gained popularity in U.S. schools in recent years. A new study examines the nature and longevity of their impact on students.
What Does Social Justice Really Mean for Psychologists?
Without clarity and consensus around what social justice means, psychologists risk perpetuating injustices that undermine their stated mission.
Study Finds Heavy Metal Music Beneficial to Mental Health
A new study highlights the role heavy metal music plays in the mental health of adolescents facing adversity.
Opening Doors in the Borderlands: An Interview with Liberation Psychologist Mary Watkins
MIA’s Micah Ingle interviews Mary Watkins about reorienting psychology toward liberation and social justice.
The Conflicts That Result From Globalizing Euro-American Psychology in India
Researchers examine the transformation of work, life, and identity in India as a result of Western corporate and psychological culture.
Climate Change, Mental Health and Collective Action: An Interview with Jennifer Freeman
In an interview with MIA's Akansha Vaswani, narrative therapist Jennifer Freeman calls for a shift away from individualistic approaches to 'eco-anxiety' and toward responses that connect us all to a counter-tsunami of action for the planet.
Western ‘Depression’ is Not Universal
Derek Summerfield, consultant psychiatrist at South London and Maudsley National Health Service Foundation Trust, challenges the assumption that Western depression is a universal condition.
People With Schizophrenia Diagnoses Actually Do Listen
Contrary to the hypothesis that delusional beliefs in schizophrenia are a persistent general deficit, patients using a well-documented advice-taking task revise their beliefs, taking...
Does Psychotherapy Reproduce or Disrupt Neoliberal Capitalism?
Researchers explore neoliberal influences on interactions in psychotherapy and question whether the radical potential of psychotherapy can counter prevailing social systems.
The Paradox of White Americans’ Mental Health
Are White Americans’ poor mental health outcomes caused by Whiteness?
Einstein, Social Justice and The New Relativity
To create his theory of relativity, Einstein had to see things differently. He used imagination and empathy to come to know a new 'reality' of existence. In this essay, we delve deeply into the nature of human experiences that lead to public concern and discover ourselves in a whole new realm.
United Nations Report Calls for Revolution in Mental Health Care
In a new report, the United Nations Special Rapporteur on the right to health, Dr. Dainius Pūras, calls for a move away from the biomedical model and “excessive use of psychotropic medicines.”
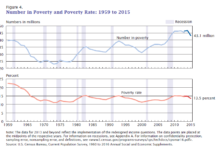
Psychotherapy is Less Effective and Less Accessible for Those in Poverty
A special issue explores the connection between poverty, mental health, and psychotherapy.
Researchers Test Harms and Benefits of Long Term Antipsychotic Use
Researchers from the City College of New York and Columbia University published a study this month testing the hypothesis that people diagnosed with schizophrenia treated long-term with antipsychotic drugs have worse outcomes than patients with no exposure to these drugs. They concluded that there is not a sufficient evidence base for the standard practice of long-term use of antipsychotic medications.
Psychologists Argue for Decolonial Approach to Global Poverty
Individualist psychological models of poverty pathologize poor communities, decolonial approaches that emphasize context and interdependence may be more sustainable.
Integrating Indigenous Healing Practices and Psychotherapy for Global Mental Health
As the Global Mental Health Movement attempts to address cross-cultural mental health disparities, a new article encourages integrating traditional healing practices with psychotherapy.
New Book Deconstructs Ideology of Cognitive Therapy
CBT forwards a hyper-rational perspective of human suffering that complements a managerialist culture of efficiency and institutionalization in the Western world.
Traditional Healing and Psychosis vs. the Promises of Modern Science
As noted in Anatomy of an Epidemic, the prognosis for someone experiencing psychosis is far better in developing countries than in industrialized countries. Robert Whitaker and others posit that this is due to the treatment models used in the developing world, as well as to debility and chronicity caused by psychiatric drugs themselves. I think it's also important to explore traditional tribal and village based models of helping people experiencing psychosis and examine why they may be effective. Do these traditional societies know something we don't?