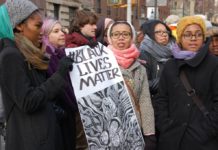Does Psychotherapy Reproduce or Disrupt Neoliberal Capitalism?
Researchers explore neoliberal influences on interactions in psychotherapy and question whether the radical potential of psychotherapy can counter prevailing social systems.
Lay Health Worker Intervention Effective at Decreasing Symptoms
Compared with standard care, results of a lay health worker intervention in Zimbabwe suggest that this is effective for reduction of common mental health symptoms
The ACE Survey is Unusable Data
Do the effects of trauma matter more, or a person's ACE score? I think this is unusable data that harms people when you gather it. Here's why.
Are Emotional Disorders Really Disorders of Love?
Could the whole array of psychiatric diagnostic categories, to the extent that they have any validity at all, be expressions of the failure to love and to accept love? Do successful psychotherapies really work by means of the therapist’s ability to encourage people to experience love through how positively he or she relates to them?
Belongingness Can Protect Against Impact of Trauma, Study Suggests
A new study explores feelings of belongingness as a protective factor for childhood trauma and adult mental health outcomes.
Social Support Improves Antipsychotic Discontinuation, Study Finds
A new study explores how people manage to discontinue antipsychotic medication and examines how social supports may improve outcomes.
Inner Fire: Healing and Recovery Without Meds
For five years, I and others worked to create a residential healing community in Brookline, Vermont, where people could recover from debilitating and traumatic life experiences, which often lead to addiction and mental health challenges, without the use of psychotropic medications. We welcomed our first six seekers to a yearlong, therapeutic and farm-based, day program last September, and we now can report on what we have learned during this time.
Robert Whitaker Missed the Mark on Drugs and Disability: A Call for a Focus...
Robert Whitaker extended one of his core arguments from Anatomy of an Epidemic in a blog post last week. His argument revolves around the claim that psychiatric drugs are the principal cause of increasing psychiatric disability, as measured by U.S. social security disability claims. But does this really explain the rise in recipients of these SSI & SSDI benefits?
Recovery: Compromise or Liberation?
The 90s were labeled - rather optimistically - as the ‘decade of recovery.’ More recently, recovery has been placed slap bang central in mental health policy. Is supporting recovery pretty much good common sense? Or is the term being misused to pressure those suffering to behave in certain ways?
Hearing Voices Network Launches Family & Friends Support Group
One of the HVN's fundamental principles is that "the person having these experiences is in the best position to decide or discover what they mean" and thus each person must "not try to speak for" another. The challenge for a family group will likely be for members to move past speaking about our loved ones to find or imagine the space where we ourselves are liberated.
Is Anxiety to Blame for Missed School?
A new systematic review illustrates features of the relationship between anxiety and school attendance patterns.
United Nations Report Calls for Revolution in Mental Health Care
In a new report, the United Nations Special Rapporteur on the right to health, Dr. Dainius Pūras, calls for a move away from the biomedical model and “excessive use of psychotropic medicines.”
The Paradox of White Americans’ Mental Health
Are White Americans’ poor mental health outcomes caused by Whiteness?
An Alternative Perspective on Psychotherapy: It is Not a ‘Cure’
Kev Harding argues against conceptualizations of therapy as a ‘cure’ to an ‘illness’ and instead offers alternative approaches.
Psychology Needs New Concepts and Healing Models for Racial Trauma
Contemporary empirical research explores new ways to conceptualize and heal racial trauma through anticolonial and sociohistorical lenses.
Traditional Healing and Psychosis vs. the Promises of Modern Science
As noted in Anatomy of an Epidemic, the prognosis for someone experiencing psychosis is far better in developing countries than in industrialized countries. Robert Whitaker and others posit that this is due to the treatment models used in the developing world, as well as to debility and chronicity caused by psychiatric drugs themselves. I think it's also important to explore traditional tribal and village based models of helping people experiencing psychosis and examine why they may be effective. Do these traditional societies know something we don't?
How to Promote Community Inclusion in Mental Health Practice
Practitioners and public leaders identify methods and barriers for integrating those diagnosed with mental health issues into community life.
Psychology Must Become a Sanctuary Discipline to Heal Racial Trauma
Researchers explore pathways of healing racial trauma in Latinx immigrant communities.
Teacher Wellbeing Matters for Student Mental Health
Teacher’s personal wellbeing plays a role in students’ mental health outcomes, suggests a new study.
Individuals With Low Incomes More Likely to Have Chronic Pain
Findings show that participants with lower levels of education and SES suffer from more chronic pain.
Searching for Zen and Finding a Cow
If I had a clinical problem, why was something as ancient and simple as meditation helping me? And if normal positive human habits could be so profoundly useful, why the heck was the field marketing pills and “clinical” coping mechanisms to me instead? This frustration helped me jump ship from the medical mindset and hop into the world of humanity.
New Study Examines User Experience of Discontinuing Psychiatric Medications
Researchers find that support and self-care were helpful for users during discontinuation, but that mental health professionals were not very helpful.
Do Social Network Sites Help or Harm Well Being?
How does social network site use influence well-being? Researchers suggest this depends on the extent to which site use is “connection-promoting."
Family Oriented, Home-Based Treatment Best for Youth with Symptoms of Psychosis
A pathbreaking new study out of Finland suggests that early intervention programs for youth experiencing psychotic-like symptoms may see the greatest improvement when treatment works within the home rather than in a hospital setting. The research, to be published in next month’s issue of Psychiatry Research, found greater improvement in functioning, depression, and hopelessness among teens in a new need-adapted Family and Community oriented Integrative Treatment Model (FCTM) program.
Long-Term Social Supports Needed After Onset of Psychosis
New data on the effects of social support after early onset of psychosis suggests that patients with intense social support function better than those without such help, but than once supports are removed the effects diminish.