I started my antidepressant taper on May 12, 2017. Just over two years later I have managed through grim determination to get down to 25% of my starting dose. The last 755 days represent an almost constant battle with a range of physical and psychological challenges. I wake in the morning feeling utterly exhausted and so fatigued that I can’t think straight, and the day generally goes downhill from that point.
My own mental health challenges were awful for myself and my family. I struggled with anxious thoughts, an intense sense of bleakness and a vomiting phobia and these issues cost me my career, our family home, the loss of friends and colleagues along with my dignity and any self-respect. In retrospect, my withdrawal experience feels far worse than those stark and terror-filled times. My feelings of utter despair or sheer, unreasoning panic were not constant, they abated, at times they were gone completely. Withdrawal does not abate, it is a cloying, near-permanent unwelcome companion that has come to dominate my life and fundamentally affect my family.
While I realise that not everyone experiences such difficulty coming off the drugs, it has been apparent for some time that antidepressant withdrawal needs more attention. A recent systematic review by Professor John Read and Doctor James Davies found that, on average across several studies, 56% of antidepressant users reported withdrawal symptoms. Critics (mainly prominent psychiatric researchers) were quick to point out that self-selected surveys are not necessarily free from bias and that a small sample doesn’t prove that the problem is sizeable. However, here’s the thing, these drugs have been in use for decades, millions of pounds have been spent investigating them to try and understand how they work. So why don’t we know more about long-term effects including withdrawal difficulties and the capacity of these drugs to result in dependence? Withdrawal effects have been witnessed during the placebo washout stage of clinical trials of psychiatric drugs. At the start of the trial, participants are taken off active medications and given a placebo. The intent is to reduce the influence of competitor drugs and to identify placebo responders. What this actually does is pitch the trial participants into withdrawal if they were already using a psychiatric drug. We know that these effects have been seen in clinical trials, yet patient advocates are often met with denial and disingenuous accusations of ‘pill-shaming’ or being anti-science.
Papers discussing withdrawal are almost impossible to find in the big medical journals, often appearing in smaller, independent publications. When a paper does appear, such as the recent study by Doctor Mark Horowitz in the Lancet Psychiatry, it transpires that the only responses allowed are critical ones. I know because I submitted my own response and assisted with the drafting of another on behalf of professional colleagues; both were supportive of the study and both were refused as they only wished to publish critical replies. This in spite of the Lancet Psychiatry wanting to encourage more ‘patient opinion’ with the paper “Service User Reviewers: extending peer review in The Lancet Psychiatry” from September 2018 asking the question:
‘How can they ensure that those with the biggest stake in decisions made over the future of psychiatry – people with personal experience of mental health problems – are a substantial, indeed a leading, part of the drive towards better care?’
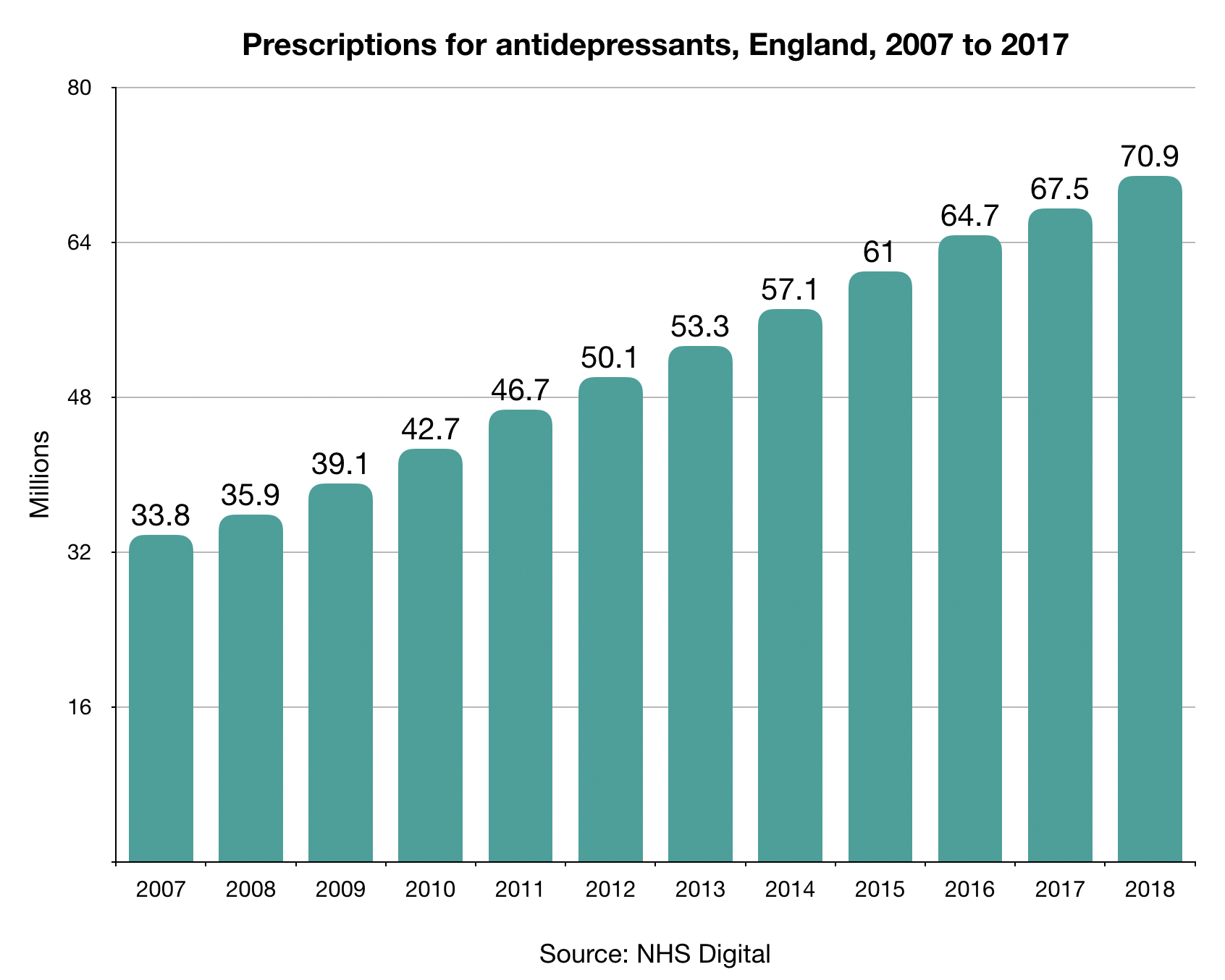
Across England in 2018, we prescribed 71 million antidepressant drugs, a near doubling in a decade. This startling figure is not even the full story as it excludes prescribing in prisons, hospitals and private psychiatric clinics. The Guardian recently reported that there are 4 million long-term antidepressant users in England. Some of those people may well want to rely on the drugs for the rest of their lives, that is their choice and should be respected, but some will have tried and failed to come off. They may well have visited their doctor or psychiatrist complaining of withdrawal symptoms but being told that they had relapsed and their mental health issues had resurfaced. It is a cruel irony that withdrawal symptoms are, at times, very difficult to distinguish from mental health problems as they encompass such a wide range of adverse physical and psychological effects. Many people who have experienced withdrawal, however, will describe tell-tale symptoms that never featured as part of their originally diagnosed condition, but only became apparent once they started to reduce the drugs. For myself, this means crushing headaches and blurred vision, a sure sign that my body is pleading with me to ‘slow down’.
It is now generally accepted by doctors that benzodiazepine drugs such as Valium and Lorazepam can result in dependence quite quickly and care should be exercised when prescribing. Plenty of prominent psychiatrists have spoken out to insist that antidepressants do not result in dependence. Recently circulated by the Royal College of General Practitioners is a guide to the ‘Top Ten Dependence Forming Medications’ from which antidepressant drugs are omitted. To my mind, it has never been proven that antidepressants don’t create dependence when taken for more than a few months. It is therefore incumbent on psychiatry to prove what it says to be evidentially true. In 2014, Professor Peter Gøtzsche, at the time a Director of the Cochrane Collaboration, writing in the Lancet Psychiatry, made the following statement:
“We noted that withdrawal symptoms were described in similar terms for benzodiazepines and SSRIs and were very similar for 37 of 42 identified symptoms. However, they were not described as dependence for SSRIs. To define similar problems as “dependence” in the case of benzodiazepines and as “withdrawal reactions” in the case of SSRIs is irrational. For patients, the symptoms are just the same; it can be very hard for them to stop either type of drug.”
On May 29th, the Royal College of Psychiatrists issued a Press Release which signalled a change of position in accepting that some people struggle with difficult withdrawal experiences. It also published a revised policy statement, calling on NICE to update its withdrawal guidelines. This welcome development follows many months of work by the Council for Evidence-based Psychiatry, along with members of the prescribed-harm community. While we should celebrate this significant progress, we do need to be aware of the positioning of formal statements. Towards the end of the ‘Position statement on antidepressants and depression revised policy statement’, there is a section which notes that antidepressant dependence is a matter of ‘public perception’. So while this change of position is welcome, there is still clearly a gulf between the experiential knowledge gained through taking and trying to stop the drugs and those that have gained their knowledge through reading papers and clinical observation. However, bridges are being built and I would like to publicly acknowledge all the efforts that have been made to get us to this point.
“If there is no struggle, there is no progress” – Frederick Douglass
Throughout my own withdrawal, I have been interested in solutions to this problem and have campaigned actively for greater awareness and understanding, launching a podcast and starting a petition which is now well over 10,000 signatures. I loudly applaud the excellent work undertaken by Doctor Peter Groot in the Netherlands to develop tapering strips. An evidence-based solution developed from a lived experience perspective and independent of the drug manufacturers. Let us hope that we can be forward thinking enough to adopt solutions rather than make grand statements while achieving little of practical value for those struggling.
In my campaigning efforts, alongside others, I stand for:
- Support for those affected by antidepressant dependence.
- True informed consent and discussion at the point of prescribing that will help to minimise the chances of someone becoming dependent.
- Fit for purpose, evidence-based guidelines that give the unadulterated facts, not theories.
- Greater expertise amongst doctors and psychiatrists enabling them to recognise and respond to difficult withdrawal.
- Proportionate use of antidepressant drugs with the person being in control of what they take and when they stop.
I believe that such aims are common-sense actions that will minimise harm and lead to better prescribing. Surely a laudable aim for medicine as well as for society.
As for me, I still have the most difficult part of my withdrawal ahead of me, I am fatigued beyond words and dispirited beyond belief. I feel in no way prepared for the challenge ahead. My life has been largely reduced to watching others get on with their lives, rather like observing the world from inside a fishbowl. I am very fortunate to be able to work with supportive colleagues who understand that I may be functioning one day and bed-ridden the next. My heart goes out to anyone experiencing withdrawal but especially those surrounded by unsupportive judgemental people, and those who are so ill they can’t work and are struggling to navigate a heartless and cynical ‘benefits’ system. Denial and minimisation of withdrawal make it even more difficult for those suffering to access help, support or seek understanding. Their only crime is to have experienced difficulty from a prescribed treatment, yet they are treated as medical pariahs.
If you do rely on your doctor or psychiatrist for withdrawal or tapering advice, you may experience a very hit and miss approach. Withdrawal from antidepressant drugs can be a significant challenge and needs to be approached carefully, with understanding and a shared decision-making approach. I want to acknowledge the brave general practitioners, psychiatrists, psychologists and researchers who have stepped away from the party line to present the raw, unadulterated truth about psychiatric drugs, including their ability to result in sometimes excruciating withdrawal experiences.
I have no wish to frighten anyone, so it is important to know while reading this that not everyone will experience such difficult withdrawal. This issue does come down to more than a difference of opinion though, we have to carefully judge whether the lack of a full and frank discussion between prescribers and patients is causing societal harm.
To anyone reading this who is concerned or may be unable to find help and support, there are some online resources that can be recommended. Mad in America holds a Provider Directory, listing therapists who are willing to support people who have made a choice to stop. The well-known website Surviving Antidepressants has provided peer tapering support for many years. Another excellent source of information is Laura Delano’s Inner Compass and the Withdrawal Project.
I sincerely hope that I won’t be writing another blog at 1,095 days but I am far from confident.
“Without deviation from the norm, progress is not possible” – Frank Zappa















James
A great blog post. Thank you for sharing your powerful and humbling story. I do believe in neuroplasticity and the brain’s ability to repair itself over time. I wish you all the best in the coming period. Please keep writing and advocating for those oppressed by psychiatry and the Medical Model.
Richard
Report comment
Hi Richard, thanks so much for taking the time to read this. I know I’m not alone in experiencing withdrawal effects and that helps hugely. I’m also fortunate to understand some of what is happening to me, many don’t and end up of course with a doctor/psychiatrist just misdiagnosing relapse and prescribing even more drugs and compounding the problem.
Report comment
I also agree “in neuroplasticity and the brain’s ability to repair itself over time.” And not even because of my “mental health” research, or my own personal healing from the harms of psychiatry.
But because of what neurologists were thrilled to discover, after my father’s death. After my father’s death, in 2013, the neurologists honestly explained to us, what my father’s doctors, when he was alive, never could.
In about 2004, my father suffered from what the doctors’ claimed was “dementia.” He suddenly suffered from memory issues, and other terribly outside the norm issues for him, as a former bank president, Phi Beta Kappa award winner, and very intelligent individual.
What the neurologists discovered, after my father’s death, was that my dad suffered from a blockage of the two primary arteries leading to his brain. And they were thrilled to describe what allowed him to recover.
The neurologists pointed out that when the two primary arteries to the brain became blocked, in 2004, the body compensated. My father’s body created many new smaller arteries to compensate for the blockage of the two major arteries to his brain. The neurologists were thrilled they had physical proof of neuroplasticity.
But I do also know, from over a decade of research, that the adverse and withdrawal effects of the antidepressants are massively being misdiagnosed by our “mental health” workers and doctors – as either “a return of the illness” or “bipolar” – which is what Whitaker pointed out in “Anatomy of an Epidemic.”
I had the common symptoms of antidepressant discontinuation syndrome misdiagnosed as the flu, pneumonia, and a lot of other things, prior to it being misdiagnosed as “bipolar.” And you’re correct, James, that is when the doctors and psychiatrists go hog wild, “prescribing even more drugs and compounding the problem.”
This is particularly true, since the current “gold standard” treatments for “bipolar” are, in reality, a recipe for how to make a person “psychotic,” via anticholinergic toxidrome – a medically known form of psychiatric drug poisoning.
The iatrogenic illness creation system, the monster, that the psychiatrists have created with their neurotoxins – and their misinformation about those drugs, and their “invalid” DSM disorders, to the public – is truly shameful. The whole system should be scrapped.
Report comment
They wouldn’t even bother to make these drugs unless they were addictive. I am convinced that prescription drugs, not street drugs, are the more common gateway to addiction.
Report comment
I understand your pain and frustration, James. It is now 27 months since I went off anti-depressants and if anything I am doing worse. At first it was extreme brain fog and an inability to focus. Now I have extreme insomnia and a host of gut issues. I cannot work and am living off savings. Somehow I need to get better before the money runs out. There is information on the internet but no in-person support.
Never in my worst nightmare could I have imagined that medicine could be so corrupt. Psychiatry for some reason thinks the Hippocratic Oath is optional. In order to find truth you have to be open to it.
But what can we do except keep moving forward? Not giving in to the despair is the hardest thing. Sometimes I just don’t have the strength to keep fighting, even though I know that I must. You have tremendous courage and I appreciate all you have done for the Mad in America community.
P.S. I was on anti-depressants and mood stabilizers for 29 years.
Report comment
Dan, I agree, especially with …”Never in my worst nightmare could I have imagined that medicine could be so corrupt.” Yes, that reality hit me like a ton of bricks.
Everyone (patients, media, public) assumes because they are ‘doctors’ they will do what is best for us and we also assume that they actually care. You don’t find out it’s a façade until after you have personally tangled with them.
Best wishes on your recovery. I found that some natural supplements can help with severe insomnia. Hang in there and keep going.
Report comment
Rosalee, Thank You for the kind words!
The perverse thing here is that I believe many of the Psychiatrists who I saw over 30 years DID care. I do not believe they intentionally tried to hurt me. But the whole system is based on trust. They trusted the information they received just as I trusted them. The corruption is at the top. A big problem here is that Doctors do NOT confront or challenge other Doctors, even when those other Doctors are harming patients.
If the Neurologists, as a group, said “Hey! ECT can cause PERMANENT brain damage! Psychiatry, you CANNOT do this to people!”, then ECT would be banned immediately. There are many who know of these atrocities, but they put themselves first ahead of their patients. For this reason, it will be a black stain on ALL of medicine.
“The only thing necessary for the triumph of evil is for good men to do nothing.”
Report comment
Yes that is so true Dan. If doctors at least challenged other doctors it would have a huge impact but it’s as you say they put their own interests first. I have seen two psychiatrists in my life time. The first was 20 years ago, he did care and was very helpful at that time. The second psychiatrist I saw was 10 years later while I was in cancer treatments. Her behavior and attitude was appalling. Too long to explain here but she was hostile, a bald faced liar and downright corrupt. She knows she did immense harm but has dug her spike heels in. She could not care less, it is all about maintaining her pride, ego and status. Having 2 completely opposite experiences I am conflicted on the matter of psychiatrist’s actually caring but I realize there probably are still a few out there.
Report comment
Thank you for reading Dan, I am so very sorry to hear that things are so tough for you at present. From my perspective you have managed to achieve so much in coming off the drugs after so long. People who haven’t been through it struggle to grasp how fundamentally the drugs inhabit your life and how much change needs to happen to come off them. I think you have done incredibly well. I have heard of people who were decades using the drugs and who had awful times coming off or in the period afterwards, but there are many incredible success stories out there and I believe that the brain and nervous system are capable of healing, but it can take a frustratingly long time. My best wishes to you and I look forward to reading your success story one day, when you are ready to write it.
Report comment
Thanks for the encouragement, James.
The withdrawal issues aren’t the same as when I started. Things keep changing, which I take as a good sign. The drugs have been with me my entire adult life, and my depression problems started as a teenager. So this gets into things like identity – what kind of person will I be off the drugs and without depression? It is exciting and terrifying at the same time. I look forward to writing that success story someday!
Report comment
I enjoyed reading about your experiences, having gone through withdrawal as well. My withdrawal from nicotine and cocaine were a cake walk compared to this poison. I will never consent to taking any psychiatric med ever again. They debilitated me for decades and then years after as I weened myself from them.
It also makes no sense that these drugs would not cause dependence and lasting changes after they are stopped. Basic human biology refutes what the “professionals” dismiss in their arguments. But then, their is no chemical imbalance that could ever be quantified by lab work so it’s all smoke and mirrors. I do have to wonder what is going to happen when the pedestals fall and this group of “experts” have to eat their own words.
Report comment
The impact on medicine will be quite profound. The anti-vaxers are criticized for ignoring scientific evidence and yet here we have a medical profession that is doing the exact same thing! The media are reporting on some of these things, but are not yet connecting the dots and seeing the massive corruption issue. The media just assume that because these are Doctors they will do what is best for patients!
Report comment
thank you so much james for all the help
and truth that you have been sharing…
i look up to you…
Report comment
Thank you for reading littleturtle, I know there is nothing particularly unique about my story, but I feel that the important thing is that we share our stories with each each other and with the world was much as we can. As for looking up to me, I’m not that tall : )
Report comment
but james i am a littleturtle…and
your podcasts are very helpful..
Report comment
I have been weaning off an antidepressant given to me along with a benzodiazepine from 2 1/2 years ago when my daughter died. I have had to wean myself off the antidepressant and am on an extremely small dose. This antidepressant is best weaned off by getting the smallest capsule and taking out a tiny bead a day. It’s so ridiculous I have to do this. This way I have minimal side effects. The doctors tried to get me off faster and I had debilitating withdrawals. I tried to get off the Benzos at the same time and was literally so sick I couldn’t function. So I’m going to start that taper as soon as I’m done with this one. I am angry I was prescribed this medication I was not told of these effects.
Report comment
They often even tell you when you DO experience these effects that they are NOT caused by the drugs, but are a sign of “relapse.” The lack of ethics in the field is shocking, or would be if I didn’t already expect it at this point.
Report comment
Dear James, I’m writhing this comment about a man I know. A man as it happens I am going to know more eventually. We played some scrabble on the iphones many times. We are planning a possible visit to play some board games in person. He was thrilled about my double word scores and they way I effortlessly move through the board getting those a lot. It’s a great strategic move. Is it defense or offense he wonders and I chuckle.
Anyway he has issues or challenges with the increased energy and also his mood and the larger word we refer to as depression. I also have some issues that I have conquered and I want to support.
This article was awesome.
Report comment
Thanks so much for reading.
Report comment
But there has to be a next step, it can’t all be a “Recovery” project. There has to be redress, legal action.
Report comment
Letting it stay as merely a Recovery project, that makes it look like with you, and with all of us survivors, it was really we ourselves who were the problem in the first place.
Report comment
I agree with you PacificDawn. We need to take action. It can be hard to do though when in extreme withdrawal and when you are just trying to survive. I hope to do more as I improve. I guess the biggest thing I can do now is tell my story, and I have to those who I know are on medication. There are VAST numbers of people out there on these drugs. If I can prevent even one person from going through the suffering I did it will be worth it.
Report comment
I agree with you Dan. We need to band together and take actions, not try and do it alone. The Mental Health System and the Middle-Class Family with its Self-Reliance Ethic work to keep people from joining forces. When we join forces, we are attacking the perpetrators at their core.
Report comment
“I am fatigued beyond words and dispirited beyond belief” I’ve copied this from your article. It describes me. When will this nightmare end? I’m still tapering lexapro and Klonopin. But they’ve had me on over 25 different psych drugs in past 23 years. I haven’t been able to taper as fast as you. I feel I will never be free. Plus, psychiatry has tried to destroy my son and I’m having to advocate fiercely for his very life and freedom which is extremely difficult. They almost killed him last summer through forced overdose in a hospital. He’s finally home, yet ill and on a neuroleptic and an antidepressant. Ugh. I’m so overwhelmed. The fatigue and depression is debilitating. I understand having to watch everyone else go on with their lives. I’m living a nightmare and have been abandoned by friends and family. They are living their lives and my son and I have been left, reeling from severe injustice and psychiatric injuries. My son only has me as a safe person and he relies entirely upon me now, but I need help myself, but have none. It would help for someone to clean or cook or just visit us. I feel so alone. We need miracles. Thank you for sharing your story. They say it helps to know you’re not alone, but it doesn’t seem to help me. I’m suffering horribly every day with no relief. And must try to be a caregiver and support—I’m failing miserably.
Report comment
When I’m hot I’m hot and when I’m not I’m hot. It’s a blessing and a blessing.
Seriously though no matter the struggle trivial or huge I have this. I have this one of my hobbies. Riding my bicycle and coming up with a screenplay. I’m not deluding myself as I know how blissful it can be and not from the tangible or concrete tangible. https://youtu.be/Zv9jveCixb8
Report comment
Finding someone you can talk to about these things in person (and not just online) can make a big difference. They can be hard to find but there are people who do care and want to help. I’ve forwarded some of the articles on this website to people I know. Not all were helpful, but some were. I sympathize with your despair…
Report comment
Thank you. I have found no one in person to support me or help me support my son. I have been on at least one antidepressant and one benzodiazapine for the past 23 years, but they have switched me around on over 25 different psychiatric drugs in different combiniations – which was scary. I never liked any of them. I guess that’s why they kept trying different drugs. Now I am done and still tapering lexapro and klonopin without help from any doctor. They refuse to help me. I do not know how I will help my son, but am trying to get healthy myself first.
Report comment
Hi mmarti2007 thank you for sharing, I am so very sorry to hear of your experiences. You mention that you feel you are failing, but from the short note above, I’d say it sounds like you are doing a magnificent job in very difficult circumstances. My best wishes to you.
Report comment
Thank you, Mr. Moore. I just want the world to be right again. I never feel well (it is tough to just get out of bed or to shower) and seeing my son suffer is just beyond traumatic. Anything I do, I feel I am dragging my body to force it to do what I really would like to do or have to do. No way to live. I suppose this journey takes a lot of patience and keeping hope alive that we will feel alive eventually as our bodies and brains repair. I look everywhere for help.
Report comment
Hi James, thank you for sharing your personal story of slowly tapering off an anti-depressant drug. It boggles the mind how this disingenuous branch of medicine has gotten away with harming lives for so long. So many unsuspecting people were brainwashed and so many still are. The one thing we can do is tell our stories and keep putting them out there. There has to come a point when mainstream media can no longer ignore the horrible damage psychiatry has done to so many lives.
I wish you all the best on your final stage of tapering off. You are 75% of the way there! And thanks for all your work at MIA, I really enjoy your great podcasts.
Report comment
Thank you Rosalee, I am incredibly grateful to have found MIA. Before I did I felt utterly alone and believed that I was totally broken and in need of ‘fixing’ and I never would have found that inner strength to challenge the falsehoods that were keeping me quiet and compliant. Thank you for your kind words, and you are right, I should celebrate how far I have come, even if I still have quite a challenge ahead.
Report comment
Dear James, thank you for posting your compelling story about the great difficulties you are experiencing with getting off of psychiatric medications. My heart goes out to you and to everyone else who finds themselves trapped in the vortex of drug withdrawal. Stories like yours help others to know about the dangers lurking behind the simple directions to take pills to manage intense feelings of pain and despair. I will be sharing your story with many friends. Thank you and all the best with your journey.
Report comment
Thanks for taking the time to read and for your wishes too Ann. There are so many struggling that benefit from being part of communities like MIA which provide support, advice and understanding that the medical world couldn’t match, even if it wanted to.
Report comment
Thanks James for working so tirelessly on this for us, especially when you are struggling. Your courage, passion and endless commitment are so very important. “The illness has returned” is what I was taught until I joined peer support services 8 years ago. Peter and Robert’s work changed my life and my attitude so much. I’m glad I only had to withdraw from Epilim, I never stayed on thew other drugs they gave me except when I really needed to sleep.
I work with a lady who 3 years ago was cold turkeyed off clozapine then taken of clonazepam, an SSRI and another antipsychotic over the next 2-3 months. They changed her label from schizophrenia (which she’s had for 30 years) to Borderline Personality Disorder and treated all her horrendous withdrawals as behavioural. Last week, 3 years later I had my first glimpse of the woman I once new. She is so tortured having visions of people being killed etc, terrible vertigo, intrusive memories. In fact when I gave the ashton manual to her sister 3 years ago she suffered pretty much every symptom in the book. It is criminal. I have been watching the antidepressant debate in the UK closely and am pleased with the fact they are going to review the NICE guidelines. A lot of NZ clinicians actually referr to the NICE guidelines so I’m hoping it will have the required knock on effect here down under. Thank you again James and your colleagues.
Report comment
Thank you for your kind words Pauline. I am shocked and saddened reading the stories of how people are got on these drugs and then simply cut adrift or given further diagnoses and more drugs when they report anything but a ‘life saving experience’. I am so glad that there are people speaking out. The review of NICE guidelines is welcome, but time will tell how much the messages of potential for harm will be softened in the process.
Report comment
So why don’t we know more about long-term effects including withdrawal difficulties and the capacity of these drugs to result in dependence?
Because “we” don’t matter. The purpose of administering these drugs to the population, despite their long known toxicity, is to keep people from openly freaking out and disrupting business as usual, and to “help” them play out the soulless lifestyles endorsed by the system. If this sometimes makes people feel better fine, but it remains a secondary concern. So are any physical or dependency issues.
Report comment
I also went through a long withdrawal from an antidepressant. I did it through the help of that great site you mentioned called survivingantidepressants.org. But, what I discovered was that the reason it was taking me so long to be able to get off of it was because I actually had undiagnosed autoimmune thyroid disease. My thyroid levels were always within normal limits and so it was not diagnosed until by accident on an MRI. Even though the thyroid levels were within the normal limits, my thyroid was not functioning well at all and the levels were not where they should have been within the normal range. I was on the antidepressant for 16 years and slowly became less and less capable of functioning. What was actually happening was that the antidepressant was causing an autoimmune attack. One of the possible side effects of many antidepressants is that it causes low thyroid levels as well. I realized my decline started after I started the medication and I began tapering off. As I was tapering off, I started to improve but still felt horrible. I thought I was just having a really hard time with withdrawal symptoms. That was not the case. I encourage you, if you are having such fatigue, to get checked as that is one of the major symptoms of thyroid issues. It took me 4 years to get off the antidepressant because I thought I was having withdrawal symptoms when they were actually thyroid symptoms.
I have been in the medical field for 32 years and I can tell you that they are prescribing these meds for just about everything in both adults and kids. I went to a clinic for what was supposed to be a dementia screening and since my doctor said it was for depression and anxiety on the referral form, they refused to even let me see the provider I was supposed to see if I wasn’t willing to go on antidepressants. I was told all that particular provider did was prescribe antidepressants. They tried to convince me that my depression was not caused by the thyroid issues (which it is) and I needed the medication. I could not believe that I was being pressured to agree to medication when I had clearly told them what I was there for and that I would not take any medication again after what it did to me. They tried to convince me that they could find the right one for me because they can now do testing to find the one that will work best for your brain. I refused and, as stated, was told there was no reason for me to see the provider and that I should get a new referral from my doctor to come back for the screening. I never went back. In the early 2000s pain pill clinics were the rage. Now it is antidepressants. People are afraid to feel and deal with their issues. I have struggled with depression almost my entire life. In my case, it was caused by an undiagnosed illness. There is a place for antidepressants, but they are by far over prescribed and often, as in my case, do more damage than they help. I will never go back on one. You have no idea what it did to me. I would rather deal with the depression. I wish you the best, James. You aren’t alone. There are many of us who stand with you who have been damaged by these drugs.
Report comment
The people who give out these drugs should be prosecuted. Otherwise the debate will never stop.
Report comment
Regarding “ psychiatric researchers “. It is shameful for those “ psychiatric researchers “ to even talk about bias. Shouldn’t they be much more concerned about the bias when testing is done by the drug companies to get the FDA approval. They should be far more concerned not only about the tests but also those results that do not get published. The bad ones are locked from public view and require a “freedom of information act” to unlock. That should be more concerning if they are truly interested in the welfare of people. Bad even if there were no serious side affects. And all the while promoting those anti-depressants to “ make people happy”. As if “Peoples happiness is most certainly their primary concern.”
Report comment