Why the Rise of Mental Illness? Pathologizing Normal, Adverse Drug Effects, and a Peculiar...
In just two decades, pointing out the pseudoscience of the DSM has gone from being an “extremist slur of radical anti-psychiatrists” to a mainstream proposition from the former chairs of both the DSM-3 and DSM-4 taskforces and the director of NIMH. In addition to the pathologizing of normal behaviors, another explanation for the epidemic — the adverse effects of psychiatric medications — is also evolving from radical to mainstream, thanks primarily to the efforts of Robert Whitaker and his book Anatomy of an Epidemic. While diagnostic expansionism and Big Pharma certainly deserve a large share of the blame for this epidemic, there is another reason.
Mental Health Concerns Not “Brain Disorders,” Say Researchers
The latest issue of the journal Behavioral and Brain Sciences features several prominent researchers arguing that mental health concerns are not “brain disorders.”
How Reliable is the DSM-5?
More than a year on from the release of DSM-5, a Medscape survey found that just under half of clinicians had switched to using the new manual. Most non-users cited practical reasons, typically explaining that the health care system where they work has not yet changed over to the DSM-5. Many, however, said that they had concerns about the reliability of the DSM, which at least partially accounted for their non-use. Throughout the controversies that surrounded the development and launch of the DSM-5 reliability has been a contested issue: the APA has insisted that the DSM-5 is very reliable, others have expressed doubts. Here I reconsider the issues: What is reliability? Does it matter? What did the DSM-5 field trials show?
United Nations Report Calls for Revolution in Mental Health Care
In a new report, the United Nations Special Rapporteur on the right to health, Dr. Dainius Pūras, calls for a move away from the biomedical model and “excessive use of psychotropic medicines.”
Mental Health Professionals Critique the Biomedical Model of Psychological Problems
While a great deal of the excitement about advances in psychological treatments comes from the potential for research in neuroscience to unlock the secrets of the brain, many mental health experts would like to temper this enthusiasm. A special issue of the Behavior Therapist released this month calls into question the predominant conception of mental illnesses as brain disorders.
Duty to Warn – 14 Lies That Our Psychiatry Professors in Medical School Taught...
Revealing the false information provided about psychiatry should cause any thinking person, patient, thought-leader or politician to wonder: “how many otherwise normal or potentially curable people over the last half century of psych drug propaganda have actually been mis-labeled as mentally ill (and then mis-treated) and sent down the convoluted path of therapeutic misadventures – heading toward oblivion?”
Renowned Harvard Psychologist Says ADHD is Largely a Fraud
From Curious Mind Magazine: Jerome Kagan, one of the most influential psychologists of the 20th century, believes that the diagnosis of ADHD is a mere...
Developing Alternatives to the DSM for Psychotherapists
A new article suggests counselors and psychotherapists are dissatisfied with current diagnostic systems and outlines some potential alternatives.
The DSM-5 Field Trials: Inter-Rater Reliability Ratings Take a Nose Dive
The American Journal of Psychiatry (January, 2103) recently published a series of articles that analyzed the outcomes of the field trials that were conducted by the DSM-5 Task Force, to determine the inter-rater reliability of the multiple diagnostic categories that will comprise the DSM-5. A table below tracks the downward progression of inter-rater reliability from DSM-III through DSM-5.
Professionals Push Back on Psychiatric Diagnostic Manual, Propose Alternatives
Criticisms of the DSM-5 spark alternative proposals and calls to reform diagnostic systems in the mental health field.
This is the Truth About Personality Disorders
From The Independent: Armchair diagnoses of personality disorders are a rising trend, from speculations that President Trump has narcissistic personality disorder to viral articles about discerning...
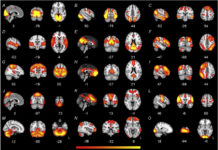
No Brain Connectivity Differences Between Autism, ADHD, and “Typical Development”
Neuroscience researchers find no differences in brain connectivity between children with diagnoses of autism, ADHD, and those with no diagnoses.
Mental Health Professionals and Patients Often Disagree on Causes of Symptoms
A new study finds that clinicians’ disregard for mental health patients’ insight into their own condition may be detrimental to treatment.
The Power Threat Meaning Framework One Year On
The team that developed the Power Threat Meaning framework as a diagnostic alternative reflects on the response to the framework after one year.
Philosophers Challenge Psychiatry and its Search for Mechanisms of Disorder
Attempting to locate the mechanisms of psychiatric disorder is a step in the wrong direction and fails to challenge potentially unjust social practices.
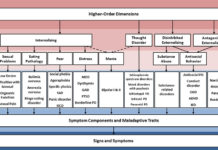
International Research Team Proposes a New Taxonomy of Mental Disorders
New data interpreted to suggest a hierarchical, dimensional system of mental disorders will aid future research efforts and improve mental health care.
German Psychologists Declare “the Drugs Don’t Work”
Jürgen Margraf and Silvia Schneider, both well-known psychologists at the University of Bochum in Germany, claim that psychotropic drugs are no solution to mental...
Lancet Psychiatry’s Controversial ADHD Study: Errors, Criticism, and Responses
Amid calls for a retraction, Lancet Psychiatry publishes articles criticizing the original finding and a response from the authors.
Time to Abolish Psychiatric Diagnosis?
‘Diagnosing’ someone with a devastating label such as ‘schizophrenia’ or ‘personality disorder’ is one of the most damaging things one human being can do to another. Re-defining someone’s reality for them is the most insidious and the most devastating form of power we can use. It may be done with the best of intentions, but it is wrong - scientifically, professionally, and ethically. The DSM debate presents us with a unique opportunity to put some of this right, by working with service users towards a more helpful understanding of how and why they come to experience extreme forms of emotional distress.
Constructing Alternatives to the DSM: An Interview with Dr. Jonathan Raskin
Dr. Raskin discusses psychotherapists’ dissatisfaction with current psychiatric diagnostic systems and explores alternatives.
Western ‘Depression’ is Not Universal
Derek Summerfield, consultant psychiatrist at South London and Maudsley National Health Service Foundation Trust, challenges the assumption that Western depression is a universal condition.
United Nations Statement Criticizes Medicalization of Depression on World Health Day
"There is a need of a shift in investments in mental health, from focusing on 'chemical imbalances' to focusing on 'power imbalances' and inequalities"
The Genetics of Schizophrenia: A Left Brain Theory about a Right Brain Deficit in...
In recent months, two teams of researchers in the UK and the US published complementary findings about the epigenetic origins of schizophrenia that have scientific communities who indulge in ‘genetic conspiracy theories’ abuzz. While these results are intriguing, and no doubt involve pathbreaking research methodologies, this line of thought represents a decontextualized understanding both of the symptoms that are typically associated with schizophrenia, and their causes.
An Alternative Perspective on Psychotherapy: It is Not a ‘Cure’
Kev Harding argues against conceptualizations of therapy as a ‘cure’ to an ‘illness’ and instead offers alternative approaches.
The Role of Racial Bias in the Overdiagnosis of Schizophrenia
Researchers detect disparity between white and African American patients diagnosed with schizophrenia when symptoms of a mood disorder are present.