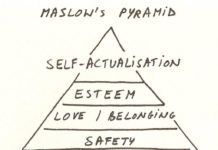
Psychologist Debunks Common Misconceptions of Maslow’s Hierarchy
Utilizing Maslow’s published books and essays, psychologist William Compton delineates common myths and attempts to respond to them.
Goodbye, Brian Wilson
I propose to call any psychiatrist-patient bond “Landy syndrome” after psychiatrist Eugene Landy, the captor, abuser and oppressor of Brian Wilson.
Mobile Apps for Mental Health Lack Transparency in Data Sharing
Research illustrates privacy concerns with how mental health applications collect and share users’ data.
Safety Analysis Weighs Harms and Benefits of Antipsychotic Drugs
The researchers find that the drug effects for reducing psychosis are small and that treatment failure and severe side effects are common.
Why Isn’t There a Popular Hashtag for Involuntary Commitment?
As uses of psychiatric force expand, can social media be better used to focus critical attention?
Integrative Mental Health: 27 Non-drug Options that Work
Four years ago I dove into a deep and murky pond: the bottomless depths of medical databases that hold mental health research. After examining over 4000 studies, and hundreds of meta-analyses, I surfaced from my research and was hit with a startling “Aha” moment: non-drug approaches really work.
We Are All in This Together
We need a new narrative of shared distress to replace the failed one of individual disorders. We need human connection and mutual support. We can learn to manage our feelings in a way that helps us through the crisis and gives us the energy to make much-needed social and environmental changes afterwards. The usual dividing lines melt away in the face of global emergency. We really are all in this together.
Open Dialogue: Does the Current Research Data Support Further Investment?
A leading US journal published an extensive literature review and analysis of currently available research on Open Dialogue. An accompanying commentary concludes, “The present data on Open Dialogue are insufficient to warrant calls for further research on the program other than those projects that are currently under way.”
That Others May Live: An Airman’s Mental Health and Medication Hurricane
“These things we do, so others may live.” It took a small army of my brothers and sisters in and out of uniform to drag me out of my abyss.
Psychologists Push For New Approaches to Psychosis: Part 1
Psychologists and people with experience of psychotic symptoms publish a report on new ways of understanding psychosis.
Social Support Improves Antipsychotic Discontinuation, Study Finds
A new study explores how people manage to discontinue antipsychotic medication and examines how social supports may improve outcomes.
Bringing Structural Competency to Global Mental Health
Structural competency is put forth as a framework that addresses social and structural determinants in global mental health.
Loneliness as Lethal: Researchers Name Social Isolation a ‘Public Health Threat’
Researchers present loneliness as a health threat facing a growing number of Americans.
False Information in UK Package Inserts for Antidepressants About a Chemical Imbalance
To state something that is blatantly false is not a “paradigm,” it is a lie, plain and simple.
Mental Health Survival Kit, Chapter 4: Withdrawing from Psychiatric Drugs (Part 3)
Cochrane has no interest in a review about safe withdrawal of depression pills but did its utmost to defend the psychiatric guild, its many false beliefs, and the drug industry.
Trauma-Ignored Care? Going to the MAT on Opioids
Our current, reductionistic approach to mental health issues doesn’t offer any insights or explanations on the etiology of most mental disturbances. Similarly, medication assisted treatment (MAT) focuses on the surface symptoms of opiate abuse without addressing the underlying causes of overwhelming distress and pain.
A Dystopian Vision of Psychiatry’s Future
As a psychiatric survivor, I was stunned to see a medical professional describe a dystopian nightmare as a vision of progress for psychiatric medicine.
The 57th Maudsley Debate: Interview with Professor John Read and Doctor Sue Cunliffe
This week on MIA Radio we turn our attention to Electroshock or Electroconvulsive Therapy (ECT) as it’s known in the UK. On Wednesday, September 19th, this emotive and controversial intervention was discussed at the 57th Maudsley debate, held at Kings College, London.
New Review Suggests Higher Recovery and Remission Rates for Psychosis
Meta-analysis gives updated recovery and remission rates for persons identified as having a first-episode psychosis and those diagnosed with schizophrenia.
Understanding the Neurobiology of Post-SSRI Sexual Dysfunction
Post-SSRI sexual dysfunction (PSSD) may be a common adverse effect of antidepressants. Researchers are now attempting to understand the neurobiology behind it.
Stimulant Prescribing Patterns for ADHD Not Impacted by Scientific Evidence
The article suggests that research challenging the evidence for ADHD drugs does not lead to changes without public campaigns.
The Language of Internalized Oppression
I realize many folks get irritated by the ‘moving target’ of language, but understand that this is a process of unlearning for us all. It’s not so much that the words randomly keep changing as it is that the oppression embedded in our words and ways of being runs deeper than most of us could have ever imagined. Unraveling it all is a long way off.
The Quiet Crisis in Mental Health: The Medicalization and Deskilling of Psychotherapy
The focus on the "worried well" and the exclusion of the "mad" serves to legitimize psychiatric control and surveillance.
Researchers Challenge Evidence for Antidepressants in Youth
Researchers shed light on the precarious nature of evidence from efficacy trials of antidepressant medication to treat symptoms of major depressive disorder in children and adolescents.
Therapists, Neutrality Is No Longer an Option — Politics Is Tearing Us Apart
To my fellow therapists: stop playing neutral. Stop minimizing systemic trauma to keep your comfort intact.