Medication-Free Treatment in Norway: A Private Hospital Takes Center Stage
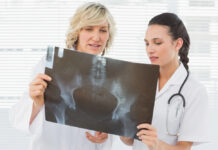
At the Hurdalsjøen Recovery Center in Norway, patients with a long history of psychiatric hospitalizations are tapering from their medications and, in a therapeutic environment that emphasizes a good diet, exercise, and asking patients "what do they want in life," are leaving their old lives as chronic patients behind.
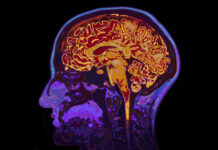
Antipsychotics Increase Risk of Dementia; New Research Illuminates Why
In JAMA psychiatry, researchers outline new theories connecting antipsychotic use in people with schizophrenia and increased dementia risk.
Antidepressant Trials Last Eight Weeks, So Why Do We Take Them for Years?
The studies are of short duration and are riddled with methodological issues like unblinding and failure to assess withdrawal.
Stuart Shipko – SSRI Withdrawal: Shooting the Odds
We interview Dr. Stuart Shipko, a psychiatrist and author who has a particular interest in the side effects and withdrawal effects of SSRI antidepressants and the need for informed consent when prescribing.
More Evidence That Antidepressants Work Via Placebo Effect
Antidepressants were more effective for depressed patients who were more “optimistic.” Still, only 30% responded to SSRIs.
Deadly Prescriptions: New Study Links Antipsychotics to Life-Threatening Risks in Dementia Patients
With pharmaceutical companies pushing antipsychotics for off-label use, dementia patients are being put at risk for devastating health consequences. Research suggests safer alternatives exist—but why aren’t they being prioritized?
Ambushed by Antidepressant Withdrawal: The Escape Story
I’m alive. More than 30,000 veterans in the past decade alone are not. I was not warned of the risks of this drug. I was not told that once on it, I might never be able to get off it, or the nightmare that would ensue when I tried. I know millions of others were not told either.
Are Antidepressants Weakening Women’s Bones?
A study spanning two decades finds that antidepressant use is associated with a 44% increase in osteoporosis risk and a 62% higher chance of fractures.
Lancet Psychiatry Needs to Retract the ADHD-Enigma Study
Lancet Psychiatry, a UK-based medical journal, recently published a study that concluded brain scans showed that individuals diagnosed with ADHD had smaller brains. That conclusion is belied by the study data. The journal needs to retract this study.
UPDATE: Lancet Psychiatry (online) has published letters critical of the study, and the authors' response, and a correction.
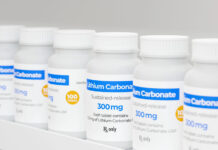
Lithium Doubles Risk of Thyroid and Kidney Dysfunction
Serum lithium levels lower than those considered therapeutic still conveyed increased risk.
Screening + Drug Treatment = Increase in Veteran Suicides
For the past 15 years, the VA's suicide prevention efforts have focused on getting veterans screened and treated for psychiatric disorders, with antidepressants a first-line therapy. This effort has caused veteran suicide rates to steadily rise.
New Study Links Antidepressants to Increased Risk of Diabetes
Using genetic analysis, a new study finds that antidepressants—not depression—are responsible for a significant rise in type 2 diabetes risk.
Contribution of Antipsychotics to Suicidality and Depression
Peter Lehmann reviews the contribution of antipsychotics to suicide and depression in schizophrenia in the current International Journal of Psychotherapy. Publications about the intrinsic effects of...
Overuse of Psychiatric Drugs is Worsening Public Mental Health, Doctor Argues
A new research article asserts that the overuse of psychiatric drugs may create neurobiological changes that hamper long-term mental health recovery.
Animal Study: SSRI Neurotoxic in Pregnancy
Researchers: Fetal exposure to vilazodone hampers neurodevelopment and leads to "long-lasting neurodevelopmental impairments."
Suicide Rates Rise While Antidepressant Use Climbs
Multiple media sources are reporting on new data from the CDC revealing a substantial increase in the suicide rate in the United States between 1999...
Antidepressants Do Not Prevent Suicides, May Increase Risk
When the CDC released data revealing an increasing suicide rate in the US, some experts, speaking to major media outlets, speculated that the increase...
Withdrawal from ADHD Medications
This guide to the scientific literature on withdrawal from ADHD drugs provides a review of animal studies, withdrawal syndromes,
and possible tapering protocols.
Is Long-term Use of Benzodiazepines a Risk for Cancer?
A large study of the population in Taiwan reveals that long-term use of benzodiazepine drugs, commonly prescribed for anxiety, significantly increases the risk for brain, colorectal, and lung cancers. The research, published open-access in the journal Medicine, also identifies the types of benzodiazepines that carry the greatest cancer risk.
Psychiatry Defends Its Antipsychotics: A Case Study of Institutional Corruption
Jeffrey LIeberman and colleagues have published a paper in the American Journal of Psychiatry stating that there is no evidence that psychiatric drugs cause long-term harm, and that the evidence shows that these drugs provide a great benefit to patients. A close examination of their review reveals that it is a classic example of institutional corruption, which was meant to protect guild interests.
Study Confirms Overdiagnosis of ADHD in Children and Teens
Medical researchers present evidence that ADHD is overdiagnosed in children and teens, which can lead to significant harm.
Do Antidepressants Work? A People’s Review of the Evidence
After a meta-analysis of RCTs of antidepressants was published in Lancet, psychiatry stated that it proved that "antidepressants" work. However, effectiveness studies of real-world patients reveal the opposite: the medications increase the likelihood that patients will become chronically depressed, and disabled by the disorder.
How to Distinguish Antidepressant Withdrawal from Relapse
Mark Horowitz and David Taylor provide advice on how to tell the difference between antidepressant withdrawal and depression relapse.
William Styron: His Struggles with Psychiatry and Its Pills
Author William Styron is often remembered for speaking about depression as an illness. But a review of his life reveals that psychiatric drugs may have triggered and even worsened his depressive episodes.
New FDA Study Shows Benzodiazepines Can Cause Long-Term Injury
The FDA has finally acknowledged the adverse effects of benzodiazepines, the dangers of withdrawal, and that the current packaging does not sufficiently warn of these harms.