The Reckoning in Psychiatry Over Protracted Antidepressant Withdrawal
Medically-induced harm—affecting tens of millions of people worldwide—has taken the field decades to take seriously.
Researchers Address Dangers of Polypharmacy and Inappropriate Medication Use
A new special issue brings together articles exploring the harmful effects of simultaneous multiple medication use.
Withdrawal Symptoms Routinely Confound Findings of Psychiatric Drug Studies
Researchers examine how rapid discontinuation can mimic the relapse of mental health symptoms and confound psychiatric drug studies.
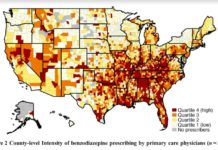
Benzodiazepine Prescriptions in Older Adults Used in Rural and Low Income Areas
Benzodiazepine prescription practices may be in response to an epidemic of distress, rather than being used to treat specific mental health diagnoses.
Nonclinical Factors are Associated with Long-Term Benzodiazepine Use in Older Adults
White race and size of initial prescription, along with poor sleep quality, are associated with long-term benzodiazepine use in older adults.
Can Education Level Predict Prescription Drug Misuse in Young Adults?
A new study examines the extent to which patterns in prescription drug misuse and substance use disorder symptoms can be predicted by education level
Unsafe Use of Sleep Drug Zolpidem is Common
Three out of four users of the sedative, zolpidem (brand name Ambien), do not follow FDA recommendations to reduce risk.
The REST Project Support Service for Benzo and Sleeping Tablet Dependence: My Story
As a service user of the REST project at Mind in Camden, I want to celebrate World Benzodiazepine Day 2018 by telling the world a little bit about what REST has done for me. I’m now 18 months off benzos, but I still attend REST regularly to process the anger and grief I feel about what I went through, and to support those who are still tapering.
Poor and Foster Care Children More Likely to be Diagnosed and Treated with Psychiatric...
Study details Medicaid-insured birth cohort’s exposure to psychiatric medications and mental health services.
My Ativan Affair and the Aftermath
My sincere message to those whose vitality and lives have been sapped and zapped by this iatrogenic dis-order: most of us DO recover! And even if it is not without some benzo remnants lodged in our cellular memory, what we learn about our own resilience will guide us to places in our lives we didn't expect to reach. HOPE was my key through the arduous path of withdrawal and recovery.
New Clinical Guidelines on Deprescribing Benzodiazepines
New guidelines recommend deprescribing benzodiazepine receptor agonists for adults.
Benzo Withdrawal: Why Don’t Doctors Know?
Many have asked: “Why doesn’t my doctor/provider know what is happening to me?” Benzodiazepine tolerance and withdrawal are not new. So, why isn’t it simple to diagnose and treat? As both a health care provider and a withdrawal sufferer, I’d like to offer an inside and outside perspective on this question.
Xanax: Children As Young As 11 Taking Anxiety Drug
From BBC: The abuse of the anti-anxiety drug Xanax is becoming widespread among children and adolescents as young as 11 years old.
"To gain an idea of the...
A Text Therapy App Plans to Start Prescribing Drugs to Users
From Business Insider: Talkspace, a text message-based therapy platform, is bringing on a team of psychiatrists to prescribe medications to patients. The app is also...
Online Communities for Drug Withdrawal: What Can We Learn?
From Psychiatric Times: Patients are increasingly turning to the internet as a source of information and support for antidepressant and benzodiazepine withdrawal due to the psychiatric...
Xanax Nation
In this blog post, Andy White highlights the role Xanax plays in silencing political dissent and keeping the public complacent. Instead of expressing anger...
Existential Therapy Assists Patients Withdrawing From Psychiatric Drugs
Confronting existential anxiety through “Basal Exposure Therapy” shows promising results in people withdrawing from psychotropic drugs.
A Quiet Drug Problem Among the Elderly
From The New York Times: Use of benzodiazepines has risen among seniors despite their increased vulnerability to the drugs' adverse effects.
"'Set aside the opioid issue,'...
CBT and Educational Intervention Reduce Chronic Pain, Study Finds
Research examines the effects of cognitive behavioral therapy (CBT) on experiences of chronic pain among low-income patients.
The Poison We Pick
In this piece for New York Magazine, Andrew Sullivan traces the history of the use of opiates in the U.S. and explores the social, economic,...
Psychiatrists Warn Policymakers Benzodiazepine Overuse Could Lead to Next Epidemic
Although opioid addiction and overuse have garnered significant national attention, similar trends in benzodiazepine overprescription and overuse continue to go unnoticed.
We Need to Encourage People to Make Advance Directives
In this piece for STAT, Jennifer Adaeze Okwerekwu describes the value of psychiatric advance directives for those at risk of experiencing an emotional crisis.
"'It’s something that can...
Benzodiazepines: Our Other Prescription Drug Epidemic
From STAT: Although benzodiazepines are some of the most commonly prescribed psychiatric medications in the U.S., few people realize how dangerous and addictive these drugs can be.
"Highly...
8 Years of Mental Health Research Distilled to 4 Infographics
Pictures are worth a thousand words. So I’ve chosen pictures to distill the mountain of mental health research I’ve examined over the last eight years. Three infographics summarize research on psychiatric drugs, and one asserts why I think Integrative Mental Health is the best path available for mental health recovery.
The Female Subject in Psychiatry From Pathology to Prozac
In this piece for The New Inquiry, Sophie Putka chronicles the mental health profession's long history of pathologizing, diagnosing, and medicating women's emotions.
"With Freud’s claims...