In the days prior to announcing her decision to end her candidacy for the 2020 presidential race, Kamala Harris released a plan to address “the mental health care crisis.” The plan was received with widespread applause from family members and those seeking to dismantle the civil liberties and privacy rights protections afforded to people with psychiatric labels. Harris’s plan was met with vociferous condemnation from psychiatric survivors, civil libertarians, and disability justice advocates, who vowed to fight it. While Harris has dropped out of the presidential race, the ideas behind her policy proposal have existed for decades, and are likely to endure.
Last month, the Senator from California declared to a crowd in Iowa: “mental health justice is on the ballot!” Harris said, “I have a mental health care policy that is robust, because I understand and have worked with these issues for years — that we have so much undiagnosed, untreated trauma in America. And we have got to stop stigmatizing this issue.” On November 25, Harris unveiled her mental health care plan in South Carolina.
We have failed to address trauma and mental health in our communities and in the criminal justice system for far too long. It's time for an intervention. pic.twitter.com/QMkyxwnJmm
— Kamala Harris (@KamalaHarris) October 29, 2019
Key elements of the Harris plan
Harris’s “mental health care crisis plan” is the latest iteration of a series of controversial mental health policy proposals, heavily influenced by pro-force and coercion caregivers and family members, that have surfaced over the last few decades at the local, state, and federal levels. These include former Rep. Tim Murphy’s (R-Pa) Helping Families in Mental Health Crisis Acts of 2013 and 2015, key provisions of which were folded into the 21st Century Cures Act in 2016; as well as the RESPONSE Act, introduced in October by Senator John Cornyn (R-Tx).
What these mental health policy proposals share in common is an emphasis on promoting a range of coercive and restrictive interventions that infringe on the rights and privacy of persons with psychiatric diagnoses; in particular, of those individuals meeting the criteria for “serious mental illness” (SMI). SMI is defined in the Harris plan as “mental, behavioral, or emotional disorders, such as schizophrenia or severe bipolar disorder, that substantially interfere with major life activities.” As Zoey Turtino writes in The Daily Campus, “This phrasing gives healthcare providers and policy makers free range to decide for themselves what is and isn’t considered a serious mental illness.” The pro-force advocates also frequently invoke the construct of anosognosia, or “lack of insight” into one’s condition, as both a defining characteristic of “SMI” and a pretext and justification for coercive and paternalistic policies. Psychiatrist Dinah Miller writes in Psychology Today that the term is “politically loaded: when someone uses it, by extension, it has come to mean that they are in favor of legislation to make it easier to treat patients against their will.”
Repeal of the IMD Exclusion
A cornerstone of the Harris plan included increasing access to inpatient hospitalization via the repeal of what is known as the Institutes for Mental Disease (IMD) Exclusion. The IMD Exclusion prohibits the use of Medicaid financing for adult psychiatric hospitalizations and residential facilities larger than 16 beds. This restriction was put in place at the very beginning of the Medicaid program in 1965 for a reason: to compel states to invest in community-based services instead of unnecessarily warehousing people in segregated institutional settings that are breeding grounds for abuse, neglect, and death.
The Harris plan called for doubling the number of treatment beds nationwide, with a priority focus on states said to have bed shortages such as Iowa, Nevada, South Carolina, and Michigan.
A key aspect of the narrative fueling Kamala’s plan is the oft-repeated assertion that “jails and prisons have become the new mental hospitals.” However, mental hospitals are also becoming the new jails and prisons, a fact which is rarely acknowledged in the mainstream media or by lawmakers. Recent suicide prevention requirements put forth by the Joint Commission, the accreditation body for psychiatric facilities, include substantial environmental adaptations that compel psychiatric hospitals to look and feel more akin to prisons rather than the therapeutic environments that they are imagined to be.
There is also a significant and growing body of research to show that psychiatric hospitalization is associated with an increased risk of suicide upon discharge, another fact rarely acknowledged in public narratives about the need for beds.
As Jennifer Mathis points out in a 2018 Psychiatric Services article advocating against repeal of the IMD rule:
“Although our mental health systems are in crisis, neither the IMD rule nor insufficient hospital beds are the primary problem. The primary problem is the failure to implement an effective system of intensive community-based services, which have been shown to prevent or shorten hospitalizations. Repealing the IMD rule would do little to alleviate the true crises in our public mental health systems and would likely deepen those crises.”
Regardless of one’s position on increasing access to institutions, a November 2018 Medicaid rule has essentially rendered the “need” for a legislative repeal of the IMD exclusion obsolete. The new rule, as mandated in the 21st Century Cures Act, encourages states to apply for Medicaid demonstration waivers to cover acute stays in IMDs, while also requiring states to demonstrate expanded access to community-based care options. In contrast, a legislative repeal of the IMD exclusion, as called for by Harris and others, would likely cost the Medicaid program around $40-$60 billion over a decade, according to a report by the Congressional Budget Office (CBO).
We are very happy to see @KamalaHarris release her plan on dealing with the mental health crisis. Highlights of Harris's plan include repealing the IMD exclution and doubling the number of treatment beds nationwide. Thank you Senator Harris! https://t.co/1sKdZrfXp6
— Treatment Advocacy Center (@TreatmentAdvCtr) November 25, 2019
Other presidential candidates have endorsed a repeal of the IMD Exclusion, including Pete Buttigieg (D) and Amy Klobuchar (D-Minn).
Increased funding and support for “Assisted Outpatient Treatment”
The plan also called for the expansion of funding and support for the “Assisted Outpatient Treatment” (AOT) program. AOT is a euphemistic term used to describe involuntary outpatient commitment ordered by a judge, with the threat of involuntary inpatient hospitalization for those who do not comply with their treatment orders. Harris’s plan says AOT is meant for those individuals who “sometimes fail to comply or cannot comply with treatment and become homeless, are arrested, or otherwise deteriorate without treatment.” AOT relies on what is called the “black robe effect” to enforce treatment compliance.
The Harris plan makes reference to “multiple studies” showing that AOT “improves treatment outcomes, lowers risk of arrest, violent behavior, and other criminal justice encounters, and reduces homelessness, all at lower costs and with fewer restrictions than inpatient treatment.”
Yet this characterization of AOT’s evidence base is based on a false interpretation of the existing scientific literature. As Robert Whitaker explains in a recent Mad in America Report, despite increasing state and federal support over the last two decades for AOT, there is scant evidence as to its effectiveness. To date, there have been only three randomized clinical trials (RCTs) of the program—two in the United States and one in the UK. A 2011 Cochrane Collaborative review of the evidence for AOT’s clinical and cost effectiveness resulted in findings that stand in strong contrast to the positive claims made by Harris and AOT advocates regarding the program. Whitaker goes on to note:
“In all three RCTs, there was no significant difference in outcomes. The Cochrane review concluded that compulsory outpatient treatment orders do not ‘result in better service use, social functioning, mental state, or quality of life compared with either standard voluntary or supervised care.’ The only superior outcome for those on compulsory orders in these three RCTs was that the patients were ‘less likely to be victims of violent or non-violent crime.’ Based on results from this review, there is no strong evidence to support the claims made for compulsory community treatment that make it so attractive for legislators.”
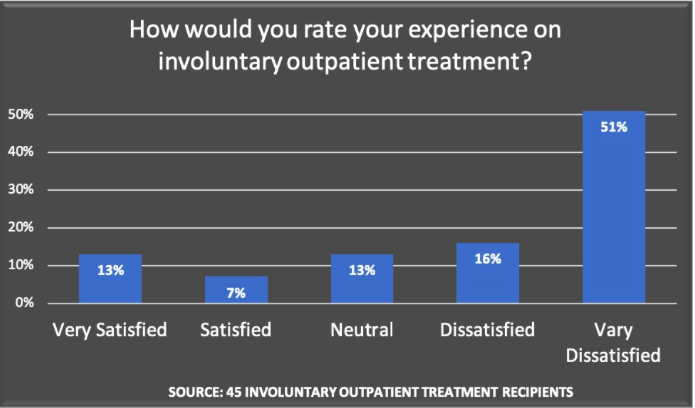
There has been little to no research conducted on how former and current recipients of AOT orders themselves experience the program. In a 2018 Mad in America survey of 45 people, over half of respondents indicated that they were “very dissatisfied” with AOT, and 16% were “dissatisfied.”
Amend HIPAA to include ‘good faith’ disclosures
An additional plank in the Harris plan revolves around substantially eroding the privacy protections afforded by the Health Insurance Portability and Accountability Act (HIPAA), originally passed in 1996. In the Harris plan, this plank is entitled “Amend HIPAA to ensure family members can adequately support persons with mental illness.” What this means is that the plan would create a lower standard of privacy rights for people with psychiatric diagnoses and disabilities, which would allow providers to disclose protected health information to family members over a person’s objection “out of a good faith belief that it was necessary to enhance the health, safety, or welfare of the person involved or the general public.”
This proposal closely mirrors that of the HIPAA-weakening provisions found in Tim Murphy’s Helping Families in Mental Health Crisis legislation of 2013. These provisions were substantially toned down in the 2015 version of the legislation, due in large part to the efforts of disability and privacy advocates. The HIPAA provisions that were eventually folded into the 21st Century Cures Act do not alter the privacy law; instead they call for HHS to clarify the law in such a way as to “ensure that health care providers, professionals, patients and their families, and others involved in mental or substance use disorder treatment have adequate, accessible, and easily comprehensible resources relating to appropriate uses and disclosures of protected health information under HIPAA, and to issue guidance to clarify permitted uses or disclosures of protected health information.”
HHS has since issued such clarifying guidance on HIPAA, in compliance with the Cures Act. But this development has not deterred pro-force advocates from continued calls to dismantle the privacy law as regards people labeled with SMI, even if such efforts actually defy Congressional intent as spelled out in the Cures legislation.
In a 2019 joint letter to the Department of Health and Human Services (HHS), the American Civil Liberties Union (ACLU) and the Bazelon Center for Mental Health Law write: “The HIPAA Rules already contain the flexibility to permit communications between healthcare providers and with family members. But misunderstanding or misinterpretations of HIPAA have led to calls for its reform. Agency efforts would be better spent in providing more information and education as to the flexibility and constraints of the Rules, rather than to undertake revisions.”
The letter goes on to say that “HIPAA Rules already permit family, friends, or others who are involved in the patient’s care to receive protected health information that they need to know about the patient’s care under appropriate circumstances, including: with the patient’s permission; when the patient has been given the opportunity to object but does not; when a person poses a danger that could be averted by disclosure, in emergency circumstances, and when a person lacks the capacity to consent or object to disclosure.”
Reclassify “schizophrenia, schizoaffective, and bipolar disorder” as neurological illnesses
An aspect of the Harris plan that has received far less attention than the policy planks mentioned above, yet is at least as controversial, is the move to reclassify “schizophrenia” and related disorders as neurological conditions. The rationale, as stated in the plan, is that “while these conditions are currently classified as ‘behavioral,’ a classification that accentuates their neuroscience will improve access to treatment and research funding.”
This rhetoric is aligned with a sustained push for the reclassification of schizophrenia, led by the advocacy group Schizophrenia and Related Disorders Alliance of America (SARDAA) and supported by the Treatment Advocacy Center and the National Alliance on Mental Illness. In May 2018, SARDAA requested to have schizophrenia included in the implementation of the National Neurological Conditions Surveillance System (NNCSS) provided for in the 21st Century Cures Act. NNCSS is a CDC program that received $5 million from Congress to gather data on the prevalence of and risk factors for neurologic conditions in the US population. Linda Stalters, a retired nurse who is CEO and founder of SARDAA, told Medscape Today, “We have the support of other organizations, family members, and patients, and there are multiple private Facebook pages supportive of caregivers and patients — for example, one has over 7000 participants, including people who hadn’t originally been supportive of this movement but are now.” SARDAA held a reclassification symposium on November 4 in New York City.
Reclassification efforts in the US occur amidst the backdrop of international advocacy efforts to do away with the diagnosis altogether, such as the Campaign to Abolish the Schizophrenia Label (CASL), headed up by psychiatrists Jim van Os and Marius Romme, as well as psychologists John Read and Richard Bentall, among many others. As Bentall told BBC News: “We do not doubt there are people who have distressing experiences such as hearing voices or paranoid fears. But the concept of schizophrenia is scientifically meaningless. It groups together a whole range of different problems under one label — the assumption is that all of these people with all of these different problems have the same brain disease.”
In a 2018 letter on the occasion of Schizophrenia Awareness Week, the International Society for Psychological and Social Approaches to Psychosis (ISPS) – Australia summed up over a decade’s worth of efforts to abolish the label: “We argue that the term schizophrenia is unscientific and stigmatising — it does more to harm than help people who may experience these extreme states.”
The Disability Community Fights Back
The Harris plan was immediately met with a swift public response from people living with psychiatric diagnoses and disabilities, as well as cross-disability advocates. Alice Wong, founder and director of the Disability Visibility Project, and co-partner, #CripTheVote, created a compilation of “responses, concerns, and critiques from mentally ill and disabled people & others.”
Vilissa Thompson, creator of #DisabilityTooWhite and founder of @RampYourVoice, and Dr. Amelia N. Gibson both questioned the HIPAA plank in Harris plan, and its assumption of universal “good faith” among mental health providers.
Do you know how many horror stories I know of that involves helping professionals who did NOT act in “good faith” to the clients they served in the mental health services field?
LOTS.
— Vilissa Thompson (@VilissaThompson) November 26, 2019
https://twitter.com/AmeliaNGibson/status/1199181407555399681?s=20
Freelance journalist and commentator Sara Luterman, in a Vox essay entitled “How Kamala Harris’s mental health plan could hurt the most vulnerable,” describes a 2014 experience with hospitalization for suicidal thoughts as “one of the most harrowing and dehumanizing experiences of my life.” Luterman characterizes the psych ward as “a world in which rights are just suggestions, and where staff exert an exceptional amount of control over every aspect of your life.”
Luterman explains how calls for increased “access” to inpatient psychiatric care run directly counter to the idea of “access” as enshrined in the Americans with Disabilities Act (ADA): “The ‘access’ promised in Harris’s plan is to locked wards, forced drugging, and the denial of the same right to privacy afforded to other Americans. Her proposed policy distorts ‘access’ beyond recognition.”
And Luterman writes of the high discontinuation rates of prescribed antipsychotics and mood stabilizers, the very drugs that people under AOT orders are typically compelled to take: “This is not because people are stupid or lack insight into their own illness. Antipsychotics and mood stabilizers tend to have heavy side-effect profiles.” She adds: “Assuming that a person is incompetent and that their perceptions are irrelevant will not make that person want to participate in mental health treatment.”
Azza Altiraifi underscored the ways in which the plan magnifies the violent intersectional oppressions faced by people of color in the carceral and mental health systems, tweeting: “This plan reflects the violent convergence of anti-Blackness, racism & sanism that undergirds the carceral state.”
https://twitter.com/Azza_Alt/status/1199153323812806662?s=20
AOT, where it has been implemented, is often done so in a highly biased manner. According to a 2014 report by the Maryland Disability Law Center et al, “Studies on outpatient civil commitment conducted in North Carolina and New York revealed that people of color and those living in poverty are disproportionately impacted by involuntary community treatment orders.” The 2005 NYLPI report found that the implementation of AOT in New York is “severely biased.” In New York, African Americans were subjected to court orders five times more frequently than whites, while Latinx persons were two and a half times more likely than whites to be under a court order.
In North Carolina, two-thirds of individuals court-ordered to community treatment were African American, despite only representing 22% of the total state population. And 88% of AOT orders in New York were found to include some forced medication component. This is especially concerning due to the increased risk of long-term severe side effects that African-Americans can face from antipsychotic medication.
Other advocates pointed out how the erosion of HIPAA protections could tilt the power dynamic in favor of domestic abusers and family members wishing to interfere with their adult trans children’s access to medical care. As Zoey Turtino writes in The Daily Campus, “This would be especially devastating for transgender youths seeking medical care without the knowledge of their potentially abusive parents.”
Victoria Rodriguez-Roldan, director of the Trans/GNC and Disability Justice Projects at the National LGBTQ Task Force, told The Hill: “A basic rule in mental health advocacy is that if the policy is being proposed solely by family members, then odds are it will be harmful,” adding: “This is because often we operate with the assumption that those relatives are the ones who know best, rather than those with lived experience, and fail to acknowledge how many times, those loved ones are not necessarily so loving, such as domestic abuse situations.”
Disability advocate and civil rights lawyer Alison Barkoff created an in-depth Twitter thread to explain what Kamala Harris got so wrong, and “what she SHOULD have focused on.”
I have spent much of the last 2 days thinking about the mental health plan from @KamalaHarris and how she could have gotten it so wrong. This thread is about that and what she SHOULD have focused on. #CripTheVote (1)
— Alison Barkoff (@AlisonBarkoff) November 27, 2019
The thread reflected on the Olmstead vs. LC decision, which began with plaintiffs Lois Curtis and Elaine Wilson, two women from Georgia living with psychiatric diagnoses and intellectual disabilities. Curtis and Wilson cycled in and out of hospitals, unable to receive the supports they needed in the community. The landmark Olmstead decision requires states to eliminate unnecessary segregation of persons with disabilities, and to ensure that persons with disabilities receive services in the least restrictive setting, and one that is appropriate to their needs. In the thread, Barkoff explains and provides evidence for how the Olmstead Rule, when enforced and implemented, results in a reduction in both incarceration and hospitalization.
In speaking only to family members regarding “SMI,” Harris was led to espouse principles that ran directly counter to her own disability plan.
The psychiatric hospitals in Olmstead are the very “Institutions for Mental Disease” that Harris proposes to double the number of beds in! If she looked at DOJ #Olmstead settlements, she'd understand that her proposal would move states further from complying with the law! (9)
— Alison Barkoff (@AlisonBarkoff) November 27, 2019
At every turn, the disability community has fought the pro-force agenda, often managing to weaken the most coercive policy proposals without eliminating them altogether. Advocates mobilized quickly to respond to the worst aspects of the Harris mental health plan. They share that Harris was about to issue a revised plan in response to the disability community concerns, which would have eliminated the IMD repeal plank, the AOT plank, and the reducing HIPAA privacy rights plank. The Harris campaign was instead planning to include more of an emphasis on enforcing Olmstead and expanding community services first before developing more hospital beds.
The Pro-force Agenda Is Not Going Anywhere
Over the last twenty years, a growing cadre of caregivers, family members, and grassroots organizations, calling themselves the “SMI community,” have been wildly successful in promoting the pro-force agenda, both in the mainstream media and in local, state, and national policy.
Robert Whitaker and others have written about the decades’ long crusade of Dr. E. Fuller Torrey to increase force and coercion, and to reduce privacy protections throughout all aspects of the U.S. mental health care system. In 1998, Torrey founded a national advocacy and media mouthpiece in the Treatment Advocacy Center, of which DJ Jaffe, author of Insane Consequences: How The Mental Health Industry Fails The Mentally Ill and creator of MentalIllnessPolicy.org, was a founding board member. Both Torrey and Jaffe are frequently consulted by both the right and left-wing media as policy experts, and their views are frequently amplified by journalist Pete Earley in his popular newsletter and blog.
On Facebook and in his newsletter, Jaffe took partial credit for the Harris plan, with credit also going to Scott and Leslie Carpenter. The Carpenters are an Iowa couple, parents of a son labeled with SMI, who have been distributing pro-force policy documents to the candidates visiting Iowa ahead of the presidential election. From their position, they are well poised to exert an ongoing influence on presidential candidates. The Carpenters are also credited directly on multiple occasion by Ron Powers, author of the 2017 New York Times bestseller No One Cares About Crazy People: The Chaos and Heartbreak of Mental Health in America.
Powers wrote an effusive blog in support of the Harris plan, in which he stated: “In one breathtaking stroke, Kamala Harris has just widened the contours of presidential campaign history and thrown light into the darkest corridors of shameful human suffering.”
Powers also wrote a blog entitled “The Anti-Treatment Empire Strikes Back” as a response to Sara Luterman’s Vox piece critiquing the Harris plan. In it, Powers resorts to a tactic often employed by the pro-force advocates: to discredit their critics through ad hominem attacks and strategic falsehoods. In this blog, Powers describes Luterman as being “anti-treatment.” But Luterman does not take an “anti-treatment” stance, just an anti-forced treatment one.
Luterman clarified: “I’m against the use of force to push medications and treatment modalities that can be harmful,” adding: “Some people are overmedicated. Some people don’t actually do better on meds and would be fine with more holistic interventions. People deserve to make such major choices about their own lives.”
In a further effort to discredit Luterman, Powers accuses her of being a “Szazian,” and by extension, possibly a Scientologist. Luterman is not a Scientologist, and told this reporter via Twitter that she has never even read Szasz. “They just made a bunch of stuff up about me out of whole cloth,” Luterman said.
In recent years, additional family members have written books with policy positions mirroring those promoted by Dr. Torrey, DJ Jaffe, Ron Powers, and their acolytes. These include DeDe Ranahan, a self-described member of the “SMI community” who wrote a book entitled Sooner than Tomorrow: A Mother’s Diary about Mental Illness, Family, and Everyday Life. Ranahan appears to be using her platform as an author to mobilize for a pro-force agenda, with a focus on the current crop of Democratic presidential hopefuls. In August, journalist Pete Earley published her group’s Five Point Plan on his website, as did Ron Powers, from which the Harris plan lifted heavily and directly on nearly every single point, down to the fine details.
While Harris is out of the race, the extremist ideas that inspired the first draft of her mental health plan, which remains on her website, continue to endure and proliferate. Over the last twenty years, the current socio-political climate has been heavily influenced by the pro-force agenda. The American public and lawmakers on both sides of the aisle are ever-more receptive to the narrative that certain people with mental health problems are dangerous and/or “lack insight,” and therefore must be forced into treatment against their will.
A study published in October in Health Affairs found that public perceptions regarding potential violence and support for coercion have been rising, especially concerning the diagnosis of schizophrenia. The study’s authors concluded: “Despite solid evidence that people with mental illness are unlikely to be dangerous, such prejudice can lead to support for inappropriately using legal means to force people into treatment.”
And the SMI community isn’t going anywhere. On December 5, shortly after Harris’s exit from the Democratic presidential race, Ranahan published an updated and expanded version of the original Five Point Plan. The new plan seems to target Olmstead protections specifically raised by disability rights advocates. There is a point under “Pay attention to supportive housing” that states: “Clarify Olmstead for SMI. Least restrictive care isn’t always least expensive or best” and “Examine, don’t ignore, a person’s ability to handle and benefit from a less restrictive setting.” This rhetoric aligns with consistent efforts on behalf of the pro-force advocates to divorce the arbitrary category of “SMI” from the rights and protections afforded to all other persons with disabilities or diagnoses.
Under the “Revamp Involuntary Treatment” category, the updated plan advocates to expand the criteria for forced mental health care, calling for “lack of insight (anosognosia) and grave disability as criteria for determining involuntary treatment.” The group wishes lawmakers to “Establish a federal standardized ‘need for treatment’ involuntary commitment law” and, in an apparent response to Olmstead, says to “Base restrictive settings on actual abilities, not wishful thinking or one-track plans.”
Ranahan clarifies the SMI community’s plans to influence candidates going forward, with a strategy to “Refocus our efforts on the remaining candidates — Republican and Democrat. Right now Buttigieg and Klobuchar have good plans. Warren and Booker are working on plans. The White House will be hosting a summit on Transforming Mental Health Treatment to Combat Homelessness, Violence and Substance Abuse on December 19. Thank you for your help.”
The Harris mental health plan rallied the disability community once again to fight for “Nothing about us, without us” and to demand an acknowledgement of the principles of the Olmstead decision. Now, the SMI community has Olmstead in the crosshairs. Decades of hard-won rights to liberty, self-determination, and privacy are in the balance.
“All we can do is share information,” Kathy Flaherty, executive director of the Connecticut Legal Rights Project, told The Hill. “It’s the elected officials or their staff who have to carefully consider all the information they receive and then make responsible, well-informed decisions. . . . Clearly we are still learning how to most effectively communicate our message to folks at the national level, but I do think ultimately it’s on them to do a bit more to facilitate access.”
https://twitter.com/aneeman/status/1199178233973018624?s=20
****
MIA Reports are supported, in part, by a grant from the Open Society Foundations





The noose tightens…
Isn’t it interesting that the so-called ‘left’ are more authoritarian than the the so-called ‘right’?
Report comment
Authoritarianism knows no party or political persuasion.
Report comment
Steve
Your comment is confusing at best, and tends to reinforce the “authoritarian” view that human beings will ALWAYS be authoritarian.
This is, in the final analysis, a justification for people to ultimately accept the status quo, and stop dreaming of, and working towards, a world FREE of authoritarianism.
Your comment reinforces the view that we all need to accept the fact that human beings will ALWAYS need to live in some sort of class based (authority) type capitalist society, because somehow this corresponds to some sort of “forever” human characteristic that can never change.
There ARE, and CAN BE, “political persuasions” that advocate for, and work towards, a world free of “authoritarianism.”
Steve, are you denying this possibility?
Richard
Report comment
I didn’t say a lot of what you think I said, Richard. I think it’s important to be careful not to read into posts things that are your assumptions. I’d prefer if you’d simply ask for clarification if what I said is confusing.
I believe that a lot of the current population is authoritarian, at both ends of the political spectrum, based solely on my own observation of people’s behavior. I believe this is mostly because of our authoritarian means of educating people and our ubiquitous authoritarian structures which seem to be “the only way” because people don’t SEE another way ever demonstrated to work. I certainly know people who are not authoritarian and believe that non-authoritarian structures can be found and/or created, and have spent a good proportion of my time on Earth working to create that possibility. However, it’s not as easy as it sounds, because we have all had this stuff hammered into us from birth, and people who are NOT authoritarian are punished for following their path. Naturally, authoritarianism occurs on a spectrum, and people are pushed back and forth based on how their efforts are perceived and reacted to by those around them. So encouraging anti-authoritarian thinking is possible and will push people in the direction of seeing things that way. But just as obviously, those who are running the current society are very invested in maintaining the current power dynamics and use authoritarian tactics to maintain them and push people to a more authoritarian view of the world. Revolutions have historically not always led to real change, because the internalized authoritarian underpinnings of the social system were not addressed, and the new rulers step into the authoritarian roles that they and the society they are part of feel comfortable with. This is a big part of why the current “liberals” in the USA have such a hard time supporting antipsychiatry as a movement – they are unable or unwilling to challenge the idea that doctors generally have their best interests at heart and should be trusted to make up rules that the rest of us should follow. That’s authoritarianism, and you see how strong it is when you try to talk to some (not all) “liberals” about the human rights concerns of those labeled “mentally ill,” with whom their stated philosophies should have great solidarity. But they don’t, because it’s not in their own structure of what is “right” and “good” and “wrong” and “bad.” They accept the authority of the doctor without questioning it. I saw a lot of this when working on creating democratic schools, where kids are mainly responsible for making up their own school rules and enforcing them. Parents and teachers SAID they believed in these principles, but when the kids’ standardized test scores started to come into play, or the District started complaining about the vagueness of the curriculum, they started getting unconsciously very nervous and bit by bit re-instituted authoritarian structures that were opposed to the mission, because they really weren’t quite comfortable themselves trusting kids to wield all that power themselves, much as they wanted to believe that they backed the mission 100%.
The world is not a black and white place. I can certainly go into examples from our current world where people on the “left” engage in authoritarian behavior and don’t recognize it as such. Examples on the “right” are perhaps more obvious and easy to identify, but the idea that all authoritarians are right-leaning politically is just plain not borne out by the facts. There are also people who identify as “conservative” who are actually quite anti-authoritarian. We need to become more aware of this if we really want to change the way we’re doing business. Because in the end, “society” exists within the people who create and participate in it, and if we want to create a new society, we have to understand our internalized oppression and deal with it, or else we will perpetrate it in our new society as well. As the Who sagely suggested, we want to avoid a “Meet the new boss, same as the old boss” situation. It is not enough to change the external structures of society. We have to change our own internalized structures, too. And that’s a lot of hard work that few are ready to take on, in my experience. That may seem jaded, and maybe it is, but it doesn’t mean I don’t think it can be done. I am saying that, as discouraging as it sounds, this reality MUST be dealt with, and pretending that it doesn’t exist will doom further revolutionary efforts to failure or limited success. We do ourselves no favors by ignoring this particular set of facts about human behavior.
I hope that clarifies things.
Report comment
Steve
Thanks for your thoughtful response. I addressed this issue in a challenging way because I have read very similar comments by you on other occasions, and never got around to responding to you (my bad).
We need to be very clear when we use the “Left” or “Right” labels (as Oldhead has pointed out many times) because its definition is now so confusing to people , when for example, Hilliary Clinton or some other Liberal can be called a “Leftist.”
I define “Leftist” as someone who believes that humanity needs to move BEYOND a capitalist system towards socialism, as an historical transition to a truly communistic classless society.
People who have made genuine attempts to fight for, and build, socialism and move towards a classless society SHOULD NOT be equated (even when they make authoritarian type mistakes) with those on the “Right” who either operate an exploitative capitalist society, and/or advocate for one.
Yes, it is true that some formerly genuine socialists (Leftists) can transform themselves into becoming oppressive authoritarians. In these cases they end up actually wanting to “go back” and/or preserve some sort of class structures that will benefit them and their family at the cost of the majority of people (they then become counter-revolutionaries). Thus, we ultimately have a RETURN to some form of capitalism (or as we call it, “state capitalism” as formerly existed in the Soviet Union, and now exists in China) – Russia is now openly capitalist in both name and deed.
Other genuine Leftists, did NOT want to return to capitalism, but instead, made authoritarian (and other related) type mistakes that set back the course of revolutionary change. These mistakes (even serious mistakes), in the course of valiant attempts at Revolutionary change are a complicated combination of ignorance, trial and error, and very much related to the horrendous pressure applied to defeat these revolutions by the old defeated capitalist class, and other countries fearing the growth of Revolutions around the world.
Steve, you said: ” Revolutions have historically not always led to real change, because the internalized authoritarian underpinnings of the social system were not addressed, and the new rulers step into the authoritarian roles that they and the society they are part of feel comfortable with.”
Here, if you are talking about “the birthmarks” of the old system reasserting themselves in the new society, then I can agree with you.
But, we must remember that historical attempts at transitioning BEYOND capitalism to socialism/communism, are ONLY a hundred and fifty years YOUNG. This is a relatively short period of time on a human historical scale. Most new experiments in both science and in the social world will NEVER succeed on just the first few attempts.
Why did the prior historical attempts at socialist/communist revolutions fail? Is this somehow because there is an “authoritarian” flaw in human nature, or are there other more scientific and ultimately knowable explanations for these unrealized (and defeated) attempts at Revolutionary change.
To simply repeat phrase about “authoritarianism” being endemic to “all” political persuasions on both the “Left” and the “Right” contributes to a commonly accepted narrative pushed by the defenders of capitalism and the status quo. This is a narrative that lacks any attempt to do justice to an accurate historical summation of revolutionary attempts over the past 150 years.
Steve, I am NOT saying this was your intention, but we all must be careful with the phrases we choose to repeat, and how that particular vernacular is interpreted by most people in today’s society.
Richard
Report comment
I think I understand you better at this point. I was simply stating that SOME authoritarianism can be found everywhere, because it is endemic to our society. By no means do I mean to suggest (or did I suggest) that it simply “human nature” – I believe, as I stated, that it is TRAINED into us from birth onwards, both explicitly by parents and churches and educational institutions and so forth, and implicitly by being the only game clearly on display, and by the hostility expressed toward those who refuse to go along with the status quo. It is a challenge to overcome that kind of training for anyone. For instance, in the “dictatorship of the proletariat” concept, the idea is that there is a temporary period during which the new ideas will become held by a majority of the people in the society, allowing this dictatorship to melt away. But during that period, there is an authority in charge of what should be taught and how it should be taught, and those doing the “teaching” ALL grew up with these authoritarian models of education. So it requires real care and attention not to replicate the same forms that we’re comfortable with, as my example of the “democratic school” shows so clearly. It is not enough to just believe in a revolution, we have to pay attention to how it will happen and what will happen afterwards. I don’t think it’s doomed to failure, but I do think these challenges are great, because a lot of the ideas and models we carry are not conscious (kind of like implicit racism or other unconscious biases). I have always found it of the greatest importance to address the dilemma of being a person of privilege and authority trying to help others to find their own freedom. How easy it is to fall into saying, “Do it my way, it works for me.” It is a challenge we must all keep at the top of our awareness any time we’re working for real empowerment of ourselves and others. That’s my experience anyway.
Report comment
And just for the record, I don’t equate efforts to maintain the status quo at all costs, which tends to be the ‘right’ leaning form of authoritarianism, with efforts to force one person or group’s vision of change on society by force, which tends to be the ‘left’ leaning form, in my view. Fascism is fascism, it’s authoritarian for sure, but not all authoritarians lean toward fascism. As you well know, there have been plenty of ‘socialist’ dictatorships and lots of human rights abuses done in the name of “socialism.” My only real point is that ONLY looking to the “right” for authoritarianism fails to take into account the internalized oppression we’ve all experienced which leaves every one of us vulnerable to either kowtow to or engage in authoritarian tactics in the service of what seems to us to be a worthy goal. It is something that must be consciously identified and resisted if we’re going to create a different kind of society.
Report comment
Given ALL the difficulties you describe about moving away from abusive forms of authoritarianism in building a new society, we must seriously address the question of RISK/REWARD.
Yes, the path moving toward a more egalitarian society free of all forms of oppression. war, trauma etc., including ending psychiatric abuse, will be long and extremely difficult.
But doing nothing (for fear of failure), OR falling for all the many traps of trying to reform a capitalist system that is functioning in a way that it is intrinsically designed to function. are both recipes for disaster.
Either Imperialist war and/or climate change will certainly destroy this plant if we unable to move beyond the capitalist system and actually achieve (through revolutionary change) a non-authoritarian socialist system as a step toward a truly classless society.
For these kind of changes to have a CHANCE of happening, we (those who believe this is necessary) need to change our attitudes AND LANGUAGE.
We need to articulate just how dangerous it is to accept the status quo, AND/OR, how dangerous it is to advocate for SLOW change.
We need to be willing to take some RISKS in making systemic change, with no absolute guarantees of success. If we don’t. this world is in danger of being destroyed.
Our LANGUAGE (including how we talk about authoritarianism) needs to reflect some of our willingness to take risks (I’m not talking about impulsive or foolish risks), but carefully summing up the past attempts at socialism (the good and bad), and then boldly move forward.
This conversation is NOT off topic. It is my view that we cannot end psychiatric abuse without ALSO ending a class based capitalist system.
Psychiatry and Big Pharma are TOO BIG AND IMPORTANT to “The Powers That Be” to be allowed to fail. The program and laws promoted by K.Harris actually targets the more rebellious sections of society. It leads to more drugging and social control of those sections in society who are most likely to be a part of the Revolution we need.
Richard
Report comment
By all means, we should never stop working toward that goal. We simply need to do it in awareness that AUTHORITARIANISM is a deadly foe that is larger than capitalism itself. Freedom and mutual respect and support are the goals we need to pursue, not a different system with different bosses and different people in powerful and oppressed roles. But I think you agree with me on that point.
Report comment
Steve, you make the mistake here of conflating liberals with leftists. “Liberal” is just another brand of capitalist, along with “conservative.” Of course liberalism is totalitarian. (This is not to say that genuinely leftist governments cannot also be authoritarian, but this would be a contradiction, and politically incorrect in the true sense of the word).
Another consideration is that some authority is legitimate, and exerting legitimate authority mandated by the people’s wishes does not constitute “authoritarianism.”
Also (quoting Richard L.):
But, we must remember that historical attempts at transitioning BEYOND capitalism to socialism/communism, are ONLY a hundred and fifty years YOUNG. This is a relatively short period of time on a human historical scale. Most new experiments in both science and in the social world will NEVER succeed on just the first few attempts.
I have often analogized the effort to defeat capitalism and establish socialism to the development of the airplane, remembering the films we used to watch in school of early experiments in flight — planes with flapping wings & the like that crashed & burned. Now even space travel is treated as second nature.
Report comment
I suppose if we define a “real leftist” as someone committed to actual empowerment of the masses, then I would agree with you. But there might not be a lot of “real leftists” around. There could certainly be people who are sincere but confused, or who have difficulty overcoming their authoritarian programming. The folks at the school I refer to for the most part really did believe in the model, at least to start with. They just got nervous and started panicking. It takes a lot of courage to really stick to one’s mission in the face of the training and pressure to the contrary. And there are a few people around pretty much any group who are mainly interested in gaining control of the group, and are only faking commitment. One school I helped create was destroyed by such a person.
As to legitimate authority, of course, I’d agree with you 100%. When I talk about authoritarianism, I’m talking about the acceptance of certain people as authorities regardless of legitimacy, and authorities expecting compliance with their demands without question, as well as both authorities and members attacking on those who are willing to question the dogma of the authoritarian group.
Again, I’m not trying to say this is hopeless or that we should give up. I am merely saying that one needs to be constantly vigilant about authoritarian types making their way into such an organization, as well as being vigilant that one’s own subconscious needs for control and safety don’t overshadow the goal of empowerment of the populace.
Report comment
Generally true — but a genuine revolutionary movement would be capable of holding authoritarian-minded individuals in check. Though socialism constitutes a “dictatorship of the proletariat,” this refers to a class of people (i.e. the 99%) being in control, not an individual throwing orders around.
There are currently no truly socialist states left btw; Cuba would probably be the closest. Hopefully this is just an interlude between phases of history, and once people as a whole gain a greater understanding of what the system is, and how it works to suppress human aspiration, we will experience a rebirth of revolutionary thought that makes the 60’s look like child’s play.
But there might not be a lot of “real leftists” around.
Or maybe we’re all hiding under rocks at the moment. But you’re right that currently many so-called “progressives” who mistakenly consider themselves “leftists” are particularly guilty of totalitarian thinking, and confuse genuine struggle with their social lives, and their need to be seen as “woke” by their friends. For example they use terms like “systemic racism,” but are clueless as to what “system” they’re talking about and what it means to actually fight racism, not just pontificate about it.
Report comment
Very well said. Can’t disagree with a word of it.
Report comment
There is one very BIG difference in this discussion about “Left” and “Right,” and why it is NOT a good idea to equate problems with “authoritarianism” within both political persuasions.
Those people on the “Right” who defend capitalism and class based societies as a necessary form of political and economic formation, believe that human beings can NEVER rise above the need for some form of “authoritarianism.”
They base this belief on the theory that this conforms to a forever (selfish) flaw in human nature. They also worship at the throne of some sort of “Libertarian” right of individual freedom, that somehow supersedes the rights of the collective whole.
Both of these outlooks by those who adhere to a “Rightist” political persuasion, guarantees the continuation of the status quo of a capitalist/class based society, where the bottom line of “profit first” will always guide us into competitive Imperialist wars and the further destruction of the environment, along with all the other problems of a commodity based culture.
ON THE OTHER SIDE, a genuine “Left” perspective advocates for, AND believes, that a cooperative classLESS society is both necessary AND possible. Thus their goals and intention is to eliminate ALL form of “authoritarianism.”
Genuine “Leftists” do NOT believe that human nature has any permanent fixed flaws, but it is quite malleable and capable of the creative conscious transformation of the world into a place with ever increasing amounts of freedom, where exploitation, trauma, war, and violence can gradually be eliminated (over hundreds of years) from social society.
Of course declaring one’s beliefs about human nature and about what kind of societies are both necessary and possible in the world. is very different than actually living up to those ideals AND making it happen in the real world.
BUT these distinctions between “Left” and “Right” are very important to be understood, AND they have deeply important moral and political implications about where we choose to stand in the world, and how we go about making the world a better place, including eliminating ALL forms of psychiatric abuse.
Richard
Report comment
Well someone needs to somehow untangle the situation. It is largely the fault of those who claim to be “revolutionary” that the populace is so politically clueless that Limbaugh & Hannity can label Democrats “leftists” and “socialists” without a peep, and without true leftists and socialists coming out en masse to clarify what socialism IS.
Report comment
Harris is a neoliberal (the Democratic version of a neoconservative). Liberals are not “leftists,” no matter what they or Sean Hannity believe.
Report comment
See above.
Report comment
In a sense this is the real “mental health crisis” in the world today: That so many people are convinced that they need authoritarian (which is to say, basically criminal) actions to handle situations in society that “we don’t have answers for yet.” The authoritarians are poised to continue to move in on governments (in particular) and other sectors of society that don’t know how to deal with the situations modern life is throwing at them. To the extent that this world remains technologically advanced, the authoritarians have an advantage and will continue to make inroads. A lot of people are rather sure that this will continue and we will end up losing our freedoms to an advanced technological society with anti-people weapons too dangerous to be confronted. Those people don’t realize that Earth is different and that we fully intend to handle this and take Earth in a new direction. Our work remains badly fragmented, but I do think that we can get better organized, find the best ways forward, and make it happen.
Report comment
To those people here and elsewhere, who want to move away from the DSM, and reclassify it as “trauma”, neurological, or some other basis.
I can only warn about, still in some way sticking to ‘suffering’, because I can tell you, psychiatry will take those systems over also.
The way a few people dealt with their children being labeled ADHD, is home school or private. They did not immediately run to a naturopath to ‘deal’ with the child.
Because often in doing so, we are simply believing in the diagnosis, and not celebrating differences in people.
I would not ‘treat’ my child for something that someone else noticed or was dissatisfied with.
Report comment
You mean shrinks will start treating folks with brain cancer, Lyme disease, and epilepsy like wanted criminals?
Report comment
Rachel,
Psychiatrist do treat those diseases now. If you become unable to sleep due to pain from your physical malady etc, it’s depression and can quickly escalate.
Physicians and Psychiatrists like to co-operate. Physicians often dislike yet support psychiatry.
Report comment
They do a great job at concealing their dislike. I no longer trust the medical profession because of this collusion.
Like a city run by a crooked police force. It may be just 5% of the police breaking the law they claim to uphold. But they couldn’t do it without all the rest supporting and covering for their corrupt buddies.
Report comment
Yes Rachel, if you get treated for what you are told is terminal cancer and develop insomnia from the cocktail of chemo drugs and steroids you can be sent to a shrink, given 4 labels and an assortment of psych drugs.
Report comment
Thank you, Leah. I always appreciate the clarity and depth of your reporting.
One thing I think was not well spelled out in this piece are the environmental conditions that contribute to the mental distress that disproportionately leads minorities and the impoverished (two groups that overlap considerably) into forced treatment. It isn’t just racism in the doctors office causing these disparities, let’s talk about lead in the urban water systems, police patrolling of certain communities, food and housing insecurity, the school to prison pipeline, the gig economy, wages that haven’t kept up with inflation, the unbanked, generational trauma (which is a much deeper and more nuanced topic than simply familial abuse), never-ending wars (see the newly released ‘Afghanistan Papers’) that siphon money away from maintaining basic infrastructure (crumbling bridges, aging water systems, and mold in schools).
We’re hearing a lot about the effects of trauma these days but very little in policy proposals to address that on a societal scale (beyond taking children away from home and subjecting them to the additional traumas of foster care) and the so-called “trauma-informed“ community is still largely taking an individualistic and responsive approach to traumatized individuals (a la teaching mental health and coping strategies in schools, for example) instead of addressing the conditions that are causing it. I find these efforts to create “trauma informed” spaces to be extraordinarily disingenuous. It’s almost as if there is NO political will at all to see the extraordinarily oppressive conditions so many people experience in the third world country known as the United States of America.
One last note is that Kamala Harris spent her career locking people up – including many POC without her own privilege. It’s not in the slightest bit surprising that her approach to emotionally distressed individuals is similarly laced with the language of force and control. If anything, these efforts bolster the arguments of those of us who understand psychiatry to be an extension of law enforcement for the purpose of social control.
Report comment
I also very much appreciate the very last tweet that was included which stated that “Bad mental health policy is, regrettably, a bipartisan enterprise.”
Report comment
If ‘bad mental health policy’ means denial of due process, segregating and gas lighting select individuals, and slowly crippling and killing the weakest–including newborns–I agree.
But it probably means the laws are not draconian enough and we aren’t dying fast enough in large enough numbers to suit the powers that be.
Report comment
I cannot disagree with any of the above. However, as a survivor of a random assault from someone who is both Schizophrenic and free to roam, I would ALSO advocate for funds to help people rehabilitate and rebuild their lives after getting their asses kicked by people who have a hard time living in society. I do not wish the guy any ill will or punishment but I also do not feel I deserve the physical and emotional pain, PTSD, and poverty that has been the result of his right to roam, and frankly, no one gives a crap.
Report comment
No you don’t deserve what you’ve been through. My condolences.
If he’s a violent criminal he should be locked up. Why is he roaming free?
Report comment
4waterwomen,
I empathize and sympathize and go as far to say that the victim and perpetrator need rebuilding.
And it comes from me having been primed, NOT by an MI person, not a schizophrenic, but a business man close to 50 years old towards me as a 14 year old, events which knocked on my consciousness when my daughter turned 14.
I then wanted to control the situation and sought out contact, and found a shrivelled up old man online and I called, looking for an apology. I spoke to him for a long time, he claimed not to remember me.
It upset me so, that I called a lawyer, I was determined to get my apology.
Instead it became a buy out, where I was offered $1.500. I was insulted. My lawyer wanted more. It kept increasing by small increments, when I stopped at $15,000, which my lawyer took $5,000 from.
I NEVER got the apology OR the healing, and ALL my life I knew I could NOT go to psychiatry with this, since I would become the bad guy.
I went my life believing I was a slut, NOT because of someone MI, but a respected father and functioning community and business man.
From this I know that for myself, I needed dialogue, holding and healing. I did NOT EVER need it for seeing him locked up.
My layer wanted it to go to court because he was sure we could win big. I was getting more and more traumatized, by the lawyer himself.
In fact I went to a counselor after this, who ended up crying on my behalf.
None of it was helpful TO ME.
Every one has their own unique feelings of how society can be improved. I know that punishment and compensation, in my case, would not guarantee me safety.
Perpetrators are all around us, shit happens and most of the perpetrators are not of a deviant sexual nature.
Because I want NOTHING to do with psychiatry that has no understanding of ME, the circumstances.
Everything to them is an illness and pathology, with no answer at all as to becoming a non victim, for the victim or the perpetrator.
In fact, all that would have happened for me would have been toxic meds.
I will never see psychiatry as the answer to keeping me safe, never.
Report comment
Violence against women and people in general is not tolerable, no matter what someone’s state of mind might be. This has nothing to do with psychiatric labels.
Report comment
Congrats on a well researched, well documented article, for those who still need everything spelled out.
Harris is a run-of-the-mill capitalist politician with a few “woke”-sounding flairs in her rhetoric, and is but another in a growing batch of so-called “progressive” prosecutors (which is pretty much a contradiction in terms). The key word is prosecutor — because despite the continuing sheep-like adherence of most people to the illusory language of “mental health,” the real interest of the system and its flunkies and front people is “law enforcement,” i.e. controlling those who resist the standards and values of the dominant culture using the trappings of medicine. And, lest this sound too abstract and theoretical, this means us.
I sincerely hope that by now the remaining holdouts understand that Democrats and Republicans are united in their support of ever-increasing psychiatric repression (and repression in general). This goes far deeper than superficial rivalries between politicians and parties, and will take far more than calling our Congress people to resolve (though that’s necessary too).
The system is not interested in how logical or reasoned our arguments are, only how to best stifle the growing percentage of the population which is dissatisfied with what it has to offer. It works to divide us and separate us on the basis of phony “issues,” and even designs the methods by which people are supposed to “resist” it.
So far discrediting and neutralizing people via psychiatrization still works like a charm, so why should they stop now? There are other methods too, of course, but as long as we allow each other to critique the construct of “mental illness” without rejecting the concept of “mental health” as well we leave the floodgates open for the totalitarian rantings of Harris, Trump, Obama, the Clintons, the Murphys, and the whole crowd.
To be “reformed” something must first have a demonstrable value — it just needs to be tweaked, or needs some corruption rooted out. Anything based on fraudulent principles from the start is by definition insusceptible to “reform,” and this includes the false branch of medicine called psychiatry.
Report comment
Oldhead.
Great comment as always. Rather I should say great conviction.
Report comment
No comments on the substance?
Report comment
Oldhead, I thought saying “great comment” was not enough, yet thought better than to try and expound on a post that spoke my sentiments, when my sentiments would say what you said, but in a convoluted way.
So I will copy and paste, the part that spoke the meat of my matter. (although I could copy and paste all of it) 🙂
” as long as we allow each other to critique the construct of “mental illness” without rejecting the concept of “mental health” as well we leave the floodgates open for the totalitarian rantings of Harris, Trump, Obama, the Clintons, the Murphys, and the whole crowd.
To be “reformed” something must first have a demonstrable value — it just needs to be tweaked, or needs some corruption rooted out. Anything based on fraudulent principles from the start is by definition insusceptible to “reform,” and this includes the false branch of medicine called psychiatry.”
Report comment
Thanks for the thumbs up; I was just wondering from your comment if you were reacting primarily to the content itself, or what you saw as the strength of my conviction. So I’m glad it struck you as being logical as well.
Report comment
thank you for this, Leah Harris. Seriously. 🙂
to me, remembering this former candidate’s mental health plan is important because…it shows what the elites want, really. not just the psych industry, not just the families, but those higher up, those who make big, big decisions for the 99+/- % of us in the USA, day in+day out.
so, apparently, draconian and ineffective measures– by ‘ineffective’ I mean policies that further damage the quality of life for ‘the least of these’ in these United States– have broad support in DC. E. Fuller Torrey and friends are helping frame the discussion, so common sense and the voices of those actually affected are effectively silenced.
I hope+pray the psych laws swing towards something more humane, less…oppressive and cruel. But then again, Szasz pointed out (in one of his many, many books on the subject…) that the psych guilds are pseudo-medical specialties that deal in lies, stigma, and–here’s the big one– social control.
my best -guess- is that this oppression, couched in self-serving jargon and mystification, is not limited to the psychiatrized or the disabled, and unless something is done about out of control inequality, pockets of deep poverty, wage stagnation, the decimation of the middle-middle class and the concentration of inordinate amounts of wealth into ever fewer hands…
more and more people will find themselves in some sort of under-class, kept under control by increasingly harsh, even violent, methods. again, my best -guess- is that the psych guilds will be there, drugs and lies and labels and all, to ‘help’ the under-classes, no matter the official category (felons, probationers, welfare recipients, drug users, etc.). power is power, after all.
the current epidemic of psychiatry seems to be the most frightening one, yet. 🙁
Report comment
Yeah_I_survived,
Psychiatry can’t be coaxed into more “humane treatment”. They don’t care even about evidence.
Psychiatry itself is treatment resistant. Open dialogue is not possible.
To try and reason with psychiatry is a waste of energy, and is what they see as “oppositional” to their truth.
And of course we can see how more and more fit the DSM, really a no brainer that psychiatry is falling into the slop pail they themselves created. Their descendants will also reap the legacy.
We might just have to watch the imploding of a dynasty, and although on the surface it appears they are ruling, their system is just so simplistic and the more ‘scientific’ they become, the more ‘disease model’, the further they get from making any logical sense. Logic is never the mere appearance of a desperate attempt at solution.
Report comment
Tie a pretty pink ribbon on torture and call it compassion.
A friend of mine left NAMI and urged me to leave “mental health” when her sister died at 49 and she saw my rapid decline. My heart is finally beating regularly again.
My family agrees the drugs did not help me. Many people are upset at the cruel, pointless experiments performed on their loved ones. Families that actually love each other. Even the sensitive types having a rough time.
How anyone could knowingly force a child to take drugs they know are crippling and slowly killing them is beyond me. At least my parents believed the chemical imbalance lie and were sincere though misguided. (By evil guides.) You can’t make such a defense in Pete Earley’s behalf. On his blog he unapologetically acknowledges this is false but claims it’s necessary to promote it to ensure “meds compliance.”
Google “Pete Earley chemical imbalance metaphor.” His blog will likely turn up with the article I’m thinking of.
Neither truth nor love.
Report comment
Where does the Trump go
Not everybody know
And if the kids are allright
Time for an intervention is lost
Report comment
I can prove I recovered as a result of stopping my depot injection medication in 1984.
Reference 1
https://drive.google.com/file/d/1PW-wn9GOkiyWAbdzgXuC8cDS-7UPEj0-/view?usp=drivesdk
(But the reference above suggests, I’ve always been okay).
The Drugs in my opinion, cause the illness and what I had to get was a ‘Power of the Now’ or “Mooji” perspective:
https://youtu.be/vdKs13kf13A
…and this worked.
Report comment
Thanks Leah for a great report.
That last copy/paste tweet says it all…. “Bad mental health policy is, regrettably, a bipartisan enterprise”.
Reminds me of an illustration I recently saw of cattle being herded into two chutes, one marked for the “Left” and one for the “Right”. But then all the cattle from both chutes were herded into the same doorway marked “Slaughterhouse”.
Report comment
(Not to distract) The Mental Health System reminds me of the Industrial Farming System:- Its very cruel, it’s ‘invisable’, and every bit of value belonging to the ‘animal’ is exploited.
[I was in a Famous NHS London Eye Hospital a few years ago after being sent there by my Optician to double check me for Glaucoma risk.
I was examined by a youngish doctor, and I mentioned to them that I had historically consumed psychotropics and that they had affected my eyes. The doctor told me that this was not the case, even though Patient Information Leaflets to most Psychotropic drugs warn of Eye Damage.
The doctor kept what I had expressed regarding my own experience off my records, and entered into my notes a Severe Mental Illness Diagnosis].
Report comment
Fiachra, wow, I did not know that psych drugs can cause eye damage too!
As if not disgusting enough that psychiatry puts spurious, unfounded labels on people but they also leave out any truth or facts and resort to writing lies. The shrink I saw during cancer treatment did not make one note about what I explained to her was going on with treatments and side effects etc.
Report comment
The best promise from a politician is that they can persuade people to be kind and decent to their little children, to nurture them and treasure their feelings, create solid connections with them, so they will not need psychiatry or social control.
Report comment
dfk
And if the parents can’t, or fail or can’t make a living, the kids are still better off than a second system abusing them. People don’t rescue kids, they hurt them more. Rescuing is helping mom and dad in a hands on way.
Report comment
“Woke” politics is VERY AUTHORITARIAN. You know, the PC police…
Why is that so hard to understand? I am waaaaaaaaay left of what is considered ‘left’ these days. The Democratic PartyTM does not represent me–they represent the 10% managerial class and their billionaire corporate donors. And they mos def has ‘authoritarian’ issues, along with all the ‘alternative’ communities I’ve lived in. Never so oppressed as when I lived in Humboldt County CA.
Left, right…the propaganda is so thick now.
Steve gets it.
Report comment
“Szazian” is just another way to discredit both Szaz and anyone else who dares to question the fact-free psychiatric dogma on which the entire system rests its ugly head.
Report comment
“Szazian” is just another way to discredit both Szaz and anyone else who dares to question the fact-free psychiatric dogma on which the entire system rests its ugly head.
Which is why we all must STAND FIRM and EMBRACE the term “Szaszian” when someone attempts to use it this way. No backing off or slinking away from the term like they just called you a Scientologist. We must never let the enemy define us, make us defensive, or cause us to repudiate something so essential to our analysis and our struggle.
Report comment
Well said.
Report comment
“As societies get larger and more complex and start heading toward collapse, the ability to connect dots gets harder. It’s colony collapse like we see now in bees.”
Yes anomie, psychiatry is making a living off the complexities. I think we will be much more concerned about where to make a living, and get food than about mental health.
The shortage of jobs and minimum wage jobs is contributing to stress… and to think along the lines that our kids should all be “mentally healthy” so they can all go out to get jobs like becoming a psychiatrist, you know, becoming that “contributing member of society”, well that idea is so unrealistic that it defies any logic.
Psychiatry cannot keep up with the complexities and even though the concept of “MI” is continuing, I think politicians one day will admit publicly that we are in fact in danger and that it is not conspiracy thinking. And that might be the turning point for all things we used to try and feed or control a society with.
There are a lot of powers beyond ANYONE’S control.
Medicine and psychiatry are not helpful. Messing with nature has proven to be the wrong move. Exploring is a fascination within us, we keep it alive by obsessions.
We should in theory be further ahead, yet we get further from the target.
Psychiatry keeps looking in all the wrong places, but I cannot believe that they are really blinded that much.
It must simply be the narrow views and cushy lifestyle, the JOB that keeps it alive, since none of their theories make any sense at all.
Report comment
As a Scientologist, I have to deal regularly with the general ignorance in society about the subject I am studying, as well as the occasional barb flung by those who believe the falsehoods advanced by those who wish this subject would just disappear. Those falsehoods have for the most part been advanced by institutional psychiatry and its supporters. Are we suddenly willing to trust their data on this subject when they have gotten everything else so seriously wrong? Scientology should be part of this discussion, but it can’t properly be as long as so many of us don’t know what it really is.
Report comment
As an orthodox Christian who attends a Church of Christ assembly based on the Bible and fundamentalist notions, I struggled with the incompatibility of my religious faith and psychiatry.
Yes, brain illnesses exist. Meningitis, epilepsy, dementia, brain cancer, ALS, traumatic brain damage. These cause cognitive problems–along with other issues like motor impairment.
But what psychiatrists–especially the high ranking kind–love to warn the public against are not people with cognitive problems. (Torrey doesn’t go on national TV to warn the populace about how dangerous all people with Down Syndrome are. Notice that?)
Basically “mental illness” refers to moral issues. If a young man goes berzerk with a gun or knife or homemade bomb he isn’t cognitively impaired. Often these murderers show great ingenuity in gaining or constructing these weapons.
The problem is moral–not cognitive in nature. The idea that any pill can cure moral problems by strengthening the conscience and rekindling love for your neighbor is ludicrous.
My religion promises help in overcoming moral problems (AKA sins) through traditional means laid out in our scriptures. But when well meaning church members urged me to get “help” and take my “meds” I wondered what good our church was. Did “mentally ill’ people like me not have souls since the Atonement was insufficient for our redemption?
No one else pondered these questions. Then I discovered most shrinks–especially the high ranking members of the APA–don’t believe in souls. They are actually monists or materialists.
My dad is a retired preacher with a graduate degree in theology. I read him Dr. Pies’s article arguing both against the chemical imbalance “metaphor” and in for hard core materialism. This turned my dad against psychiatry–realizing it was actually a rival religion sneaking into churches by posing as a branch of medicine.
Report comment
I have never heard of a shrink calling the “chemical imbalance” trope a metaphor, as opposed to a very concrete pathology.
You are also correct that psychiatry’s contradictions come to the forefront when questions of the “soul,” and consciousness independent of corporeal existence, come into play. Obviously one’s view of how life is to be reasonably conducted will be different depending on whether one is looking forward to some new form of conscious existence, or to total annihilation. So the potential “therapist’s” view on such spiritual or metaphysical matters should be known from the start.
Report comment
Dr. Ronald Pies did in a couple articles published in the APA journal.
He was very indignant that anyone thought members of his profession were ignorant enough to believe the lies they told those who trusted them. 😀
Report comment
OK wait I do remember that. But he’s pretty “fringe.”
I’m more interested in your reaction to the 2nd part of my post, which I consider more significant, as this issue is rarely mentioned in MIA discussions.
Report comment
Rachel
How do you reconcile the very close similarities (and harmfulness) of the doctrine of “original sin,” and the genetic theories of “mental illness” promoted by psychiatry and the Medical Model?
Richard
Report comment
That’s a good question Richard.
A major difference between “original sin” and “mental illness” is the playing field is level. We’re ALL sinners. And genetic defects–though they exist–don’t make anyone inherently better than another.
Whereas psychiatrists believe the majority are born sane. Such as themselves.
Furthermore the doctrine of “original sin” goes along with the doctrine that all human beings are special beings who bear the divine breath within. And have basic rights to life and liberty by nature of our common humanity. Regardless of intelligence, strength or beauty.
Report comment
Rachel
Thanks for the response.
I would say that the concept of “original sin” imposed on society by various religions. has actually done FAR MORE harm to people in the world (up to this point in history) than the harm done by psychiatry and their genetic theories. Although psychiatry is doing its best to catch up.
When you look at how children, in particular, respond to trauma experiences by deeply internalizing toxic guilt and shame, you can see the tragic results of this religious doctrine. People (especially children) feel completely abandoned by the adults they are taught to respect and obey, and who are suppose to protect them in the world.
They also end up not feeling worthy enough to be protected by their “God” and negatively judged, as a “sinner,” by their “God,” and ultimately “punished” by this same god. These kind of very harmful beliefs are often repeated by many trauma victims in multiple ways, and carried into adulthood.
Rachel, you said:
“the doctrine of “original sin” goes along with the doctrine that all human beings are special beings who bear the divine breath within. And have basic rights to life and liberty by nature of our common humanity. Regardless of intelligence, strength or beauty.”
This comment ignores the fact that the Bible is filled with quotes that promote harmful patriarchy against both women and children, including stoning and death as a punishment for various types of so-called disobedience and disrespect. And one of the 10 Commandments actually upholds slavery. Overall, there is very little “rights to life and liberty” depicted in the morale standards of the Bible.
I believe there is no such thing as “sin,” which implies some type of eternal “good AND “Evil” in ALL human beings and in the world.
There is, however, “right and wrong” in the world as determined by an evolving code of human morality that has fortunately evolved far beyond (in some places on the planet) than the more primitive standards laid out in the Bible.
I have to say that the uncritical and blind interpretations of biblical scripture and religious doctrine that some engage in reminds me very much of the uncritical and blind interpretations of the DSM Bible and the entire Medical Model.
Rachel, I love almost all your comments and your overall presence at MIA, but I just can’t let these contradictions in thinking slide by without responding in a direct and honest way.
Respectfully, Richard
Report comment
“original sin” might make the playing field level to the degree that we ALL buy the notion that we are ALL imperfect.
But that is ONLY IF we adhere to same thinking, which we do not. The sinner was always the other guy, or the other church or race.
Psychiatry tells us we are “sinners”, just in different terminology, and they are never the sinners themselves.
Churches today are not as outspoken about their prejudices, since they no longer hold power to chastise the “sinner”.
But in the past they held a lot of power, or should I say that they came about through want of power.
Power and ideology, or ideology and power. Not sure which came first.
Obviously within any animal society we do need power to keep some control, but this does not seem to come without great damage and on some level ALWAYS involves enslaving.
The nutty thing is, we cannot rely on our own thoughts to be the truth? and is a subject for philosophy. I think the bottom line is, whatever thoughts we hold, if those thoughts result in action that harms others within society, for being “different”, even if only causing derision, such as being an outcast, felt in one form or another, then the power was not used properly.
To feel outcasted sometimes simply seems to come from within ourselves, example , if I within my church start doubting the theories. Yet is it only from myself?
Often when we have beliefs and theories we do, even if silently, hold them against people or groups.
But it is the harm it can cause, on a psychosocial level. And combine the beliefs with real application and chaos/pain results, but never felt by the ones who applied it.
Often Psychiatry points to “lack of empathy”, in certain MI.
We all lack empathy when it comes to certain people or groups.
Psychiatry is very guilty of absence of empathy as is evident in their very judgemental positions, positions that result in “othering” and to the degree that “othering” affects people.
Report comment
Thank you for your directness and honesty Richard.
I’m not sure which of the 10 Commandments you refer to supports slavery. The one against coveting perhaps?
BTW, you have your own reasons for rejecting organized religion. This is not an apologetics site so I will not debate you.
Since you don’t believe in it, the cognitive dissonance you experienced with psychiatry is purely biological and moral. Not theological like my own.
Blind and uncritical thinking bring trouble wherever they occur. I agree.
As someone with nothing to gain by helping us survivors I applaud you in supporting our movement.
Report comment
Yes, Anomie. Survival of the Fittest as the standard can be brutal to those judged unfit. Weakness is viewed as the ultimate crime–worse than robbery or murder.
Report comment
Psychiatry has its own version of original sin, which is the inculcation of the belief among the masses that their misery and dissatisfaction result from neurological and/or psychic defects, rather than “natural” human reactions to oppressive circumstances.
This is “original” in the sense that these oppressive circumstances preceded all of our births, hence our reactions seem to be ingrained or natal traits. But it is a man-made quagmire.
Report comment
I urge you to take a closer look. Mr. Hubbard has recognized this problem since 1950. We came into this movement very early in its development, helping to defeat the “Siberia Bill” in 1956. We now have content on TV and the internet, so you can learn more about the subject in the safety of your own home. It’s great to be “left alone,” but that’s not the world we live in today. In a world full of connections, communications, and interdependency, we need criminality out of the picture. And we are dedicated to working towards that end.
Report comment
What’s the “Siberia Bill?” I’ve never heard of that one!
Report comment
“Siberia Bill” – officially, the Alaska Mental Health Enabling Act. It was intended to set up an independently-run mental health system in the territory of Alaska. Per the Wikipedia article on it, the bill was “innocuous” but used by several groups as an example of creeping loss of freedoms in the U.S. The bill would have established a Trust to finance the Alaskan facilities, funded by potential revenues generated by a million acres of Alaskan land. Provisions were included for treating citizens of the lower 48 states on a reciprocal basis. It doesn’t sound that innocuous to me, particularly considering what has rolled out since that time.
Report comment
I read up a bit on it, too. It sounded like the big objection was that people from the Lower 48 were going to be shipped to Alaska for “treatment.” Seemed like the article was a whitewash. Definitely see some very real concerns about THAT idea!
Report comment
l_e_cox_
“As a Scientologist, I have to deal regularly with the general ignorance in society about the subject I am studying”
There always seems to be a problem with identifying with groups. A group rarely has all our opinions/views neatly “grouped”. Evidence is, parting of churches, political parties, critical psychiatry, the playground……If your group is anti-psychiatry and recognizes the harms thereof and has some basic solutions for kids without them having to belong to a certain group ideology or identify with a term, seems sufficient. We have to be more concerned with education about falsities and control, giving alternatives to low income people, instead of covering up the issues. To do that, we don’t need to do that in the name of anything.
I mean in the end, we could name a group “insightful” “the church of the insightful”. Perhaps we need a group called “action”, as opposed to “theories”. Psychiatry and oppression are the “action” group at the moment. It’s not working and not because there needs to be more of this theory in action.
I belong to a church called “these ideas and implementations are harmful and not working, let’s try something else that has some common sense”
We are all in an experimental stage and we got a lousy hundred years max to practice. So far it’s looking pathetic. Thank god it’s less than hundred years allotment.
Of course some groups are working towards living longer, which is a scary thought.
Report comment
“I belong to a church called “these ideas and implementations are harmful and not working, let’s try something else that has some common sense””
I want to be a member of YOUR church!
Report comment
🙂 yeehaw Steve.
I am not breaking away from my MIA church though.. 🙂
Report comment
Does that mean I’m in?
Maybe we can shorten it to “The Church of Sanity and Common Sense.” CSCS is a workable acronym. Anyone else want to join?
Report comment
Steve, on second thought my church sounds a lot like MIA principles. So why ruin a good thing.
I really can’t come up with ideas to improve. Our jobs are to recruit. Maybe I’ll start knocking on doors or leave pamphlets. 🙂
Report comment
https://www.youtube.com/watch?v=cgwvSTzWF6w
The Church of What’s Happening Now is the one true faith.
Report comment
I love me some Flip Wilson!
Do I got an AAAA-MEN!
Report comment
Steve,
When I returned to Boston in 1969 after a diesel submarine tour of Asia, including the war zone, Flip Wilson and Bobby Darin were both very popular. Bobby Darin has just released his “Simple Song of Freedom” which was covered by local bands. Bobby Darin was a musical genius and a good-hearted libertine, not a libertarian, and there is an important difference.
Just saw this clip of him and Flip together. Fantastic! Unfortunately, most people bring up the image of a child predator who played the part of Bobby Darin in a major motion picture. This is the way we need to remember him.
https://www.youtube.com/watch?v=ORH3y3DtYqY
https://www.youtube.com/watch?v=UZ1ohsissjE
Good Luck (you’re going to need it) and Good Hunting to freedom fighters everywhere!
Subvet416 out
Report comment
Anomie, Rachel.
I understand now. Sometimes I am a step behind
Report comment
I generally have difficulty with language that is descriptive.
The language is invented by man, and he designs around the words what it means. (or visa versa)
“moral”, “ethical”, “intelligence”, “god”, “mentally healthy”, “truth” ….
And I really dislike words and their meanings imposed on me, words that mean different things to people, words that are open to interpretation.
It is difficult for everyone to be on the same page at the same time. A 60 year old really cannot hold the same standards for a 16 year old, as they do for themselves.
A lot of judging occurs within humanity, of ourselves and others, it is totally natural, but becomes a huge issue when it hurts.
Our judgments are our “truths” applied to others. And sometimes not even to ourselves.
“crime” and the judging that happens after the fact, was preceded by judging long before the crime happened. It happened perhaps within childhood, within their community, and finally within themselves and is why I have a kind of empathy for the criminal, especially if they are young.
Two young men go on a “killing spree” and it results in 5 deaths, including their own. The media garners info and describes them as “loners”, “gamers”. There were many times in those young lives that intervention could have helped. But no one did. No doubt in my mind that the young men internalized anger and projected it. This is not a “moral” issue IMO. It is not a “mental illness” issue. It is an environment issue. And that sits on the shoulders of all of society.
The answer does not lie in trying to identify “criminals” in grade 3. It lies in seeing a kid in need to supply him with inclusion and to tailor his life in a way where inclusion is natural and not simply tolerance.
I really believe that we need our school systems changed, since we cannot go into each individual home to change environments.
Everyone needs stability and we cannot get there by pills or counselling, which are the result of labelling. In all of society, labels have done more harm than good.
No one tells the public that even if parents are honest within themselves and go for “help” for lack of parenting skills, that the parent actually gets no help, but is seen as “ill”. This happens ALL the time. It is a sign of how sick the system (society) is.
It wants to deal with problems within a “moral” compass, their own interpretation of that word, and apply their own solutions, which of course are never “solutions”.
The real effective solutions simply take more time, involvement and effort, and an insight to not just the person involved, but history and present society. They claim the costs are too high to implement systems for a healthier society. That is a lot of BS. A different system, different schools, after school programs ran by people who love kids, and love and include all kids would in the long run employ just as many people. In fact kids could be identified NOT as “MI”, but as having a need to be more included and can easily be dealt with by knocking on doors of those kids that like to hole up and taking them by the hand to an after school program. The only jobs a new system threatens are psychiatric ones.
My son does this now in their tiny special school. He literally drives to pick kids up either at their homes or the group homes. The government allows only a tiny budget for this school, and inclusion is narrow. It is again political, making it seem as if the system is doing good, but they make sure it is small, and not highly available and the pay to employees is low, making it not so attractive.
The aftermath of the present and past systems is the actual wheel that causes the failures and costs. We refuse to change anything, because the failures are a business.
The concept of “MI” keeps this failing system even more entrenched. No one can argue logically for more “MI”, without radically changing the way we have done things. But every new change is on a small scale, purposefully aiming for it to fail, by governments not investing in the changes.
People such as Harris have this judgemental “moralistic” attitude that blames the victims, not society. In crime, the victim and criminal are both victims.
People are easily convinced to believe in the “MI” model when they don’t have the capacity, experiences, or years lived. And we simply cannot have systems created where there is lack of insight as to the existing problems. “MI” is a diversion, not a fix.
Report comment
Anyway, fuck this shit. The cycle repeats: more “Black faces in high places” to trick a gullible populace into believing the system is addressing racism — or psychiatric oppression, as the case may be.
There is no “lesser” evil.
Report comment
The world has exploded in the last year, and I am loving it. Let’s celebrate the end of an era and possible an age *blows horn*
Report comment
It is worrying that a high-profile American politician exhorts non consensual treatment and blatant human rights abuses. Shouldn’t such eugenics be fought against with the upmost rigour? What did my father fight against in the second world war? Actually it was just that!
Report comment