The neuroleptic tranquilizers commonly referred to as “antipsychotics” are often used as a first-line treatment for those deemed “at risk for psychosis,” as treatment providers attempt to stave off the worsening of psychotic symptoms associated with schizophrenia. However, there is little evidence that this approach is effective, and the drugs are associated with many harmful effects.
In a new study, published in the Australian & New Zealand Journal of Psychiatry, researchers wanted to investigate whether antipsychotics might prevent “conversion to psychosis” in people who were identified as being at “clinical high risk (CHR) of psychosis.”
The researchers found that antipsychotics were consistently associated with worse outcomes—higher rates of “conversion to psychosis” were found in those who took the drugs, those who had multiple prescriptions, and those who took a higher dose of the drugs.
“Administration of antipsychotics to CHR patients is potentially harmful with no preventive benefits. We do not recommend antipsychotic treatment for CHR individuals, which is practiced widely in China, and strongly advise caution if these drugs are used.”
TianHong Zhang led the research at the Shanghai Jiaotong University School of Medicine, China.
 The Study
The Study
The research was a part of the SHARP (ShangHai At Risk for Psychosis) trial. Five hundred seventeen participants between the ages of 13 and 45 were identified as “CHR” based on a clinician-administered measure, the Structured Interview for Prodromal Syndromes (SIPS). Four hundred fifty of the participants completed a 2- or 3-year follow-up.
None of the participants had ever received a previous psychiatric medication or previous psychotherapy.
This was not a randomized, controlled trial, but rather a real-life trial—designed to see how people fared in actual practice, rather than in a controlled lab setting.
The researchers argue that clinicians often discount the results of RCTs with the excuse that real-world situations are more complex, and clinical judgment cannot be tied to controlled trials. Therefore, this real-world assessment was designed to showcase actual results for clinicians to take into their practice.
The participants were prescribed antipsychotics based on their personal clinician’s judgment. However, the researchers were able to stratify their results by several measures, including by severity of symptoms. This means that they could compare those with mild CHR who did and did not take antipsychotics, those with severe CHR who did and did not take antipsychotics, and those on different doses and more prescriptions of antipsychotics.
Results
For those with mild CHR, antipsychotic treatment was associated with worse outcomes—higher rates of “conversion to psychosis.”
For those with more severe CHR, antipsychotic treatment still resulted in no improvement. Instead, the rates of “conversion to psychosis” were the same on average whether someone took an antipsychotic or not.
Among those that did take antipsychotics, those on a single drug and those taking a lower dose were less likely to “convert to psychosis” than those prescribed multiple drugs and higher doses.
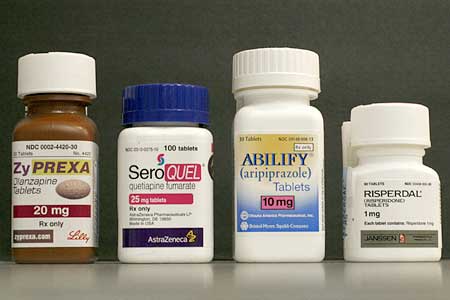
Many different antipsychotics were used, including aripiprazole, olanzapine, risperidone, amisulpride, and quetiapine. The researchers write that their “results did not favor any specific type of antipsychotics.”
In summary, the researchers write,
“When the baseline severity of symptoms was considered, no significant difference was detected in the severe CHR group in terms of conversion rate, but even worse, those in the mild CHR group who been treated with antipsychotics were at an increased risk for psychosis.”
Of note, none of the participants were provided with psychotherapy—so this was a comparison of people given antipsychotics to people receiving no treatment.
The researchers write that people receiving no treatment may do better due to living normal lives without the stigma of medicalized distress and the adverse effects of neuroleptic tranquilizers:
“It is noteworthy that those patients not treated with antipsychotics may have functionally benefited from less stigmatized stress, adverse effect, and living in a more ‘normal’ and relaxed environment.”
Previous research has found that about 73% of those with the CHR label never go on to develop full “psychosis.” Other research has found that just being given the CHR label leads to stigmatizing effects. Researchers have also critiqued the whole paradigm of using the CHR label.
Even in full-fledged first-episode psychosis, researchers have found that CBT without antipsychotics is just as effective—adding the drugs provided no additional improvement.
The evidence against the use of antipsychotics for early psychosis and at-risk states is clear. Guidelines recommend against their use in these situations, and a substantial body of studies found no improvement—or even worse outcomes—for those taking antipsychotics.
However, according to the authors of the current study, doctors tend to ignore this evidence.
“Although RCTs and guidelines have recommended against the use of antipsychotics for CHR individuals, clinicians often do not follow the guidelines. The complexity of daily clinical practice has often been used as an excuse for clinicians to offer easy therapy instead of optimal therapy.”
****
Zhang, T., Xu, L., Tang, X., Wei, Y., Hu, Q., Hu, Y., . . . & Wang, J. (2020). Real-world effectiveness of antipsychotic treatment in psychosis prevention in a 3-year cohort of 517 individuals at clinical high risk from the SHARP (ShangHai At Risk for Psychosis). Australian & New Zealand Journal of Psychiatry, 54(7), 696-706. https://doi.org/10.1177/0004867420917449 (Link)















The embarrassing thing about this is that you probably could lower the rate of “CHR” individuals losing their marbles by pretreating them with a basic 3g/day of B3 and C instead of antipsychotic drugs.
But then manufacturers wouldn’t make any money, the most important element of present-day psychiatric treatment.
Report comment
Thanks Peter.
IF we were dealing with something scientific or medical, perhaps then one could try and develop something, according to the need, IF the client felt a need to ingest that which was developed.
However, a simple observation into human behaviour is not scientific. There is no physical test to determine WHAT is happening. Nor the WHY. So how could one possibly develop a drug that “addresses” “IT”. That unwelcome phenomena.
It is simple if we develop a spect scan and we decide to call that lack of red “mental illness”, and from then on, each person with the “lack of red”, has “mental illness”? It is a no fail test then, because you are inventing what the color red means, yet here we are, it does not apply even half the time.
Nor are there blood tests. The only thing we have is an observer who is prejudiced against what he sees.
Misinterpreting what we see happens all the time. What we see is not at all that person’s state. It is your own state, full of bias and prejudice. And so, we have absolutely no right to “diagnose” or prescribe poisons to states and ways of being which we are simply not privy to.
Report comment
And I also have an issue with “early psychosis” as a guideline for “treatment”. Perhaps I can have one migraine or years of migraines. Perhaps they will worsen or get better without treatment. Perhaps I don’t want “medication” for my migraines.
Report comment
If you go down the road of pharma treatment for migraine, can almost promise you will get worse, much worse. I know more about those drugs than psych drugs. Plus the root causes of migraine and solution is known and can bring it well under control to being just a minor issue. But after the drugs, which many will have used for years, it’s a real battle to get it under control.
As for AP’s – vile killer stuff.
Report comment
“… higher rates of ‘conversion to psychosis’ were found in those that took the” antipsychotics. That is because the antipsychotics create “psychosis,” via anticholinergic toxidrome.
The antidepressants can also create “psychosis,” any of the anticholinergic drugs can make a person “psychotic.”
If we could just get the doctors to stop prescribing the anticholinergic drug classes, especially in combination, we could greatly reduce the incidence of “psychosis.”
Report comment
This is so utterly blatant and predictable. And I don’t believe it is a choice of “easy” vs. “effective” in most cases. It is a choice of “making money” vs. “makinig a lot less or no money,” at least in the USA. Providing “no treatment” not only makes doctors feel less valuable, it means they can’t bill for their continuing “services” to their drug-dependent patients. Hence, WORSE outcomes mean MORE MONEY for the doctors, so the science has no impact, because improved outcomes (consciously or unconsciously) don’t appear to be the goal of many if not most psychiatric practitioners. Otherwise, they’d be excited to learn about this kind of thing instead of pretending it doesn’t exist.
Report comment
It’s a choice of accepting that you hurt and killed a lot of people or denying it to save moral, social and financial face. It’s not just that they are making money. They get their social status and power from the status quo. Admitting their lies harm/kill people means all fantasies that they are good decent people go away. The quote “It is difficult to get a man to understand something when his salary depends on his not understanding it.” Misses a bigger point. If your profession has been hurting and killing people all along your morals depend on you not understanding it.
Report comment
Well said, willow.
Report comment
Yes, psychiatry’s “invalid” disorders, and their neurotoxic drugs, are killing “8 million” innocent people EVERY year.
https://www.nimh.nih.gov/about/directors/thomas-insel/blog/2015/mortality-and-mental-disorders.shtml
That would be about 400,000,000 people murdered by psychiatry in the past 50 years. We are living through the biggest psychiatric holocaust the world has ever seen. Yet oddly, this relevant information doesn’t even make the “news.”
Report comment
You might benefit reading my post-and the smart replies. Or maybe not.
Report comment
As a known practitioner of Crtimethink, I’m obliged to agree with you here, Steve.
Report comment
Neuroleptics AKA “Antipsychotics” (according to my verifiable experience) CAUSE the Symptoms associated with “those at Risk of Psychosis”, they do not alleviate them.
I felt okay not taking “antipsychotics” to begin with. But when I attempted to come off them some years later (abruptly, with permission), I had 4 hospitalizations in 5 months a suicide attempt and an almost suicide.
It took me 6 years to carefully withdraw from a dosage suitable for “schizophrenia”. But I wouldn’t have made it, if I had not come to the realization that I was suffering from the “High Anxiety” of “antipsychotic drug withdrawal”.
I had never previously experienced anything like this Anxiety. My exposure to these drugs could have driven me MAD.
To cope with the High Anxiety of Neuroleptic drug Withdrawal, I had to learn to sit with “acutely uncomfortable feelings”, and to “stay out of my head” at the same time. When I “balanced off” my thinking would return to a “hypothetical level”, which was always safe for me.
I Recovered as a result of stopping Neuroleptic / Psychotogenic Drugs.
Report comment
Glad to hear it Fiachra.
Report comment
Thank you Sam.
Report comment
Difference between a therapist -and a physician? Physician is responsible for having to make the decision. A therapist on the other had-observes and comments on it. If therapists were legally liable for this misinformation-they might be more circumspect.If you cant spread truth, dont spread make believe. These are risk/benefit decisions. Ask all the people who take them -and hate them bo the multitude of terrible side effects-wt gain, metabolic syndrome, TD.Ask them why they still prefer to be on them???Many people can get off them, should get off the, should never have been placed on them as a result of garbage psychiatry. hype (I am a psychiatrist). That said-this stuff-is ridiculous at best and destructive at worse. So do no harm does not apply to “therapists”? Do you want to be medically responsible for this opinion? If one person reads this-stops their medication-and god forbid has a terrible outcome-take a look in the mirror.The last person who argued with me after their misguided incomprehensible point-stooped to saying “what do you know-you spelled Thelonious Monks name wrong”. Ha-I guess they could not get the joke…If you are out there-read his biography.
Report comment
theloniusmonk,
I came off my Modecate Depot Injection (with permission), because of its disabling side effects in late 1983, and ended up in hospital fairly quickly afterwards. I was put back on an increased dosage of Modecate while in hospital – and I experienced an Akathisia induced suicide attempt in early 1984.
I then tried to come off the Modecate Injection again, but I couldn’t, so I asked my doctors for a medication with less side effects. Another medication Depixol Depot Injection was recommended – but after taking the Depixol injection I became suicidal (with Akathisia) and I had to fight my way back into hospital (where I stayed for less than 2 days).
I then asked doctors to prescribe me an Oral “medication” which they did, but I found I also suffered from “Drug Withdrawal High Anxiety”. This “High Anxiety” could have driven me MAD, had I not learnt how to deal with it.
I was able to function with the Oral medication and as my ability to deal with my “High Anxiety” improved, I was able to cut the Oral Medication down very gradually, to eventually nothing.
Doctor David Healy was around during my “Drug Withdrawal” at Galway Ireland Regional Hospital 1983/1984, and I visited him with my notes, in Wales in 2018. Dr Healy provided me with a letter stating that he was confident that I had never suffered from Severe Mental Illness to begin with, and that it was likely that the treatment had been the problem.
But, if I hadn’t learnt how to overcome my ” Drug Induced High Anxiety” through Psychological Means, I’m sure I wouldn’t have been in a position to challenge any “Diagnosis” – I would more than likely have been DEAD.
https://www.bps.org.uk/what-psychology/understanding-psychosis-and-schizophrenia
“…Understanding Psychosis and Schizophrenia. The problems we think of as ‘psychosis’ – hearing voices, believing things that others find strange, or appearing out of touch with reality – can be understood in the same way as other psychological problems such as anxiety or shyness…”
Report comment
TY for a great reply
Report comment
I suppose if you told them that their suffering was an “illness” and that they needed the drugs made specifically for that “illness”, then people might risk taking them. Many people take chemo even though the physician is pretty sure it won’t save the clients life. But he has a “legal” responsibility. Not a moral one.
Report comment
excellent point.
Report comment
Lots of people have no choice Dr. Monk. Do you really think there are no social or legal repercussions to such a decision? It’s almost never an informed one.
After a break down following 3 weeks of sleeplessness from a bad reaction to the drug Anafranil my shrink cheerfully told Mom it wasn’t HIS fault her daughter had schizophrenia. Joyfully ruined my life causing everyone to write me off as a psycho killer.
Put me on 10 mg of Haldol. Hell between my ears. Seizures, constant dry mouth, tardive psychosis, eyes rolling back. All attributed to my illness.
Psychiatrists go around telling how those they diagnose are all would-be mass shooters. Through guilt by diagnosis/association they claim we’re morally defective in some intrinsic way no other human beings are. Only drugs can save us from becoming violent, suicide, cheating on our spouses, lying, stealing. All “symptoms” in various DSM categories known as “mental illnesses.” Whether we actually DO any of the above is irrelevant. The doctor has pronounced us morally diseased so we’re automatically worse than felons.
(I don’t know you personally Dr. Theolonius. But prominent members of your profession have gone on national television to warn society of the monsters posing as humans in their midst. Also known as “schizophrenics” and “bipolars.” You aren’t directly responsible for what Dr. Fuller Torrey says. But you must be aware of it.)
I was repeatedly told for 25 years that I had a brain disease with a known biomarker. That it had already been proven my “illness” came from a chemical imbalance in my broken brain. Not for two decades did I read William Glasser and then articles by the President of the APA declaring otherwise.
Had to relocate and start over where no one knows me while slowly tapering. No help from any doctor. I knew better than to ask for any.
For years I took the XXXX pills though they doubled my weight, made me seize, vomit, lose teeth, grow so tired I couldn’t keep up with simple ADLs like bathing regularly. They made me miserable and numb. Yet I took them conscientiously. Not for myself but for my loved ones. I didn’t want to hurt them or be a burden.
Because of my wrecked body…real doctors who don’t know all my psychiatric history have diagnosed me with IBD and other autoimmune diseases…I still can’t work. All iatrogenic I firmly believe. More of a burden then ever from trying to do the right thing as a “conscientious consumer with excellent insight.”
Obeying the rules doesn’t work in a corrupt system.
I wish I’d broken an actual law instead of seeing a shrink. That would have had fewer legal repercussions. Seriously. Criminals have more rights in our society than law abiding citizens labeled as “severely mentally ill.” Once you get that label how you behave–the content of your character–is completely irrelevant. Everyone expects the worst of you. Especially if they know you’re “off your meds”
Been off mine for nearly 3 years. Doing better in many ways. No melt down despite lockdown stress. My parents acknowledge I wasn’t crazy after all. I’m an embarrassment to the psychiatric profession. And doctors in general who remain thick as thieves and will carry the banner for men like Farid Fata.
Not anti-medicine but I don’t trust doctors. Buy the used car but don’t believe a word the salesman says.
Report comment
sometimes-either do I. Sometimes. Like police, politicians etc or anyone granted a perceived power over one in a less powerful position-there are good and less good and bad. IMOSeems the question is-are the medications bad-or those who dispense them. That seems to be sometimes missed. thank you for the thoughtful reply.
Report comment
You’re welcome.
I wish you well.
Report comment
theloniusmonk,
LACK OF RESPONSIBILITY OR AKATHISIA
https://www.irishtimes.com/news/damages-for-man-whose-wife-drove-off-galway-pier-1.1131888
“…Mr Nugent said Mrs Palmer was admitted to a psychiatric unit at the hospital under the care of Prof Fahy. She was kept there for a week. To the consternation of her husband, her own family and her friends who contacted the hospital, she was released. ..”
https://www.irishtimes.com/news/last-minutes-of-a-woman-tormented-1.1131911
“…”This is hell”, nine times over. “A disgusting waste of two beautiful girls – two human beings” on the reverse. These were among the last words written by Mrs Catherine Palmer, jotted on a note found in her trouser pocket by Garda Michael Harte after her death…”
POLICY OF SUPPRESSION OF AKATHISIA
https://drive.google.com/file/d/18EilU4iOzu3MlTHsq6HtgBFKWk2jAyt5/view?usp=drivesdk
Report comment
I would like to say something helpful here that is self-evident …
If you or a family member is “mentally ill”, do NOT go to a psychiatrist. Go to a psychologist.
Stay away from psychiatrists …. they are dangerous.
The reported journal article is just another piece of confirmation.
Report comment
Gotta watch the psychologists, too. Many are wannabe psychiatrists who believe fully in the “biological brain disease” concept, especially for “schizophrenia” or “bipolar” diagnoses. If you are looking for a therapist who might have a chance of being really helpful, start by finding one who firmly believes the DSM is a useless doorstop and is more interested in what YOU think you need than in slapping some label on you. Just being a psychologist is no guarantee you won’t be routed down the same label-and-drug pathway!
Report comment
Yes Steve, and thanks for bringing this truth up. The majority of “mental therapists” are invested in the idea that they are “treating”.
Report comment
Absolutely true, Steve, the DSM billing code “bible” believing psychologists are every bit as bad, if not perhaps worse, than the psychiatrists.
Report comment