A new randomized, double-blind, placebo-controlled trial has found bright light therapy to be a powerful intervention that could provide an alternative to medication for people with “bipolar depression.” Two-thirds of the people receiving the light therapy improved, compared with one-fifth of those who took only medication. The research was led by Dorothy Sit at Northwestern University and published in the American Journal of Psychiatry.
The study included people who had a diagnosis of either bipolar I or bipolar II disorder, but who were not currently meeting criteria for a manic or hypomanic episode. All participants were taking “antimanic” medication, also known as “mood stabilizers” (e.g. lithium).
Many (78.3%) of the participants were also taking antidepressant medications, and the researchers made sure that both the control group and the intervention group had similar numbers of people taking these drugs. All participants also met criteria for continuing depression, despite their current medication regimen.
One group of 23 participants was exposed to 7000-lux bright white light daily, between noon and 2:30 pm. They initially began at 15 minutes of light use, then gradually increased to the “target dose” of 60 minutes per day at week 4. The other group received a placebo light intervention that was described as “50-lux dim red” light.
The difference in improvement is startling. 68.2% of people who received the bright light intervention no longer met criteria for depression (what researchers refer to as “remission”), compared with only 22.2% who received a placebo light intervention.
This difference was not due simply to an improvement in sleep quality, as sleep was observed to improve equally for both groups. There was no difference in side effects between the two groups, indicating that light therapy did not create any additional adverse events. No one experienced a hypomanic or manic episode.
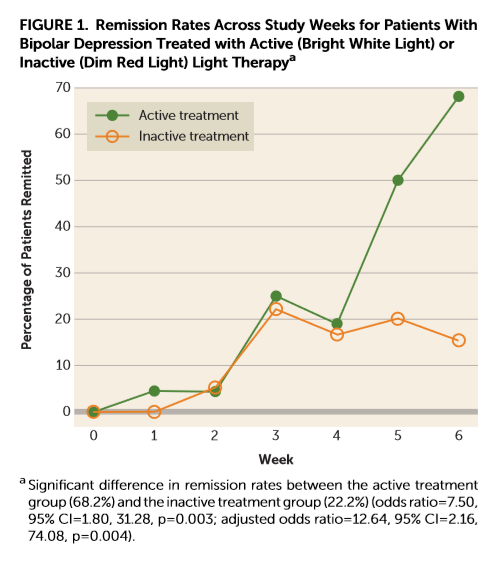
The improvement in depressive symptoms appeared to occur between weeks 4-6 for most participants, which the researchers theorize is due to reaching the 60-minute per day “dose” of light at week 4 (see graph below).
 Particularly surprising is that, despite most participants being on antidepressant medications, only one-fifth of those who did not receive the light therapy experienced remission of their depression. As noted by the researchers themselves, the antidepressant medications did not seem particularly effective in this case. They further write that antidepressant medication is often not recommended for this particular population, as it could trigger manic symptoms.
Particularly surprising is that, despite most participants being on antidepressant medications, only one-fifth of those who did not receive the light therapy experienced remission of their depression. As noted by the researchers themselves, the antidepressant medications did not seem particularly effective in this case. They further write that antidepressant medication is often not recommended for this particular population, as it could trigger manic symptoms.
Thus, given the lack of effectiveness of antidepressants, and their associated risks, bright light therapy could be positioned as an effective non-medication option for improving mood for people with the bipolar disorder diagnosis. The researchers also suggest that this could be an intervention suitable for pregnant women, who may not wish to risk taking psychopharmaceuticals.
****
Sit, D. K., McGowan, J., Wiltrout, C., Diler, R. S., Dills, J., Luther, J. . . . Wisner, K. L. (2018). Adjunctive bright light therapy for bipolar depression: A randomized double-blind placebo-controlled trial. American Journal of Psychiatry, 175(2), 131-139. https://doi.org/10.1176/appi.ajp.2017.16101200 (Link)















I just read the title of this article and thought that bright light therapy might also be more effective in treating Santa Claus’s depression, the Easter Bunny’s ADHD, and the Tooth Fairy’s Schizophrenia.
Good grief people. There’s no such thing as “bipolar disorder.” It’s a figment of the psychiatric imagination, just like every other bit of the myth of “mental illness.” There’s no such thing as an “antidepressant” either.
It’s simply sickening to considering how much money is being wasted on “studies” such as these. Nietzsche mocked the modern scholar who would become an expert on the brain of a leech, but he could never have foreseen the extent of the stupidity of the modern psychiatric researcher.
Report comment
Studies on “psychiatric” illnesses are frequently a waste of time, because the alleged diagnoses are simply descriptions of groups of behaviors that may or may not be linked. Within these “diagnostic” groups are individuals suffering from a heterogeneous bunch of conditions; it would be lucky to determine anything real about all the groups within such “diagnostic” categories.
Interesting enough, light therapy for psych patients has been around for about 40 years, but back then it was treated by the orthodox as a sort of equivalent to crystal gazing or having the witch doctor dancing around the fire, chanting and tossing mineral salts into the flames to get multi-colored flashes.
Report comment
Translation: Some doctors don’t know what they’re doing, and in the realm of quasi-medicine, if you happen to be a practitioner of such, that can be a big plus. How best treat an imaginary disease? With an imaginary cure, of course.
Report comment
lol
Report comment
It is pretty sad, these “mental health professionals” are still pretending the DSM disorders are real diseases, despite the fact all the DSM disorders were debunked as “invalid” by the head of NIMH five years ago. Goes to show how insanely delusional, and seemingly “incurable,” today’s DSM believing “mental health professionals” really are.
But at least he’s trying to educate the “mental health professionals” about the ineffectiveness of the “antidepressants.” And he did point out that the “antidepressants” are also dangerous, since they can create “mania.” I’ve met very few doctors who will actually admit to this. And, no doubt, this is a systemic problem amongst today’s medical community, since they’ve already misdiagnosed the common adverse effects of the “antidepressants” as “bipolar” in millions of people, including many children.
What’s really sad is the psychiatric industry’s response to Whitaker pointing this out was to make such a DSM-IV-TR “bipolar” misdiagnosis, an acceptable iatrogenic pathway to a “bipolar” diagnosis in the DSM5. Talk about absolute corruption within today’s psychiatric leaders.
I will say I do use a light box in the winters, and as a person who had the common adverse effects of an “antidepressant” (given under the guise of a “safe smoking cessation med”) misdiagnosed as “bipolar.” I have never suffered from the “depression” part of the “bipolar” misdiagnosis. I don’t know if that is because I use the light box or not, however.
Report comment
Well said
Report comment
Since prior to the time when Emil Kraepelin separated the redeemable bipolar disorder, then manic depressive psychosis, from the imminently irretrievable schizophrenia, his dementia praecox, this kind of leap to medicalizing judgment has been the trend. Yeah, “bipolar disorder” has represented one of the stalwart pillars of the “mental illness” religion, especially with the flipped coin genetic twist. If you want to be “sick”, like the magazine, this is your big chance. Jump on board. You, too, can fight the “stigma” of any psychiatric label’s unpopularity and tendency to buck the trend. You can start by introducing yourself to your friends as “Hi. I’m Bipolar.” Should a doctor agree, there’s money in it.
This is way up there with all of the Aut of the Autistic. Where, after all, culturally would we be without it? The institution has spawned it’s own variety of gallery debutante, and this disposition has a great potential for changing the world. (Not fast enough to suit me, of course.) What more can I say, but what an incredible update on ye ole chimpanzee!
Report comment
is bright light therapy helping anyone here…
is it helping the suffering that we experience…
bio/psy/soc model of causation is still here…
Report comment
You’re absolutely right, the only thing that this research is doing is promoting made up illnesses aka bi-polar.
Report comment
Back in the early ’90s, I noticed a strong correlation between the darkening of the days and the darkening of my mood. I used to journal almost daily, so it was right there in the pages, a big difference between the me that wrote in spring/summer and the me that wrote in the fall/winter was easy to discern. So I located a guy who made high-intensity full-spectrum light boxes (not easy before the internet) and bought one. Mine was 10,000 lux and I used it first thing in the mornings, for about a half-hour. The theory went like this: our circadian rhythms are primarily cued by the light we see. For some people, during the darker months when mornings are not as early or as bright, the light cue they take in visually is not strong enough to signal the brain to slack off on its melatonin production. So you boost the strength of morning light by adding the light box. Later, they came out with a “dawn simulator” version that you’d set like an alarm clock to brighten your bedroom gradually each morning. I never tried that- the light box I bought worked wonders.
Yes, it is another neurotransmitter imbalance theory. But considering that the biggest risk to the “treatment” was a little bit of UV exposure (less than I experienced in the summer sun) it was easy to test this theory on myself. I slept better. I had more energy in the day. I felt more human and less like a grumpy hibernating bear. So yes, my system improves dramatically with the introduction of a strong light cue to help my body regulate its melatonin production. To me, that’s no different than drinking extra water when I’m constipated: I’m just giving my body a bit more of an essential it needs to perform basic functions better.
Report comment
The mental health system including the psychotherapy industry is disordered and seems to do more harm than good – just helping to hide the misuse of power is a pretty nasty unintended consequence – not to mention pathologising people for suffering with seems more accurately like cultural experience disorder
just come across this ex therapist explaining why he is an ex therapist
nice honesty https://www.youtube.com/watch?v=f0Fi32LbXHA
Report comment
Anyone read Emil Kraepelin’s Psychiatric Observations on Contemporary Issues written just after WW1?
Here’s a couple of quotes…
“While one can accept or reject the legitimacy of the nobility, there can be no doubt that the fathers of the old noble lineages at some point distinguished themselves in relation to their countrymen by their special qualities. And history teaches us that more than a few of their progeny (offspring) produced a long line of superb personalities… One can furthermore assume that their positive traits were inherited and thus that later generations of an old family line which had defended its position over the centuries has, to a certain degree, retained those characteristics which once facilitated its rise.” croaks Kraepelin.
Kraepelin believes that royalty are genetically superior to us common as muckers and they have inherited ‘special qualities’, which is a prime example of blue blood thinking. Blue blood thinking is rampant in fairy tales and biological and genetic psychiatry. According to fairy tales all nobility, kings and queens, princes, princesses, lords and ladies, have blue blood, they are biologically different to the poor, they are cleverer, beautifuler and their inherited wealth is because of their inherited blue blood. He also thinks that the human race has evolved because of the survival of the fittest, that it’s only through war and violence that people progress.
“On the other hand it seems obvious that the ancestors of those belonging to the lower classes possessed, in general, no traits equipping them for extraordinary achievements and hence could not pass such traits on.” craps Craplin.
What the grandfather of psychiatry is saying here is that our great, great, great, great grandparents had no blue blood so couldn’t possibly do anything amazing, important or worthwhile, they passed on this worthless blood to their children, aka us who also can’t do anything amazing, important or worthwhile. Well, that must be the reason why I’m skint.
Report comment
The Kreep’s really pissed off that Germany lost the war and goes on to blame the selfish sick, Jews and women (of course!)
“The war has carried out a terrible selection among our most able and self-sacrificing men; it was above all the unfit and selfish individuals who remained unscathed…the humanitarian efforts to support the weak and to help the suffering, sickly, and the decrepit serve to counteract significantly a systematic rearing of the fit: they load the shoulders of the able-bodied (on whom our hopes for the future rest) with ever greater burdens under which the latter’s energies must ultimately expire.” kraps Krap.
Kraepelin is saying that only the good strong men died in the war, the one’s who couldn’t fight because they were old or sick are a burden to society and get in the way of an efficient war machine.
“The advance of combat neurosis was aided to a great degree by the fact that during the war the requirements for the physical and mental fitness of new recruits had to be lowered time and again. More and more incompetent, mentally deficient, infirm and morally inferior persons had to be drawn into service.” continues the Kreep.
Kraepelin also blames the soldiers who suffered shell shock for Germany’s loss of WW1.
“It is impossible to know how many imbeciles, epileptics, psychopaths, criminals, prostitutes and vagabonds are the children of alcoholic and syphilitic parents and have inherited the inferiority of their parents. Of course, the damage will in part be compensated for by their poorer ability to survive. But unfortunately, our ever-expanding social welfare programmes have the effect of impeding the natural self purification of our people. We have little reason to hope that, in the long run, our ability to regenerate ourselves will be strong enough to neutralize the ever growing dangers that threaten our germs.” curses Kraepelin.
Kraepelin says it’s a fact that poor people are born with nasty infections, mental illnesses and poverty. He’s really pissed off that the German people have a social welfare programme and want to help the poor but perks up a bit when he states that the sick have less chance of surviving because of inherited infections and poverty. He then goes on to scare the German people implying that they’ll all become weak and deformed because the sick people will mix with the blue blooded people and create sick babies who will destroy the human race.
“The well-known example of the Jews, with their strong disposition to nervous and mental illnesses… certainly also leaves its distinct imprint on the race.” curses Kraepelin.
Kraepelin states it’s a fact that Jewish people are born with mental illnesses, he is setting the scene for the holocaust, for the mass murder of the ‘mentally unfit’, criminals, prostitutes and next the Jews.
“In part it was the women who proved to be ill-prepared for the prolonged state of war and who tormented their sons and husbands at the front with their complaints and at times breached the trust of those in the field.” krap kraps Kraplin.
Blame the women again.
Report comment
This is the mind of the man who lay the foundations for the ‘modern’ diagnostic system of mental illness. His text books are an absolute gas too, he gives his patients drug cocktails, isolates them and generally treats them like shit then theorises why they behave a bit odd.
I work at the forefront of technology and I tell you, if psychiatry was a piece of software it would’ve been permanently deleted years ago, we would’ve switched on the virtual vacuum cleaner, emptied the defrag bag and moved on.
Report comment
Bingo. rawSienna, where do you stand with regards to the abolition of psychiatry and anti-psychiatry?
Report comment
Trash psychiatry, it’s not science, just sciency sounding stuff
Report comment
Amen.
Report comment
Light therapy is not a real therapy, but a means of neutralizing the deleterious effect of artificial light by mimicking natural light. It is rather a useful technology in a society where buildings hide sunlight and artificial light is omnipresent.
Light therapy, music therapy, work therapy, environmental therapy: what is part of the culture is transformed into “therapy”. That does not mean that all these things are bad, but simply that the psychiatric environment turns them into commodities.
Report comment
Exactly. I’d much rather have people exposing themselves to light rather than drugs, but why do they have to be “diagnosed” to do so? And what about the impact of the society that deprives its members of sufficient natural lighting?
Report comment
I think if you do something, possibly anything, that you expect might make you feel better, it probably will. And if you were in a study, and someone was acting even sort of half way like they were interested in how you felt, that would help you feel better. I tried a light like that once, and it didn’t seem to do anything, but I wasn’t expecting it to. What helps me is when anyone shows what I perceive to be a genuine interest in what I think or feel. I have never understood how therapists or psychiatrists hope to do anything with their cookbook methods.
Report comment
Yeah, really, it’s not rocket science. Listen empathetically, be interested, care, be real… don’t need to go to school for those, and in fact, no school can really teach them. What it requires is being in touch with your humanity and putting out your energy to be there for someone else. Apparently, that skill is in short supply, though!
Report comment
Spot on
Report comment
my psychiatrist asked if I was interested in light therapy….
I was and I tried using his light box for awhile..
I don’t think it helped…but it did help my friend…
my psychiatrist gets paid by medicare…he uses the
diagnosis of mdd…but he tells me he doesn’t think the dsm
is useful…only to get paid…he just thought maybe the light
would help my depression….I have had a major problem with
depression….I still am searching for the cause of my breakdowns..
Report comment
It’s really hard when you feel down and don’t have the right support, be that financial or emotional. What helps me is other people, yoga, painting, walking the dog and the knowledge that my sadness is temporary and if we didn’t feel sadness we could not experience joy as our emotions are relative. Sometimes it’s good to stop searching for causes, throw your coat on and walk.
Report comment
my psychiatrist is looking at this site…he does not like what is being
said about psychiatry and psychiatrists…I try to tell him that people here
have been hurt very badly by psychiatry and psychiatrists…he doesn’t like being
included in the bad part of psychiatry…he thinks psychiatry is mostly bad…
but he says you are throwing the baby out with the bathwater…he likes
critical psychiatry….getting rid of the bad…he sees psychiatry as being very sick..
Report comment
A note on… “All participants were taking “antimanic” medication, also known as “mood stabilizers” (e.g. lithium)”
Mood stabilisers are not generally considered specifically ‘anti-manic’ – they are instead generally considered as exactly mood stabilisers, in that they prevent ascent into mania AND descent into depression – as well as being used to treat acute mania and depression.
Thanks for the report.
Report comment
The term mood stabiliser is simply marketing, mood stabilisers are downers with very damaging side effects and ‘mania’ is merely a temporary state of heightened awareness, that might even prove to be an integral part of the healing process, if perceived and supported appropriately.
Ask yourself what is the correct mood to have at a wedding, a funeral or a rape scene?
Report comment
For some with mania it may be as you describe, for others it’s horrible and destructive and it’s far more than heightened awareness. Mood stabilisers, for all their terrible side effects have proven efficacy in reducing relapse rates to depression and mania.
What is the correct mood to have? Well only the individual can really be the judge of that, but many of those I’ve worked with would be very happy to sacrifice some heightened awareness in order to never again have a manic or depressive episode. Others feel that the benefits of medication in no way make up for the side-effects.
Report comment
“Particularly surprising is that, despite most participants being on antidepressant medications, only one-fifth of those who did not receive the light therapy experienced remission of their depression.”
SHOULD BE:
“Only one-fifth of those who did not receive the light therapy, most of whom were on drugs called “antidepressants,” experienced remission of their depression.”
“As noted by the researchers themselves, the antidepressant medications did not seem particularly effective in this case.”
SHOULD BE:
“Antidepressant drugs were not effective for 80% of those using them.”
“They further write that antidepressant medication is often not recommended for this particular population, as it could trigger manic symptoms.”
SHOULD BE:
“Beating around the bush, they submit that putative antidepressant drugs are not recommended for people diagnosed with bipolar depression because they reliably cause first-episode mania (occasioning the “bipolar” embellishment upon many patients’ depression diagnoses). This has no bearing on the matter at hand, which is that, as usual, the drugs didn’t relieve symptoms diagnosed as depression any better than countless time-honored therapies including placebo, distraction, the passage of time, dumb luck, a real problem, new shoes, a roll in the hay, and voodoo.”
Report comment
Fantastic BetterLife, very astute observations, or is it yet another case of can’t see the wood for the trees?
Report comment
Well done! Gave me a couple of laughs!
Report comment
Do not get scammed with those “special lights”
That 300 watt old school incandescent light bulb in the hardware store puts out the same color spectrum at the proper intensity.
I already researched this for the article on seasonal depression
Report comment