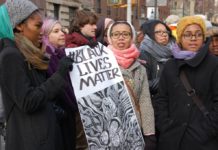Opening Doors in the Borderlands: An Interview with Liberation Psychologist Mary Watkins
MIA’s Micah Ingle interviews Mary Watkins about reorienting psychology toward liberation and social justice.
Discrimination Leads to Mental Distress for Gender Diverse People
Researchers seek to identify adaptive coping responses to discrimination for the transgender and gender diverse community.
Time’s Up: Culture of Denial Impacts Mental Health of Sexual Abuse Survivors
Study finds that not believing sexual abuse survivors often leads to self-blame and mental health issues.
Economic Deprivation and Social Fragmentation Drive Suicide Rates in US
Major study finds that economic deprivation and a lack of social capital are driving increasing rates of suicide in the U.S.
No Graphic Detail: The Injustice of Being Silenced
They tell us we’re too fragile to speak our own truth, and that those around us are too fragile to hear it. If you must name what happened to you, at least slap a “trigger warning” on yourself, and don’t “paint a picture.” Fuck that. The truth is that graphic detail can make some of us stronger in a way that silence never could.
Psychotropic Medications Serve as Powerful Tools for U.S. Military, Imperialism
Ethnographic research sheds light on extensive psychopharmaceutical use by soldiers in post 9/11 U.S. wars.
The Role of Intergenerational Trauma in the Perpetuation of Childhood Maltreatment
A new study examines the role parent borderline pathology plays in the perpetuation of childhood maltreatment.
Psychology Needs New Concepts and Healing Models for Racial Trauma
Contemporary empirical research explores new ways to conceptualize and heal racial trauma through anticolonial and sociohistorical lenses.
Researchers Identify Demographic, Ideological Factors Associated With Refugee Prejudice
A new analysis finds multiple antecedents of refugee prejudice, including religiousness, conservatism, and education.
Psychology Must Become a Sanctuary Discipline to Heal Racial Trauma
Researchers explore pathways of healing racial trauma in Latinx immigrant communities.
Psychologists Advise How to Help and Minimize Harm Working With Migrants and Refugees
While well intentioned, providers and volunteers can do more harm than good at the border. The Global Psychosocial Network issues guidelines on how to work for the benefit of migrants and refugees.
Study Identifies Psychiatric Patients at Greatest Risk of Coercion
In an effort to reduce coercion, researchers isolate associated factors including age, relationship status, location, and diagnosis.
Individuals with Psychosis Symptoms More Likely to be Victimized
Individuals diagnosed with a psychotic disorder are 4-6 times more likely than the general population to experience victimization.
What is Loneliness And How Can it be Addressed?
As an increasing amount of research seeks to address the epidemic of loneliness, conceptual clarity is needed.
Integrating Indigenous Healing Practices and Psychotherapy for Global Mental Health
As the Global Mental Health Movement attempts to address cross-cultural mental health disparities, a new article encourages integrating traditional healing practices with psychotherapy.
Study Finds Deteriorating Mental Health Among Poor White Americans
Researchers find evidence of low socio-economic status White Americans’ rising distress and declining well-being since the mid-1990s.
Outcomes of Childhood Bullying on Young Adults’ Wellbeing
A qualitative study explores young adults’ childhood bullying experiences.
Does Psychotherapy Reproduce or Disrupt Neoliberal Capitalism?
Researchers explore neoliberal influences on interactions in psychotherapy and question whether the radical potential of psychotherapy can counter prevailing social systems.
The Psychological Effects of the Zero-Tolerance Immigration Policy
Journal releases a compilation of articles detailing how zero-tolerance policy may impact mental health.
Sociologists Interrogate Neurobiological Explanations in Criminology
A discourse analysis conducted by sociologists finds problematic assumptions and practices in the field of neurocriminology.
Correcting Misconceptions of Trauma-informed Care with Survivor Perspectives
Trauma-informed approaches have the potential to promote recovery but must involve survivors and service-users to prevent the experience of retraumatization within psychiatric and mental health services.
Current Immigration Policies Create Mental Health Vulnerabilities for Families
Researchers investigate the impact of immigration policies on the mental health of arriving Mexican and Central American immigrants.
What Does Social Justice Really Mean for Psychologists?
Without clarity and consensus around what social justice means, psychologists risk perpetuating injustices that undermine their stated mission.
Out-of-home Placements for Children Increase Odds of Psychiatric Issues
When controlling for social and family characteristics, separating children from parents into out-of-home care increases psychiatric issues, prescriptions, and criminal activity.
Sociologist Questions Effectiveness and Ethics of Mental Health Services
Medical sociologist David Pilgrim argues that mental health care is neither effective nor “kindly,” as it often relies on flawed research and ineffective treatments.