Earlier this year, Ronald Pies and Allen Frances wrote a series of blogs that collectively might be titled: “Why Robert Whitaker is Wrong about Antipsychotics.” In regard to reviewing the “evidence” on that question, Pies did most of the heavy lifting, but he also told of drawing on the expertise of E. Fuller Torrey, Joseph Pierre and Bernard Carroll. Given the prominence of this group, it could be fairly said that Pies’ review reflects, to a large degree, the collective “thoughts” of American psychiatry.
And with that understanding in mind, therein lies an opportunity, one not to be missed.
Over the past 35 years, psychiatry—as an institution—has remade our society. This is the medical specialty that defines what is normal and not normal. This is the medical specialty that tells us when we should take medications that will affect how we respond to the world. And this is the profession that determines whether such medications are good for our children. Given that influence, we as a society naturally have reason to want to know how the leaders in the profession think, and thus how they come to their conclusions about the merits of their drugs. The blogs by Pies and Frances provide us with just that opportunity. We can watch their minds at work and ask ourselves, do we see on display the type of thinking—the openness of mind, the critical thinking, the curiosity, the humility of character, and the devotion to public wellbeing—that we want to see in a medical specialty that has such influence over our lives?
There are two aspects to their review of the “evidence” for antipsychotics. The first is their dismissal of the case against antipsychotics (e.g., that they worsen long-term outcomes in the aggregate), and the second is their making a case that the drugs provide a long-term benefit. In each instance, there are specific studies to be reviewed, and, as a result, a warning to readers is in order: this is going to take some time to do.
The Case Against Antipsychotics
As I first detailed in Anatomy of An Epidemic and have expanded on since (including in a January blog), I believe there is a history of science, stretching across 50 years and composed of many types of studies, that tells of how antipsychotics, in the aggregate, worsen long-term outcomes for schizophrenia patients and those with other psychotic disorders. The case against antipsychotics doesn’t consist of just a few studies, but rather arises from that history of research, and what I find so compelling is how the various kinds of evidence fit together, and how they do so over time. This is not the place to go over that history once again, but if readers are interested, they can see a summary in my January blog, and a review of many of the studies here.
It’s not important, for the purposes of this blog, to come to any pro-or-con conclusion about whether antipsychotics worsen long-term outcomes. What is important is to see how Pies and his colleagues responded to that argument and evaluated it.
Neither Pies nor Frances addressed the larger history I wrote about. Instead, they focused on the recent literature that is part of this “case against antipsychotics“—research by Martin Harrow and Lex Wunderink, and MRI studies that have found that antipsychotics shrink the brain. They also addressed the question of whether antipsychotics induce a dopamine supersensitivity that could increase one’s biological vulnerability to psychosis, which is something I have written about.
Harrow’s Longitudinal Study
In any area of medicine, it is essential to research the “natural” course of an illness. Prognosis is dependent upon that knowledge, and this knowledge also provides the framework for assessing whether a treatment is improving long-term outcomes. Such research is exhausting, difficult, and expensive, which is why the long-term study of schizophrenia and other psychotic disorders by Martin Harrow is so important. It provided information that had been missing from psychiatry’s “evidence base” for so long.
Harrow’s was a prospective study, which means he followed the 200 subjects from early on in their “illness,” mostly at the start of their having been diagnosed with schizophrenia or another psychotic disorder. Their median age was 22 years and nine months, and most were suffering either a first or second hospitalization. At the end of 15 years, he still had 145 of the 200 in his study, which—as any schizophrenia researcher can attest—is an extraordinary result on its own. Harrow had gone to extraordinary lengths to keep track of the subjects enrolled into his study, which made his findings that more robust.
There is much to be learned from his published results, and if there is one response that I think our society would want to see from the psychiatric establishment, it is just that: a keen curiosity about the results, and a desire to use this information to improve treatment protocols. Harrow’s results belied the common beliefs that have driven societal thinking—and treatment protocols—for the longest while.
The first surprising finding was that, as a group, patients who stopped taking antipsychotic medications notably improved between the 2-year and 4.5-year follow-up. The conventional wisdom is that this group could have been expected to deteriorate and suffer from multiple relapses, but Harrow found the opposite to be true: on the whole, their psychotic and anxiety symptoms abated, and 40 percent of the group were in “recovery” by the end of 4.5 years. And Harrow defined recovery in a robust way: an absence of symptoms; working or in school more than 50% of the time; and a decent social life.
This is exciting news. This is the only place in the research literature where you can see this potential for healing play out over this longer period of time, and it tells of the possibility that a significant percentage of patients, even those diagnosed with schizophrenia, can get better and resume a meaningful life, and do so without suffering the many adverse effects of antipsychotics. This is a finding to be embraced, with the profession challenged, one might expect, to develop protocols to maximize this possibility.
The second surprising finding, however, was quite dispiriting, given the current standard of care. The medicated patients, as a group, worsened during this same time frame (2 to 4.5 years): the percentage of patients who were psychotic increased; the percentage who were highly anxious increased; and the recovery rate decreased, to the point it was only 1/8 the rate for the patients who had stopped taking antipsychotics.
The divergent results also led to an obvious question: Did the medications, for some reason, block or thwart the natural healing process seen in many of the unmedicated patients? Medication is thought to be an essential treatment for schizophrenia, and yet these findings, which remained stable throughout the study, did not support that belief.
Moreover, any researcher digging into Harrow’s data would have found reason for this concern to deepen. In every subgroup of patients, the medicated patients did worse over the long term. The good prognosis schizophrenia patients who got off medication did better than the good prognosis patients who stayed on, and the same was true for the bad prognosis patients, and for those with milder psychotic disorders. In each subset, the off-medication group did much better. Even more compelling, the schizophrenia patients who got off antipsychotics did better than those with milder psychotic disorders who stayed on the medication, as can be seen in the graphic below.
These are the findings that Harrow’s longitudinal study, the best of its kind in the modern drug era, presented to American psychiatry. This was data, it seemed, that should be added to the “evidence base” for antipsychotics. However, Pies did not see it that way:
“Patients in the Harrow study were not randomized. This means those with milder symptoms may have ‘self-selected’ to discontinue medication, whereas those with more severe illness—who would be expected to have a poorer outcome—elected to stay on medication. So the Harrow studies did not prove that long-term antipsychotic treatment per se worsened outcome. It is more likely, as Dr. Pierre notes, that the type or severity of patients’ symptoms determined whether or not they and their doctors decided to continue medication. Thus, in analyzing the Harrow studies, some critics of antipsychotic treatment may have misperceived the ‘arrow of causality.’ ”
The response by Pies has been the same argument voiced by others who have criticized Anatomy of an Epidemic, and fairly sums up how psychiatry, as a field, has responded to Harrow’s study. There isn’t much to be learned from it; the fact it wasn’t randomized provides an explanation for the results; and the likely explanation for the divergent outcomes is that the more severely ill patients were the ones who stayed on an antipsychotic, while psychiatrists helped the less severely ill get off the medication.
This is a response that does protect psychiatry’s belief in its antipsychotics, and its sense of self. But it is one that is absent of any curiosity about the study, and absent of any desire to use this information to improve treatment protocols. Pies’s dismissal also reveals a lack of knowledge about the details of the study, or — and this may be more likely — a turning of a blind eye to them.
First, the idea that a difference in severity of illness explains the divergent outcomes is belied by the group-by-group outcomes, and by the fact that the more severely ill who got off the drugs did better than the less severely ill who stayed on. Perhaps there is a non-drug explanation for the divergent outcomes, but the available facts don’t support the “severity of illness” speculation.
Second, the idea that psychiatrists helped the off-medication group get off their drugs is plucked out of thin air too. Those who stopped taking medication and got better mostly dropped out of care. These were non-compliant patients who did better.
Third, the “correlation not causation” dismissal is also not descriptive of the actual data. A naturalistic study, of course, does have its limitations. However, an antipsychotic is meant to be a causative agent, and thus change the course of the illness, and so what you have in this instance is “correlation with a causative agent,” which is a very different thing. This is a correlation that provides reason to give the outcomes further weight. The findings in Harrow’s study don’t prove causality, but particularly once the group-by-group outcomes are detailed, the study — at the very least — provides reason to worry about possible causality.
But such worry is missing from Pies’ response, and indeed, if his response is carefully parsed, you can see that instead he praises his colleagues for their scientific acumen and their prescribing skills. He and his colleagues, being men and women of science, understand that correlation doesn’t equal causation, unlike psychiatry’s misinformed critics (e.g. me). Psychiatrists could also take credit for the good outcomes of patients off medication in Harrow’s study. Psychiatrists had assessed how well their patients were doing, and in collaboration with their patients, successfully identified those who could discontinue their medication. His profession is doing quite well, thank you.
Wunderink’s Randomized Study
A few years after Harrow reported his findings, Lex Wunderink from the Netherlands published the seven-year results from his study, which included a randomized element in its design. His findings, broadly speaking, replicated Harrow’s.
In Wunderink’s study, 128 first-episode psychosis patients who had remitted on antipsychotics were randomized into two groups: drug treatment as usual, or treatment that involved dose reduction or discontinuation from the drugs. In essence, his was a randomized study that compared long-term outcomes for patients treated, at a single moment in their care, with a different treatment protocol.
At the end of two years, the relapse rate was higher for the low-dose/discontinuation group (43% vs. 21%.) However, by the end of seven years, the relapse rate was slightly lower for the no-drug/low dose group, and the recovery rate was more than twice as high for this group (40% versus 18%.) This study revealed the long-term benefit of a drug-tapering protocol following initial remission.
If Wunderink’s data is carefully studied, there is one other comparison to be made at the end of seven years. During the followup, there were patients in the low-dose/off-med group who ended up on regular doses of antipsychotics, and conversely, patients randomized to regular treatment who stopped their medication, or got down to a low dose. Here are the seven-year results grouped by medication use:
Together, Harrow’s and Wunderink’s studies provide evidence—or so it would seem—for psychiatry to rethink its treatment protocols, which today emphasize medication compliance as the key to a successful long-term outcome. These studies argue for a treatment protocol that would try to help first-episode patients get down to a low dose or discontinue antipsychotics altogether. That strategy, these two studies indicate, would produce much better long-term recovery rates.
Pies and those he consulted didn’t see it that way. Much like Harrow’s study, Wunderink’s could be discounted. Pies wrote:
“First of all, most of the subjects in the dose/reduction arm of the study actually remained on antipsychotic medication, although at a reduced dose. Secondly, as Dr. Pierre notes, ‘while the initial treatment allocation was randomized, the subsequent dose changes in both treatment groups were based on clinical response and occurred at the whim of the treating psychiatrists.’ Thus, this was not really a randomized study. And rather than antipsychotic treatment worsening outcome, it seems more likely that patients perceived by their doctors as doing relatively well were, understandably, given lower doses of medication; conversely, patients perceived as doing worse were likely maintained on higher doses . . . this study does not support the claim that long-term antipsychotic maintenance is causally related to poorer outcome.”
Once again, there apparently is little to be learned from Wunderink’s results. There is no drug-tapering protocol to be adopted; it seems psychiatrists are already quite good at helping their “less ill” patients get down to low doses, or off the drugs altogether. Nor is there reason to worry that antipsychotics may be doing long-term harm. As was the case with their review of Harrow’s study, Pies and his colleagues saw Wunderink’s findings as another account of less-ill patients doing better than severely ill patients, with psychiatrists helping their patients find the right medication path. The study, in their view, provides no reason to think that medications played a role in the divergent outcomes.
MRI Research
The advent of MRI technology twenty-five years ago enabled researchers to begin studying brain volume changes in patients diagnosed with schizophrenia and other psychotic disorders, with such changes measured over time. By the late 1990s, investigators doing such research had reported that antipsychotics caused basal ganglion structures and the thalamus to swell, and the frontal lobes to shrink, with these changes in brain volumes “dose related.” In 1998, Raquel Gur, from the University of Pennsylvania, reported that the swelling of the basal ganglia and thalamus was “associated with greater severity of both negative and positive symptoms.” This was disconcerting news: the brain volume changes were associated with a worsening of the very symptoms the drugs were supposed to treat.
Soon Nancy Andreasen, who was then editor-in-chief of the American Journal of Psychiatry, weighed in with her findings from a study of 500 schizophrenia patients. In 2003, she reported that their frontal lobes shrank over time, and that this shrinkage was associated with a worsening of negative symptoms and functional impairment, and after five years, with a significant worsening of their cognitive abilities. She at first attributed this shrinkage to a disease process, but subsequently reported that it was related to antipsychotic usage, and was in fact dose related. The “more drugs you’ve been given, the more brain tissue you lose,” she told the New York Times.
This research appears to tell of a clear iatrogenic process. Antipsychotics cause changes in brain volumes that are associated with a worsening of negative and positive symptoms, and a worsening of functional impairment. Then, once Harrow reported his findings, the pieces of an “evidence-based” puzzle seemed to come together. The MRI studies told of drugs that worsened long-term outcomes, including psychotic symptoms, and that is what Harrow had found. Investigations of different types had pointed to the same conclusion.
In his review of the MRI studies, Pies acknowledged that they “indicate an association between antipsychotic use and reductions in cortical gray matter.” He also acknowledged that such findings “are surely concerning.” But in his review of the MRI literature, he didn’t include reports by Gur and Andreasen that such brain changes were associated with a worsening of symptoms and functional impairment. That salient fact was missing. Instead, he directed his readers to a 2015 study by investigators at the University of California at Davis who, Pies wrote, found that “while short-term treatment with antipsychotics was associated with prefrontal cortical thinning, treatment was also associated with better scores on a continuous performance task.”
The suggestion being made here is this: Although the drugs may cause brain shrinkage, they may still improve functional outcomes.
This finding, at first glances, seems at odds with Andreasen’s and Gur’s. But if you read the UC Davis study, you find that the psychotic patients in this study had been on antipsychotics for a short time (mean duration was 99 days), and had suffered a first episode of psychosis less than one year earlier. The finding that the medicated patients scored better on a continuous performance task at the end of 99 days is consistent with the idea that these drugs provide a short-term benefit. However, Andreasen charted brain shrinkage over a number of years and found that, over this longer period of time, it was associated with worsening symptoms and impairments. The MRI data reviewed here supports the idea that while the drugs may provide a short-term functional benefit, they induce brain-volume changes that are harmful over the long-term.
That would be the picture to be presented from a full review of the brain shrinkage evidence. But Pies focused on the UC Davis study, and having done so, he concluded: “In my view, we need more research to sort out this complex issue, while always weighing carefully the neurological risks of antipsychotic treatment (including movement disorders) against their very real benefits.”
In this summary, Pies has recast the brain shrinkage as an adverse event, which needs to be weighed against the drugs’ very “real benefits.” That is a statement that tells of drugs that still reduce symptoms over the long term, rather than make them worse, and it also lessens a sense of immediate alarm. Gur’s study may now be nearly 20 years old, and Andreasen’s not far behind, but this remains today a worry to be sorted out in the future. Until that time, patients prescribed these drugs will just have to hope that Gur’s and Andreasen’s research, linking brain shrinkage to a worsening of symptoms and functional outcomes, is wrong.
The Case For Antipsychotics
Having dismissed the case against antipsychotics, Pies then set forth a summary claim about the evidence for the drugs: “I believe that most randomized, long-term studies of schizophrenia support the benefit of antipsychotics in preventing relapse. Some data also show better ‘quality of life’ with maintenance antipsychotic treatment, compared with drug discontinuation.”
Although this statement makes it appear that there are a great many randomized, long-term studies that tell of better outcomes for the medicated patients, Pies doesn’t cite any such studies. But he does cite a meta-analysis of drug-withdrawal studies by Stefan Leucht, and so it appears he is referring to this body of research, which is the very “evidence” that psychiatry has long pointed to as reason for maintaining their patients on these drugs.
Relapse studies
In his meta-analysis, Leucht identified 65 drug-withdrawal studies that had been conducted from 1959 to 2011. The median age of the patients was 40.8 years; their mean duration of illness was 13.6 years. More than half of the studies were in hospitalized patients.
In 54 of the 65 studies, the antipsychotic was abruptly withdrawn. In the 11 other studies, the medication was either tapered over at least a 3-week period, or depot treatment was allowed to lapse. In two-thirds of the studies, relapse was based on “clinical judgment” or patient seen “in need of medication,” as opposed to the use of a scale to measure psychotic symptoms. In other words, relapse in the majority of studies was dependent on an eyeball assessment by the psychiatrist.
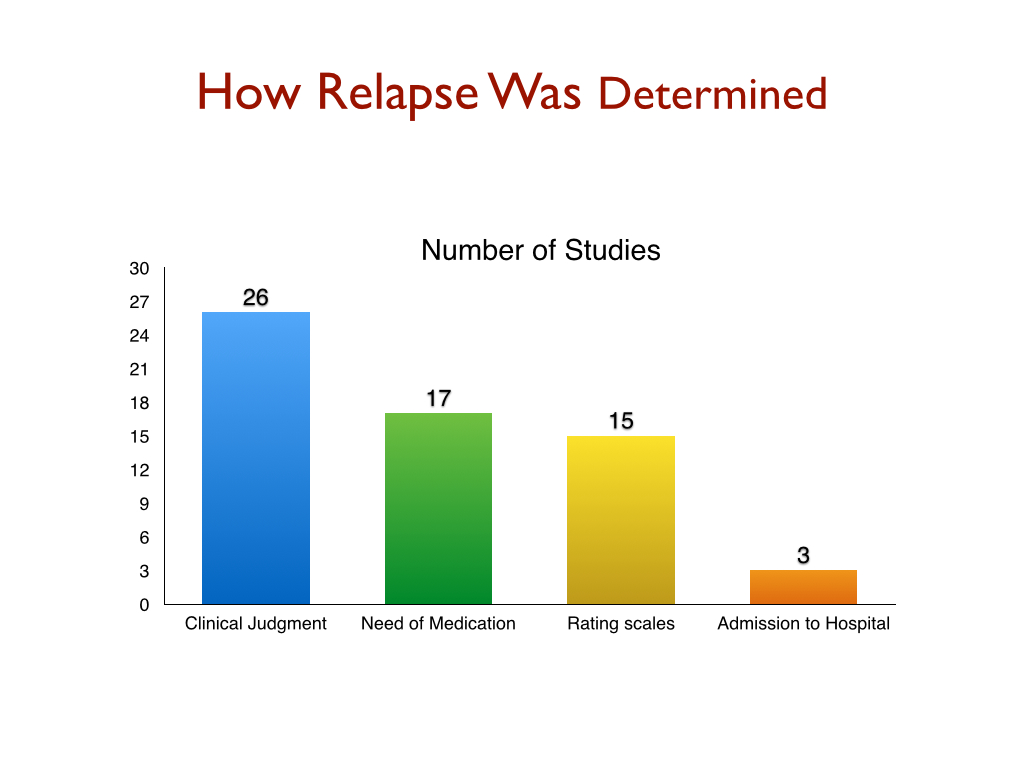 At the end of three months, the relapse rate was 12 percent for the drug-maintained group versus 37% for the drug-withdrawn group. At the end of one year, the relapse rate was 27% for the drug-maintained group versus 65% for the drug-withdrawn patients. Although the superiority of the drug-maintained group lessened over time, there was still a higher percentage of relapses in the drug-withdrawn group from months 7 to 12 (among those patients who didn’t relapse in the first six months.)
At the end of three months, the relapse rate was 12 percent for the drug-maintained group versus 37% for the drug-withdrawn group. At the end of one year, the relapse rate was 27% for the drug-maintained group versus 65% for the drug-withdrawn patients. Although the superiority of the drug-maintained group lessened over time, there was still a higher percentage of relapses in the drug-withdrawn group from months 7 to 12 (among those patients who didn’t relapse in the first six months.)
Data on “quality of life” from this relapse literature was “poor.” There were only three studies–out of the 65– that assessed this outcome; in two of the three studies there was “an almost significant trend” favoring the drug-maintained group. There was no significant difference in the third. The data on unemployment was “very poor,” as it had been collected in only two studies, and in those two, there was no difference in employment rates. There was no data at all on “satisfaction of care.”
Although “relapse” rates were lower in the drug-maintained group, 70% of these patients either failed to improve or worsened during the study (versus 88% among the drug-withdrawn group.) In the inpatient studies, only 5% of the drug-maintained patients were discharged.
Such is the data from fifty years of relapse studies. If the findings are critically accessed, what conclusions can be drawn?
Now, I have to admit, I had looked at the relapse literature before, but I didn’t realize, until I read Leucht’s study, just how flimsy this literature was. What does “relapse” even mean in most of these studies? Since the determination relied on “clinical judgment” in two-thirds of the studies, rather than a measurement of psychotic symptoms, were insomnia, agitation, or loud behavior symptoms of relapse? Wouldn’t withdrawal symptoms, whether one was abruptly or gradually withdrawn from the drug, often be seen, in the clinical judgment of the psychiatrist, as evidence of “relapse?” In fact, based on patient accounts of withdrawing from antipsychotics, it would seem that nearly everyone withdrawn from the medication would be seen, at some point, to have “relapsed.”
At the same time, what does it mean to be on the drug and to not have relapsed? If 70% of the drug-maintained patients failed to improve or worsened, with only 5% of the hospitalized patients who stayed on medications discharged, what is the state of a “non-relapsed” patient? Is a patient who sits quietly on a ward in a subdued state judged to have been “non-relapsed”? If someone is still too dysfunctional to be released, how does that qualify as a “good outcome,” e.g., non-relapsed?
And how is it that in fifty years of this research, which was designed to assess whether patients should be maintained on antipsychotics, there have been only three studies that even assessed quality of life, or employment?
But such are the questions that occur to my admittedly “untrained” mind. Pies, for his part, found this research to be reassuring. The meta-analysis, he wrote, suggests “that long-term antipsychotic treatment clearly improves outcome in schizophrenia . . . quality of life was also better in participants staying on medication.”
In that phrase, the results have been transformed: a difference in “relapse” rates is equated to “clearly improves outcomes,” and “poor data” on quality of life is remade into a broad conclusion that drug-maintained patients have a better quality of life. (Leucht, in his abstract, similarly turned the “poor data” described in the discussion part of his paper into a broad conclusion.)
No Evidence of Dopamine Supersensitivity
Pies and his colleagues also found comforting evidence of another sort in the relapse literature: it provides reason to discount the worry that antipsychotics induce a dopamine supersensitivity that makes patients more biologically vulnerable to relapse, which exposes the patients to severe relapses upon drug withdrawal.
The “dopamine supersensitivity” concern arose in the late 1970s, after a series of NIMH-funded studies found that relapse rates, over longer periods of time, were higher for medicated schizophrenia patients than for patients never exposed to the drugs. This led two Canadian investigators, Guy Chouinard and Barry Jones, to posit a biological explanation for why this might be so.
Antipsychotics blocked dopamine receptors in the brain (and in particular a subtype known as the D2 receptor.) In compensatory response, the brain increased the density of its D2 receptors. The brain was now supersensitive to dopamine, and Chouinard and Jones reasoned that that this could have two harmful effects: It could lead to severe relapses upon drug withdrawal, and yet, if patients stayed on antipsychotics long-term, there was the risk that a persistent, chronic psychosis would set in. In 1982, they reported that 30% of the 216 patients they studied had signs of “tardive psychosis.” When this happens, they wrote, “the illness appears worse” than ever before. “New schizophrenic or original symptoms of greater severity will appear.”
Chouinard has since written several articles on supersensitivity psychosis, noting that it often appears “with the decrease or withdrawal of an antipsychotic.” This “discontinuation syndrome,” he wrote in 2008, produces “psychiatric symptoms that can be confounded with true relapse of the original illness,” and if clinicians would recognize this, “long-term maintenance treatment could be reduced and avoided in some patients.” This rebound psychosis was “known to occur within 6 weeks following the decrease or withdrawal of an oral antipsychotic or within 3 months for a long-acting injectable antipsychotic.”
In other words, from Chouinard’s perspective, many of the drug-withdrawn patients in the relapse studies were likely suffering drug-withdrawal symptoms, as opposed to a return of the illness, and counting such patients as relapsed leads to a mistaken understanding of the “benefits” of using antipsychotics as a maintenance treatment.
Numerous other researchers have weighed in on these withdrawal risks. Australian researchers surveyed 98 users with varying diagnoses who had stopped taking antipsychotics and found that 78% experienced “negative effects” during withdrawal, which included “difficulty falling or staying asleep, mood changes, increases in anxiety/agitation, increases in hallucinations/delusions/unusual beliefs, difficulty concentrating/completing tasks, increases in paranoia, headaches, memory loss, nightmares, nausea and vomiting.”
Meanwhile, Japanese investigators have reported how drug-induced dopamine supersensitivity leads to “treatment-resistant” schizophrenia in a significant percentage of patients.” Philip Seeman, in animal-model experiments, concluded that this was why antipsychotics “fail over time.” Martin Harrow cited drug-induced dopamine supersensitivity as a possible reason for why such a high percentage of the medication-compliant patients remained psychotic over the long-term, while the majority of off-medication patients became asymptomatic.
Leucht and his colleagues, in their review of the relapse literature, briefly addressed this worry. Although the relapse rate for drug-withdrawn patients was particularly high in the first three months, there was no significant difference in those rates in the meta-analysis depending on whether the drug was abruptly or gradually withdrawn. This argued against the dopamine supersensitivity theory, they said.
In addition, they noted, the relapse rate during months 7 to 12 was still higher for the drug-withdrawn patients. These results, the researchers concluded, did “not support the suggestion that beneficial effects of antipsychotic drugs could be merely because of supersensitivity psychosis.” At the same time, they wrote, it was “possible that supersensitivity psychosis explains a pattern of the decreasing effect sizes in longer trials.”
In essence, Leucht and his colleagues had not put aside the dopamine supersensitivity worry, but had argued that, even apart from that possible confounding factor, the drugs appeared to provide a real benefit in reducing relapse, at least to some extent. However, Pies found reason, in the relapse data, to dismiss the worry that the dopamine supersensitivity was a confounding factor.
“Critics sometimes charge that apparent relapse among persons with schizophrenia does not represent a bona fide recurrence of the original illness. Rather, they claim, it is simply a ‘withdrawal effect’ that occurs when antipsychotic medication is rapidly discontinued, owing to a flare-up of ‘super-sensitized” dopaminergic neurons. Yet when we look at the time course of psychotic relapse, it usually occurs several months after discontinuation of the antipsychotic. This is not consistent with what we know about most drug withdrawal syndromes, which usually occur days to a few weeks after a drug is suddenly stopped. Thus the ‘withdrawal psychosis/super-sensitivity psychosis’ notion remains, at best, a highly speculative hypothesis, in so far as psychotic relapse is concerned.”
Once again, this is a misreading of the data in Leucht’s meta-analysis. In fact, 37% of the drug-withdrawn patients relapsed within the first three months, which belies Pies’ claim that relapse “usually occurs several months after discontinuation of the antipsychotic.” It is this initial post-withdrawal period that creates most of the difference in relapse rates between the two groups. (See graphic below.)
But Pies saw this data as reason to downgrade the worry about dopamine supersensitivity to a “highly speculative hypothesis.” Much like the MRI studies, this was another concern that could be punted down the road. Perhaps, in the future some researchers could look into it a bit more.
Harrow No, China Yes
Although Harrow’s and Wunderink’s longitudinal studies were not seen by Pies and his colleagues as providing useful information about the effects of antipsychotics over the long term, Pies did find one longitudinal study, conducted in rural China, worth citing in this regard.
“Recently, researchers in China carried out a 14-year prospective study of outcome in people with schizophrenia (N=510) who had never been treated with antipsychotic medications and compared outcome with those who were so treated. Consistent with the Leucht findings, the Chinese investigators found that partial and complete remission in treated patients were significantly higher than that in the never-treated group—57.3% vs. 29.8%. Moreover, the authors concluded that . . . ‘never-treated/remaining untreated patients may have a poorer long-term outcome (for example higher rates of death and homelessness) than treated patients.’ ”
Five years ago, when I gave a psychiatry Grand Rounds presentation at Massachusetts General Hospital, which was followed by a rebuttal by Andrew Nierenberg (in which he concluded Anatomy of an Epidemic should come with a black box warning), Nierenberg also pointed to this Chinese study as providing evidence of the long-term efficacy of antipsychotics, while similarly dismissing Harrow’s research as meaningless. As such, by examining this study, we can see the type of longitudinal research that psychiatry’s Thought Leaders find worthwhile.
The Hong Kong investigators, in a survey of more than 100,000 people in a rural community in China, identified 510 people who met the criteria for a diagnosis of schizophrenia. In this cohort, there were 156 who had never been treated at the start of the study in 1994, and 354 who had been “treated,” which was defined as having received antipsychotic medication at least once.
The two groups were not at all similar at baseline. On average, the untreated group was 48 years old and had been ill for 14 years. People in the community who had suffered a psychotic episode but then recovered without treatment would not have shown up in this group. In layman’s terms, this was a chronically “crazy” group that researchers had identified. Moreover, compared with the treated patients, they were “significantly older, less likely to be married, more likely to have no family caregiver and to live alone, had a lower education level, and fewer family members.” The “untreated” group also came from families with a significantly lower economic status, and they were more likely to have been abused by their families. In addition, the never-treated group was more severely ill at baseline: they had a “longer duration of illness; higher mean scores on the PANSS positive subscale; and had higher PANSS negative subscale and general mental scores.” Eighty three percent had “marked symptoms/or were deteriorated,” compared to 53% of those in the “treated” group.
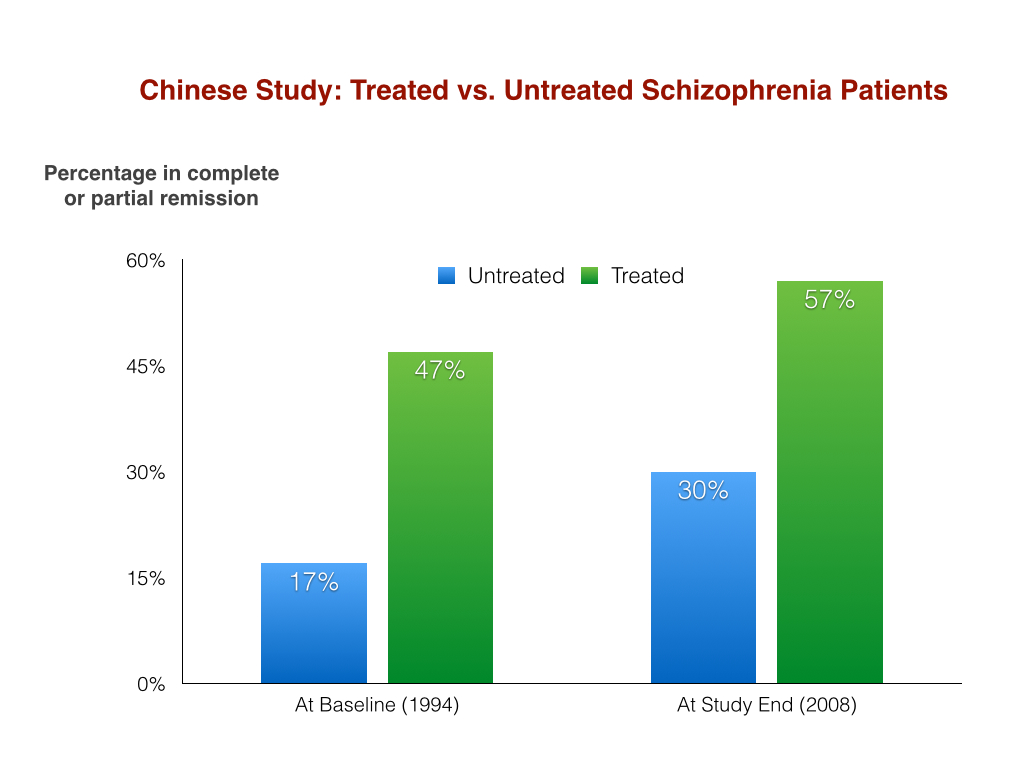
At the end of 14 years, the treated group—which simply meant that they had exposure to antipsychotics at some point in their lives—was still doing better. Fifty-seven percent were now in complete or partial remission, up from 47% at the start of the study (an increase of 10%). Thirty percent of the untreated group were now in complete or partial remission, and while that was still lower than the treated cohort, it meant that there had been an increase of 13% in this good outcomes category.
In sum, the percentage of the untreated group who had improved was actually greater than for the treated patients, but since they had been so much more severely ill at baseline, with so many worse prognostic factors, their collective outcomes were still worse at the end of 2008.
We can now see, quite clearly, the “mind” of psychiatry at work in its assessment of the research literature. Pies and his colleagues dismiss an NIMH study (Harrow’s) that followed patients from early on in their “illness” and regularly documented their functioning on a number of domains, and the reason they give for their dismissal is that “correlation doesn’t equal causation.” They use this reasoning even though those with a milder diagnosis at baseline who stayed on the drugs did much worse over the long-term than those with a more severe diagnosis at baseline who got off the medications. Yet, the profession can find merit in a study that isolates a group of chronically ill, “crazy” people in a rural Chinese community, and compares them to a less ill group that also has many social advantages, and then finds that this latter “treated” group is doing slightly better, in terms of percentage who were in remission, at the end of 14 years. The “correlation doesn’t equal causation” refrain is now suddenly absent.
At this point, I have to confess that I am reminded of how Pies began his piece. Assessing psychiatry’s evidence base, he said, was a task best left up to the profession itself, as critics lacked the necessary expertise.
“This article is by no means a comprehensive review of the voluminous, decades-old literature on AP (antipsychotic) maintenance: rather, it is a commentary on some recent studies and their sometimes controversial interpretation. I would argue that interpreting these complex studies requires an in-depth understanding of medical research design, psychopharmacology, and the numerous confounds that can affect treatment outcome. Unfortunately, a lack of medical training has not stopped a few critics from confidently charging that psychiatrists are harming their patients by prescribing long-term AP treatment.”
It requires a certain medical training, it seems, to see the scientific literature in the way they do, and I have to agree, that is true. Pies’ writings reflected the same assessment of the literature that Andrew Nierenberg made years ago, when he “repudiated” Anatomy of an Epidemic at a Grand Rounds. It is now five years later, and I still cannot see the Harrow study or the Chinese study in the way they do. Perhaps if I went to medical school, and became trained as an academic psychiatrist, I would — and I am not being sarcastic here — see the studies in the way they do. We think of medical training as providing doctors with an expertise, but it also inducts them into a tribe, which has a terrible tendency to think alike.
The Record Has Been Set Straight
Pies’ piece was published in the Psychiatric Times, which means that it was directed as his peers, a post designed to assure them that all was okay in the world of psychiatry, and with its use of antipsychotics. Frances then incorporated Pies’ piece into his blogs on this topic, where, over the course of three posts, he told of “setting the record straight on antipsychotics.” Here are a few salient quotes from his blogs:
- “Bob’s position that antipsychotics cause more psychosis than they cure is based on his fundamental misreading of the research literature. . . . (in the case of Harrow’s study, he makes) the classic error of confusing correlation with causality.”
- “There is no real evidence that (drug induced dopamine hypersensitivity) is related to the return of symptoms (upon drug withdrawal.) It is just Bob’s unproven and in a way irrelevant theory.”
- “Bob’s stubborn insistence on blaming meds for causing psychosis also flies in the face of history and everyday common sense experience.”
- “Bob’s doctrinaire, ideological, and one sided warnings of medicine’s harms can lead to reckless risk taking.”
- “My hope is that Bob will present a more balanced and objective view in his future writings and talks.”
- My two previous blogs show why Whitaker is wrong.
- Typically, “dissatisfied patients . . . have had a disastrous experience with psychiatric medication that was prescribed in too high a dose and/or for too long and/or in odd combinations and/or for a faulty indication. They are angry for a perfectly understandable reason—meds made them worse and going off meds make them better. Their natural conclusion is that medicine is bad stuff, for everyone. And this is confirmed by the journalist Robert Whitaker’s misreading of the scientific literature, leading him to the extreme position that ‘I think that antipsychotics, on the whole, worsen long-term outcomes . . . people treated with antipsychotics, would be better off if these drugs did not exist.’ “
I think I come off as a little deranged in Frances’ descriptions, and so be it, but the last quote attributed to me caught my attention. I knew that I had never said that “people treated with antipsychotics would be better off if these drugs didn’t exist.” It’s not the type of blanket statement I ever make, and so I wrote Frances, which triggered this email exchange:
Me: Would you please tell me where you are pulling this quote from, that I said, “people treated with antipsychotic drugs, would be better off if these drugs did not exist.”
Frances: Don’t know. I will pull if you like.
Me: I am not asking you to pull it from your published piece. I am asking you to tell me where you got it from. So when I said pull it, I am asking you to tell me where you got it from. You wrote it and so it should stay part of the piece.
Frances: Sorry for screw up, Bob. Didn’t mean to misquote you. Reconstructing it, I started doing this as a shared piece with someone else, who then got too busy and had to drop out. It was in his section and I included it in the final without checking accuracy. My bad. Probably best if I just ask to have it deleted. What do you think. Sorry for inconvenience.
Now I guess I could be upset by this. Many people might find it more than an “inconvenience” when the head of the DSM-IV task force puts words into your mouth to make you look extreme, without any real concern of whether it was true, and then, when asked about it, apologizes for the “inconvenience.” I am not sure if he and his colleagues would find it an inconvenience if I had done the reverse. But then I figured it was all of a piece, and that if the blogs by Pies and Frances gave us an opportunity to watch their minds at work, and we had the opportunity to see their embrace of the China study, while simultaneously dismissing the Harrow study, then this making up of a quote, and shrugging it off as an inconvenience, was just one more little tidbit of information for us mind-watchers to mull over as we contemplate the authority that this profession, with their diagnoses and drug treatments, has over our lives.
A Case Study in Cognitive Dissonance
The writings of Pies and his colleagues, I believe, provide a compelling case study of cognitive dissonance. Cognitive dissonance arises when people are presented with information that creates conflicted psychological states, challenging some belief they hold dear, and people typically resolve dissonant states by sifting through information in ways that protect their self-esteem and their financial interests. It is easy to see that process operating here.
Harrow and Wunderink belie the conventional belief that antipsychotics are an essential long-term treatment for schizophrenia and other psychotic disorders. As such, these studies are bound to provoke conflicted feelings in those who hold such beliefs. In order to resolve that psychological conflict, Pies and his colleagues need to dismiss these studies, and so their minds reach for the “correlation doesn’t equal causation” refrain, which allows them an easy way to do that. Similarly, by focusing on an MRI study that found drug-induced brain shrinkage to be associated with better scores on a cognitive test, they can put aside other MRI research that found that changes in brain volumes were associated with a worsening of symptoms and functional impairment. And so on. Seeing the drug-withdrawal studies as measuring the return of the illness, rather than as research confounded by withdrawal symptoms, allows them to conclude that their protocols are “evidence-based.” The Chinese longitudinal study helps them believe that too — even if it requires ignoring the details of the study. Finally, another regular feature of cognitive dissonance is to see the critic as biased, or uninformed in some way, and voila, here I am, cast in that role.
Indeed, in this review of the “mind of evidence-based psychiatry,” we can see all of the elements of cognitive dissonance at work. Pies and Frances reviewed the evidence in ways that allowed them to remain comfortable with their medicating practices and their professional sense of self. Unfortunately, what we don’t see is a curiosity and openness of mind about findings that challenge their medicating practices, and what we don’t see is a desire to plumb the scientific literature to figure out how to improve treatment protocols. And what that means is that psychiatry, as an institution, isn’t capable of adopting evidence-based-practices. The information on psychiatric drugs that is to be found in the research literature is simply too threatening to psychiatry, and it provokes what I like to think of as an institutional cognitive dissonance. When that happens, the institution is going to sort through the scientific literature in ways that protects its power, its prestige, and its products in the marketplace.
Which leads to a challenge for us as a society: How can we yank power from a medical discipline that resides within such a dissonant state, and yet has such an impact on our lives?
* * * * *
Robert Whitaker Britain’s Parliament















“Unfortunately, what we don’t see is a curiosity and openness of mind about findings that challenge their medicating practices…”
Yes, I’d say the same thing, that there is a lack of curiosity and open-mindedness to that which challenges their perception and reality. I’d call that ‘resistance to the truth.” It is extremely stubborn, to the point of madness, I’d say.
I’ve had all sorts of projections thrown at me, misinterpretations insisted upon, and words put in my mouth when attempting to dialogue about my healing, and how the psych drugs made me catastrophically ill after a long time taking them, which lead to a period of disability that went on much longer than it should have thanks to that very lack of curiosity and open-mindedness. There was an equal amount of disinterest in how I healed at quantum speed when I withdrew from them, abandoned any form of mainstream ‘mental health care,’ and found my true healing path.
I’ve not had terribly good luck talking about this without resistance and backlash, as though it were all so threatening, rather than celebratory. I get it, and it makes me wonder WHY the truth is not getting out there, as it should, to save a lot of lives from needless disaster.
Report comment
It also should make people wonder that goes on in those private 1-1 “dialogues” that take place in a client session. While I know that the psych drugs are definitely a factor in why we have so much “chronic mental illness” that would more than likely (imo) not be the case otherwise, I’d also point to the quality of the dialogue between clinician and client behind closed doors. When it is laden with negative and false projections (stigma) on anyone that challenges their version truth and reality, that is highly oppressive, dangerous, and abusive to a vulnerable and trusting client who is seeking help, and often times desperately.
Report comment
The answer to your question as to why the LIES of the pseudoscience drug racket known as “biopsychiatry” are so pervasively believed, “Alex”, is, *MONEY*. Not to get all Biblical, but the Bible clearly states that “LOVE of money is the *root* of all evil”. ( II Timothy, 3:3, & 6:10, for you scholars./). So, it’s “money-love”, or GREED, and also the vanity of “professionalism”. Ego run amok. Psychopaths, sociopaths, and narcissists, all wearing white lab coats, and holding M.D. degrees as “psychiatrists”. And PhRMa. The pharmaceutical industry. Legions of drug sales Reps. A whole sick, corrupted medical infrastructure. But I’m just preaching to the choir, aren’t I, “Alex”? Like you, psych drugs did me far more harm than good. Good to see your comments here, and talk with you again, “Alex”. KEEP UP THE GOOD WORK. Helping others is also a very important part of MY healing journey. ~B.
Report comment
Thanks, Bradford, and I do agree of course, that financial interests are part of the reason for resisting what is so evidently true. I also think that there is a lot of fear of judgment (and self-judgment) were they to themselves to awaken to these hard truths. I have compassion for that, we all wake up to hard truths in order to grow, and sometimes they can be real doozies. But that’s exactly how we evolve in consciousness, and it is a must if we are to heal this sick society.
Still, my question about why the truth isn’t getting out there is more about what I’m starting to feel are corrupt lines of communication, so to speak. It’s like speaking on the telephone but all you can hear is static, no clear words, nor even the tone of a person’s voice, just random electrical energy.
So there is defensiveness, accusations, judgment, name-calling, ridicule, and denial. These are examples of dialogue? The entire mental health profession is based on two things: drugs and dialogue. Seems they are both now toxic. Sheesh.
Report comment
Yeah, this is a downer. It is all so threatening, rather than celebratory, as you say. Does Pies actually treat patients? If he does, I can see him telling them not to be so foolish as to believe that they can taper off their medication and stay well. Better to be medicated, your whole life long. This doesn’t even sound like what a “normal” doctor should say to a patient.
Report comment
And he, as others do, would write in his notes ALL the evidence of why he is right, and more than likely it is based on falsehoods and a very skewed and stigmatizing perception of the individual. Not only does this cover his ass, but obviously, he would rather be right about deeming someone chronically ill rather than so pleasantly surprised to be proven wrong, because that would be better for the individual.
When the need to be ‘right’ trumps the need for truth for the good of the client, then we have corruption as the result of utter lack of integrity.
The clinicians whom I’ve challenged with the story of my healing would always get gaslighting on me, and attempt to ‘remind’ me of my past troubles, by bringing up what had been painful experiences in my past when I had clearly moved way past that and was–and still am–perfectly in present time with myself. That’s what I’d call “the Nurse Ratchet syndrome,” and sadly, I’d say it is epidemic and, to my mind, the foundation of why this is such a disaster. It’s common, insidious, and terribly toxic and crazy-making. Go figure.
So it comes down to who wants to know the truth, and who is simply invested in ‘being right?’ Is this about the greater good or individual egos? Personally, I believe one focus is way superior to the other, that would be my judgment to own.
The reason I feel this is because when we focus on the greater good, there are no exclusions, we are invested in collective well-being; whereas needing to be right at the expense of others and ‘the truth,’ is what causes marginalization, blatant oppressive sabotaging stigma, and a whole host of myriad social ills.
Report comment
Ok, I am going to start this off with the possibly annoying point that “schizophrenia” is not a valid diagnosis, not a medical condition, and not something that can be reliably or meaningfully studied via the type of research that Whitaker is discussing above.
The discussion above assumes that some coherent, valid entity called “schizophrenia” exists, and that the effects of antipsychotics on “it” can be known… but perhaps that is not the case.
Report comment
I am going to quote here an excerpt from a much longer piece Paris Williams shared with me recently, about the limitations of quantitative linear positivist research, which is relevant to this article (of which the examples Whitaker gives would be examples):
“While there are a number of different scientific paradigms (also known as epistemologies) that have emerged in the West over the past centuries, the paradigm that has greatly dominated for several hundred years and continues to dominate today is positivism. The roots of positivism extend all the way back to the dawn of Western philosophy, with Aristotle’s emphasis on substance (matter) over pattern, and the belief that patterns or processes could be ultimately reduced to substance. The main cornerstones of positivism are “materialism,” “objectivity” and “reductionism”—these include the assumptions that all that exists can be reduced to matter or matter/energy; that we can understand the whole by isolating its parts and studying them individually; that by isolating these parts, we gain a greater understanding of the whole; that there is some absolute truth that we can observe as completely detached observers; and that it’s possible to observe this so-called objective world without influencing or biasing what we observe in any significant way.
In my opinion (and in the opinion of many others who’ve grappled with these epistemological questions), the core tenets of positivism have been soundly debunked, and done so ironically by many of the same scientific fields that have emerged directly from positivism — especially modern physics, the life sciences (especially within ecology, microbiology and evolution theory) and systems theories such as chaos theory and complexity theory. The new picture that continues to emerge is that the whole is greater than the mere sum of its parts, that process itself appears to be more fundamental than matter, and that it really isn’t possible to observe the world in any kind of unbiased and entirely non-influential manner.
The entrenchment of these positivistic tenets is especially evident when we look at our attempts to better understand subjective experiences (such as the so called mental disorders) by placing the vast majority of our attention on the brain and body rather than what is actually occurring within people’s minds, and by relying predominantly on randomized controlled trials, or RCTs, rather than on research that explores people’s actual experiences in situations that are as natural as possible. I don’t mean to completely discredit the value of controlled trials and quantitative analysis in general — I do believe that there’s a place for them as long as we don’t forget the very strict limitations of this kind of approach, especially when we’re dealing with (a) very complex systems such as living systems and organisms, which are guided by circular- and network-causality as opposed to linear causality (which is generally assumed within positivistic thinking), and (b) when we’re exploring experiences that are by their very definition subjective, which of course include those experiences that we label “mental disorder,” “mental illness” and “recovery.”
The problem is that we’re not acknowledging these limitations, and all we have to do is take a look around to see the serious trouble this is causing. We have continued in full force for over a century trying to locate the so called mental disorders within the brain, but to absolutely no avail. Just think of what we could have accomplished in these many decades and with these many billions of dollars if we had instead been putting our emphasis on trying to understand people’s actual experiences and trying to address their actual needs. Imagine how different the world would be today if rather than seeking for those “magic bullets,” we instead focused on the cultivation and implementation of support systems that we already know work very well—addressing poverty and discrimination, cultivating relationships and negotiations between individuals and groups, ensuring that everyone has access to meaningful education and activity, providing individual- and family-based interventions and empathy-based sanctuaries to those in crisis, etc.”
———-
Paris’ ideas might seem tangential, but to me they really offer an important critique of the value of the back and forth debate between Whitaker and Frances/Pies about “the value of antipsychotics in the treatment of schizophrenia.”
This debate exemplifies the malinvestment and waste of time and resources that goes into so much in American psychiatry. As Paris notes, we already know how to support people effectively without drugs. The primary reason for the debate Whitaker is wading into above is little to do with real science or attempts to help people at all. It has everything to do with the need of corporations to make money and the need of psychiatrists to continue to be seen as real doctors… which they are not!
Further, Whitaker continues to seem to naively believe that psychiatrists will get curious about his points and want to explore them and change their way of practicing. He misunderstands these people and their motivations.
Going back to the debate over the actual data itself, Whitaker and the reductionists researchers (like Pies/Frances) are interpreting these studies as if they might support some absolute position about antipsychotic drugs. But they are forgetting that the people are arbitrarily chosen, terrified/nonfunctional people, who have two out of five arbitrarily chosen behaviors, not people who have a specific disease. Thus, this is not a study of people who have a common condition. This is something that Whitaker tends to forget or overlook, over and over.
I am also going to recopy my quote of Smedslund’s critique of this type of research.
To Robert Whitaker, I encourage you to think about what this quote says about the value of the research you are discussing, and the uncertainty we should attribute to it:
““The main conclusion to be drawn from irreversibility is that empirical research in psychology… can only be seen as mapping temporarily stable statistical tendencies at the aggregate level. These mappings must be evaluated on pragmatic grounds, i.e. as yielding possibly useful knowledge in limited domains for a limited time…The regularity that is nevertheless observed cannot be taken to reflect permanent laws, but only temporarily stable feedback-loops. These are like whirls in a stream which are stable only as long as the total flow of water does not vary and the stones on the bottom maintain their positions… The findings in psychological journals may superficially appear to be of the same order as those reported in physics or chemistry and, hence, psychology may superficially look like an empirical and accumulative science. The conditional and transient nature of psychological findings is rarely acknowledged, perhaps because the publication and preservation of empirical findings will then appear unjustified since they cannot be taken to be useful in the future. The scarcity of attempted replications also allows psychologists to avoid thinking about this problem.”
This really is a powerful critique, in my opinion. It means that single studies, or even a small number of such studies in different settings, really don’t allow us to make generalized conclusions about antipsychotic drugs which would apply to other settings. That is the myth that is operating behind so much of what psychiatrists say – the notion that the studies they run are similar in kind and quality to true experiments in physics or chemistry – and it’s important to see through it.
Report comment
But there’s more.
It annoys me to see these type of phrases in here: “Medication is thought to be an essential treatment for schizophrenia.”
I’m not sure why these type of words are being used. There is no medication for schizophrenia, since there is no such disease. A medication treats a specific medical condition, as I’ve said many times. There are psychiatric drugs. Let’s get the terminology right, Robert.
Furthermore, “schizophrenia” should be in quotes. Japan and Korea already abolished that word, and there are movements in Europe and America to do away with it; for example the initiative by Van Os and the Dutch service users.
So, don’t kowtow to pseudo-doctors by using their oppressive language. Many of us here do not appreciate the uncritical use of the (unquoted) word “schizophrenia”, with all its harmful implications, nor the use of the equally inappropriate usage of the word “medications” to describe antipsychotic drugs.
I am going to keep repeating this in every article until people start to pay attention.
The word “schizophrenia” should in my opinion not be used without quotes. And people so labeled should always be called “people labeled or diagnosed with schizophrenia”, and not “schizophrenia patients” or some other stupid medical term.
One other thing, Pies was said to suggest, “the fact it wasn’t randomized provides an explanation for the results”.
How can you have a valid/scientific randomized study when an arbitrary label like “schizophrenia” is being used, not a real illness entity?
Report comment
Ok, after all the criticism, I also have some positive things to say.
I agree with Robert that Pies/Frances and biological psychiatrists in general are profoundly defensive, subject to massive cognitive distortions, and also profoundly unaware of better approaches like Open Dialogue or intensive psychotherapy for severely distressed people that can lead to much better chances at a good outcome.
Interestingly, I talked once to Martin Harrow, live (yes really), and I found out a lot about his history of working with psychotic people. It turns out he has never done intensive psychotherapy with people diagnosed as “schizophrenic”, although he has worked with a few of them once a week, but always from a disease model. So, even researchers like Harrow do not really know what they are missing. When I talked to Harrow, he kept using the words, “illness”, “disease”, “medication”, in a way that made it clear he sees things in biological and reductionist terms. The other thing I noticed is that he’s a very nice guy; but he’s simply profoundly ignorant. This is true of a lot of psychiatrists – nice, but very harmful.
I have something positive that I am doing. I am working on a .com website about “curing so-called schizophrenia” that is going to be a major F U to biological psychiatry in as much as it will brutally expose the lack of validity of the “schizophrenia” diagnosis and the lack of efficacy of antipsychotic drugs, and, hopefully, a major source of encouragement to people diagnosed psychotic and stuck in the system. It will extensively describe successful psychotherapeutic/person-centered work with psychotic people and show how this can be accomplished without drugs. It will have a massive resource section and it will all be free. And I am going to talk to a few hundred people a year, on the phone and via email, as much as I can, about a non-medical approach to psychosis and how they get help outside the system. Like I already do with people labeled “borderline.”
I can only speak to a few hundred people a year, and even though many thousands my read my website, my impact is limited. I have to trust that other psychiatric survivors and other non-medical model professionals will pick up the slack and DO SOMETHING to confront establishment psychiatry’s lies, like I am.
Oh and, MIA could always publish one of my articles. Unless there’s some arbitrary reason not to…
Report comment
I am working on a .com website about “curing so-called schizophrenia”
Your skills are much better utilized as an anti-psychiatry activist than a wannabe psychologist. Again for the millionth time treating “so-called schizophrenia” as any more valid a category than straight-up “schizophrenia” is bogus. And talking about “curing” anything is a medical model approach no matter how many quotation marks you use.
Report comment
I know that oldhead. I am using these terms deliberately and consciously, although ambivalently. Most people will never find such a site unless it uses medicalized terminology to get people in. I know how most young people think and write about these issues, since I am one. If you go on PsychCentral, PsychForums, and Reddit and look for the mental illness forums, you will see what I mean. These people in the system search on google for terms like “schizophrenia cure” and “schizophrenia recovery”, not for “antipsychiatry.”
As you know, I don’t at all believe in the validity of the term schizophrenia, nor think that cure is an appropriate word.
But framing a site with those terms in its “entrance” is a challenge to psychiatry – saying that experience they say is hopeless or intractable is, actually “curable” or transformable. It is in your face, and it rejects the status quo. Once I get people in the site, I will challenge these concepts and reframe them.
I already have successful experience doing this on my “borderline” sites. I know that it works to help people, at least some people.
I don’t think there is anything bad with being a psychologist, necessarily, by the way.
Report comment
I guess that it is a little bit of a double standard for me to be writing about these labels as I do and then criticize Whitaker for his language when he engages the “professionals”. Will have to think about that.
Report comment
Ok Oldhead, here are some forums to make you cry:
http://www.psychforums.com/schizophrenia/
http://forums.psychcentral.com/schizophrenia-psychosis/
https://www.reddit.com/r/schizophrenia/?
Just read the titles of these threads.
The number of people on these forums for all sorts of “illnesses” – “schizophrenia” and dozens of others – who mainly believe they have an illness and often are taking drugs – is FAR greater than the number of people aware of let alone contributing to discussions on Mad In America.
I am trying to find a way to engage more of these people by speaking in their language, at least at first.
They would not understand the way you talk; it would be totally alien to them to think in non psychiatric terms, at least at first.
Sometimes you have to meet people where they are to start.
Report comment
What it would take to have an impact is a cadre of MIA volunteers to penetrate these forums with enlightened “survivor” comments. One person won’t do much good, it might take some “good cop-bad cop” type approaches. I’m game to participate whenever about 5 others are too. This could be discussed on the Organizing Forum.
Report comment
Actually, psychiatrists are real doctors in the fact that they are General Practitioners. Some of the worst psychiatrists that I know are pretty damned good doctors when they work in the medical sense of doctoring. It’s their specialty that is fraudulent and false. At this point it is no specialty at all.
Report comment
The fact that in order to qualify as a psychiatrist one needs a medical degree is Exhibit A whenever a psychiatrist claims to not subscribe to the medical model. How many “anti-medical model” shrinks would publicly campaign to eliminate this requirement?
Report comment
I should be clearer Stephen, but I mean that psychiatry is not a genuine field of medicine, i.e. that psychiatrists are not practicing medicine when they make psychiatric diagnoses and give “medications”.
Report comment
“Neuroscience News”(online) has recently run several articles about how “neuropsychiatrists” are “studying” the “genetic roots”, and “genetic markers”, of so-called “schizophrenia”. They’d be better off getting linguists, sociologists, and anthropologists to study the fabrication, invention, and perpetuation of the mythical “illness” known as “schizophrenia”, or “dememntia praecox”, as it was known back when we still had practicing *PHRENOLOGISTS*…. LOL…./not.
Report comment
Is using the phrase “chronically CRAZY ” as “layman’s terms” for the individuals in the “China” study really necessary? And later using it again, rather than replacing it with “seriously ill” or “distressed” or “symptomatic” or even “psychotic”?
Otherwise, a wonderful article exposing the truly scary way these “renowned” psychiatrists “think”, or rather refuse to actually “think” and process scientific evidence. What would it take for them to actually admit how wrong they have been and continue to be if overwhelming evidence is not enough?
Report comment
This is a valid critique; Whitaker should not have said “chronically crazy”, as that is stigmatizing. Psychotic experience does not mean people are “crazy”, it means they are using maladaptive strategies to survive the best way they can, in a way that may not make sense to the rest of us, but may have been lifesaving for them (although maladaptive now).
I don’t think these psychiatrists are all renowned, btw. Perhaps Frances, but not the other three, two of whom even I, with all my obsessive reading about psychiatry, knew nothing about. Let’s not puff these people up more than they already inflate themselves. They aren’t that big.
Here are words that are more palatable to me when writing about “schizophrenia”: severely distressed, having a crisis, anomalous experience, having a breakdown, going through a transformative experience, unable to function, having hallucinations or delusions.
The above represents descriptive language that actually means something with reference to what is going on. The word “schizophrenia” is meaningless. It should at most be used to describe what other, ignorant people like Pies/Frances said to label another person (e.g. “labeled with schizophrenia.”).
Terms like “chronically crazy” should never be used. No psychotic person is continuously crazy; every psychotic person has a smaller nonpsychotic part of their mind, as Bion described. And being psychotic is never a continuous or inevitably lifelong condition, as the Dutch survivor movement which is against the word “schizophrenia” has described drawing on their own experiences as psychiatric “patients”. (see Bill George, Jim Van Os)
To Robert Whitaker: You should change the “chronically crazy” terminology in your article, because it is a problem.
Report comment
I hope I’m not on the flame list for using “schizophrenia syndrome”. On this website, I feel more comfortable with that than something like “metabolic dysperception”, which only folks like SA’s will grasp very thoroughly.
Report comment
Whitaker should not have said “chronically crazy”, as that is stigmatizing.
Disagree. (Unless your problem is with the “chronic” part.) I’d much rather be called crazy than “ill.” And I call people crazy all the time. It’s a subjective term not pretending to be scientific. And fuck stigma.
Report comment
I agree I call people crazy mofos too. What I don’t like is mainly the “chronically” part. It has the ring of the disease model and of “incurability.”
On the other hand, how one uses the word crazy is important. If someone is really having a problem dealing with their life and is having delusions and hallucinations, I don’t think that is “crazy” – at least in one sense, i.e. in that they are just trying to cope and adapt as best the can using these anomalous modes of adaptation, and thus if understood, their craziness is not so “crazy.” Just crazy from a certain perspective, from the perspective of “normality.”
Telling a friend they are crazy for making a certain decision or acting in a weird or funny way is different.
Report comment
Yeah, “oldhead” – *STUCK**FIGMA*!…. 😉
Report comment
Crazy has to be better than psychotic. We can all be crazy from time to time, just like we can all catastrophise.
Report comment
As we know, psychiatry plays fast and loose with facts and evidence. They just say and write anything to refute what you are saying, no matter if it is true or not, and no matter if they even know it is false or may be false. If you say drugs are the mainstay of American psychiatry and mental health , they will say that lots of people get therapy. If you say that people are forced into treatment and hospitals, they say NO, there are diversion programs and even name one here in NYC which has NOTHING to do with diverting people from forced Tx, but most people in the audience do not know this. If you say that many people are overmedicated and that these drugs are studied one by one, but people are taking multiple drugs at the same time and there are few/no studies, they say that they use low dose and few drugs, and that psychiatrists are well aware of all this. Complete deception and also always think they are there to dominate the conversation in an audience among survivors or interested people, and to “set everyone straight” with their blatant privilege and to answer all questions rather than the moderator answering them, and in general, being arrogant psychiatrists in charge of all thoughts, feelings and behaviors for everyone wherever these psychiatrists happen to be. With patronizing smiles and texting when they do not agree with the speaker, etc.
Report comment
Yes, I agree, this has been my experience, too. I have found mental health clinicians, in general, to be contrary, as a rule, and needing to control at all cost, not just in public, but in private client sessions, as well. It just is this way, and it boggles my mind.
I do not see how these common professional cultural characteristic of non-transparency, avoidance, lying, and ‘cherry-picking evidence’ (good and relevant phrase, thank you) is in the slightest bit copacetic with achieving truth and clarity so that people can improve their health, relationships, and their general lot in life, and to feel better!
Trying to reason and show evidence contrary to the “official” psychiatric dogma brings only defensiveness and hostility, including being hostilely snubbed, it is felt. What does that reveal about a person’s psychological state of being?
To me, this is not a personal issue, this is a professional issue. I think it’s logical, like simple math, 2+2=4. Fear-based, controlling, and defensive clinician + vulnerable trusting client = bad prognosis, more than likely getting re-traumatized..
Unfortunately it is a very common and sabotaging power dynamic that is holding everything up. How can clarity be achieved in that environment? These are spinners of mythical tales and fabricators of illusion, and they project it everywhere, when it is truth and clarity we desire and seek. Insanity.
Report comment
Hi Eileen, Alex,
Psychiatry is a very insecure medicine – it can’t afford discussion.
Report comment
It probably was a mistake to use that term, “chronically crazy.” The reason I did was that it showed that the origins of this study was that the researchers basically went into this rurarl community, and said, tell us who your “crazy” people are, as clearly they weren’t asking who had “schizophrenia.” The point is that even the “diagnostic” beginnings of this study were far from the western diagnostic construct used in Harrow, which would seemingly be of more value to American psychiatrists. I should note that this group of “untreated” people regularly worked–early in the study 88% were working, and then as they grew older, by the end of the study, it was 64%. But I see how that point is missing here, in terms of why I used that language.
Report comment
“Crazy” is not a mentalist term in my book, don’t sweat it. 🙂
Report comment
To BDP: There of course are critiques of schizophrenia as a diagnostic construct that can be made, and even mainstream psychiatric researchers don’t believe there is one “schizophrenia,” but rather a “group of schizophrenias.” But if you are going to write an article about how psychiatry as an institution weighs its “evidence,” you have to do so within their diagnostic constructs. Challenging its constructs is a whole other exercise. As I have written before, it is about engaging psychiatry on its own diagnostic terms, and accepting its own scales, and then saying, what does the evidence show. And what you see here is that even when that is done, psychiatry’s sorts through the evidence in ways that serve its guild interests, rather than in ways that might improve its treatments.
Report comment
Ok, thank you for the response Robert. Let me say, I do appreciate the work you are doing to challenge these people, and know you mean very well. Sometimes, in the zealousness of my feelings against psychiatric diagnosis, and the urgency of my desire to help people be free from the stigma of these words, I can get a little bit too critical. I will say I do think it is naïve to expect that these psychiatrist will get curious about their distortions. That does not mean I think you are a naïve person, only that I think you may be being a bit naïve in this one instance, based on your (admirable) hope that they would respond in a way that would be more hopeful. I am a cynic based on my experience in the system, and thus do not have this hope for them.
Anyway, I am not going to go into a longer response to this idea now, only to say that I wonder whether it is absolutely true that one “one has to (write an article about how psychiatry weighs its evidence) within their diagnostic constructs.” Maybe it is true, for your purposes.
But it seems to me that little progress results from these discussions of issues on psychiatry’s terms, as the slippery terminology and the illusion that real scientific/diagnostic constructs are being discussed seems to play into their hands.
Meanwhile, I think that through focusing on Open Dialogue trials and in reaching people and helping them become free from the coercive, harmful aspects psychiatric system in whatever ways we can, we may be using our energy more effectively.
I wonder what others think?
Report comment
Hey, “BPDTransformation, B.A.” – I agree with BOTH YOU, and Robert Whitaker. I do think I understand your perspective, and Robert’s too. Each of us – especially us “former mental patients” (*grin*/LOL), has our own unique viewpoint, biases, etc. It’s easy for us to want to push our own personal agenda, and lose sight of our common understandings and goals. Frances, Pies, and those other “Medical deities” aren’t EVER gonna respond to a comment from ME, but they have bent over bass-ackwards to rebut Whitaker. And thus, they lose. They expose the LIES of the pseudoscience drug racket known as “biopsychiatry”. So-called “mental illnesses” are exactly as “real” as presents from Santa Claus, but not more real. And Whitaker’s journalism is Pulitzer-worthy. I mean that…. And I always enjoy “BPDT’s” comments, too! KEEP UP THE GOOD WORK!….~B./
Report comment
Thank you for your encouragement Bradford. I agree with what you say about “mental illness”.
Of course, Pies, Frances, etc. are hardly gods (as you joked) but just profoundly ignorant, biased, professionally insecure, and sometimes greedy human beings.
Report comment
But it seems to me that little progress results from these discussions of issues on psychiatry’s terms, as the slippery terminology and the illusion that real scientific/diagnostic constructs are being discussed seems to play into their hands.
The latter is certainly a risk, however I would consider the target audience here to be those with formal scientific educations who may not recognize the fraudulent and illogical claims being made about psychiatric “research.”
Report comment
“Pies’ piece was published in the Psychiatric Times, which means that it was directed as his peers, a post designed to assure them that all was okay in the world of psychiatry, and with its use of antipsychotics.”
This very excellent critical piece being published in MIA is having the same impact as Pies piece in the Psychiatric Times – directing it to people already inclined to believe the argument. I know that Robert is trying to engage in a dialogue with the psychiatric community and the reason information like this is confined to this site is more an indictment of the psychiatric community (and frankly scientific community in general) actively denying the opportunities for debate and an open exchange of this VITAL critique.
As someone dealing with severe after-effects of discontinuing 15 years of Paxil and 6 years of xanax (only to find himself stuck back on zoloft and ativan), I get very little out of spending too much time on this site. It’s not that I don’t agree with the majority of what’s written here. It’s that without the curiosity of people in the field, it’s just preaching to the choir.
This underscores Bob’s main post here and the one earlier re: the antidepressant forum’s muted reception to his presentation. There is a genuine lack of curiosity or concern about the long-term effects of these medications. I know there is something wrong with my nervous system that is the result of being on these medications long-term. I’ve talked about it at length with the doctor I see. She tells me that I’m “an unusual case” and also agrees that there’s not much psychiatry can do for me. But there is absolutely no feeling of responsibility. And beyond just lack of curiosity, the lack of feeling of responsibility is even more distressing to me.
I’m not exactly sure what general point I’m making other than just profound disappointment that these very important debates are not really happening in an interactive forum. It just make me feel more stuck and trapped. Lack of validation is tough to take. Explaining a nervous system disruption to those who’ve never heard of it, puts one in the position of sounding like a neurotic who makes up vague symptoms for sympathy. So I don’t say anything to anyone.
We’re just too siloed off right now. We either need to find a way to bring people like Pies and Peter Kramer into this site to actively engage in a discussion (without ad hominen attacks) or find a better way to get the message – backed by the solid evidence and research Robert brings – out to the field.
Report comment
To Bob Whitaker,
I wonder if you have ever attempted to have your writings, or have had your writings, published in mainstream newspapers or magazines, and/or featured on any TV shows? And what was the result…
Report comment
Regarding psychiatrists helping patients reduce or get off the psychiatric drugs.
From my personal experience , if I said to my psychiatrist “I want to reduce the dosage” the psychiatrist would do the opposite and want to increase the dosage.
Psychiatry is not a doctor and patient relationship as they sell. It is a master and slave relationship , for there is no physical disease in the “patient”.
You can not judge yourself sane ( if you were insane you would not know it: ones confidence is so high), another person or group can judge your actions as sane or insane.
The question “How do we remove the power from a group that has dissonant cognizance?”
We can’t. There is no way to stop a religion( that isn’t a religion because we say so), a religion entrenched in law. A psychiatrist determines if someone is responsible for a crime. Did they know wrong from right? Why did they do the crime? before even a trial is heard. If there is too much evidence of guilt , they must be crazy. If the person can lie, and is lying about a crime, then it can go to court.
The lackadaisical response of Dr Frances : “Don’t know. I will pull if you like”. Is because his life is not on the line. He and the profession of psychiatry are making billions of dollars and are unstoppable.
https://en.wikipedia.org/wiki/List_of_revolutions_and_rebellions
Putting people in jail after their crime VS putting people in jail BEFORE they commit a crime.
Report comment
If only Matthew de Grood could have been put in jail before he committed his crime, everyone says.
http://www.theglobeandmail.com/news/national/calgary-man-found-not-criminally-responsible-in-stabbing-rampage/article30149179/
No one asks what was done to his brain ( by psychiatric medicine) before he lost his rational thought. “Neuroleptic-induced supersensitivity psychosis” written by Chouinard G, Jones BD, Annable L. : Am J Psychiatry. 1978
He is back on the magical medication now.The system is perfect. A perfect confidence job.
Report comment
I’ve experienced Rebound syndrome and I didnt last long. I had asked to come off my medication but after a while I was asking to go straight back on.
Coming off the medication eventually – was a slow process.
Report comment
Greg,
You are absolutely right that, in terms of having an impact, the problem here is that the audience for this critique is already of a mind to accept it, whereas Pies was speaking to an audience ready to accept his writings. Huffington Post then ran Frances’ blogs, and his incorporation of Pies’ work. I will now approach Huffington Post to see if I can publish a version of this there. Frances also blogs on Psychology Today, and I used to have a blog there, and so I may resurrect it there. But that’s the real issue; how can this “discussion” move into the general public arena?
Report comment
If you can syndicate your posts by making them simultaneously on multiple platforms like MIA, HuffPo, PsychologyToday, and other Webzines, that would be great… and other MIA authors could do the same.
Then, perhaps there would be some way for you to also get published in mainstream newspapers and/or TV shows. I don’t know anything about that. Maybe it is not possible because these outlets are scared of reprisals from their funders, the corporations.
Report comment
Please make sure MIA announces any such HP or PT pieces you may do as soon as they appear, so that people can discuss them in the comments sections in real time.
Report comment
I am so glad you will try to get this piece into places like Huffington Post and Psychology today. I think it would be so valuable for the average citizen to be able to compare the pieces back and forth.
I followed the blogs of Pies and Frances and tried to argue points and at times they seemed to be genuinely trying to listen to what responders were saying and trying to use logical arguments to back up their points. But as time passed it became too mind numbing to participate – I could clearly see what could only be described as this ‘cognitive dissonance’ you speak of, in action. Frances present studies that supported their position, and then Pies responded to points that had been made by critical studies only when they came up from commenters. A series of papers were written, each becoming more ‘sleek’ then the previous one in terms of presenting their case. Seeing that the whole discussion was initially prompted, I think, by an ‘overview of studies’ that had recently been published and that did NOT show that psychotic medications improved outcome, it was mind boggling to see the final article by Pie (in The Psychiatric Times) be given the title “Long Term use of antipsychotic treatment: Effective and often necessary with caveats” . How does “effective and often necessary “come from a review of studies that does not prove antipsychotic medication improves outcome?
Frances and Pie have both spoken about how forced treatment is either a ‘paper tiger’ that rarely happens, or that ‘consent’ is important. Yet our experience with a very trusted and prestigious hospital showed us that forced treatment happens regularly, and very quickly, and neither of these men seem to either acknowledge or speak to this issue.
The most compelling point for me is described when Whitaker writes the following:
“At the same time, what does it mean to be on the drug and to not have relapsed? If 70% of the drug-maintained patients failed to improve or worsened, with only 5% of the hospitalized patients who stayed on medications discharged, what is the state of a “non-relapsed” patient? Is a patient who sits quietly on a ward in a subdued state judged to have been “non-relapsed”? If someone is still too dysfunctional to be released, how does that qualify as a “good outcome,” e.g., non-relapsed?”
I feel like I have figuratively jumped up and down screaming about this issue, saying “what about ‘do no harm’ ” ; only to have ‘good’ psychiatrists reply “well that is how it works in medicine…you do your best judgement with what you know at the time”…..How can it possibly be in anyone’s best interest to be given medications (often without informed consent) that leaves them in such a subdued and dysfunctional state….for years!!!!!
I remember Sandra Steingard’s describing how she felt after she read Anatomy of an Epidemic, and how it caused her to rethink Psychiatry. I wonder why more psychiatrists did not have responses like that. Perhaps they have, but perhaps many of them are afraid to voice their opinions as Sandra Steingard, just like Robert Whitaker, have been viciously criticized by prominent psychiatrists in the field, when they have tried to present alternatives to the current ‘narrative’ surrounding the use of antipsychotic medications.
Report comment
They don’t want to lose their jobs and income; that’s another big factor. It’s not so hard to understand. These psychiatrists are getting $200-300k per year (or more), they drive Mercedes and BMWs, they own McMansions, their kids go to great colleges, they are respected as “expert doctors”… and to maintain this, they have to kowtow to the drug companies and preach that psychotic experiences constitute real brain diseases for which “medications” provided by the drug companies are required to “treat” them.
If they gave up their profession and stopped prescribing willy-nilly, they might look forward to getting a $50,000 a year job as a therapist working with people for 60 minutes at a time rather than 15, while rarely or never giving patients drugs. Who would want to do that?
It’s not really rocket science. And it’s no mystery why these same psychiatrists do not show more interest in Mr. Whitaker’s thesis. They have hundreds of thousands of reasons not to do so.
Report comment
I also think there may be some deep shame and guilt lurking underneath this rock hard defensiveness, which would surface should they choose to once and for all to awaken to the absolute truth of their profession. After all, these are common feelings transferred directly to so many clients. Of course, that would trigger a great deal of healing for them and for society, but they’d have to own the egregious errors of their ways, first.
Report comment
And they’d have to lose income. It all comes back to money.
Report comment
I don’t know, I think shame, guilt, self-judgment, and even a perceived fear of consequences, are extremely powerful deterrents to waking up to truth. Although sure, fear of financial consequences is quite powerful in our society.
But I wouldn’t underestimate the power of repressed negative emotions as a factor in their unreasonable and extreme stubbornness. Some of these folks could retire very rich right now, and still have to live with the truth of our negative feedback. If only they were not so fearful of emotions and their own shadow! So, so ironic.
Report comment
In 1982, they reported that 30% of the 216 patients they studied had signs of “tardive psychosis.
I’m determined to read this all before drawing any conclusions, but meanwhile, is this what I think it means — that the organic brain damage known as tardive dyskinesia has been relabeled “tardive psychosis“?
Report comment
How can we yank power from a medical discipline that resides within such a dissonant state, and yet has such an impact on our lives?
Wow, such a bold sign-off for such an (on the surface) academic piece. I like it.
I’m getting used to Bob W.’s using all sorts of pseudo-medical psychiatric terms and concepts without using the quotation marks which I’m starting to realize he probably does use in his head. I understand that RW’s mission is to methodically deconstruct the conclusions of the psychiatric thought “leaders” (if you want to call them that) using their own professed logic and perspectives, and in their own language. Probably no one does this better at the moment. Still, it’s excruciating to hear all this very serious talk of outcomes, relapses, symptoms, psychoses, etc. as though we’re really talking about a health issue rather than a law enforcement/prison reform issue.
Is there a branch of scientific study which studies studies? I’m wondering if there is an officially recognized “higher authority” to which this and similar pieces by Bob and others can be presented for confirmation that these indictments of psychiatry’s research methods, and the lack of an evidence base for it’s conclusions and practices, represents a major blow to the credibility of psychiatry in general, and whether the corporate media (and progressive media) would finally be forced to report on it.
Report comment
John Ioannidis is a good researcher critiquing scientific studies.
Here is a relevant article – http://www.vox.com/2016/3/14/11219446/psychology-replication-crisis
I think it is already established that arguments like in the article above represent major threats to the credibility of establishment biological psychiatry’s narrative. Maybe I am biased.
Report comment
Phil Hickey’s pretty good.
Report comment
Oldhead,
The terms tardive dyskinesia and tardive psychosis are linked, in a way, but separate. Tardive dyskinesia, of course, is the appearance of motor disabilities that regularly don’t disappear in adults even after withdrawal of the drug. The thought with tardive dyskinesia is that, after time, the drugs have permanently damaged the basal ganglia part of the brain, which is a region dependent upon dopamine neurons. I should note that tardive dyskinesia is also associated with cognitive decline, functional decline, etc. It’s not just a “motor” disability.
The thought with tardive psychosis is that antipsychotics, over time, lead to a more permanent dysfunction in the limbic area of the brain, which–within the “disease” model of schizophrenia/psychosis–is thought to be a mediator of psychosis. Thus, the thought that dysfunction in this area of the brain, which is also a region dependent upon dopamine neurons, will often lead to later onset (e.g. tardive) psychosis.
So tardive dyskinesia is thought to arise from drug-caused damaged to the basal ganglia; tardive psychosis is thought to arise from drug-caused damage to the limbic system.
Report comment
They may not be so permanently damaged. Many of those with dyskinesia can be successfully treated with manganese and/or niacin.
Report comment
Yes, anything can heal and there is no permanent damage. If anything, there is transformation into wholeness. I wish they would stop making up these things that spell d-o-o-m to people. This is a bottomless pit of fabrication and illusions which only serves to bring humanity to states of fear and despair, or deepen them.
Report comment
This is a bunch of New age claptrap and very irresponsible. Yeah, sometimes people with nails in their brains heal too, that doesn’t mean it’s likely, and to suggest it’s just a matter of will power or using holistic treatment is bs. Ever seen anyone with tardive dyskinesia?
Report comment
Your judgment and projections aside, it’s the truth. It has to be discovered on one’s own, which will not happen with fatalistic thinking. I did not say in my comment how to focus that healing, so you’re putting words in my mouth. It requires a flexibility in perspective and consciousness.
Report comment
Maybe some people find healing from this but when I worked in a nursing home/retirement center there were a number of people who were permanently disabled both physically and cognitively by the tardive dyskinesia that was the end result of the so-called “antipsychotics”. I suspect that it all hinges on how long a person takes the damned things. I think younger people see some or total reversal but older people have a much greater difficulty in bouncing back from these kinds of things, especially if they’d been on them for a long time. But, don’t quote me since this is only anecdotal evidence that I’m working from here, and I’m not a doctor.
Report comment
It’s true that the older we get, the more challenging it can be to heal, and I believe that’s mainly because we are more entrenched in our habits of thought and beliefs. A younger person has more flexibility here, they are still experimenting with life, so what they grew up learning is not as deeply embedded. Life is more fresh and their minds are more malleable, so learning new things and shifting perspectives comes more easily the younger we are.
That’s the secret to self-healing and solving complex issues, from what I have learned and experienced–being flexible, creative, open to learning new things, and allowing different perspectives to be considered in order to allow new ideas and realities to emerge above and beyond what is presently even conceivable. That’s the process of exploration and discovery in life, and how new things are created.
Still, regardless of age, some people are naturally very flexible and fluid in their thinking, while others have grown more rigid. The older we get, the more rigid we tend to be in our thinking, because our lives have shown us the evidence of our beliefs over and over again, and it is our beliefs and chronic thoughts which dictate our focus, from habit.
It’s certainly possible, however, for an older person to be very flexible in their thinking, which, to me, translates to humble living, and therefore they more easily allow themselves to consider new perspectives. That would be to their benefit, because people who are flexible in their thinking tend to be more creative, and therefore, are more than likely to be able to create solutions for themselves for anything that is a problem for them, including health issues which some might deem as ‘permanent disability,’ rather than wait for someone else to do it for them. Were we to wait for solutions from the mental health field, we will wait a very long time, since from here, what we get are the problems.
Solutions are found in flexibility and creativity, and this can transcend age.
Report comment
Alex: If you’ll notice my response was not directed specifically to you, there’s another button for that, so let’s ease off on the “words in my mouth” stuff. I’m trying hard to not provoke or even engage with you but this is offensive to anyone who has had to deal with tardive dyskinesia.
Anyone know a TD victim who has been cured to address this? 🙁
Report comment
How on earth can providing hope for a cure for anything be offensive? That makes no sense to me. There was a time when many things were thought to be chronic and terminal that is no longer the case. How about we raise the bar and let in some hope, and some space for exploring and discovering new things.
Personally, I find that being adamant that ‘there is no cure’ about ANYTHING is far and away more damning and hopeless–and therefore, offensive–than anything I’m proclaiming here. But that’s just my opinion, and I’ll stand by that, regardless of what others think. After all, we just don’t know about the future in any respect.
Report comment
The reason I started posting here is because I was one of the ones told that I’d never heal and live a normal life, and dang if the psychiatrist who adamantly insisted that I “face reality” was wrong. And I was very ill, could barely function, or even speak for a while my body was so damaged from psych drugs.
Turns out the psychiatrist was the one with who would have been better served facing the reality that he was not only wrong, he actually took away my hope at one point, which I believe is very dangerous for people.
Fortunately, I found hope again, along with my real and true healing path, by investigating my options outside of psychiatry. I worked hard to heal and got on with things, and ended up establishing myself as an actor, filmmaker, teacher, and now, musician, living the life I enjoy now.
I’m happy and fulfilled now, despite having been deemed ‘permanently disabled’ with ‘poor’ chance of recovery. Nothing could have been further from the truth. This is a message I like to spread around, to give hope. I also back it up. I’ve helped a lot of people heal from tough things over the years, including disabling extreme states of being. I think it’s self-sabotage to give up hope, kind of suck the life out of us when we feel hopeless. There are always new ways to look at and think about things, for the purpose of uplifting humanity and moving forward.
Report comment
Hope is important, but you seem to be saying that people continue to suffer from tardive dyskinesia because they just haven’t wished hard enough for it to go away. That’s messed up.
Report comment
Absolutely not what I’m saying, in the slightest. First of all, hope is more than important, it is essential. Without it, nothing shifts and nothing heals, and we suffer.
The healing process is multi-layered. It’s not about wishing, it’s about beliefs. I’ve talked about this before in here and others feel it rings true, but it does seem to put people off (which surprises me, so that speaks of a different mindset, I guess, to me that is GOOD news). So I’m not inclined to say too much more about that, but it’s been my education, training, and applied experience, that’s all I can go by. Apparently, it is not something well-received in here, that does baffle me, I have to say.
But for sure I’m not at all talking about “wishing something away,” that would be rather messed up. I’m talking about how our chronic thoughts and beliefs impact our bodies, perspective, and life experience. We have the choice to hold out hope and seek whatever it is that will make us feel better and evolve from wherever we are; or we can choose to believe there is no hope for healing, and focus on something else. Perhaps for some that is more acceptance, which I do feel is healthy. If that’s the case, then I’d call it the first step in healing. Again, that’s from my perspective on healing.
It really is a matter of how we choose to think, what we choose to believe, and where we choose to focus. I don’t believe in right or wrong here, but I do believe in cause-and-effect, when it comes to our beliefs and chronic thoughts, which is what dictates our energy.
All through the evolution of time, we’ve been advancing by doing things one thought impossible. And a lot of people who were ridiculed, called crazy, locked up, and even persecuted as “heretics” proved to be exactly right, and the truth is what made them targets for social abuse. Why are we insisting that healing is not possible for everyone? We can’t even entertain that notion, it’s offensive? I don’t get it.
I won’t argue with anyone who believes they are stuck with what they have going on, whatever it is, but just as a general rule, there are a lot of us in the world who think otherwise, it’s not even an issue. Perhaps that is not the case in this particular community. I’ll respect that, but we do have a choice about what to believe, and anyone can test the impact of that in their own lives.
Report comment
Uprising — It’s not you “misunderstanding” something. While it’s a no-brainer that a hopeful and positive attitude is important in any healing or quasi-healing process, organic brain damage is nothing to sneeze at. It borders on victim-blaming to suggest otherwise.
Report comment
Okay, so, to rephrase – You (Alex) seem to be saying that people continue to suffer from tardive dyskinesia because they just haven’t believed hard enough that it can go away.
While I don’t doubt your sincerity in wishing to offer hope, I feel that some of your comments in this thread minimize the impact of tardive dyskinesia – which is, after all, brain damage caused by standard-of-care psychiatric intervention and not by anyone’s personal beliefs or attitudes.
Report comment
I do understand your misgivings, and I’m afraid that I don’t have the capacity to get more into this on this website. The way you mirror this back to me is not what I’m intending, so I blame myself for my not being able to communicate clearly my intention here.
What I do know is that I’ve been practicing this for over a decade, this has been my education, training and practice. I have a perspective regarding the energy of these physical conditions that lends itself to expanding awareness around how we self-heal, which is everyone’s unique path.
I have plenty of hard evidence of all of this in my own life and in my work. I’ve worked with clients for a long time and have helped people to heal from all sorts of things that the medical community could not accomplish. I have these testimonials. I also work with people who have contacted me from reading my posts about energy healing, and they saw for themselves.
I should be happy with that, then.
Thanks for the feedback, uprising, I appreciate it. I should no longer talk about this on here, then. It’s the new paradigm–of that I’m certain, I’ve been doing this for a long time–which does require some rethinking of language and perspectives, but I can’t seem to say what I mean, apparently! I’ll work on it, for when that time comes around again.
Report comment
Yes, “oldhead”, I saw somebody with tardive dyskinesia every time I looked in the mirror. My case was early-onset, primarily manifesting as uncontrollable twitching of my left eyelid, and face. (BTW, over 2 decades later, I had left-side Bell’s Palsy – can’t say for SURE that it’s directly related, *BUT*….). At the time, I was being given Triavil 4/25’s, 3x day, by a quack shrink named Dr. Louise K. Dierker, who later had her medical license revoked by the State…. The TD cause me to abruptly terminate the drugs, which resulted in a near-fatal toxic withdrawal reaction. Yeah, I KNOW what I’m talking about, because I LIVED it, too. As have MANY of us here at MiA…. Healing and recovery ARE POSSIBLE….
Report comment
Bradford, thank you so much for offering your testimonial, and congratulations!! Obviously, your voice is needed here, and in the world. Bravo.
Report comment
Oldhead never said that healing and recovery are impossible. What I think he objected to – and what I object to – are statements like this:
“Yes, anything can heal and there is no permanent damage.”
This is nonsense. (What about someone who has lost a limb?) As I said earlier, statements like this minimize the damage caused by psychiatry. And I say this as someone who used to have twitches in my left eye and cheek.
Report comment
What is nonsense to you or anyone can be truth to me or others. That’s what I mean by ‘two divergent realities co-existing together.’ Again, we have choices about what to believe, and I know with certainty that which choice we make will impact our realities accordingly. You are simply making a judgment, and that is your personal choice.
Report comment
Also, uprising, what I say about healing has nothing to do with the impact of psychiatric abuse and malpractice. Those are two different issues. Like so many others, I was also horrendously injured in multiple ways by psychiatry that I was led to believe would never heal. I challenged those beliefs, and I won the challenge.
Why so argumentative? This could be a neutral, interesting, and perhaps enlightening discussion that could help others, were it not for all the personal slurs. I empathize with Bob when he attempts to dialogue with the psychiatric suits. Key words: open-mindedness and curiosity.
Report comment
Perhaps you can tell me how the statement, “Anything can heal and there is no permanent damage,” might apply to someone who has lost a limb. And please, no more passive-aggressive remarks about how some people just can’t see things from your “enlightened” point of view.
Report comment
As far as I know, I never, ever said anything about my ‘enlightened’ point of view. I truly believe everyone is enlightened, and everyone’s perspective is to be honored and respected. Dialogue can help us to grow and learn more, from divergent perspectives, but how am I supposed to have a neutral dialogue about important with this kind of energy coming at me? As far as I know, I’ve been extremely direct, where was I passive aggressive?
Again, we are in two different realities with divergent interpretations of words and meanings. That makes this particularly challenging.
Re growing a new limb, absolutely this is possible, as cells naturally regenerate. What stops this natural self-healing and self-regeneration process is our cynicism, doubt, and fears. There is tons more to say about this, to fill in the blanks about how this process works, but this is not the place for it. However I have taught classes in how this works.
I don’t know whether or not this will satisfy you, and I don’t mind being challenged. But can you please be a bit more neutral and open about it, if you really are after clarity? I’m not looking for a fight. I’ve had enough of that in the system.
This is about clarity and solutions, and getting personal and angry because you don’t like what I’m saying is more on you than on me, as far as clarity goes. Clarity and real true progress toward change would require a clearing of static like this. That’s just a fact.
Report comment
And what personal slur? Disagreeing with something you wrote does not constitute a personal slur.
Report comment
Okay, good. If you teach a class on human limb regeneration via the power of positive thinking, then it should be easy for you to provide proof that this is possible.
Report comment
No, you would have to prove that it is IMpossible. Others of us will be busy regenerating our cells on a daily basis. In the meantime, you are trying to prove that full healing is not possible, and I don’t get how that is helpful to anyone.
I’ll forgo the ‘personal slurs’ debate. I think what I say above is far more significant.
Report comment
Sorry, that’s not how this works. If you are the one making a claim, then you have to provide the proof. You are claiming that you teach people to regrow limbs. Surely you must have tons of evidence if this is successful. It should be easy for you to prove.
Report comment
Maybe that’s not how it works in your reality, but that’s exactly how it works in mine. I told you, we are coming from completely different perspectives. From my perspective, we create our realities. I know that is horrendous for some people to hear on here, but that is my full-bodies truth. And I’m not alone. There is a lot on the internet to explore about this, expanding consciousness. ‘Nuff said about that, here.
I said I teach how our negative emotions and cynical beliefs undermine our natural healing capacities. I’ve done workshops in several different agencies in a couple of different cities, including Dept of Health & Human Services in my county, to clinicians and clients of the mental health system, and they were well received. What you are asking me to ‘prove’ is covered in these workshops.
You get me a nice big grant and set me up, and I’ll be happy to put that money where my mouth is. I’m confident about what I teach. Shouldn’t I be? Or should I be insecure about it an full of doubts. I don’t think so!
Report comment
Oh, and the reason I’d hold out for $$ this time is because I was doing all of this pretty much as a volunteer (although I did get paid for a couple of gigs). But most of my work in this arena has been as a volunteer. And I’ve regretted it, because it is SO DRAINING to go into the mental health arena. I do my music voluntarily as community service, happily, because those people are grateful. But the politics of the mental health world is overwhelming. There is no room for healing here. I’d have to be well paid to back into that pool of sharks. But for the right price, I’d do it, if you really want to know how to grow a new limb!
Report comment
Sorry about all the typos, btw. Typing fast, and adrenaline is going. Been enjoying this, thanks uprising. Lots of juice on this I feel.
Report comment
Actually what you seem to be describing are known as “pseudo-parkinsonian” symptoms which do tend to go away when the drug involved (generally a phenothiazine) is withdrawn.
Btw I never said that people never ever recover. What I’m objecting to is the implication that people who don’t heal are responsible for their condition. If we were to take this logic to its extreme there’s no reason for any of us to even involved with MIA, since if we only would stop complaining and attain the proper enlightened mental attitude (for a small fee) all these seemingly real, material, objective struggles we are involved with here would all magically disappear. Poof.
Report comment
(For Ragnarok)
it seems to me like TD is something like the myelin sheath in our brain nerves being frayed so the nerves kind of ‘short-circuit’ sometimes
Maybe…I think in the post by Bob Whitaker that started this all the damage is to the basal ganglia.
Report comment
I’m not implying, I’ll be totally direct about it—people—adults, specifically–are responsible for their own health and well-being, regardless of any condition or how it came to be. Who else would be responsible for it? I don’t expect anyone to be responsible for my health, other than myself.
Even the temporarily debilitating conditions which were the result of psychiatric malpractice and social injustice were, in the end, mine to deal with. Only by taking full responsibility for my health and life was I able to turn it around and live the life that I most enjoy now, with excellent health and pure freedom. That took some doing, but it did not happen by my going around judging everything I did not understand or berating that which did not sit well with me. I was very open to facing hard truths, and I took fruitful action.
I know a lot of people who take responsibility vs. those who sit in blame and resentment, and it is easy to pick out and discern who is whom by who is more relaxed, centered, grounded, and enjoying life. Not everyone who has been traumatized by life and who lives with chronic pain–whether emotional or physical–is angry, resentful, and bitter. That can change, and, indeed, when it does, we become healthier, clearer, and create better things for ourselves. I don’t see how it can be any other way.
And no, it’s not magic and it does not happen overnight, it’s hard work and it takes time, patience, diligence, and focus. It’s a choice what we believe and what actions we take. From whatever we put out, it comes back to us, one way or another. I don’t think that’s such a stretch.
And, you’re right, I think if we each took responsibility for our own lives and stopped trying to be saviors for others, and let each of us choose how to direct our lives best we know how and to be the best people we can be at any given moment, including flawed shadowy human and all, then, indeed, there would be no need to be “mad” in America. I’d prefer “healing” in America, but that’s just my own personal opinion.
No charge.
Report comment
And I’m not implying that anger is a bad thing, I understand being angry about all of this, and it was an important step in the process, allowing myself to be angry, and to express it.
But I found that after a while, it became exhausting to be chronically angry, and it did not help my situation too much after a while. In fact, I think when we hold on to anger for too long, it becomes self-sabotaging. At some point, I think it’s sound to get past the anger, and start looking at things from a different perspective. Again, that’s my personal experience. Perhaps others feel better in the anger, that’s not for me to say or judge. If that is the case, then I imagine there is a reason for the anger at that point in time.
Like I said, though, eventually, I found that hanging on to the anger and resentment only served to wear me out, keep me stressed, and at least bordering on being only sabotaging, and keeping things stuck.
I think change best happens when we open up–like lowering the dam so the water can finally flow through. Chronic anger dams up energy. That can even be felt in our bodies, it’s not healthful.
Report comment
And olhdead, no this is not victim-blaming, it is victim-empowering. Indeed, that might seem to be a subtle distinction, but I know for a fact there is a huge difference in the outcomes and prognosis for well-being.
Report comment
Also, to answer your first question, have I ever seen anyone with td? I did work in the heart of the mental health system social services in San Francisco for years, so indeed I have. I saw just about everything. I was social worker at the time, so I was not acting as a healer or teacher, that came later.
But I had clients with all sorts of issues whom I helped and matched with jobs that they enjoyed, which they actually desired. A couple of them had been deemed ‘unemployable’ (for what I knew were stupid reasons, it was all so personal).
I’ve been extremely successful in working with helping people, when I was in the system, and even now working for myself, off the grid. No one has ever doubted my empathy, or has accused me of blaming them for their plight. Were that the case, I would not be successful at what I do, and I have been since I started.
I didn’t blame myself, either, when I was a victim of the system, I learned what all this was about and I know there is plenty of victimizing going on. But I did take full responsibility for where to take it from there, and I got myself out of that quagmire, first, by having an open mind about my healing, and second, by asserting myself with the corrupt powers that be.
I took it upon myself to file a law suit, I took it upon myself to make film calling out the system, and I took it upon myself to get myself hardily trained and certified in what I knew was effective. That took years and I did several internships and intensive trainings.
All this while on disability in an exorbitant city like San Francisco. I didn’t know how I was going to do it, nor did I sit around and think about how I can’t because of this or that. I just walked forward and expressed my needs, which were finally met by healers, because it had nothing to do with ‘mental health.’
I just made my second film, which is not about any of this, but still about healing, through music, for residents of an assisted living center, to uplift them. They swooned over the experience, their joy lasted for days after the screening.
I do my best to contribute to the world best I know how with what I have, which is not much, in terms of resources. I hardly make a dime doing it. Still, my needs are well met and I am abundantly rewarded in life, with fulfillment in the knowledge that my healing journey can have meaning for others. I am by no means privileged, I was drained by the system. But I am very creative and have a fertile imagination, so I lack for nothing.
I have plenty of compassion and empathy, but I do not feel sorry for people, that would only be patronizing and defeating. I like for people to feel their power to heal and to create. If that makes people angry, I’ll accept that, but it begs many questions. To me, that would be some kind of block. I dunno, it’s interesting, but this does have me scratching my head a bit.
Something to sit with and think about…
Report comment
This is my last response, I’ve been trying hard to take people’s advice and not engage you but you seem to want to belabor this. Still waiting for those cured TD victims to come forth. As for the rest I don’t see how it’s relevant.
Report comment
Point being, if you believe something is impossible, you are limiting yourself before even trying, which is self-defeating. Whereas when you are, as Bob so aptly put it “curious and open-minded,” than all sorts of possibilities you never dreamed of will come to light. That has happened all throughout history. It is also logical.
Naysayers are limited because they believe in the limitations. Those with fertile imaginations and open minds are the pioneers, because they know they can manifest anything, including good health & wellness. And lots, lots more…
Report comment
I didn’t read all the text in these comments (yeah I know, me who writes essays as a response didn’t read others responses, but meh, I’ve had a few drinks), I’d like to leave my own two cents.
While I personally have not been officially diagnosed with TD I’m fairly sure I have atleast a mild to moderate form of it (twitches/spasms in face, neck, back, legs, and right hand). And yes, I took anti-psychotics, aswell as anti-depressants and several others in my teenage years. That drug cocktail also resulted in long term seizures (sooooo not fun for anyone that’s never had one).
Anyways, I’m by no means an expert on TD, but to my understanding TD is something that affects the physical brain. Depression, PTSD, DID, etc, are mental, meaning they affect the mind. Sure these experiences can alter the brain after a long time, but they are initially and primarily mental. TD however seems physical.
To put this in metaphorical terms, say you wanted to do the high jump (track and field stuffs). Depression for example may make you feel like you aren’t good enough or anxiety may make you anxious of performing in front of people, but with enough belief in yourself you could do it (with a bit of practice of course). TD however is like being in a wheelchair and wanting to do the high jump. No matter how much belief you have you still have physical inadequacies. So while mental issues you may be able to overcome with belief and practice and help and whatnot, certain physical issues are not so easily (if at all) overcome.
Someone that is far more knowledgeable about TD correct me if I’m wrong, but it seems to me like TD is something like the myelin sheath in our brain nerves being frayed so the nerves kind of ‘short-circuit’ sometimes. Consider a power cable that has the wiring inside and the plastic/rubber coating on the outside. If you remove that outer coating then the inner wiring is exposed and can get disrupted or short circuit or something similar. How do you fix that? I’m not an electrician, but apart from replacing the cable maybe you could pour plastic/rubber over the exposed wiring to try to ‘fix’ the damage. Maybe this would work, maybe it wouldn’t. But how would you be able to fix an exposed ‘power cable’ inside your brain? You can’t. You might be able to improve your diet, or exercise more, or believe anything is possible like the Little Engine That Could, but surely there’s a limit to how much you can improve considering the physical nature of the damage.
Although I hate saying it because I personally experience and am stuck with this, I’m not saying that TD is something that can never be improved in any way, but I am saying that due to the physical nature of the damage that there surely is a limit to how much the condition can be improved.
Report comment
It’s also fine to take the advice. My comments are my truth, and which I, and some, feel are relevant. Doesn’t have to be everyone, nor does it have to be the majority or even anyone, really. We all have our unique perspectives.
When someone responds to me, then I respond back if there is a question or a challenge, or something I particularly agree with emphatically. You do have a choice whether or not to dialogue with me.
None of this is personal to me, it is all information for the purpose of clarity relevant to these issues, for creating much needed change. I lived the journey in living color, so I have every right to express my truth here. Much of it overlaps with the majority who post here, and some of it is my unique perspective. That’s not so far-fetched.
I have nothing personal going on with anyone here. This is about collective well-being, as far as I’m concerned, way far and above anything personal or eg0-related. I get that my truth makes you angry, but I can’t help that! I can be passionate about my beliefs, but ‘m not even nearly attacking you nor anyone, not even close.
We have two different realities going on, great example of ‘diversity.’
Report comment
Ragnarok, this is the key, what you say here:
“I’m not saying that TD is something that can never be improved in any way,”
That would be the belief to follow. It is one step at a time. Start with taking steps to improve it, and don’t look past that, stay in present time with the belief that you are taking steps to improve, and then mark the improvement. That will shift your energy automatically, and changes will begin to occur, inside and outside your body, because you are going toward feeling relief. See what happens, but don’t try to predict the future. Just stick with the belief that you can, indeed, improve, and start asking yourself “how?” then see how you are inspired, then go for it.
When you say this,
“but I am saying that due to the physical nature of the damage that there surely is a limit to how much the condition can be improved,”
then you are kind of setting yourself up for limitation, because maybe that is true and maybe it is not. Anyone can be the first to heal from something deemed un-healable. At the initial stages of healing, we just don’t know what to expect, the healing process is a bit mystical, there are unknowns at play.
But if you can keep your focus on “I know this can at least improve,” without any doubt, then you have embarked on your healing journey. Embrace the unknown and go simply toward FEELING BETTER, and see what happens.
Report comment
Also, in general, detaching from what other people think is always a way to feel much better about any situation, that brings tons of relief. Then, we can simply focus on our truth, and our inner guidance, which is exactly how we discover our true selves and the paths we intend for ourselves.
This is all about self-healing, we really do have quite a bit of untapped power there. To me, were we to foster this diligently, that would put most traditional western medicine out of business–at least the corrupt part of it, which I guess may be most of it, I don’t know. Hard to tell what is going on in all that smoke-screening, but I do know we have the power to focus our own healing when we detach from outside opinions about the trajectory of our own lives.
Report comment
Oh, and speaking of Psychiatric Times, has anyone seen their current “Diagnostic Championship” contest? (This is not satire):
“How much do you really know about mental health disorders? Can you choose the most appropriate treatment given limited information and time? Then face-off against your peers and test your skills in a battle for diagnostic supremacy! For the next five weeks, Psychiatric Times presents the “Diagnostic Champions Challenge.” Each week will feature a set of multiple choice clinical dilemmas to test your diagnostic and therapeutic acumen… The top scorer of the finalist round for the MD and non-MD track will be recognized as the champion!”
To “play” go to http://games.psychiatrictimes.com/
Report comment
Haha that is unbelievable. Thanks!
Report comment
It’s funny that in Round 1 the psychiatrists/physicians were beaten by the laypeople!
http://games.psychiatrictimes.com/leaderboard/198
Report comment
The defense against the very uncomfortable experience of cognitive dissonance is clearly seated in the principles of pseudoscience:
1 – Hostile to criticism, rather than embracing criticism as a mechanism of self-correction
2 – Works backward from desired results through motivated reasoning
3 – Cherry picks evidence
4 – Relies on low grade evidence when it supports their belief, but will dismiss rigorous evidence if it is inconvenient.
5 – Core principles untested or unproven, often based on single case or anecdote.
6 – Utilizes vague, imprecise, or ambiguous terminology, often to mimic technical jargon.
7 – Has the trappings of science, but lacks the true methods of science.
8 – Invokes conspiracy arguments to explain lack of mainstream acceptance.
9 – Lacks caution and humility by making grandiose claims from flimsy evidence
10 – Practitioners often lack proper training and present that as a virtue as it makes them more ‘open’
Pies and Frances are only the most public psychiatric apologists, but those standing on the highest ramparts will be the last to see the tide washing the psychiatry sandcastle away.
Report comment
If this were a court case, methinks the jury would find defendants Pies and Frances guilty on all counts!
Report comment
This is what I wrote when I first read Pies’ piece in the Psychiatric Times in February…I didn’t send it because I knew Robert would write something.
“Dr Pies: “I would argue that interpreting these complex studies requires an in-depth understanding of medical research design, psychopharmacology, and the numerous confounds that can affect treatment outcome. Unfortunately, a lack of medical training has not stopped a few critics from confidently charging that psychiatrists are harming their patients by prescribing long-term AP treatment.”
Surely you’re not suggesting, Dr Pies, that people without medical training do not have an understanding of research design, psychopharmacology and confounds. Research design is a major part and dare I say, proportionately greater percentage of many disciplines other than traditional medicine. Also there are many critics of long term psychiatric drug use who are highly medically trained, e.g. Dr Peter Goetzsche founder of the Nordic Cochrane Collaboration (quoted below but ascribed to Robert Whitaker), Dr Joanna Moncrieff, Dr Pat Bracken, Dr Terry Lynch, Dr Peter Breggin, Dr David Healy, Dr. Marcia Angell, among many, and increasingly, more.
Then there is a large group of highly scientifically trained researchers who might be surprised to be told that their observations are inadequate because they have not qualified as medical doctors. I’m not sure but appears to be a tiny whiff of a suggestion that there is a conspiracy by these inadequate critics to undermine psychiatry?
– And perhaps it is bit disingenuous to suggest that if a person gets well without antipsychotic medication they didn’t have the disease? Here you appear to take as read that schizophrenia is a discrete and `very chronic illness’ and therefore if people recover, it can’t be schizophrenia. Given that current diagnostic constructs fail to reach even minimal scientific reliability levels, is it really possible to make such a claim? This might question the validity of the use of antipsychotics, not only in the long term, but at all.
– Whilst you have given us an extremely detailed analysis of the Harrow, Wunderink and Sohler studies, we don’t seem to have a similarly rigorous examination of the studies from China and India. Perhaps at another time.
I’d like to take issue with your emphasis that the Sohler study found that while, `these data were also inadequate to conclusively evaluate whether long-term antipsychotic medication treatment results in better outcomes on average’;…The authors explicitly state, “Our study did not support the hypothesis that long-term treatment with antipsychotic medication causes harm.”
First, even if the were no evidence of physiological damage caused by along term AP use, and that `schizophrenic’ symptoms are not made worse, we have to consider whether it is harmful to spend year after year taking drugs that provide little or no benefit, have a plethora of, at best, uncomfortable, at worst, debilitating, isolating and potentially deadly side effects such as Tardive Dyskinesia, chronic akathesia, emotional and intellectual dulling, obesity, diabetes and death 20-25 years earlier than the population average. Is is `harmful’ to be a marginalised welfare `patient’, stigmatised, hopeless, depressed and socially disadvantaged for life, with no hope of recovery and no help from the `so-called’ treatment? In any illness, particularly a `mental illness’ surely the psychological effects of the medications are least as important as the physiological effects.
– Could we also have definition of `outcomes’? This seems to be assessed by psychiatrists as a reduction of symptoms, a clear illustration of the medical model at work. However for the person, an acceptable outcome might be the ability to work, to have a family and friends, i.e. live a `normal’ life. This may be, and often is, achieved despite having often quite substantial residual and/or recurring, `symptoms’, as the Hearing Voices movement so graphically demonstrates.
– I find it interesting that you have omitted the surveys done in India, Nigeria and Colombia by WHO in the 1990s, where the recovery rate from schizophrenia was approximately 60% in those without drug treatment but 16% with it. The severity of the illness was not an issue, poverty and unavailability of medication was. It is also interesting to note that more recent surveys, where western psychiatric practices have increased, indicate that the recovery rate in these countries is declining.
– More interesting is your failure to mention programs such as Open Dialogue, the Soteria House Project and Hearing Voices. All of these initiatives involve minimal or no psychotropic drug use and all appear to have extremely good outcomes for psychosis. Open Dialogue and Soteria have been operating for over 30 years with a success rate of over 80% functional recovery rate, and whilst Hearing Voices is relatively new, its success rate for allowing people to live meaningful lives in the community is promising. None of these decry the total use of antipsychotic drugs but use them very sparingly and with the full involvement of the individual. Most only take them in the short term and many never do.
– Finally, we should remember that the public, in other words, “users of mental health services, have a strong preference for psycho-social explanations and treatments. In 24 of 25 countries where surveys have been conducted the public believes that social factors play a much greater role than genes or chemical imbalances in the etiology of mental health problems, with the only exception being the USA. Similarly, in 14 out of 15 countries the public prefers talking therapies and social support to drugs or electroshock.” (Professor John Read 2016)
The fact that a program providing psychotherapy training for psychiatrists has recently been closed down because of a lack of interest indicates that psychiatry is not in sync with what the public wants. Where more and more the evidence supports that social and psychological intervention produces the most successful outcomes for even very severe psychological distress, the constant pursuit of expensive, but to date relatively fruitless scientific activity will not sustain the medical model indefinitely. Maybe the fact the nothing genetic or organic as a cause of mental illness has surfaced after 100 years of searching suggests we should turn to Einstein, `To raise new questions, new possibilities, to regard old problems from a new angle, requires creative imagination and marks real advance in science.’
`Insanity is doing the same thing over and over again and expecting different results.’
Report comment
In my opinion “schozophrenia” is a waste of money.
The symptoms of “schizophrenia” are much the same as the symptoms of “anxiety” . And what works for anxiety also works for “schizophrenia”.
In 1980 I requested psychotherapy; and after 1984 I moved to psychotherapy and this is what worked.
Report comment
…The more I ‘think’ of my loved one’s ‘symptoms’ to be a result of severe anxiety….the more everything starts to make sense…….
Report comment
Hi Sa,
Yes, and there are solutions.
Report comment
Some very good points Dee.
Here is some more data on non-drug approaches that were successful:
http://internationalpsychoanalysis.net/wp-content/uploads/2015/04/Successful-non-neuroleptic-treatments-for-Schizophrenia.pdf
http://www.drtobywatson.com/schizophrenia.html
The bias almost bleeds from the way Pies and Frances selectively write about the issue.
And yes, it is VERY disingenuous to suggest that people who get well never had “the illness” to begin with. What bullshit. For that to be valid, a biological or genetic mechanism or group of mechanisms would have to be identified as causing a discretely, validly defined schizophrenia illness in some cases but not others. I don’t think that’s happened yet…
Report comment
They don’t know their own history. The old Moral Treatment institutions of the 1850’s were able to get 50% or so of their patients well enough to function without remissions, despite being unable to treat their neurosyphilitics and only partially able to treat their pellagrins.
Report comment
You can imagine what its like when someones terrified and they go somewhere safe where people are nice to them.
Report comment
Heaven on Earth 🙂
Report comment
Hi everyone,
In my opinion theres definitely such a thing as supersensitivity syndrome, and I think whether a person survives or not depends on having effective ways of dealing with it.
I’ve tried years of genuinely compassionate psychotherapy but what worked for me was a CBT type approach. I needed to know exactly what to do in the middle of an anxiety attack but when it was gone it – the external problem wasn’t hard to deal with.
MIND UK website suggests a person wouldn’t need to taper from depot medication – this was not my experience. I had to taper very carefully from depot medication and if I didn’t, I’d still be “sick” – so “schizophrenia” as an illness is a bit of a lottery.
Report comment
There’s not a lot of incentive to overcome ignorance when your livelihood depends on it. But they must be getting anxious because Ron Pies keeps on writing ambiguous pieces for the Psychiatric Times where he attempts to play on the bio team and the `psychosocial’ team at the same time. In doing this he treads on his own feet so often that it’s becoming clear he has a ridicule wish. His contradictions invite people like Robert Whitaker and Phil Hickey to take him apart again and again, and what gets me is that he still can’t see it! Frances also has denial down to a fine art. He decries the DSM V and its embracing of ADHD and seems to have forgotten that he almost singlehandedly INVENTED it in the DSM IV. Do these people think everyone is stupid or is it their stupidity that stops them seeing how truly stupid they look?
Report comment
It’s their grandiosity and sense of being the total “expert” that gets in the way. Their arrogance is unbelievable.
Report comment
Adamantly claiming to have more insight into a person than that person has for him-or herself, when these opinions clash, is certainly the epitome of arrogance. It’s also very dangerous, and can make the client especially vulnerable to power abuse.
Report comment
Hi Bob,
I think yanking the power from Psychiatry would mean getting across the message that there IS complete Recovery available outside of the medical system for “schizophrenia”, and that a Recovery model would save billions.
Also, that the Medical approach is one of long term illness and disability and that it probably makes society more dangerous.
And that “schizophrenia” is not an illness, but an exclusion condition.
Report comment
So am I correct in assuming that correlation coefficients were found to be statistically significant but it was blown off because it does not show causation? Okay, so what now? Numbers don’t lie. People do and only to protect their own self interests.
They are afraid that you are going to put them out of business is what they are afraid of, my father always told me “they don’t kick dead dogs”. And their bedfellows, “the pharmaceutical companies” are starting to show some pretty risky behavior in obtaining more revenue. Recently off label selling and getting fined for it for one example. I even saw something on the TV news that pregnant women have an app now to diagnosis depression. Where this is heading is scary. It’s already been shown that psychiatry tries to gather prestige of a medical doctor and shake off the label of “quack”. They have a long way to go and if they think that the pharmaceutical company will help them to find a biological marker for mental illness, that would fly in the face of their and limit the amount of consumers that the pharmaceutical companies can obtain.
Before you even read the study you have to ask a million questions before you even read it. Who sponsored it, is it ghost written, was the raw data provided, where did you find the patients, how did you qualify the patients, what were they taking before the study, when did they stop. The list goes on and on It’s exhausting and insulting to any dignified scientist who respects the scientific method.
The only way that these doctors will have their comeuppance will be when their bedfellows screw up. And the time is coming but it will not include mental patients, the suit will deal with their families. Let’s face it, mental patients are easy to disqualify in court. If you don’t believe me ask one of us about divorce or custody. Our rights are automatically taken away.
I also find it amusing that they throw in the fact that there are dissatisfied patients and how we are a thorn in their side. My question to them is “Can you show me the satisfied ones?’
Report comment
You might find a satisfied one writing for “Bipolar Burble.” Of course I think her last two brain cells are shaking hands from that funky chemical “cocktail” she religiously takes.
Report comment
Bob:
While you grabble with the intellectual debate (the macro) in the public, many of us are grabbling with how to steer the treatment team involved with the care of a loved one to a place where an honest dialogue can take place (Micro)
We in the micro world benefit when there are shifts in the macro debate but those of us in the trenches are more keenly aware of the high stakes involved.
When you feel remorse for being publicly slandered, misquoted, or economically disadvantaged because of the conflict that exists between book sales v.s scientific integrity, I hope you pause to consider that your discomfort pales in comparison to what my child is enduring: being forcibly medicated with toxins she knows are slowly killing her. This is a modern form of crucifixion which is so horrible it is beyond understanding. To chalk up the rationalization for my daughter’s torture as corporate greed and corruption misses the mark slightly. There is a patriarchal power struggle in play which I can’t completely wrap my mind around ; it has to do with the cover up of child abuse and domestic violence, as well as environmental destruction, human genocide (indigenous peoples in particular) economic instability leading to immigration. racism. living in a police state v.s individualism, etc.
This is so much deeper than an epidemic of people with ‘chemical imbalances. Your book Anatomy of an Epidemic is to the movement to change the mental health system what Rachel Carson’s book Silent Springs was to the environmental movement. Maybe not a lucrative best seller but a pivotal point in history.
Report comment
madmom,
Your experience frightens me.
Toxicity:-
from E Fuller Torrey (believe it or not)
“…..a study published in 1982 reported that when a group of patients with schizophrenia were each given 20 mg of fluphenazine, the difference between the highest and lowest blood level of the drug was 40-fold…”
Toxic Drugs can drive a person Mad:-
My suicide attempts and disablity (1980 to 1984) ended, when I stopped taking fluphenazine.
Report comment
Madmom,
Sorry to ask this in public but, and maybe you have answered it before but… do the laws of your state not allow your daughter to have any say in taking drugs or not? What about you, can you not take her home and choose what doctor she works with?
I apologize if these are obvious or offensive questions. I am outraged by this situation and hope you daughter can be extricated from it.
I am also at bpdtransformation (at) gmail (dot) com
Report comment
Looking at this from afar, my thought is that enough money will finance a competent lawyer who could find some shrinks to counter the testimony of whomever appeared in court to claim that involuntary “treatment” was needed. At a certain point it won’t be worth the hassle & expense to them. Not that I’m implying anyone has money, but I think it’s worth mentioning.
Report comment
Absolutely. I believe the only thing that will turn the tide is MONEY. If governments = tax payers, realise they paying out huge amounts of money to keep people a) in hospitals and b) on welfare, as well as forking out for the drugs and shock that CAUSE people to NEED to go on welfare, they might start asking questions. (This is already starting in the UK with the government inquiry into antidepressant use – and a small article in the Australian Medical Journal). These moves are very tentative but governments are sensitive to taxpayers asking questions. The problem of course is that politicians are beholden to donations and I suspect the APA is VERY supportive in this. Sadly, corruption breeds corruption.
Bring up the cost to the taxpayer of these screening programs as they stand now and estimate the cost of putting vastly more numbers of people on expensive drugs that will ultimately prevent them from working etc etc. I estimated on figures from 2010 in Australia that a single patient receiving ECT alone would cost the government approximately $75,000 in a single year + plus future welfare payments, and the same patient receiving no ECT, on full support for psychotherapy would cost $17,000 in a single year. Of course we have government funded universal health insurance as does the UK, but you get the idea.
I know that the insurance companies are anxious about the chronic nature of psychiatric treatment as one attempted to implement a therapy program to keep people out of hospitals, so they could benefit from a comprehensive run down of what is happening, and the rorts perpetrated by psychiatrists. (There are plenty but they’re not getting caught because neither the patient nor the insurance clerks know what is being billed.) Are they aware that they are paying far and away more costs than they need to for `illnesses that should not be chronic, lifetime sentences? Okay, they just up their premiums, but more and more people are winging it without insurance because of this.
Cutting off funding for psychiatry is the best way to stop them.
As for the legal/human rights issues, do law students do doctorates? Could a thesis involve investigating the legal/ethical/moral issues surrounding compulsory medical care? Only a very young person would attempt this as ideals disappear as incomes increase, but maybe there are still SOME revolutionaries around. Bring back the 1960s, Gay Rights, Women’s Lib, Make Love not War.
Jim Gottstein has tried, surely there are others amongst your 250 million people, our 24 million and the UKs 80(?) million, as well as the Europeans and others who value ideals more than money?
India had Ghandi, South Africa had Mandela, can we find NO ONE?
Report comment
There used to be lots of idealistic law students, now they all seem to be all about money and go into corporate law, etc. instead of human/civil rights oriented stuff. If the legal minded folks at MIA could form a caucus they could identify the most important needs in terms of fighting psychiatric oppression and perhaps do some outreach to budding lawyers, ACLU types and others. Much education needs to be done around how to cross-examine testifying shrinks.
Report comment
I’ve said it before and I’ll say it again. Psychiatrists don’t treat the insane. They are the insane.
Psychiatry is a medical profession that has no medical tests. Psychiatry diagnoses ‘mental illnesses’ base on checklists of ‘symptoms’ which are primarily emotions, behaviours, personality traits, or coping mechanisms, which are natural human characteristics not diseases. Psychiatry pushes the biological perspective of chemical imbalances, brain diseases, and genetic defects, even though there is a lack of evidence to support such claims and much evidence to actively disprove such claims. Psychiatric diagnosis is far from an exact science, where the same individual presenting with the same ‘symptoms’ could be diagnosed with different ‘disorders’ based on which country they are in or which ‘doctor’ they are seeing. Psychiatry claims psychopharmaceutical medications are ‘safe and effective’ even though studies frequently show they are little better than a sugar pill yet come with a wide range of potentially harmful adverse effects, including suicide and/or homicide. Big-Pharma also claims their drugs are ‘safe and effective’ yet time and time again it is revealed that positive drug studies have data manipulated or omitted or are ghost-written while negative studies are often failed to be published, so even though the published material gives a glowing positive review, the data produced by the corporations themselves frequently show lack of efficacy or harm, such as aggression or suicide, which they bury for blockbuster profits (Big-Harma buries the evidence and the bodies all in the name of profit).
Albert Einstein said “The Earth is the insane asylum of the universe” and the truly insane people are the ones running the insane asylum. Psychiatrists don’t treat the insane. They are the insane. And their insanity is infecting everyone else (how many people fully believe they have a ‘chemical imbalance’ or ‘brain disease’ that never existed?)
Report comment
Hey Bob,
How many times have you gone over the Harrow study and pulled it apart in front of this crowd. The next time they ask to do this, ask them to bring the raw data of the FDA drug study from the drug they prescribe most in their practice.
Somehow, I don’t think you’ll get it and it’s amazing they are not criminally or civilly liable from the side effects that some of these drugs THEY prescribe.
And yes, I agree with the previous poster. This is insane.
Report comment
There’s a lot more than Harrow, lots of people make full Recovery.
Report comment
` Hostile to criticism, rather than embracing criticism as a mechanism of self-correction.’ The first tenet of pseudioscience is also a clear indication that concern for the patient is secondary to self interest, i.e. money, status, and power. Cognitive dissonance is created by the conflict between one’s actual performance and the TRUTH. `Cognitive dissonance’ the more one invests in a belief, the more value one will place in this belief and, as a consequence, be more resistant to facts, evidence or reality that contradict this belief.
Then we have the `True-believer syndrome’, the phenomenon whereby no amount of evidence, no matter how good it is or how much there is of it, is ever going to convince the true believer to the contrary…No amount of logic can shatter a faith consciously based on a lie.”(Witness `Creationism’)
And, `Confirmation bias’ which contributes to overconfidence in personal beliefs and can maintain beliefs after the evidence for them is shown to be false. This is contrary to scientific thinking which is the search for falsifying as well as confirming evidence.
The prerequisite psychological (delete logical), profile for candidates for psychiatry must include these forms of self-deception. Of course some may come to maturity via a critical mind, and the only ways to deal with the accompanying cognitive dissonance is a) denial; b) keep quiet and take the money i.e. the psychopath’s way; c) have a breakdown/drink/take drugs; d) change your ways; e) become a reformer. The last 2 happen but are rare. See Critical Psychiatry, Peter Breggin et al, Council for Evidence Based Medicine (are they doctors).
Report comment
It’s important to sum things up. I’ll do just that; psychiatry and the “mental healthy” professions rely on money and prestige, the latter of which produces for the the former.
Whitaker has now, and often times before, proposed a question that is still unanswered;
“How can we yank power from a medical discipline that resides within such a dissonant state, and yet has such an impact on our lives?”
Stop ruminating. Stop “acting”, stop protesting and stop arguing. Start thinking.
Report comment
An interesting question is How is MIA doing financially, and does it have enough resources to continue its operations securely and do more? Hopefully Whitaker will post on that again soon.
Report comment
My impression has been that’s been settled at least for the rest of the year, right?
Report comment
Oh and Peter Breggin appeared before a Senate committee in 2010 regarding antidepressants, suicide and violence in veterans. 2010! His case was unassailable I thought, but NOTHING has changed. Instead they’ve now added ECT SHOCK to treat the suicidal effects of antidepressants! These people will do anything, sacrifice anything and anyone, lie, cheat and kill to keep their place. They have to GO.
Report comment
This has been an interesting discussion. A couple of notes in response to comments above:
Anonymous: I don’t think a statistical analysis of correlational coefficients has been done. The p values on the differences between the medicated and unmedicated patients in Harrow’s study were quite strong though . . . the differences between the two groups were huge.
Madmom: As you say, there is a macro struggle and a micro struggle, and whereas the macro one may occur at an abstract level, the micro one is where the power is really exhibited by psychiatry, and the pain, and the loss of real life is really experienced. The only reason the macro struggle has any meaning is because of what is happening to the lives of individuals. The struggle at the individual level is infinitely harder than any struggle at the macro level, and I emphasize the word “infinitely.”
As for the financial stability of MIA, I don’t think we will need to have another fundraiser this year. In addition to the earlier fundraiser we had, we have a number of readers who support us with a monthly donation, and that is a vital form of support. At the same time, I do wish we could ramp up our operations, and hire a reporter, and then we could become a publisher of steady, original journalism. It’s all part of a process of trying to grow MIA as a force for the “counternarrative” that can be found in these pages.
Report comment
It may be good later this year to consider a post discussing ideas for expanding what MIA does, which can be debated and brainstormed over by readers. The current state of income could be compared with what projected level of income would be needed to hire a reporter and add other operations. People with business / fundraising experience could offer ideas or offer their time on a volunteer basis in meeting the needed revenue – and of course, any reader even without a financial background could offer valuable ideas.
Report comment
Hire a reporter? Could you elaborate on this?
Report comment
Robert,
Pie and Frances aren’t the only ones who wish you would stop writing. I make my honour-roll 16-year-old read your pieces because they’re ESSENTIAL to a young person learning about how REAL science functions in the REAL world. Yes, he groans when I make him read them, but there was welcome comic relief in Frances’ replies to you. My teen noted with a face-palm that Frances’ replies looked exactly like his friends’ texts. All that was missing was the ‘chill, dude’.
Regarding the ‘micro/macro’ argument, it’s worth noting that the message is getting from some of us parents to a new generation. That should be heartening to those who feel this is all just preaching to the choir. We all just do what we can!
Liz Sydney
Report comment
Thank you, Mr. Whitaker, for repeating and synthesizing studies on antipsychotic medications. I heard you did a great presentation yesterday at PRA conference in Boston. Today, Kim Mueser, PhD at Boston University’s Center for Psychiatric Rehabilitation made a presentation today at PRA conference in Boston discussing some of what you presented (Harrow’s study) and focusing on NAVIGATE Program for first episode psychotic episodes. A point made was that those who went off antipsychotic medications altogether and did well not needing medications again, tended to be “higher functioning” to begin with, i.e. working, supports of family, friends, etc., then others that either sometimes took antipsychotics and sometimes stopped and then those who stayed on antipsychotics long-term. Due to sensitivity of medication side effects which we know can have serious health consequences, use of short low dosages of atypical antipsychotics for first episodes for extended period (no more than a year) is recommended, and if no symptoms then reduce maintenance dose and eventually stop. 20 percent of those diagnosed with schizophrenia have psychotic symptoms due to PTSD which complicates the process of healing. Conclusion was that not everyone should be prescribed antipsychotic medications, some do well without medications using variety of recovery-oriented interventions including psychotherapy, CBT, family support, psychoeducation and encouragement to go to work and school. Working collaboratively with our clients and their families in the Open Dialogue model of providing immediate help, shared decision-making and collaborative psychopharmacology with informed consent in a context of a caring, nurturing relationship between providers (“teams”) and those we serve is what is going to heal. Antipsychotics are still part of treatment if needed but only for short term use if that, to just alleviate symptoms enough to do the work of psychotherapy and rehabilitation. I hope that Dr. Pie and Dr. Frances get to work more in this vein of treatment and rehabilitation and collaboration with those they serve.
Report comment
To Knowledge is Power (and others):
That is encouraging to hear of Kim Mueser’s presentation at the PRA conference. It shows that the discussion is changing . . . and that the “antipsychotics for life” mantra of mainstream psychiatry is now, increasingly, not being accepted. That is a sign of a real change.
In terms of getting this discussion into the mainstream media, I have found it to be basically impossible. When I wrote Anatomy of an Epidemic, there were almost no newspaper or magazine reviews that appeared, even though this was my fourth book, and the one that did, in the Boston Globe, was written by a Harvard-affiliated doctor who likened me to an AIDS denier. I have had magazine pieces commissioned and then killed, on such topics as PSSD (post SSRI sexual dysfunction) and the failure of suicide prevention campaigns (cross-cultural data shows that, if anything, they tend to increase suicide rates.) More recently, I had a piece killed related to the recommendation by the U.S. Preventive Services Task Force to screen all American adults for depression. This one was for a major medical journal, which solicited my essay as an opinion piece, and when I wrote that there was ample evidence that universal screening would turn a number of people with ordinary, transient problems into people with chronic psychiatric difficulties, with some ending up on disability, the psychiatrists who reviewed the piece said it should be killed. Surprise, surprised.
In short, the narrative, in magazines and most other public forums, is controlled by the “experts” and the influence of pharmaceutical advertising dollars.
This is why, in the future, I would like MIA to be able to hire a reporter. We need to be able to do our own reporting on these issues, such as the Murphy Bill, forced treatment, and the media’s treatment of these issues, in order to become a journalistic outlet for this needed critique of the conventional narrative. My hope is that, with time, we will develop the financial resources to be able to do that.
Report comment
God Bless you, Mr. Whitaker….
My name is Bill, or Brad, or Bradford Hutchinson, – all the same – and I want to be known as “The Man Who Destroyed (ok, “exposed”) the Lies of the Pseudoscience Drug Racket Known as “biopsychiatry”….
Psychiatry kills. I’ve said for years, that I’m “living proof of the lies of psychiatry”…..
Over 40 years ago, I was inducted into the psychiatry-drug-game. I was told by several psychs that I would need to “be one drugs (“meds”) the rest of my life”…. I’ve been (almost) completely drug-free, and 100%SHRINK-PROOF for over 20 years now. Gee, Doc, what happened to my “lifetime mental illness”? I’ve seen proof of the lies right here in my hometown…. I can think of several folks I’ve known 30 years, who are STILL psych drug zombies, and to my eyes, they PROVE that long-term use of psych drugs ALWAYS results in worse outcomes. They are truly brain-fried psychiatric drug zombies. I’m not trying to be rude, or cruel, or “Non-PC”…. They are, or were, my FRIENDS. I’m using strong language for a reason. Weasel words, and weak words, and “PC” *KILL*. Today, in 2016, “biopsychiatry” has devolved to a PR campaign. The primary tactic used in this new “Change Direction” media blitz is known as “appeal to authority” – in this case, retired N.H. Supreme Court Justice John Broderick, who was attacked by his “mentally ill” son, who supposedly had “depression and anxiety”. (The case was heavily publicized years ago….).
I’ve seen, up close and personal, literally EVERY DAY, the failures of the whole “Community Mental Health Center” scheme. It’s a DRUG RACKET. But I already said that.
Thank-you again, Mr. Whitaker. I’ll stay in touch. And THANK-YOU ALL here on MiA….
(c)2016, Tom Clancy, Jr., *NON-fiction
Report comment
The mainstream is hopelessly corrupt, the stream is diversifying now. Best to simply create a new world, with integrity this time. Walking our talk is how desired change will occur.
Report comment
I think a reporter would be AWESOME. I also think that some on-line journals may be willing to publish stuff that WaPo and NYT and their ilk would not go near. Huffington Post might be an option worth exploring – probably as close to mainstream as we can get. More radical publications like Mother Jones might be willing as well.
Thanks again for all you’ve done – you have really catalyzed a movement!
—- Steve
Report comment
I am astounded by the reactivity and anger toward you, Mr. Whitaker, for asking really good questions, questioning the “experts” and the way the mental system and professionals work. Why so reactive, psychiatrists, especially you Harvard Medical School doctors? I guess some are invested in their own view of the world of psychiatry, it works for them and challenging that well would mean causing some distress, an ego-dystonic reaction. Now with that said I also know of some really down to earth, approachable psychiatrists with degrees from prestigious schools who are willing to be vulnerable and state that there are a lot of mistakes psychiatry has made, that there is much we do not know about the brain and that medications are not the sole answer. The problem is psychiatrists are no longer trained like they use to be in psychotherapy, instead psychopharmacology pays higher salaries,so 15 min. session. Many have lost their skill set as psychotherapists, because they do not practice the art and science of psychotherapy. I am a psychoanalytically trained psychotherapist and I know that we have failed our clients at times too when pushing own theories of recovery and infantilizing our clients out of our own need to be needed. At this point in time it is about integrated care, having teams with specialities from a variety of fields, OT, SW, psychology, nursing, psychiatric rehabilitation and psychiatry. Peer specialists getting in their too. I like seeing priests, ministers and rabbis being part of teams too. But most importantly, it is about making our clients and their families the center, empowering them with decision-making about their own health. This is where healthcare in general is going. Funding is the tricky part. Keep up the good work, Mr. Whitaker, you are on the right path. We love you in the psychotherapy and psychiatric rehabilitation world.
Report comment
I would like MIA to be able to hire a reporter. We need to be able to do our own reporting on these issues
OK…as opposed to everyone “reporting” via their blogs, etc.? Nothing wrong with that of course. But MIA doing its own reporting would still face the problem of it not making it past the pages of MIA, unless something else comes into play.
At this point in history major civil disobedience actions are the only thing that will break into the headlines of the corporate media, and even then it’s not a sure thing — witness the many anti-war, anti-corporate demonstrations numbering in the tens of thousands of participants that have been ignored. However, basing what we do or judging its success on what the corporate media thinks is a losing strategy.
I’ve seen serious movements ignored which later blossomed via grassroots organizing to the point where it became impossible to do so. When we reach a point where significant numbers of people start to reject psychiatry on an organized basis, the mass media will be there to distort and misrepresent us. At that point we’ll know we’re succeeding. And when reporters see that we don’t need them or particularly care what they think they’ll become very interested indeed.
I still think people are blowing an opportunity by not calling into right wing talk radio and also into liberal “mental health” discussions on NPR & the like. And I think it’s high time that conscious survivors started to subvert these “psychforums,” etc.
Report comment
To break the Monopoly, former patients who do not continually take the psychiatric drugs-meds (and are reasonably recovered) have to be published and demonstrated to the public.
But as all are sinners, anyone can have a mistake or bad day at any time. No one is a perfect flawless machine.
Report comment
I’m a little worried about the psychiatric system infiltrating the survivor movement. Since they don’t really need the information the survivors can provide. They already know all of this and choose not to act or change their methods. So every time I hear psychiatrists talk about “co-operating”, I actually hear “control”. By simply being part of the survivor group, they can take edge off and steer the movement into different direction.
Report comment
They already did that in the 1980’s; we’ve yet to recover. How do you think terms such as “mental health consumer” originated? Certainly not with us!
Report comment
Criticism of psychiatry was much more acceptable 30 or 40 years ago than it is today I’m afraid. I’ve long been ready for a sea change, and I think it may come, but there is little indication of it at present. The change that occurred way back when, and I’m referring primarily to the arrival of the DSM-III, went in the other direction.
I’d say that a big part of the problem has to do with the power of money. The drug companies have it, and the victims of psychiatry don’t have it. I’ve always felt that mental health treatment is more akin to police science than it is to medical science. It is going to be an uphill struggle to convince certain people of the innate humanity of mental patients, and when that is done, the argument that health is being damaged by current practices has a chance.
Psychiatry’s arguments regarding so-called schizophrenia hinges on judging people inferior, that is, deteriorated from whatever was expected of them. I don’t think you’re going to get a lot of improvement in outcomes if those outcomes are a matter of wending one’s way through a rat maze. Given a bad situation in the first place, more bad situation is not likely to elicit a lot of positive change. I don’t think psychiatry can ignore the results of its own research forever. Although it’s done pretty well thus far, sooner or later, the truth should prevail. Or, considering how things have gone, not.
It never ceases to amaze me how much psychiatrists like (Lieberman) Pies and Frances are invested in not seeing what’s going on, even with what they do acknowledge as wrong. I think part of it is this ‘those things happened in the old days that don’t happen now’ attitude. Some of ‘those things’ are still happening. Some of the defenders are posing as critics, but it’s only a pose. Allen Frances, for instance, would defend his profession from extremists. Ditto, Pies. However neither of them are very astute at acknowledging the extremism within their profession. That would be like, given a history lesson, stopping eugenic mass murder before it occurred.
Report comment
I see psychiatry taking a different tack, Frank…. (There MUST be a FEW “good” psychs left….)…You know it’s “Mental Health Month”, and that means the publicity propaganda is running thick in the media….Lots of various stories about various “mental illnesses”, mostly touting the standard, pro-drug, no-hope, party line.But little mention of psychiatrists, or psychiatry. NAMI seems to be doing the heavy hitting with the fraudulent statistics….And, of course, the weasel words. What’s a “diagnosable mental health issue”, which 25% of the population has, according to NAMI? The psychs are re-branding themselves as “neuropsychiatrists”, because that’s where the big ($$$) investment ($$$) is…. “Genetic cause of “mental health issues”, doncha’ know….
Here in N.H., no less than former N.H. Supreme Court Justice John Broderick is spearheading a fairly well-funded “New Direction” (or something like that….) PR campaign, and it’s touted as “the first time a State has….”….yada, yada, whatever…. But, here in Keene, a major population center for 10% of the NH population, the local psych unit closed because of no psychs! Despite the much ballyhooed “Heroin / Opioid crisis”, the local inpatient drug rehab can only fine *ONE*, 82-yr. old psych to sign in new victims for insurance billing…. // The IRON is HOT. We need to STRIKE….just sayin’….Can’t you hear me **SCREAMING**….????….
(c)2016, Tom Clancy, Jr., *NON-fiction
I’m ready, willing, and able to go PUBLIC, with my story….
Report comment
Would they be selling “mental illness” with such abandon though if there weren’t big bucks in it? I say not, and I think there we are in agreement. Given that it is so lucrative, of course, countering it is going to be a problem even if that is the stated purpose of the psychiatrist.
All the talk about loss of production, etc., is looking at one side of the issue alone, the other side of the coin is all the work that is created by any individual’s invalidation. There’s a lot of coinage in that. You can’t talk about one side without ignoring the other. How else is NAMI going to get that 25 % estimation you are talking about? A sensible approach, something that we are not going to have anytime soon, would be to put a big dent in the drug industry, and that in turn would carve a big furrow in the “mental health” treatment business, but you can’t do so, and maintain a thriving “mental illness” industry at the same time.
It’s all connected, and with psychiatric cynicism, but because that cynicism pays. I think the biggest problem is that it doesn’t pay to get people out of treatment programs, and so there is no enthusiasm in the idea. They can shake their heads over other people problems until the cows come home, but that’s what puts bread and butter on their tables. Holding patients pays, getting them out of the system, that doesn’t pay, it costs instead. There is no incentive to remove people from the system, not so long as the system is going strong, despite the costs to the physical health of the patients.
Report comment
Frank, you’ve got a point about profits being a big motivator for the current psychiatric ideology, but it’s not just profits. It’s the status quo in general, which is power, profit, and control. Sure profits are a big thing, but it’s primarily about the control and power. Psychiatry and Big-Harma may make billions of dollars in profits, but they also have the political and legal power to detain and drug anyone against their will and also the control over peoples lives based on arbitrary labels. Profits are a big part of it, but don’t forget the other aspects of the status quo, which is power and control. The profits are the bonus, however the power gained from the control are the main points. It’s all about control. And psychiatrists and governments are absolute power tripping control freaks.
Report comment
True enough, for them it’s about maintaining the status quo. A status quo backed up by big bucks, law enforcement, and all sorts of institutions. The thing that makes it so difficult for us is, precisely as you say, we represent a challenge to the status quo, and a status quo that doesn’t like challenges. After all, the force (army, navy, air force, wall street, etc.) is with them, to paraphrase Star Wars. The powers that are not yet powers, well, it’s their drive that we must bank on.
Report comment
This is mainly a comment for Bob, so please read it Mr Whitaker, however it also involves others. Beware, essay ahead!
So, a little backstory first. Over the past 2-3 days I heard about a Youtube channel (H3H3) being sued by another youtuber for using videos and being critical of him which he claims were not fair use. Another youtuber (Philip De Franco) made a video about it saying how stupid and possibly precedent setting it would be for one youtuber to be able to take down another youtuber’s video/channel because they didn’t like something that was posted and claimed under fair use. Long story short(ish), Philly D created a gofundme page which in like 24 hours got over $100,000 for H3H3 to fight these bogus fair use claims.
Getting closer to the main point, MiA is a brilliant website with many contributors talking about how flawed and corrupt psychiatry is and that psychiatry is pseudoscience not real science and it is harmful not helpful. However, the information presented here on MiA doesn’t get much further than the MiA community so really only those who are already aware of the ‘anti-psychiatry movement’ will be exposed to this information.
So here’s the point I’m getting at. Couldn’t we, as a community, do something similar to what H3H3 and Philly D did? We could, for example, create a 5-15 minute video, with a number of the many well known contributors to MiA and anti-psychiatry (Whitaker, Breggin, Hickey, Moncrieff, Kirch, Goldacre, Angell, etc etc, not to mention the psychiatric survivors) talking about the many flaws of biological psychiatry: ghostwritten or manipulated studies, DSM lacking validity, psych drugs lacking safety and efficacy but having potential for harm, Pharma bribes of doctors and ‘thought leaders’, etc. Kind of like a mini documentary. This could be posted on and shared on sites such as Youtube (and spread the link through other social media sites like Twitter or Facebook). We could also get popular youtubers, who post specifically about psych related stuff or are just popular open-minded peoples, to also talk about it and spread the word. This mini-documentary could then be tied to a gofundme or similar site to raise money to afford a) a journalist to post stories on mainstream media like Bob mentioned above in a comment, or b) a lawyer to essentially take biological psychiatry to court and prove it fraudulent and harmful. With option b, it may cost a lot of money, but surely there would be a lot of people worldwide willing to contribute a little money (and a little from a lot adds up quickly) to combat organized psychiatry because so many people have been harmed by it. And since this community has the truth on our side, with all the evidence we could easily argue in court that biological psychiatry is not a real science and is harmful not helpful. Psychiatry would not be able to argue that they are right because psychiatry is based on lies and marketing not truth and science. So, since we’d have all the information proving our side it should be an easy (though maybe costly/lengthy) win because psychiatry has absolutely no evidence to support its claims (brain diseases, chemical imbalances, valid diagnoses, safe and effective drugs, etc).
Biological psychiatrists (Pies, Francis, Lieberman) will not publicly debate those who are opposed to biological psychiatry (such as those awsome MiA peoples mentioned above) because they know they could not win the debate. So, take ’em to court. Prove it in court. Set a precedent. Right now there are laws saying it is legal for psychiatry to kidnap/detain people and forcibly drug/electroshock them against their will if they are deemed a ‘hazard to themselves or others’ based on bogus psychiatric labels. Well, prove it in court, with all the evidence to back it up, that psychiatry is fake science, that ‘mental illness’ is not a real illness or disease, that psych drugs are potentially harmful or even lethal, that electroshock is brain damage not a cure, etc. Once that is proven in court then it will come back on government policy that supports biological psychiatry and psychiatry itself. Lets say, as a completely made up example, that psychiatry says cyanide is a cure for mental illness and governments approve the forced use of cyanide, then you prove in court that cyanide kills not heals, the government and psychiatry will be forced to change their stance on forced cyanide or be exposed for the harmful and corrupt organizations they are because if they don’t make changes it will be proven that they support something with zero scientific backing that can potentially harm or even kill people. If people still want to take cyanide then it is up to them as an informed choice, but it would no longer be forced or used as a front line treatment. I hope I’m getting my point across in my usual roundabout way.
To do this would of course take a bit of time and organization. It would need to have some proper planning and not be rushed. Psychiatry still flourishes because they have the money backing them, because information like what is presented on MiA and other such sites only reaches a small audience that is already aware of the information, and because we as a community are divided (compared to organized psychiatry) and we only chip away slowly at the lies promoted by psychiatry and Big Pharma. We need to put down our differences and work together. And we need to put down the chisel and grab the sledgehammer. There are hundreds of articles on MiA and elsewhere talking about the many flaws of psychiatry but it hasn’t really done anything. Psychiatry is still here. In a year, two years, or ten years, nothing will have changed. Sure psychiatry is starting to tremble a little but our information frequently fails to make it into the mainstream and the public psyche. They currently control the public narrative. So we need to come together as a community. Get a video to present the information to the public, create a gofundme (or similar) page to gather funds, gather all the information that challenges psychiatry, and find a lawyer willing to fight psychiatry in court.
Biological psychiatry does not have the evidence to support their claims of brain diseases and chemical imbalances. It’s false advertising and fraudulent and a few other words I probably shouldn’t say on a public forum. Psychiatry needs to be exposed and torn down. We have all the information and evidence, now we need to up our game. If the mainstream media will not present this information (as Bob above has mentioned where media fails to report on his and others books and refuses to print any articles critical of psychiatry) then we should use social media to share the information ourselves. And do it on a massive scale. The few dozen authors on MiA will surely have a following based on their articles or books or videos and will likely have atleast one social media account (youtube, facebook, twitter, etc). If everyone made some noise and pointed to a mini-documentary and fundme site the word would get out and spread fairly rapidly (obviously after said documentary and funding site were set up). We’ve chipped away at the edges of psychiatry for long enough. Time to pick up the sledgehammer. Or maybe we should should … *breaks into song* come in like a wreaaaking baaalllll!!
Report comment
Well, prove it in court, with all the evidence to back it up, that psychiatry is fake science, that ‘mental illness’ is not a real illness or disease, that psych drugs are potentially harmful or even lethal, that electroshock is brain damage not a cure, etc. Once that is proven in court then it will come back on government policy that supports biological psychiatry and psychiatry itself.
Now you’re talking. We need a test case or two or three, with the combined testimony of experts in medicine, law, language, logic, interpreting “studies,” history, political science, eugenics, brainwashing, etc etc. pooling their expertise to discredit the institution from all angles, and demonstrate that there should be a clear separation of government and psychiatry at all levels just as there is supposedly a separation of church and state.
If Amnesty International would take the case of the court-ordered shock victim in Melbourne (Garth?), if he’s still alive by now, it could have international repercussions for psychiatry, and perhaps save a life. And anti-psych folk from all over could jump on board to support him.
Report comment
THANK YOU! I’m sorry but most of this `discussion has been almost, if not more of a w**k than a smug, group of `research’ psychiatrists working out how to get yet another grant from the government. At least they’re thinking of ways to get something. I’m out of it. Come up with solutions or shut up!
Report comment
I think the lack of open-mindedness and curiosity has something to do with deeply embedded extreme anger which closes the heart, which I feel is a significant source of our consciousness. I imagine that these cannot exist in the same space, they do not seem to be compatible. It’s either the first two or the other.
Report comment
I recently watched a film on Netflix called “Requiem for the American Dream” . It’s an interview with Noam Chomsky and for me gives background to many of the points made in the above discussion.
Report comment
Antipsychotics make no claim to cure, and they don’t cure. They treat symptoms, sometimes with a faint hope that the patient will cure themselves. If the patient does cure themselves, they disappear from the system. If not, they keep buying. CURE is not defined for any illness not caused by a parasite. Cure-rate, used for cancers is just a fancy name for ‘wait and see’. The word cure does not appear in Webster’s New World Medical Dictionary, third edition. Neither does cured, nor cures. http://healthicine.org/wordpress/websters-editors-removed-cure-dictionary/
If we are to cure any illness, including illnesses of the mind (not just the brain), of the spirit, and of the community, we need to define cure, aim for cure, and recognize, investigate and celebrate cures when they occur.
to your health, tracy
Creator: Healthicine.org
Report comment