The pain assessment chart. We’ve all seen it on the wall in the ER, the doctor’s office.
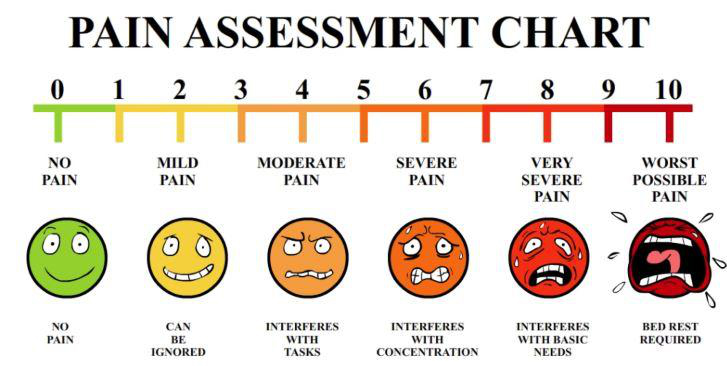
I remember laughing at it when I first saw it in the local pain clinic in October of 2017. I’d gone in to get deep Botox injections in my neck — 24 of them — for my seized neck muscles, one of the many neurological conditions caused by psychiatric medications.
It was October 2017, and I’d been off the offending medication, Latuda, for over a year. Latuda is one of many “new generation” atypical antipsychotics that, once upon a time, were only given to the “severely mentally ill.” Atypical antipsychotics were FDA-approved for bipolar disorder, bipolar depression, treatment-resistant depression, and unipolar depression. They are also routinely prescribed by all manner of physicians to treat insomnia, postpartum depression, PTSD, and other mental and physiological disorders.
I pointed to the pain scale and said to my husband, “I wish ‘10’ and ‘bed rest required’ was my ‘worst possible pain.’” He agreed. I looked at the pain scale in the pain clinic with no small amount of anger and feelings of loss and betrayal because by that time, I’d been to see four doctors — three neurologists and one ER doctor — all of whom didn’t, and don’t, believe I was in pain when I came in to see them.
Which, looking back, seems odd to me. They (doctors) believed me when, in the 1990s, a CT scan showed I’d sustained a concussion and whiplash after being violently assaulted. They believed me when I presented with all the symptoms of a traumatic brain injury (TBI) and was experiencing depression as well as cognitive difficulties — things I’d never before struggled with — consistent with a TBI, such as a substantial loss of executive functioning. They believed me when I said I felt myself heading for a brick wall physically and emotionally. They took my word for it and gave me more and more medications to try to stop the collision.
Fast-forward years later:
In 2016, after years of suffering with an extrapyramidal side effect caused by the medications they gave me beginning in 2004, I told these three neurologists and the ER doctor the name of my suffering: akathisia. The bastard child of psychiatric medications that no one wants to claim. I knew the name because my former psychiatrist and neuropsychologist diagnosed me and told me to see a neurologist. They took one look at me and all but ordered me to the ER. They assured me the physician there would admit me, and I’d get a full neurological workup. I didn’t want to go, even though I finally knew why I was feeling this pain. A drug side effect? Unbelievable.
I couldn’t believe a medication could cause something so completely disabling — a pain that blurred the lines between emotional and physical: the type of pain you feel when you can’t eat after a horrific loss or trauma. Pain that ground inside me every day, without a reprieve. How bad is the pain? The following is a short YouTube film I wrote and produced. It shows you just how bad the daily pain can be. And how the “good” medications we’re given caused it.
I’d been told it was my “illness,” so I battled shame, guilt, and daily thoughts of ending my own life due to how agonizing it had become. The pain seemed to center right in my solar plexus, and it was so unrelenting, I was almost entirely homebound. My career as a public figure dwindled to a whisper. My world, our world, had shrunk from a panoramic window of infinite possibility and adventure to a peephole.
The Pain, as I called it, was not depression, not anxiety, and it wasn’t a worsening of an underlying mental illness, as I’d been told. I’d been treated successfully with talk therapy for depression as a teen. I knew “depression.” I’d had some anxiety and knew how to deal with that well enough. But when I began taking antipsychotics, the pain I experienced was something else altogether, and I knew it.
“Akathisia: restlessness and feeling like you can’t sit still, right?” Not quite. Not entirely. That’s like saying “Ah, cancer. So, losing some weight, are you?”
But when I told these four doctors I had drug-induced akathisia, and it was tardive, acute, chronic, and getting worse — when I told them how akathisia presented in me and for me subjectively, because there is a “subjective component” of akathisia that’s been documented, which all four acknowledged…
They did not and do not believe me.
I’m not even sure my current doctors believe me. I think they believe *I* believe I am experiencing “real or perceived pain.” But they don’t fully believe it’s the neurological movement disorder, akathisia. This begs the question:
When did my credibility suddenly disappear? And why?
It’s simple, really. I lost credibility when they misdiagnosed me in the 1990s with a mental illness after I sustained the TBI. In other words: They stopped believing me when I chose to believe them.
* * *
When they ignored the classic TBI symptoms with which I presented at the county-run, sliding-fee mental health facility back in 1996, the only care I could afford with no insurance, they went with the easier diagnosis: “bipolar disorder.” The other obvious issues I faced didn’t fit their categories.
I couldn’t google symptoms of a brain injury in 1996, and I had no financial help. All I had was implicit trust in doctors, something my parents handed down to all of us, and why I have a disproportionate number of doctors in my family, I’d wager. In the world in which my parents had grown up, doctors were akin to clergy: sacrosanct, and impervious to baser human frailties.
They asked me questions at the mental health clinic, and I offered up the other symptoms that had caused me to lose jobs, and flunk out of college because my professors suddenly spoke in “word salads.” Panic gripped me as I watched my once off-the-charts reading comprehension dissolve into an inability to follow a simple cake recipe. But they didn’t want to hear about those symptoms. Instead, they misdiagnosed me, and I believed them, because they were supposed to know more than I did.
In the last 2+ years, I’ve been searching for help, specifically from neurologists, since “neurological” is right there in my diagnoses. I have what is called DIMDs, or drug-induced movement disorders, and they are neurological. Most recently, my dystonia has advanced. It is now beginning to affect not only my ability to swallow, it has progressed to the point where my respiratory muscles can, and have, seized up. When this happens, I cannot breathe. I literally feel as though I’m suffocating. And as it progresses? I could.
But I no longer feel safe going to a new doctor, nor the hospital. That’s because the three neurologists and one ER doctor we saw told us, and wrote in their clinical notes, that I am psychosomatically ill.
Each doctor wrote in my chart, to be seen by every healthcare provider I see “in-network,” that I have Conversion Disorder, now known as FND — functional neurological disorder — and that I should be evaluated by a mental healthcare professional/specialist.
They all said that the subjective “pain” caused by akathisia, the pain I experience, is not neurological. Doesn’t “subjective” mean it’s different for everyone? Yet their unilateral diagnoses, which relied on my health history and their clinical, subjective opinions, have been validated by their white coats.
Further, two of the neurologists suggested that I had features of a Cluster B Personality Disorder. In case you’re not familiar, these include Borderline, Histrionic, Narcissistic, and Antisocial Personality Disorder. The Cluster B’s are characterized by emotional instability, cries for attention, unstable self-concept, and by being overly dramatic, pathologically dishonest, manipulative, and lacking empathy for others, among other “features.” In other words, the neurologists all concur that I am the most unreliable “narrator” of my own subjective experience and pain.
One neurologist, who seemed extremely hyper-focused on my need to see a “mental health specialist,” wrote that I should be evaluated specifically for Borderline Personality Disorder. Because they are not “mental healthcare specialists,” they are not qualified to diagnose me themselves, despite obliquely doing exactly that.
After they all cast doubt on the reality of my pain with what they wrote in my chart, they all concurred that I have drug-induced neurological movement disorders: tardive akathisia, dystonia, dyskinesia. They also confirmed the TBI. An MRI of my neck a year ago (before the Botox shots) confirmed the herniated discs in my C-spine, but the injuries were not new. Had I been in a car accident 20+ years ago? asked the pain-clinic doctor.
But what the neurologists categorically deny is that akathisia is “painful” — specifically, “subjectively, emotionally painful.”
One neurologist, the second one I saw, wrote a redundant narrative throughout my chart about my emotional “instability,” and suggested the BPD “evaluation.” Usually it takes a while for even a therapist to make that call. He diagnosed it, wrote it in my chart, despite the fact that he knew I am currently in therapy and have been most of my adult life, due to the trauma of sustaining a TBI in a violent assault, but also dealing with what we now know to be the direct result of iatrogenic harm.
Yet, he told us akathisia does not cause feelings so painful that they can lead to suicide.
“Sure. Akathisia does cause some ‘restlessness’ and that can be ‘uncomfortable…’ but akathisia is a motor dysfunction characterized by… and it does not ‘cause’ suicidal feelings…”
The pain of akathisia is worse than anything I’ve ever experienced in my life. I’d rather go through natural childbirth, daily. Yet Dr. “Uncomfortable” then told me my movements weren’t “consistent with akathisia presentation.” He proceeded to dance like a belly dancer in his chair, “showing” us what akathisia looks like. We left, and I was in tears. I was worried that perhaps I was mentally unstable. He gave us patient handouts about akathisia. Dr. Uncomfortable showed us an adorable belly-dance routine while my body shook and jittered exactly as his patient handout described.
My account was the same as I spoke to these doctors, varying only a little, because how does one purport to describe the indescribable? I’m a writer by trade, so, I used my skills to convey the pain of the persisting akathisia to each doctor and neurologist this way:
Take every horrific feeling you’ve ever had in your life, all at once. Now, times them by 200, right in your gut. The “my-mother-just- died-and-so-did-my-cat-and-my-wife-left-me-for-my-best-friend” feeling. On top of those? A feeling of terror, panic, fear, as if you LIVE in a horror movie, and you must do something, or everyone you love will die, YOU will die — and you’ve no clue what that “something” is. So sick with this pain, caused by this neurological condition… so sick from it you can barely eat. That is how akathisia pain feels. It’s how it feels to me, and countless others who are experiencing it, or who have.
And they have all methodically undermined my credibility in my permanent record — a medical maligning that could cost me my life.
Because if it’s emotional, then it’s my fault. My problem. My issue. When, in fact, my symptoms were not present before they gave me the medications in the first place. Hardly a causal link in the world of science. But when I walked into their offices? I was not suicidal.
Yet, all I had to do was tell them I was in emotional pain when I walked into the doctor’s offices in the 90’s, then again in 2004, and they believed me enough to give me dopamine-altering medications that can, and have, caused permanent damage to my brain.
And this is because they do not know, and rather than admit that, they dispute my subjective experience, and the experience of countless others, and add “mental health” determinations they are not qualified to make based on less than 30 minutes of face-time. A personality disorder. And according to their criteria and the general definition of Cluster B Personality Disorder they adhere to from the DSM-5, symptoms must:
- not be due to another disorder
- not be due to an isolated stressful situation
Well, they’re right about one thing: It isn’t due to only one, isolated stressful situation — not anymore. The TBI from having my head bashed into a car by someone I once trusted? That was only the first of many blows to come.
The first neurologist I saw in Salt Lake City is a specialist in movement disorders. After telling me there was no viable treatment for them, specifically akathisia, she went on to write this characterization of akathisia and its subjective component:
“Tardive akathisia . . . most often associated with antipsychotic drugs, which antagonize dopamine receptors. The subjective component can be characterized by the aforementioned restlessness, as well as tension, panic, irritability and impatience.”
Along with this, she wrote her impressions of me, impressions that seem particularly callous and paradoxical, given her diagnoses:
“PHYSICAL EXAMINATION: General. Extremely frustrated, anxious and at times tearful woman.”
Two weeks prior to seeing her, I had lost my ability to walk normally, had begun to move involuntarily, was developing aphasia (an inability to understand or express speech), and let’s not forget The Pain — akathisia — a pain so horrific I wanted to die to escape it.
Yes, when she told us she had nothing to offer, I was upset, emotional, and began to sob in the exam room. With no answers, no hope in sight, I behaved exactly how a person who had sustained a TBI would behave; exactly how someone who suffered from the neurological disorders each doctor diagnosed me with (including rapid-onset dystonia) would behave. According to the Dystonia Medical Research Foundation’s website:

Finally, I behaved exactly how any human being would behave and react when told there is no treatment, no cure, no hope, and that her pain is not real, not physiological, but an emotional and mental health issue.
My brain injury has impacted me for over 20+ years, and I did not know it. I had suffered from drug-induced akathisia for 12+ years and did not know it. My dopamine has been dysregulated by medications, and yet they told me that akathisia could not cause subjective emotional pain, despite the role dopamine plays in our brains’ control centers for all our physiology — including our emotional states.
And if I suddenly can’t breathe due to a dystonic seizure of my respiratory muscles again, and it’s worse than the last attack? I can’t call for help. Even if I make it to the ER, it’s possible a nurse or doctor there will read through my chart and see, hidden in the medical language of those who have made their arbitrary dismissals: “Unstable, unsound. Don’t believe her.” And as I slowly suffocate, they could very well pat me on the head and tell me to calm down while they go find a sugar pill.
Well, at least a sugar pill won’t make my akathisia worse.
The article on “Talking to Your Doctor About Pain” that arrived in my Inbox the other morning made me bark a laughter as bitter as my chicory-laced coffee. It suggested that we don’t “shy away from ‘flowery language’ to describe [our] pain.” Flowery language? I’ve written a whole book of flowery language: flowery, plain, in-your-face-obscene language, medically accurate and appropriate language, all describing akathisia pain. I tried flowery. But my doctors didn’t hear it. They searched for categories in which to place me. And they’ve succeeded.
After the premier of my “How Bad Can Good Be” video, messages and emails came pouring into our site’s contact form (akathisia.life — the website my husband put up to help bring awareness to those who don’t have the resources we do). The messages all had horror stories, more horrific even than mine, and the single, common thread within the messages, from those who are suffering with akathisia:
“Thank you for writing the feelings I couldn’t express and conveying the horror I feel every day.”
My film has been shared on social media (it now has over 10k views on Facebook alone), and one chilling tagline was simple, and terrible, in its implications:
“It has a name.”
And now it also has a face. To capture the horrifying pain of akathisia, I created a painting with charcoal and photo collage:

This is my worst pain, far beyond “bed rest required.” Tell me, does the image above convey simply “uncomfortable” to you?
I’m going on 14+ years now with drug-induced, now tardive, chronic akathisia. As I’ve searched for a neurologist to be on my “care team” to help me deal with the drug-induced movement disorders, specifically help with ways to deal with the progression of drug-induced dystonia, they brush me off.
More to the point, they brush akathisia off. “Uncomfortable,” remember? Not so painful you want to end your life. Not so horrific you might take someone else’s with you to the other side. No. Uncomfortable.
If I were as “emotionally unsound” as they say in my medical chart, I’d say it’s almost like they want me to end my life, so they can write it off as “another tragic suicide caused by mental illness.”
Only, I’m not mentally ill, based on their own criteria. The only mental health issues with which I currently deal? The trauma of iatrogenesis and living, every day, with these conditions created by medications as I fight for my life.
Sorry, Doctor Uncomfortable and Co. I’m not going anywhere. And your patients? We are reading the same studies as you — and more. Because your motivation is to keep the status quo, aka your jobs, your relevance, your authority. So, you will only seek out studies that support what you believe. Call it confirmation bias, call it professional and publication bias, it’s all the same stuff. Our motivation? We want you to hear us, help us, and tell us what we do NOT know. Admit what you cannot do, and then do your jobs. HEAL. You broke it: fix it. And only pressure from you, the “dealers,” will change the way pharmaceutical companies create and market medications.
Our pain is real. And too many medical professionals have actually caused it by their willful ignorance, coupled with blind, medical arrogance. Yes, it takes two to form a lie: we are complicit. We want professionals to have the answers, so we give them the answers they need to give us our labels, medicate us, so we can go on with our lives. But the lies are killing us.
And when we begin trusting ourselves, and arming ourselves with the facts and studies coming out of Europe (the more-evolved cluster of First-World countries who provide universal healthcare to their citizenry), we will defer to them, because they are not motivated by the greed that riddles the polluted, crooked, for-profit healthcare system in the U.S.
For any of you who have taken medications that cause akathisia, arm yourselves with facts. You can google. Look it up. You’ll officially know more than most neurologists.
Watch my video. Look at the website for akathisia info. Read Robert Whitaker’s book, Mad in America, and the others out there who are trying to wake you up. We are trying to save your lives.
Then share what you learn like your life depends on it.
Because statistically… someone’s life does.
And yes, it will be uncomfortable. Challenging accepted wisdom usually is.
But look into the “face” of that pain, above. I promise you: Confronting your doctor with your truth isn’t nearly as “uncomfortable” as a pain that invades your entire being, finds every soft and vulnerable place within you, and rips it out with its teeth as you watch in horror…
Because “it” isn’t holding the gun to your head, or stringing the rope up in the rafters:
It’s you.
Flowery enough for you?














Yeah that’s a good video… forces it through with intensity. You can be perfectly still with it as well. Horrific. Pharmacogentics will prove the ‘doctors’ did it with the full knowledge of the drug companies.
Report comment
Clearly different people will identify different experiences as tardive akathisia. I can’t relate to your attempt to turn it into words and maybe that’s because it can’t be. Every time I’ve read an attempt to narrate akathisia I’ve been left cold. Important to add that this includes my own attempts.
I did like you pointing out on your website that akathisia gets red-lined as a spelling error often. As it does here. Which I have remarked on in the past yet it still goes on making me doubt. Which of course is taking the piss.
(tardive also gets red-lined which again is a massive piss-take for a place like this)
A lot of your agony seems more connected to dyskinesia. And you seem to be blurring the distinction.
I’ve asked myself seriously if it is important to maintain the distinction and I think that it is. Dyskinesia is a very visible movement disorder. Akathisia is often an invisible torment.
But I wish you well. And I hope one day I get to talk to you in person.
Report comment
Thank you for your comment, and yes, it is a very important distinction. The article had to be edited for length, but originally I’d included the chart for the cluster of drug-induced neurological movement disorders (DIMDs) and each are distinctive. Dystonia, not dyskinesia, is the second source of pain for me, and it is progressing.
However, dystonia presents in so many ways, to arbitrarily say “I have dystonia,” and for people to say, “Ohh, yes, I know what that is” is akin to saying, “I have cancer.” No one says, “Oh, yes, I know what that is.” They say “Where? What kind? What stage? What is the prognosis?” Stage I skin cancer is a very different beast than Stage IV pancreatic cancer.
Dystonia is, within itself, a cluster of different movement disorders and the etiology of it is as diverse as its presentations. For example, “childhood onset” is totally different than “task-specific” dystonia. Task-specific includes, for example, “writer’s cramp” and “musician’s cramp.” What would happen if a doctor said to a concert violinist who played for the London Philharmonic: “Your hand seizing up like this when you play the violin is a subconscious desire to QUIT the violin and do something else. Perhaps golf or soccer? Tell me about your childhood.” Think about that. It’s absurd.
As to “my” presentation of dystonia, the short answer is that I have drug-induced, acquired dystonia that effect several parts of my body and in different ways. The fact it shows up in public more than when I’m home, in my “safe, controlled” environment is decidedly INconvenient for me and others with dystonia, but some people think it proof-positive that (drug-induced) acquired dystonia is a “cry for attention.” Trust me, I can think of better ways to get attention than suddenly having my back or neck seize, causing me so much physical pain, I am nauseated.
My presentation of akathisia is from having it for over 14 years now. Imagine the “fight, flight, freeze” response in your brain on HIGH-ALERT, all day, every day. Isn’t it conceivable, then, that after a while, someone’s brain might perceive the constant barrage of fear from their limbic system as “pain”?
I had a doctor suggest that the film, and now this article, is my “payoff.” That it’s an attention-grabbing behavior which supports their conclusions. I was stunned. “Yes. Because THIS is how I want to be remembered.” Any writer or artist will tell you: we want to be known and appreciated for our WORK, not for a gimmick or “schtick.” Certainly not for an illness. Pretty sure Michael J. Fox wishes his great roles in many movies and television were the first things that come to mind when we speak of him, not Parkinson’s.
If you were to read any of my previous work–poetry, novels, short stories–less than .001% of my writing has to do with “bipolar disorder,” or the pain of akathisia. The singular exception is the book to create awareness coming out next year. So there’s no history of using any medical issues or social platforms to call attention to my work. It stands alone and I am quite proud of what I’ve been able to accomplish while dealing with drug-induced akathisia.
Back to your excellent point: I believe akathisia, once they truly begin to accept and acknowledge its existence that is, ought to be classified in the many differing ways it presents, just like dystonia.
For example (and of course, this is my non-medical attempt to classify): inner akathisia (with or without motor sensations), inner akathisia with suicidality, agitation, and/or rage and violent features, outer akathisia with purposeful movements, mobility-dependent relief, lower-extremity focused, distractions can mitigate movement and inner pain, etc. Acute; severe; chronic; rapid-onset; mild, intermittent…
And on it goes. However, one thing remains a constant: it is caused by medications. Period.
So how do you “classify” akathisia’s subjective presentation when, for some people, it feels as though they get electrical shocks? For some, the need to “jump out of their skins.” Or slow-onset, where at first it causes feelings of mild-to-moderate hyper-anxiety, feeling the need to DO something–anything. For many, it causes a type of “frozen” immobility that leaves them home-bound and unable to interact with others. They even wrap their arms around themselves as if warding off a blow that has yet to come. Others I’ve spoken to are in so much pain, breathing hurts, standing upright hurts, and their concentration? Poof. Gone, because the feelings overwhelm everything else.
MISSD has a fantastic new video out that shows real people who have filmed themselves as they experience akathisia. One woman–the look on her face–I know it well. Her words, simply, “It hurts. It hurts.”
So yes, distinction is vital. And the one distinction akathisia has as opposed to other neurological movement disorders is as I wrote above. It is not organic or passed down genetically, like diabetes or dystonia or Parkinson’s. No.
Akathisia was birthed in laboratories; its creators? The very people who became research medical scientists in order to help humanity. Improve quality of life. Cure diseases. Treat chronic illnesses. I’m pretty sure no one walked into a big pharma lab with the intentions of creating this horrific condition.
But when they realized they had? What they did NOT do is ultimately how history will judge them.
And to all who have commented here and written that doctors-in-training ought to be required to take AAPs for 2 weeks, then go cold turkey? BRILLIANT. I agree. I recently asked my doctor if he would prescribe these meds to his own children. He didn’t reply exactly. He sort of demurred, smiled. Then, in my clinical notes he wrote, “She sure seems mad.”
Gosh, do I?
Thank you for your comment–and thanks to everyone who has shared and supported this message.
Peace to you all–
J.A.
Report comment
Thank you for this powerful and painful advocacy.
For demanding that knowledge and awareness of AKATHISIA replaces the inexcusable ignorance and denial which dominates the presentation of this common, life-threatening and life-destroying neurological adverse reaction to many prescription drugs, but especially to psychotropic drugs. (ADR).
There have been times when I am so moved, and so hurt by the refusal of my own profession to prevent suffering on this scale, and of this intensity, that the only words that come into, and refuse to leave my mind, are those words of Robert Oppenheimer at Los Alamos which captured the impact of the first atomic explosion.
“FOR I AM BECOME DEATH, THE DESTROYER OF WORLDS”.
I have quoted these words on MIA before.
I feel that they represent what is happening every time AKATHISIA is caused to each individual person by
ill-advised, marketing-driven prescribing, ignorance of psychopharmacology and toxicology, and the sloppy, misdiagnosis of alleged “mental illness”.
The patient whose iatrogenic AKATHISIA is misdiagnosed as emergent “Severe Mental Illness” –
(“Bipolar Disorder”, “Schizoaffective Disorder”, “B.P.D.” ) – is not only incarcerated and forced to ingest more and more AKATHISIA inducing drugs, they are also labelled for life as societal rejects.
Forcibly subjected to physical, social, psychological, economic, relationship injury and deprivation.
They are sentenced to be disbelieved, rejected, ridiculed, blamed and no longer worthy of compassionate, empathetic day to day, year to year, routine medical care and attention for the rest of their lives.
Routine psychiatric labelling errors are truly devastating, and are as irremovable as tattoos.
Each new psychiatrist only sees the injuries caused by the neurotoxic, akathisia-inducing drugs, coerced or enforced by the previous psychiatrist.
Their ADRs are routinely misdiagnosed as new, emergent, or relapsing mental illness.
Only the parents, loved ones, partners and carers knew, remember, and grieve so profoundly for, the charismatic and enchanting human being, their son, daughter, lover, parent who has been condemned to a living death, or indeed died from AKATHISIA induced self-death.
The latter will of course be mislabelled as suicide.
Please, if possible, look at the M.I.A. link to:
“My Baby, Psychosis and Me: A lesson In How Not To Make A Documentary About Mental Health”.
BBC Television 2016. (Rai Waddingham, M.I.A. November 26th 2016).
At about 26 minutes, anyone who knows and recognises Akathisia might be inlined to believe that the featured consultant psychiatrist is talking to a mother “treated” for post-partum psychosis – talking about “these awful diseases”, apparently oblivious to what appears may be extremely severe acute, psychotropic drug-change induced akathisia ???
If so, her wretched suffering is apparently of no consequence
I have studied and/or practised medicine for just over fifty years.
Despite my commitment to life-long learning, I had never heard of AKATHISIA until my young adult child’s beautiful life was destroyed by a GP persuading her to take an SSRI for exam stress instead of giving a few needed words of reassurance.
The word AKATHISIA had been deliberately hidden from us as prescribers by regulators and by drug manufacturers.
Her acute and overwhelming akathisia was first treated by changing to sertraline.
The inevitable, even greater akathisia was then misdiagnosed as “psychotic depression” resulting in an endless and ridiculous cascade of some of the most toxic prescription drugs ever mis-licensed for use on human subjects.
They would not listen to me when they induced tardive dyskinesia. – “It doesn’t happen on olanzapine”!
When we eventually got her home she could no longer walk or speak.
Her mask-like face so typical of extra-pyramidal brain injury.
A face so beautiful before AKATHISIA IGNORANCE.
The concomitant major injuries to other systems have been described here before.
After half a century, I am left ashamed of my own profession.
I also hold the belief that, until my profession embraces AKATHISIA PREVENTION, we are missing one of the greatest opportunities to reduce death, morbidity and suffering on a scale that few of us have yet conceptualised.
We, as a profession also need to find the humility to consider it likely that the most common cause of acquired serious brain injury is avoidable psychotropic drug neurotoxicity.
TRM 123. Retired Consultant Physician.
Report comment
This makes me weep:
“The patient whose iatrogenic AKATHISIA is misdiagnosed as emergent “Severe Mental Illness” –
(“Bipolar Disorder”, “Schizoaffective Disorder”, “B.P.D.” ) – is not only incarcerated and forced to ingest more and more AKATHISIA inducing drugs, they are also labelled for life as societal rejects.
Forcibly subjected to physical, social, psychological, economic, relationship injury and deprivation.
They are sentenced to be disbelieved, rejected, ridiculed, blamed and no longer worthy of compassionate, empathetic day to day, year to year, routine medical care and attention for the rest of their lives. ”
I was incarcerated in a mental hospital in the 1980s, unable to get myself out until a colleague from my research profession recommended that I hire an external psychiatrist to help me fight the institutional psychiatrists. I finally was released, but this horror has remained with me to this day, and I am terrified that it could happen again, now that my psychiatric diagnosis has been entered into my permanent medical record.
I have been forcibly drugged, put in restraints, subjected to ECT against my will, sexually abused, and humiliated in so many ways by “mental health professionals” that I will never recover from the trauma. I was able to continue working in my profession, but just a few years ago I discovered just after my boss died that he had disclosed my psychiatric diagnosis to many of my colleagues! The truth of this sentence: “Forcibly subjected to physical, social, psychological, economic, relationship injury and deprivation” has so tangibly played itself out in my life.
I am in my mid-60s now, so I’ve survived more successfully than many with similar experiences. I read a lot and work with a Jungian analyst, so I have a wider perspective on much of this; nevertheless, I remain terrified of the medical profession, so much so that I will be leaving the country (as I describe in another post below) to escape both my medical record and the far too many people who know of my diagnosis.
There ARE compassionate doctors, including a few psychiatrists, but far too few to protect us. Medical education is now under the control of Big Pharma, Big Medical Device Companies, and worst of all, Big Medical Insurance Companies. The “healing profession” no longer exists in this country.
Report comment
All the smarts and education don’t matter to a hill of beans if a doctor lies all the time and doesn’t give a rip about his patients.
Dr. Mengele was a highly educated, licensed medical professional. He used it all to harm people in hopes of furthering his prestigious career. Stupidity and ignorance were not the issues with him.
Report comment
Thank you both.
Such iatrogenic destruction of every aspect of human experience, and the global annihilation of all quality of life.
Even to the point of exile.
Experiences of their evil, their absence of empathy, their arrogance and their ignorant brutality.
And still, this devastation passes for “medicine”.
In Medicine’s Enron, aka “Psychiatry” there is no accountability. No Duty of Candour.
Psychiatry means never having to say you’re sorry.
I had just re-watched the Tardive Akathisia video above when: –
At lunchtime on BBC Radio 4 today, a psychiatrist – (and Royal College of Psychiatrists – Chair Re Old-Age M.H.) – was unchallenged when she claimed that the drugs used for elderly depressed patients were – “Tailor-Made Drugs”.
Yes indeed, every last toxic molecule hand-stitched by devoted pharmaceutical robots no doubt?
People “fear they are terribly addictive” – “Well they’re NOT” she emphasised.
So no AKATHISIA, no TOXIC DELUSIONS, no bleeding, no cardiac dysrhythmias, no falls with fractured neck of femur –
No emotional blunting, no disinhibition, no iatrogenic aggression.
No multi-modal sexual dysfunction which is unrelated to depression.
And NO “Discontinuation Syndrome” aka Withdrawal Syndrome apparently?
Do they perfect this propaganda on their own, or do they use group training?
Can they really believe in such fantasy?
Report comment
When “schizophrenics” kill themselves it’s usually in the early years after diagnosis (- before they sort out the drugs causing the problems).
My suicide attempts were drug induced (AKATHISIA); and in the first few years (before I left psychiatry).
Report comment
I don’t know how I missed your comment. Probably because I try not to dwell on this subject too much. But I read your words and I am simply blown away. You sound like you’re maybe in the UK?
As I write my song about this nightmare, I’ve been paying attention to the music coming out–that’s been coming out–and these children that were medicated, they are in pain.
So many songs about psychiatry. It reminds me of the song I loved in high school by the punk band, Suicidal Tendencies, “Institution.” When parents began pathologizing teen behavior–normal teen behavior–I might add, and doctors began to tell them, “Your child needs medication.”
And all I wanted was a Pepsi.
Thank you for your words of wisdom ,validation, and hope–yes, I find hope in them. Because if *you* see and saw what’s happening, other good men and women in the medical profession are seeing it, too. And that gives me hope.
Report comment
J.A. C-W.
Thank you so much for responding to my comment.
I was personally, profoundly moved by your writing, and although it was difficult for me to respond, and painful for myself, and my family (involving personal, professional and family risk of repercussion) – I was sincerely touched by your compelling and important narrative.
I am now inspired by the concept that the few words, which I struggled to assemble, were found by yourself to convey, wisdom, validation and hope.
It was your reference to “HOPE” that has inspired me.
HOPE is the first and last gift that a committed medical practitioner, acting impartially, and with sincerity, can freely give to anyone who is suffering.
I have been astonished by the ROUTINE DESTRUCTION of HOPE which, apparently, is the day-to-day “modus operandi” of “main-stream” psychiatry.
This is alien to every ethical tenet that I learned, experienced, and aspired to achieve during over half a century of studying and practising medicine.
I was trained at a time when many primary care physicians sincerely believed that patients and doctors were “Equals of Different Experience”.
Over a lifetime, some of my medically-qualified patients had far greater knowledge, skill and experience than I did.
With honesty, openness, and ease of the essential response : – I’m sorry, I don’t know: –
To the best of my knowledge, they felt cared for?
How can any “medical practitioner” deny HOPE, and subsequently believe that they have anything “therapeutic” to offer. This is surely delusional?
How can anyone who deprives a human being – (with, or without “mental illness”) – of their freedom, their human rights, and their inalienable right to insist: – “These drugs are unbearable for me” – how can they fantasise that a therapeutic relationship might ever exist between them?
What stops psychiatry from encouraging their trainees to feel confident and comfortable telling a patient: “I’m sorry, I don’t know”?
TRM 123. Retired Consultant Physician. (uk).
Report comment
I am so sorry. You won’t if all you read is pharma literature. You must look at the other extreme drug safety organizations and independent medical journals.
Report comment
My teenaged-daughter, Natalie’s, prescribed suffering and death was caused by akathisia and serotonin toxicity. I first heard the word, “akathisia” when consulting with medical experts after her avoidable death. I’ve since helped create a free, accredited online course called Akathisia 101 available at missd.learnupon.com. See missd.co for more information about akathisia. My child’s story of prescribed harm is at https://www.youtube.com/watch?v=1haYwZGcSRY&t=4s and https://rxisk.org/kidnapped-natalies-story/
Unfortunately, school districts are increasingly inviting pharma-funded organizations into the classroom to teach children an illness approach to mental health challenges. No surprise this instruction embraces risky drugs often not meant for children. See https://fiddaman.blogspot.com/2018/11/truth-or-fiction-what-are-parents-to.html#.W_HkbPZFwps
Report comment
Kristina,
Your two chilling reports on the infiltration of schools by advocates of drug-dependent, biological psychiatry
are more suggestive of a horror movie based on the Pied Piper of Hamlin rather than any valid child-health process.
The predictable outcome may be the mass abduction of children into an anti-therapeutic environment:
aka: “Mental Health”, and inappropriate, exposure to the morbidity and mortality caused by chronic psychotropic drugging.
CHILD ABUSE?
“Federal Legislation provides guidance to States by identifying a minimum set of acts or behaviours that define child abuse or neglect”.
This includes: “An act, or failure to act which presents an imminent risk of serious harm”.
Based on this Federal guidance, is the exploitation of the supposed sanctuary of the school environment now subject to the possibility of State and Market Sponsored Child Abuse?
As if the AKATHISIA-driven school shootings are not horror enough.
Report comment
It absolutely is child abuse for schools to allow drug pushers of any type into the classroom. Most people would support physical and mental wellbeing instruction for children. But much of what is now happening under the guise of “mental health” is not in the best interest of children and their families. Organizations creating and delivering school instruction have profit as their primary goal regardless that their greasy PR claims otherwise.
Pharma/psych industry school “health” curriculum is ultimately designed to identify new customers for products and services. The multi-layers of misinformation and deceit have deep roots of collusion far beyond what most people could fathom. Unfortunately, the school blog series is just a tip of this bone-chilling iceberg.
As you aptly noted, it is akin to a horror story with the Pied Piper of Hamlin. But instead of a flute, he carries a gun.
Report comment
It’s Ridiculous, in my opinion.
I saw this on the BBC and thought you should see it:
‘Compulsory’ mental health education call to tackle suicide in Wales – http://www.bbc.co.uk/news/uk-wales-46277389
I had one suicidal hospitalization after another on Strong Psychiatric Drugs – the only reason I’m still alive is because I moved completely away from the Mental Health System.
Report comment
Thank you very much for writing this.
I think AKATHISIA is something Doctors + Medical Systems + the Pharmaceutical Industry are terrified of. Because in retrospect, a lot of patient fatalities, serious ‘acting out behaviour’, and longterm Neurological Disability can be traced to Drug Induced Akathisia.
My GP in Central London on October 12 2018 recorded on my records:- “..Has experienced akathisia with depot antipsychotics back in the early 1980s with extreme restlessness unpredictability , and ‘the most unpleasant feelings of his life’ Sensitivity FLUPHENAZINE DECANAOTE (all components considered allergens) – akathisia..”
… I had described Akathisia on a letter dated November 8 1986 to doctors in Ireland requesting ADR Warning be sent over to the UK (below):-
ADR Warning Request ltr Pg 1
https://drive.google.com/file/d/0B0zhbh8V4MBAZlVTbHdBRDFFSHc/view?usp=drivesdk
ADR Warning Request ltr Pg 2
https://drive.google.com/file/d/0B0zhbh8V4MBAZ0otNjFyN0NJajA/view?usp=drivesdk
ADR Warning Request Ltr Pg 3
https://drive.google.com/file/d/0B0zhbh8V4MBAcExwMzhEMVRzdm8/view?usp=drivesdk
In Response a “Mental Health Summary” dated November 24 1986 was sent over, but WITHOUT Requested ADR Warning.
My GP had been very courteous to me at the time, but afterwards, sent a letter to me dated October 17 2018 stating that I was to be removed from his list.
(… my GP has been very courteous to me since).
I think the NHS rule is that acknowledgement of AKATHISIA is to be completely avoided.
Report comment
I had a chance consultation with a neurologist 16 years ago because I was in excruciating pain and he informed me that I had the worst Akathisia he’s ever seen in this entire neurological practice (this man was in his 70s). The neurologist screamed in my face, “these drugs were killing you”. I was on Seroquel, 2 SSRI and two benzos. I had no idea what Akathisia was then. Below is part what he wrote In his medical notes about me.
“The overall presentation was startling in that she was constantly in motion with sharp jerks, twist, bands and more or less constant movement of the face, tongue and extremities. When this was pointed out she was able to control it to some extent but standing with feet together and arms out reached there was a constant piano playing movement of the fingers”.
After all these years later I’m still astounded how I was being destroyed emotionally, physically and neurologically by psychiatric drugs. Every time I mentioned one of these toxic side effects the psychiatrist would tell me it was my worsening mental illness. The Akathisia ignored.
Report comment
That is horrible! Especially when we can be pretty certain the psychiatrist at least observed these reactions and knew what they were. Though some psychiatrists are astoundingly ignorant about their own drugs. I am appalled, even with what I know about psychiatrists and their practices and have seen similar situations ignored. It is a criminal act.
Report comment
I got diabetes from psychiatric poison. Residual Akathisia absolutely. Sometimes people interpret my moving as nervousness but that’s not what it is.
It would almost be fun to put some Zyprexa in one of these quacks food or beverage so they could spend a day in Akathisia. Death has been reported after an acute overdose of 450 mg, but also survival after an acute overdose of 2000 mg. I think it would be “safe” to dose them with 100 mg.
You may be thinking what a horrible comment and maybe I need some psychiatric ‘help’ but what the hell I was told it was perfectly safe for insomnia and anxiety. The false information I was given before taking it makes what was done to me a poisoning. Martin Luther King famously said “An eye for an eye leaves the whole world blind” I disagree, I think at worst it only doubles the number of eyes put out. I think it would make going around hurting peoples eyes less appealing to those so inclined if they think they might get hurt back.
Would I poison that guy who gave me Zyprexa if I was given immunity from prosecution ? I don’t know but those psychos at Eli Lilly that lied and pushed that stuff I would have them locked up and fed nothing but food laced with 20 mg of Zyprexa till the day they were dead.
They poisoned millions of people worldwide and no one went to prison for that. Not even an arrest. I read the crime made them 65 billion in profit but only a 1.4 billion dollar fine for their criminal behavior.
Report comment
I think 100mgs of a neuroleptic should be a mandatory part of training. Nothing would be more likely to facilitate change.
Report comment
I write on here and other sites all the time that parents should should adjust for body weight and try their child’s ADHD and other psychiatry drugs on themselves first so they get a small clue what they are doing to their kids.
Report comment
And the psychiatrists and teachers and family doctors/nurse practitioners that prescribe should also be required to do the same.
Report comment
Absolutely – required to!
There is no way of making a person see aonther as fully human, or of installing a conscience in one who is seriously deficient or entirely lacking one. But for those trainees still in possession of a soul, it could make all te difference.
Report comment
I totally agree! Ignorance and arrogance is a deadly combination in medical professionals.
Report comment
Agree. Zyprexa (olanzapine) is THE most evil drug ever concocted. The akathisia it causes is pure hell and resulted in my attempted suicide. I suspect that even after close on 10 years since my last dose I am still affected.
If given immunity from prosecution I would happily force it on those doctors who forced it on me. When I complained about it to them and asked if they had ever taken it, their response was universally, “I am not mentally ill, and so it wouldn’t do anything”. I’d like to see them to prove that!
Report comment
I posted a link to this story https://www.psychforums.com/anti-psych/topic210460.html That’s how you spread the truth about Akathisia. Help make psychiatry’s dirty secret a household word. Post links.
I just got this at least 100 views over the next few weeks, if the other 670 people that read this before me posted a link worth 100 views…
Report comment
Urgent checks after fake psychiatrist practised in NHS for 22 years
“Zholia Alemi was jailed for fraud in October this year after she changed an elderly patient’s will to make herself a beneficiary.”
“The General Medical Council has apologised for “inadequate” checks made in the 1990s and for “any risk arising to patients as a result”.
https://news.sky.com/story/urgent-checks-after-fake-psychiatrist-practised-in-nhs-for-22-years-11557796
How many more. Jail is too good. How many lives did this woman ruin in 22 years? The punishment should be akathisia which she undoubtably caused to very many.
The GMC is a disgrace. I proved with the Health ‘Trusts’ OWN letters that I was subject to polypharmacy for three years in reply to my complaint which stated that I was not subject to polypharmacy. THE GMC IGNORED that evidence. Once you become a MH patient you’re just trash and trash to be exploited if you have money or valuable assets.
Report comment
More information on this appauling story… she gets 5 years in jail and will probably serve only half of that:
http://www.psychcrime.org/news/index.php?vd=2909
http://www.psychsearch.net/zholia-alemi/
Report comment
Just wish to say something about Brexit in the UK because things are getting rather toasty. The way the Tories (that’s Republicans in the US) are going we shall have a true Labour Govt before not too long. The Tories have historically torn themselves apart over Europe and it is playing out again. The Tory fools voted for a Prime Minister: Theresa May who is an EU remainer to deal with Brexit.. how stupid, and now we are facing a Hotel California deal from the un-democratic EU bureaucrats and they still can’t get rid of her, they still can’t decide who will be leader and get her out. Gutless headless chickens running around and Jeremy Corbyn awaits.
Report comment
They have to get rid of May now before the House of Commons vote around the 11/12 December …it will not happen.
How ever much Nigel Farage is an embarrassment of right wing nationalism, he was the one who championed what the UK public democratically voted for and should have been part of Brexit…a verbal ninja who went to Brussels and off-loaded all guns blazing with British sarcasm and directness.
‘Isn’t it funny’
https://www.youtube.com/watch?v=tQjWV9Bhc0g
Report comment
You know about the classic Mike Hodges film: Get Carter. Well we are living through: Get Mrs May.
She’s going to get us all here in the UK…who – the hell – can get Mrs May ?
Report comment
BBC R4 Today program reporting the UK Govt refusing to release the legal (binding) terms of Brexit and unclear what the other parties can force the UK Govt to reveal. The last time this happened was over Tony Blair and the Iraq war.
My view – if the US has the details they should be – very much in the public interest – leaked to Nigel Farage.
Report comment
Thank you for this. It does not take long for these drugs to cause permanent damage. But I don’t know which is worse: the neurological damage caused by psychiatric drugs or the psychiatric diagnoses that act like nuclear weapons dropped into a person’s life.
I had the interesting experience of managing to keep my psychiatric diagnoses out of my general medical records until just a few years ago when I had to apply for disability (resulting from multiple failed surgeries, another horror story). I went from being treated like a colleague, or at least an intelligent, knowledgeable, believable human being, to being subjected to outrageously disrespectful behavior from ALL medical personnel. I have 2 doctorates, one of which is a medical degree. I know more about the conditions affecting me than 90+% of doctors I go to. And yet now that my psychiatric diagnosis is plastered all over my medical records, I am treated like an imbecile, at best; a criminal, at worst.
My life has been put in danger, just like the author’s has, because of stigma, discrimination, and arrogant ignorance of medical professionals. It has gotten so bad that I will be leaving this country forever so that I can escape my medical record. How outrageous is that?? To have to leave the country to escape the death sentence of institutionalized discrimination dictated by a few words in one’s medical record…
Psychiatry, and in fact medical practice in general, have not advanced since the Nazi-era abuses. All the technological toys just hide the blunt truth. Torture by medication is now acceptable medical practice. Denial of medical care because of outrageous discrimination based on ignorance is obviously being taught in medical schools. In reality, this is a systemic problem in our society: hatred generated by fear of something/someone different. Until Homo sapiens evolves beyond limbic system domination over “thought processes”, nothing will change.
Report comment
maradel, as someone diagnosed with paranoid schizophrenia I definitely don’t think that the diagnosis in itself is worse than the damage caused by psychiatric drugs. I got my diagnosis more than 6 years ago, but I am able to lead a normal, happy and free life because I was on neuroleptics only for a short time.
Very few people know about my diagnosis, so it is not really stigmatizing to me. I am very glad that I never told anybody in my former workplace that I had been diagnosed with schizophrenia. Keeping this secret has been much easier to me than facing the consequences of “coming out”…
If your disability results from failed surgeries, why did you have to reveal your psychiatric diagnoses when you applied for disability? This is something I feared myself in the past – the possibility of being treated worse than other patients because of my psychiatric diagnosis. I am so sorry about the way you are now treated by doctors! But doesn’t their attitude change when they find out that you have two doctorates? (I am sure that my own PhD and my academic job made doctors and nurses treat me better when I was at a psychiatric hospital).
I think that migrating to another country is a great idea in your situation – wonderful that it’s possible for you! And you are right: fear of those who are different is surely one of the main reasons why “mentally ill” people are treated so horribly!
Report comment
My Dx ended up in my record at the Big Corporate University Medical Practice (that has bought up most of the independent medical practices in this state) by “accident”. My records from a previous doctor whom I entrusted with that info got sent to a doctor within the Big Corp Medical Practice. My previous doctor had retired and instead of his office having control over my records, the records of all his patients were turned over to some medical records management company that had no interest in being careful about what info got sent to whom. In fact, I didn’t even realize the Big Corp Med Practice had requested those records, but there was some signature on some paper somewhere that gave them carte blanche to obtain any and all previous medical records when I went through the grueling process of applying for disability!
It’s shocking how many people know my Dx without me disclosing that information. I was diagnosed with schizophrenia in the 1980s. I was a fairly prominent young neuroscientist at the time. The shrinks at the Big University Psych Hospital where I was incarcerated gave a grand rounds presentation featuring me, and colleagues of mine at that university ended up attending! That was the end of my career, in reality, even though I did continue to work. I try not to think about that very often because it makes me feel suicidal.
Never, Never, Never assume that you have any privacy in any aspect of your life, especially now with everything digital.
By the way, don’t assume that doctors appreciate smart, educated people. Most don’t, especially smart educated women who don’t let them get away with sloppy BS. They are very insecure and enjoy their massive power trips. I told one doctor I would have failed him in physiology if he had been in one of the classes I taught. I wasn’t always such a b*tch on wheels, but I finally gave up trying to be a compliant nice patient. Best thing I ever did.
Report comment
You are right, doctors are often threatened by intelligence and independent thinking.
I always give any doctor I have to see a preamble that I’m an intelligent person who will appreciate their ADVICE, but will consider it and do my own research and come to my own conclusions, which may be to refuse their advice completely, and if they have any problem with this, to let me know right now so I can seek another provider right away. It generally shuts them up pretty quickly.
Report comment
Thank you for explaining your situation, maradel. Fortunately I know for sure that doctors don’t know about my psychiatric diagnosis. And even if a doctor finds out about it one day, I am not worried because after my psychotic episode I had absolutely no contact with the psychiatric system for more than 6 years – doctors would probably assume that I must have been misdiagnosed or that I am a case of full recovery from schizophrenia.
No one knew about my diagnosis in my former workplace – I did not tell even my boss about it. Wherever I go, no one knows that I was once an involuntary mental patient.
In my own experience, some doctors have been clearly impressed by my education level and outspokenness. The head doctor at the mental hospital even lent me a book on the history of psychiatry and was very respectful towards me. Another doctor (a non-psychiatrist) not only likes me and respects me, but has once even shared with me an article from a medical journal! So fortunately there are doctors who don’t feel threatened by women with doctorates…
At the same time, I have to admit that I am trying to avoid conflicts with doctors unless I strongly feel that I have to stand up for myself. As to compliance, in my opinion a certain level of compliance is very wise in psychiatric hospitals. Thanks to my compliance I was not put into restraints and I did not undergo forced injections. Thanks to my compliance I was not really traumatized by my stay in the mental hospital. Sometimes it’s better to be compliant – it can even save our life…
Report comment
Yes. Fighting can lead to more drugs, longer stays, and shocks.
If you can quietly “tongue” or “cheek” without arousing suspicions that’s good. But otherwise take it. And never question anything told you–especially by the shrink.
It’s like being kidnapped and held hostage by bad guys with all the power on their side. They’re the ones calling the shots so you play by their rules till you can escape.
Report comment
maradel says, “They [doctors] are very insecure and enjoy their massive power trips.”
100% TRUTH.
Report comment
The first term that came to me as I read this story was “gas lighting.”
Acknowledging these pills cause these torments would be unprofessional and unethical. That would be “pill shaming.” Pills can never hurt anyone unless they deserve it (unmasking mental illness.)
“The meds never do that….”
They said when Anafranil kept me awake for 3 weeks in a row sending me into a psychotic mania I never experienced before or since.
They said when Risperdol made me gain 60 pounds in 3 months.
They said when Haldol made me seize with eyes rolling back into my head.
Escaped after wising up but it took 25 years and the damage is done. Pill rolling and mindless scratching. Could be worse. But my relatives scream at me for them when I stress out on visits. Stress makes it worse but they think it’s my “illness” and yelling at me will help since they believe I take my “meds” or they’d attribute my tics to being naughty. Everyone assumes seizures, tics, etc. come because you aren’t taking your “meds.” (Must be great to be that stupid since it means they never took these poisons.)
Horribly dishonest, manipulative, utterly lacking in compassion/empathy for those they hurt. The people who exhibit these behaviors the most love to “diagnose” them in others. Projection. Freud was right about some things.
Report comment
Rachel, how can your relatives yell at you? They are behaving in a very abusive way and they should stop thinking that your “illness” gives them the right to abuse you. This is emotional abuse of the worst kind! I would stop visiting people who are so abusive!
Report comment
It is a bad habit I wish I could stop. When it’s really bad I have scratched bald spots into my head. I try to stop but can’t. Wish they could understand but they think reminding me often enough should help. (Usually they don’t yell, but it does irritate them.)
Sad how family members turn on the “mentally ill” member they used to love. Thanks for alienating my nearest and dearest psychiatry. You helped a lot. 😛
Report comment
I understand, Rachel, but still they have no right to yell at you – it increases your stress, and I don’t think that it will make you stop… Maybe you could try to replace scratching by vigorously massaging your scalp with your fingers? But such habits are not unusual in any sense – my mum used to bite her nails until they bled when she was a young girl…
I think that your family members don’t realize that they are hurting you emotionally. Maybe they have not experienced healthy, non-abusive love themselves!
Report comment
I’m moving to a city where family doesn’t live and no longer stay at my brother’s house.
They’re not always that bad. The sad thing is with my MI “diagnosis” many folks view me as having symptoms instead of feelings. I had the same way of viewing my emotions till recently. All symptoms of my disease where most people have feelings and souls. They scared me so when I felt anything “too” strongly I would run to my psychiatrist for help numbing out the sadness/depression or the joy/mania.
Latuda made me very angry for no reason. When I told my shrink she tried to double the dose!!! Thank God my case worker managed to talk her out of it since my behavior was weird enough to scare her too.
Report comment
This is so corrupt and terrifying because so many of us believed we could implicitly trust doctors. We thought they actually cared and would honor their oath to “Do no harm”. There are still some around but they can’t save us from the rest.
I recently purchased “Chris Beat Cancer” written by Chris Wark. He writes of many egregious deceptions in conventional cancer treatments, including very misleading statistics on toxic chemo drugs and how doctors fear monger and coerce patients to comply and take toxic drugs that are ineffective and instead hasten or cause a person’s death. I experienced everything he writes of. As Chris states, “earning a medical degree does not make you a moral or ethical person”. It is devastating to discover that reality after we are harmed. Agree with Rachel777, these doctors have severe issues with lack of empathy/compassion, dishonesty, manipulation and delusions that they then project onto the patient.
Sending healing vibes and prayers there may be a path somewhere to healing that doesn’t include medical doctors.
Report comment
Well, I’m afraid it may be time for manganese supplementation. I’m also afraid you probably don’t live in the Bay area where a Richard Kunin, MD practices. One of his specialties is treating dyskinesias (of which akathisia is one) caused by psych drugs with manganese (and sometimes B3). He does have a web site, though.
Report comment
J.A. Carter Winward, your performance piece in your video is brilliant and remarkable on so many levels! Brava! You nailed it. I haven’t developed akathisia but it definitely sounds like hell on earth. I agree with a few of the other commentators that it’s criminal that prescribing doctors are not held to professional and legal accountability for not providing warnings to their patients. I was on an SSRI for twenty years and weaned off it three and a half years ago, thankfully. That was very rough but so worth it. I also was never given any warnings about how difficult it really would be to discontinue them. My doctors always told me they were harmless and non addictive and that I’d probably have to take them for life. I proved them wrong. I’m just so sorry you and so many others developed these horrible painful iatrogenic symptoms. Thank you for speaking out and for making such a powerful presentation in your video.
Report comment
It horrifies me to think of how many unfortunate people have lost years of their lives to this phenomenon –
The patient is given drugs that purport to ease their distress. But the drugs increase their suffering. This is assumed by an ignorant doctor to demonstrate that the patient’s condition is worse than he had anticipated. So the dose is increased, and predictably, the patient feels even worse. The process continues until the terrified patient stops saying anything and is severely disabled and looks like a classic “mental patient”, even to themselves. The pain is now unbearable. The patient is dependent on the system because they are now acutely “ill” and incapacitated.
Disabling/pain inducing drugs are continued. New drugs are added due to patient failing to improve. Friends abandon the patient and family members treat them as a sub-human lunatic as do mental health staff.
This was my story when I was a child. At this point I got out. How many in this situation either give up on themselves and accept their “fate” or kill themselves?
This is an industry with absolutely no objective mechanism to inform them that they are wrong about anything. I was once diagnosed with a serious medical disease. Luckily, the diagnosis had to be confirmed by blood test because the treatment would have killed me if there had been no way the doctor could have learned that the diagnosis was wrong. Real medicine, for all it’s faults, relies on objective data.
Report comment
Great comment! So good to know that you got out of the system of psychiatric drugging!
Report comment
But even within their own system, when the person gets worse, shouldn’t this indicate that they are barking up the wrong tree? I’ve pointed this out a number of times as an advocate, and always seem to get bafflement from the audience. It’s like observing that “treatment doesn’t seem to be helping” is some weird taboo! It’s not just that there is no objective way to determine success, they don’t seem to want to even THINK about whether or not their approach is successful! I find it utterly baffling!
Report comment
Yes out, “Real medicine, for all its faults relies on objective data”.
Psychiatrists make life altering diagnoses and order dangerous drugs/treatments for alleged diagnoses that have no objective data and are not factual, real or verifiable. Anyone can be a psychiatrist – the only requirement is that you can read so as to read the “DSM” and go “eeny meeny miny moe” and simply pick one (or more) of many made-up diagnoses of which most have overlapping alleged symptoms. It’s like a game, a total crapshoot – but one that is playing with people’s lives.
Report comment
This seems pertinent to this discussion, right out of the recent issue of Psychiatric Times:
http://www.psychiatrictimes.com/mental-health/mental-illness-will-cost-world-16-usd-trillion-2030
“A new Lancet Commission report on mental health said that mental disorders are on the rise in every country in the world and will cost the global economy $16 trillion by 2030. The economic cost is primarily due to early onset of mental illness and lost productivity, with an estimated 12 billion working days lost due to mental illness every year……
The report shows that in many countries, people with mental disorders still routinely suffer gross human rights violations—including shackling, torture, and imprisonment. Bringing attention to these kinds of abuse and discrimination, the Commission calls for a human rights-based approach to ensure that people with mental health conditions are not denied any of their fundamental human rights—not just to health but also to employment and education, among others.”
Now, I don’t mean to detract from attention on human rights violations perpetrated against people with “mental illnesses” in some third world countries, but there are many of us within “first world countries” who have suffered gross human rights violations, such as painful restraints, torture by medication and medical devices (ie, ECT), sexual assault, and imprisonment.
The members of this special Commission need to look right in their own backyard, in their own psychiatry training programs, within their own oversight of acceptable psychiatric practices and do a whole lot of house cleaning.
What a bunch of cynical bloviators.
Report comment
Quite so. I also wonder how folks can read that the amount of “treatment” is dramatically increasing worldwide, and yet the “burden of mental illness” is also increasing lockstep with increasing “treatment.” If the “treatment” worked, shouldn’t the “burden of mental illness” be dropping? What happened to our new technological understanding and wonder drugs? At what point does the obvious question rise to the surface: “What are we doing wrong?”
Report comment
Its the patients fault for being treatment resistant …
Report comment
But of course! But calling it “treatment-resistant depression” or whatever even takes that level of agency away from the patient. They couldn’t HELP resisting! They were powerless to their “depression” which is what resisted! Imagine, a concept resisting a drug! It is beyond ludicrous, but they get away with it. Why not just say, “My treatment failed” or “I don’t know how to help you?” At least that keeps alive the idea that someone else might have a better idea.
Report comment
“Why not just say, “My treatment failed” or “I don’t know how to help you?” At least that keeps alive the idea that someone else might have a better idea.”
But Steve, that’s too rational!!
Report comment
Sorry, I got too excited…
Report comment
Good point. RW has already pointed this out.
Also, if more psych drugs were the answer to mass shootings, why were these shootings not a “thing” till the 90’s? Back in the 60’s all they had were thorzine and a few other drugs they seldom gave unless you were totally out of it and maybe violent. Shouldn’t 0 psych drugs mean more mass shootings than today if they were the answer?
Report comment
A point which seems to bypass the media at every opportunity they are given to observe it.
Report comment
With all their drug company sponsors why should they observe it?
The few journalists who criticize psych drugs are on Youtube instead of MSNBC, C-Span, or FOX. Big Pharma owns TV and this is evident in the shows–not just the countless drug commercials.
Report comment
Only one drug that I took, Seroquel, has caused horrific akathisia and tardive dyskinesia and tardive dystonia. I have constant spasms in both my feet and can’t drive anymore because of this. Is there any hope that this will ever be healed?
Report comment
Some people improve over time, but apparently some do not. I’d advise talking to other people who were victimized in this way, and see how they have learned to deal with it. Professionals are not going to be a lot of help here, unless it’s a dissident professional who is willing to admit to how TD is caused and to really work to find solutions. Alternative medicine might also be an option, though I’ve never explored that avenue specifically regarding TD.
Report comment
I’m a couple decades out from the intense polypharmacy of psych drugs inflicted on me, including injectable depot haldol. Intense, intense misery. I still suffer bouts of akathisia, and it can be triggered by “non-psych” medications, or for no obvious reason. Of course, many people don’t realize that many “non-psych” drugs do enter the brain and have effects, even some antibiotics.
I finally spent the money to go out of network to a doctor trained in both internal medicine and integrative medicine. Very smart woman who thinks outside the box. She ran lots of tests (Genova Diagnostics has some excellent tests that provide a much more comprehensive metabolic and endocrine profile). The whole thing was interesting, but one that stood out and shocked my very experienced MD was that I have extremely low levels of dopamine metabolites in my urine. She told me that she only sees that in her patients with severe Parkinson’s Disease! Of course there are potential explanations other than low dopamine production in my brain, but my symptoms correspond to low CNS dopamine production. Shocking and terrifying.
Also, I have bizarre paradoxical reactions to preanesthetic and anesthetic drugs that a very experienced psychiatrist told me he had never seen in 30 years of practicing psychiatry, but these are the kinds of things that happen when your neurotransmitters are totally screwed up.
There are reports in the medical literature documenting permanent brain damage by neuroleptic drugs. Psychiatrists prescribe these and other psychopharmaceuticals in combinations that defy rational thought processes. Throw a little (or a lot) of ECT into that mix and it is nothing short of medical malpractice.
The field of psychiatry is trapped in it’s own delusional world view and psychiatrists are causing widespread, intense suffering…and death. The fact that they have created this delusional world view to boost their financial bottom line makes it criminal.
HOWEVER, psychiatry is not the only field of medicine that indulges in intentionally delusional thinking in order to hide massive financial conflicts of interest. Take a peek behind the curtain of implanted prosthetic devices and you will find the same morass. As one who has had 7 failed hip replacements, accompanied by heavy metal toxicity, tissue and bone destruction, and nerve damage, I have personal experience wading in that swamp.
Report comment
Oh, I should add this comment based on the riff above on “it’s the patient’s fault”
The last orthopedic surgeon I consulted about the worsening pain and dysfunction in my hips told me that I would have to have them both replaced again. That would make NINE total hip replacements. I can’t even get my head around that. When I tried to have a discussion with him about the culpability of defective prosthetic devices causing these repeated failures (BTW, I have no pending or planned lawsuit over any of that), he denied that that could possibly be the cause and then said:
“THERE MUST BE SOMETHING WRONG WITH YOUR PHYSIOLOGY”
BWWAAHAHAHAHAHAHAHAHAHA
Report comment
Wow, YOU caused their devices to fail! You appear to be VERY powerful!
Report comment
i wonder if the fake psychiatrist was any worse than the “real “ones ??? watching someone with akathisia who cannot sit for even one minute and being completely ignored by the trick cyclist “it’s just the psychosis lets increase the drugs and add in beta blockers,benzos and sodium valporate…oh and temazepam and 2 anti depressants.. that was the end of our faith in any psychiatrist or engagement with ‘services’ so it was actually a good thing to see him in all his glory that early in the piece and again i wonder if the fake one could’ve been any more cruel,indifferent or manipulative….
Report comment
Even if you manage to shake off a mental illness label…you might be surprised about how little “healing” goes on in western medicine. They were ready to cut my thyroid in half that maybe has a centimeter large tumor. My fiance got put on more and more blood pressure meds that did nothing. I’m starting to understand why my highschool teacher avoids doctors.
Reiki, diet, cats, my fiance and his family have helped me heal a lot.
Report comment
🙂
Report comment
I believe you and know that you are telling the truth. The way you were injured and decieved, gaslighted, blamed, and ignored is horrible and unacceptable. I was also permanently maimed by SSRIs; and am still dealing with the psychological trauma of the horrible mental state that akathesia puts people in; my best friend from school killed herself while akathesic. You are doing a public service.
Report comment
JA, I read and viewed everything on your site. It made me want to cry.
I hope your prognosis is wrong and you get better. 🙁
Your daughter needs a new doctor. Soon!
Report comment
For the love of God, start taking Gabapentin at high doses. Doctors will prescribe it like candy.
If that doesn’t work, then take Mirapex.
It’s for Restless Leg Syndrome, but Akathisia is an advanced form of RLS.
Report comment
Rcarpane,
Respectfully, and “For the love of God,” please start researching medications like “Gabapentin at high doses.”
Anti-seizure meds can actually worsen neurological damage that’s been done by psychotropic medications. I know this because I’ve taken them, and that’s was my experience.
While “doctors will prescribe it like candy…” I assume you are not. A doctor, that is. And doctors handing medications out “like candy” is the reason most of us are in pain and have severe neurological damage.
“If that doesn’t work,” perhaps you ought to stop reading about akathisia, since it seems to vex you…
Mirapex is also a side-effect nightmare and I’m not willing to risk further pain and damage by submitting to a guessing game.
As for RLS, the pathophysiology might be similar to akathisia, but that is not the same as an “advanced form.”
Example: an advanced form of “mild chiding” would be “sarcasm,” yet many people confuse irony and sarcasm all the time.
And while it’s ironic you wrote two identical comments on two very different subjective experiences of akathisia, (this article, and the poem by Marci Webber on this site called “Psychotic Akathisia”) it’s also ironic that your comment(s) seemed to miss the thrust of both our pieces, while providing reductive answers to questions that were not posed.
You see, this article is not about how to best treat or medicate akathisia, it is about the wanton disregard specific medical professionals displayed when I presented with drug-induced neurological movement disorders, specifically tardive akathisia, their attitudes toward me, along with their lack of relevant knowledge about how akathisia presents individually and subjectively.
So, in relation to your comments, Ncarpane–THAT is irony in it’s most sublime form:
Your comment(s) show a wanton disregard toward our experience and words and then you threw out the names of more brain-altering medications–without the relevant knowledge to do so–as if they were candy.
Which, of course, they are not.
Sincerely wishing you peace–
J.A. Carter-Winward
Report comment
Thank you for this very informative article. I never heard the term akathisia during the decades I spent in treatment.
I was treated with benzos and SSRIs for “treatment resistant depression” then, when I got worse, with Adderall, then, when I got psychotic, ECT, then, when the ECT didn’t “work”, I was told it was because I had borderline personality, so more SSRIs and now mood stabilizers and antipsychotics (one kind psychiatrist told me that Abilify would “heal” the problem in my brain that caused the borderline), then I could no longer work, went on disability, spent the next five years in and out of Yale IOP and Yale psych ward, I was severely anemic but no one noticed as Drs wrote “patient is thought to have poor judgement” and so much worse in my chart, I started self harming, had briefly become addicted to methadone while trying desperately to hold on to my job, so methadone withdrawal, more antipsychotics, higher doses (why is she so angry??), throw in an SNRI, some Geodon, Lamictal (if you break out in a rash let us know; otherwise you can assume “your” meds are working against your powerful, intractable, innate severe mental illness), now an MAOI which led to hypertensive crisis (“just try not to make yourself hysterical”), Latuda, the new and improved Abilify, hospital, hospital, hospital, garbage patient borderline recidivist, abandoned by family and friends, spit out of the system.
No one ever mentioned akathisia. Every time I said “iatrogenic” the understanding DBT clinicians would point out, “That’s not helpful” (treatment interfering behavior, urge to argue, please make a star on your diary card).
Unbelievable.
Report comment
Another psychiatric success story! How can these people not see when their “treatment” fails utterly? In what other profession are the professionals allowed to blame their failure on the person/machine/process they are supposed to be fixing? “The bridge collapsed because it was a span-resistant river.” “We couldn’t fix your breaks because they are repair-resistant.” “You were poisoned because our chef had the misfortune of serving health-resistant food.” Come on, who the hell else would ever get away with it?
Report comment
The food was fine. Our chefs can do no wrong. You only got food poisoning because of your defective digestive system.
Report comment
Oh, right, you have Toxin Oversensitivity Disorder. Not EVERYONE gets sick from eating our food – it must be YOU have a problem!
Report comment
When I had an ongoing (months-long) hypertensive crisis as a direct result of being put on Parnate, they did use this kind of twisted logic with me. First they said my BP had shot up to 170/140 because of my age (“welcome to your 40s, you have hypertension”), then they said it was because I had violated the restricted diet for people on MAOIs (I hadn’t, but that didn’t stop them from writing in my chart that I had). Finally, they declared that I had an innate, underlying case of hypertension which was “revealed” by the Parnate. I told them, that’s like, if I punch somebody in the face, and then tell them, “you had an innate, underlying black eye. I just pointed out with my fist.”
A few months later, the Dr who’d prescribed the Parnate said, “I don’t know, Kate, maybe you just really get to people.”
They don’t like being called out on their idiocy, that’s for sure.
Report comment
I LOVE your “underlying black eye” theory! I’m totally going to steal that.
Do you mean at the end that they are blaming YOU for being mistreated because you get under people’s skin???
Report comment
Thanks, Steve. I was proud of that one.
The psychiatrist who said that to me, about me getting to people, this was at the end of 5 years of hell they put me through starting with ECT, the BPD diagnosis, many hospitalizations (all traumatic), dozens of different drugs. During that 5 years I lost basically everything that I cared about.
So I was sitting in this Drs office at the IOP, and I think he could see how hopeless I was, and he wanted to say something but I guess didn’t have much to say, so he mentioned a ketamine study they were doing at Yale for depression. He said maybe I could try to get into that study.
I knew I’d be excluded from the study due to the bpd diagnosis, and I was pretty sure the Dr also knew this (it’s common practice to exclude “borderlines” from depression studies) so I just said, “Hey, it’s a chance to get high.”
That’s when he said “maybe you just really get to people.”. I was so broken at that point, it didn’t even hurt my feelings. I just didn’t care.
Report comment
No point in being upset about comments from those with no credibility.
So sorry you had to deal with this hell!
Report comment
Thank you, Steve. I actually had a good relationship with that Dr in the beginning, but he prescribed the Parnate and when I had the severe hypertension even after they stopped the drug, he could not or would not admit that the Parnate had anything to do with it. Any time they came close to admitting the connection, it was still always about what I’d done wrong, like saying that I’d violated the diet. They just abandoned me to deal with the medical crisis on my own. Even the Drs and therapists that I had a good relationship with in the begining – every time, something like that would happen, they’d show they were loyal to the system, not me…then they beat me over the head about my problem with not trusting “the people who were trying to help me.”
I should write a book. We should all write books.
Report comment
Why should you automatically trust them? Isn’t trust earned by trustworthy behavior? Isn’t one of the “deficits” of “borderline personality disorder” (as they frame it) a difficulty deciding who can and can not be trusted?
It is clear that these people don’t really know what they’re doing, and they get very insecure when anyone starts making it clear that they don’t, they get defensive and start blaming the person telling them the truth. It’s like The Emperor’s New Clothes! Lord help anyone who points out that the King is naked!
Report comment
Patient led study would be interesting.
Report comment
J.A.
What can I say, but I am sorry.
I am sorry for what the practice of psychiatry and the medical field has participated in.
They left a lot of animals wholly damaged, to be put to death, while they watched drugs wreck havoc, which they then passed on to the drug approvers.
Two legged animals then become the next experiment, but since we can talk, they simply ignore.
There are no words that will ever make a difference to them. Them is whoever is part of the lies and destruction.
No point in pleading with anyone. Many in the past have pleaded with accusers, it does not work.
The actual mental illness only ever existed in the inability to see their twisted self protection.
It is life wasted to spend one second in trying to reach psychiatry or other doctors who are in self protection mode.
They could not care less about the killings they were part of. It is in their genetic makeup
Report comment
Wonderful article. Akathisia (one of the many strains of EPS) can be horrendous, especially when it is met with no compassion.
The cognitive bias of many psychiatrists borders on pathological. Short story on the subject: my pain started about a year prior to getting off meds (Clozapine); I made the decision to stop only to be met with an unsubstantiated statement by my MD that “going off the medication brought a much higher likelihood of relapse” (I asked for the study he was referencing and he said he didn’t know of one…); my withdrawal from the drug was not pleasant; the EPS lasted and still lingers a bit; I made a point to have 2 phone calls specifically about the EPS symptoms with him, and he didn’t ask one follow up question on the subject – rather he moved on to ask if I had any psychotic recurrences and if my wife thought I was ok; he not only didn’t recognize the severity of the pain/disability, nor show compassion, but he seemingly ignored it; I grew perturbed; after the call, I requested my medical records to see his notes; no mention of the pain or EPS (just that patient wanted to stop pharma due to side effects.)
My MD presents as a nice man and I liked him on first impressions. I now see him as a myopic drug dealer with little true compassion besides the algorithm he calls treatment. Ahh, if I had more time….
The system is broken in many ways and I’m so pleased to see the alternatives being touted more, at least from the outside.
Report comment
Your story is so disturbingly familiar. I had multiple psychiatrists over a 15 year stretch when I was being treated for borderline personality disorder. Some of the psychiatrists were just arrogant, demeaning and callous from the outset, but there were others who seemed pleasant, caring…a couple who even seemed to actually care about me as a person and who, I still believe, really wanted to see me doing well. The common denominator between all of them was that not one ever attributed my often extreme agitation, accompanied by suicide urges, to the drugs they were prescribing. Those episodes, which often landed me in the psych ward, were always put down to my “severe mental illness” and repeated “failure to utilize coping skills”. None of these doctors ever told me – or probably any of their patients – that the drugs they were prescribing could cause a not-rare condition called akathisia.
In retrospect, I think the psychiatrists who seemed caring at the outset caused more pain than the ones who didn’t — I was devastated when they each, in turn, gave up on me. Now I feel a huge sense of betrayal and a lot of rage.
Report comment
Removed for moderation.
Report comment
I havnt read the whole article but this condition was enough to make me want to end it. I was given strong anti Ps when I went to ED sometimes, often for nausea but occasionally later on I’d try some mild ones for depression & sleep.
It took me YEARS to figure out what on earth was making me feel beyond terror, horror, anxiety because I couldnt think of a word that existed for how horrible I felt & what I felt. I didn’t even get much movement issue, I got a feeling lije no matter if I sat, lay down or stood it dodnt help, that made me feel worse as there was no escape (usually one of those things helps conditions ease a little). I woukd Google vague things but nothing came up for years, it wasn’t till I correlated a med given to how hideous I felt for a week+ after being given it that I found the word for this condition, but like you drs looked at me like they had no clue what inwas talking about & didn’t believe me, at least how bad it was. I’ve NEVER experienced anything so hideous to endure & if I was ever told I had to live woth it forever I’d end myself asap. The last time it happened with a med I was trialing and I didn’t really click until the 2nd dose it was occurring (it was a low dose) but after the 2nd dose I wanted to d1e I felt so bad. I had to keep texting someone and looking up the half life, the friend kept having to tell me it would only last x amount more time but that felt like forever as far as i felt. I now tell hosp and drs I’m “allergic” to anti Ps because explaining the reality is just too difficult & inwas never told what they wete giving me & won’t risk that again. This condition is so terribly understood, I’ve spent alot of time in psyc wards due to depression etc & I believe what I see in many psychotic patients is akathesia which the poor souks have no chance explaining to a dr. I feel so so bad for them because even if they coukd thed still be injected etc with the med.
Report comment