This week Mad in America Continuing Education is launching a course on “creating system change,” and while marketing it to national organizations, we have been reminded anew that even though the societal discussion around psychiatry and its treatments has changed dramatically in the past twenty years, systems of care are—for understandable reasons— resistant to actually changing their practices.
The inventor Charles Kettering, who was director of research at General Motors from 1920 to 1947, summed it up this way: “People are very open-minded about new things, as long as they’re exactly like the old ones.”
We have close to 100 people signed up for the course, and we are encouraged by that. But when Bob Nikkel, the director of MIA Continuing Education, conceived of this course, we had set our sights on “reaching beyond the choir” and getting larger provider organizations to promote the course to their members. We were dreaming of an audience of 500 or more. I suppose that we had let our optimism get ahead of our grip on reality, but this occurred because it seemed that there is now a growing societal understanding that our current mental health system, from a public health perspective, has failed.
Markers of Failure
From a public health perspective, there are many findings that tell of the failure of our current paradigm of care. Here are just a few:
- The burden of mental illness has dramatically increased over the past 35 years, such that “neuropsychiatric disorders are now the leading cause of disability in the United States.”
- The number of adults on government disability due to psychiatric disorders has increased from around 1.25 million in 1987 to more than 4.5 million today.
- The suicide rate in the United States has been steadily increasing over the past two decades.
- More than 20 percent of the prison population is said to be suffering from a “severe mental illness” (up from .7 percent in 1880!).
In addition, research on the long-term outcomes of people treated with psychiatric drugs tells of a failed paradigm of care.
- Long-term recovery rates for schizophrenia patients have worsened since 1990, and are now the lowest they have ever been since the diagnosis was first constructed more than a century ago.
- A number of studies of schizophrenia patients in the current era have found higher recovery rates for unmedicated patients.
- Affective disorders—depression, anxiety, and bipolar disorder—run a much more chronic course than they did in the pre-antidepressant era.
- A number of long-term studies of depressed patients have found worse outcomes for the medicated patients.
Together, these data tell of both a public health failure and a therapeutic failure. They cry out for change.
The Supporting Story of Science Has Collapsed
Our current paradigm of drug-centered care, for a diverse group of diagnoses, took hold in the 1990s, and did so in response to a story told jointly by the American Psychiatric Association and the pharmaceutical industry. The public was informed that schizophrenia, depression, bipolar, ADHD and so forth were diseases of the brain; that these diseases were due to chemical imbalances in the brain; that psychiatric drugs fixed those imbalances, like insulin for diabetes; and that a second generation of psychiatric drugs had come to market that was much superior to the first generation.
All of that told of a golden age of scientific discovery and therapeutic advance. Yet, that story—at least in research circles—has now utterly collapsed.
- The brain-disease story: The diagnoses in psychiatry’s Diagnostic and Statistical Manual are now understood as “constructs,” which group together people with somewhat similar symptoms. The field still lacks biological markers for diagnosing distinct brain diseases.
- The chemical imbalance story: This story has been tossed into the waste bin, and so thoroughly that Ronald Pies, former editor-in-chief of Psychiatric Times, has written that “in truth the chemical imbalance notion was always a kind of urban legend, never a theory seriously propounded by well-informed psychiatrists.”
- The second-generation story: Prozac and other second-generation antidepressants are understood to provide, at best, a marginal benefit over placebo in the short term. In government-funded studies, the second-generation antipsychotics were not found to be any more effective than the first generation.
So we can now see a one-two punch for change: The story of “science” that led us to adopt a drug-centered paradigm of care has collapsed, and there is ample evidence that this paradigm of care has proven to be a public health disaster.
Resistance to Change
Since psychiatric care is seen as medical treatment, it is psychiatry, as a medical specialty, that establishes the “evidence base” for what should be done. Psychiatrists write the texts, set clinical care guidelines (for standards of care), teach the Continuing Education courses, author the research articles, and so forth. Providers are under strong pressure to conform to those standards, and thus change in most real-world settings needs to come from the top.
There are many individual psychiatrists who are championing the need for change in their field and working in new ways. However, psychiatry, as an institution, has not shown much interest in reflecting on the failures cited above.
The history of medicine repeatedly tells of the capacity of doctors to be deluded about the merits of their treatments, and thus to unwittingly do harm. To best serve its patients and the public good, a medical discipline needs to have an open mind regarding the merits of its practices, and the capacity to respond to evidence that one of its treatments isn’t effective, or even worse, is doing harm.
Unfortunately, American psychiatry—as an institution that sets standards of care—has not demonstrated this openness of mind. Psychiatry has long had something of an inferiority complex in relation to other medical disciplines, and in the post DSM-III era, its leaders have regularly responded to criticisms with a mixed sense of outrage and self-pity. Those who would criticize its treatments are often dismissed as being “antipsychiatry,” which is to say that their criticisms are driven by ideology and not any reasonable review of science. Is there any other medical profession, its leaders lament, that has to suffer such insults?
Here is Jeffrey Lieberman, former president of the American Psychiatric Association, speaking before Congress in 2015, pinning the blame for a failing mental health system on its critics:
“Stigma of mental illness is pervasive in American society and is actively perpetuated by a virulent Anti-Psychiatry Movement. Psychiatry has the dubious distinction of being the only medical specialty with a movement dedicated to its eradication. (There are no anti-pediatrics, dermatology or orthopedics movements.) This movement is comprised by diverse constituencies who dispute the concept of mental illness and way to treat them including Scientology, the latter being motivated by financial designs rather than ideological reasons.”
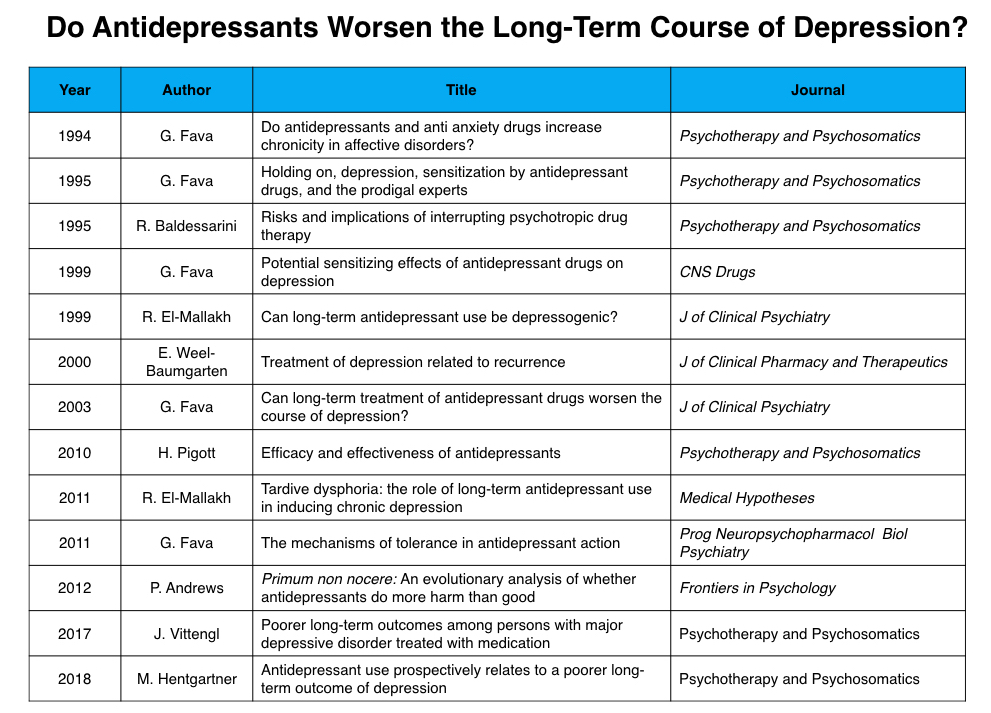
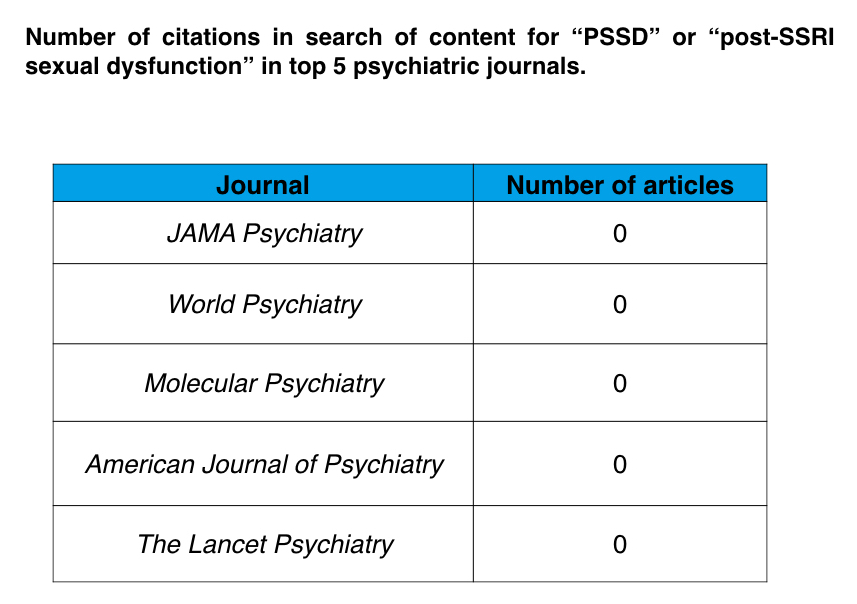
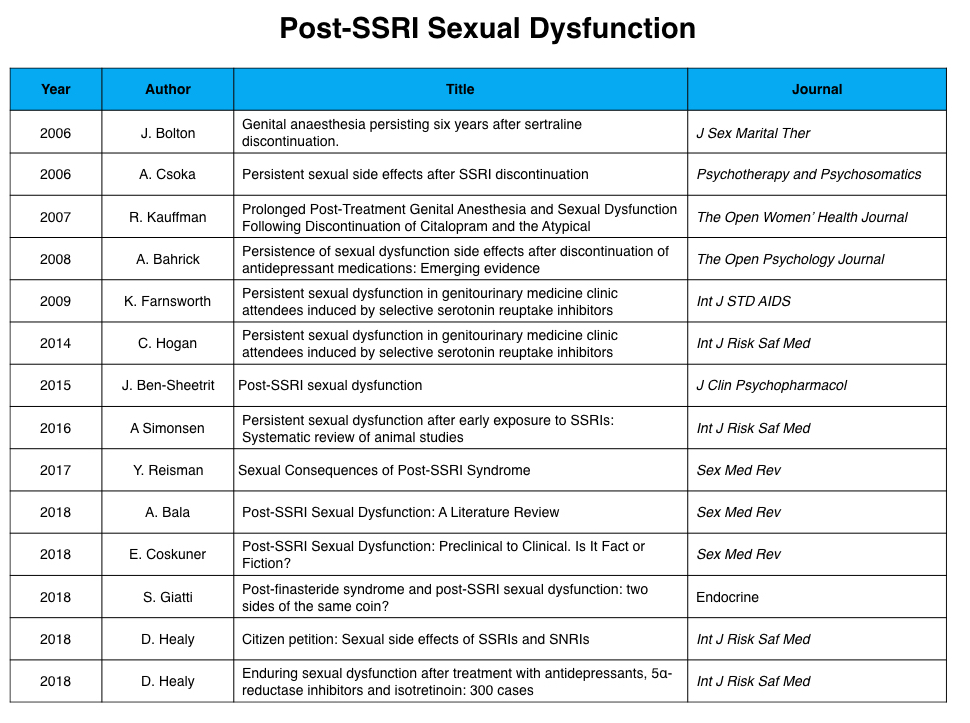
This past spring, I was invited to present at a conference on scientific integrity organized by Peter Gøtzsche and others, and as part of my presentation, I investigated whether the top five psychiatric journals, in terms of their impact, had ever published articles on two issues of concern with the use of antidepressants. Do these drugs worsen the long-term outcomes of depression? To what extent do they cause PSSD: post-SSRI sexual dysfunction?
I could not find any mention of these two concerns in any of the five journals. Research findings on these two issues, which are of such obvious importance to informed use of these drugs, could only be found in less prestigious journals.
While these are topics that had been addressed in MIA Continuing Education webinars, I am pretty certain that there have been few, if any, CME courses offered to psychiatrists through mainstream channels that have ever addressed these concerns.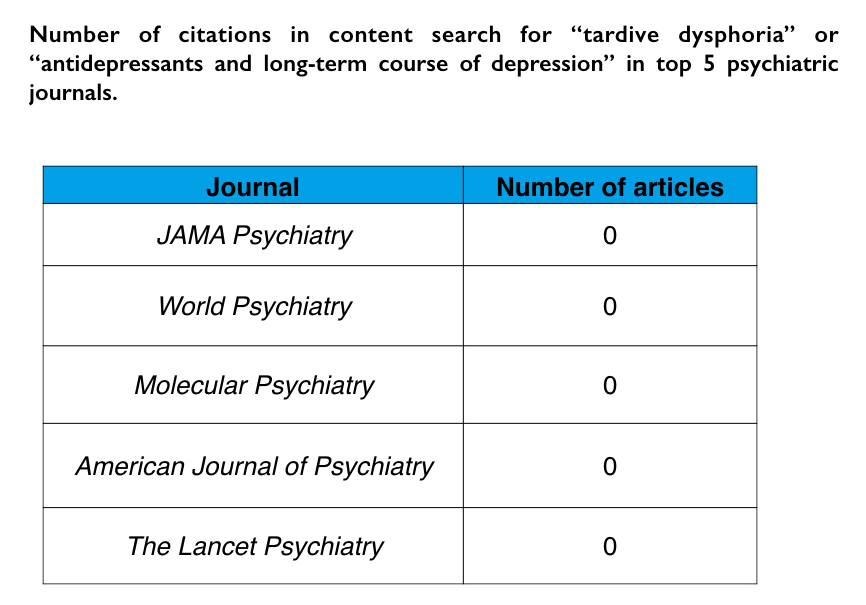

Providers in a Quandary
Without a mandate for change coming down from a governing medical specialty, it becomes nearly impossible for care providers to embrace systemic change. They may adopt new programs that add on to usual standards of care, or develop a more welcoming environment for their patients, but insurance companies are going to want to pay for the first-line therapies set forth in clinical care guidelines. Add in the usual resistance to change in most any organization, and it is easy to understand why providers of mental health services would be resistant to even hearing about ideas for “systemic change.”
That, I think, sums up the current status of psychiatric care. The story that was used to expand the psychiatric enterprise in the 1990s and early 2000s has collapsed and there is ample evidence that our current paradigm of drug-centered care has failed, but the medical specialty that oversees this realm of care has not shown any willingness to investigate or even acknowledge this failure. As a result, providers just keep on doing what they have been doing, which of course puts psychiatric drugs at the center of care.
Our Mad in America Continuing Education effort is, I know, a small enterprise. We are like a little gnat buzzing around a great big elephant that can be swatted away with a quick flap of the ear. But our new 10-session course will at least explore this landscape of “systems change,” with the presenters bringing to this topic a diversity of experience and perspectives. The presenters include psychiatrists, leaders in peer services, former directors of state mental health programs, and trainers experienced in helping providers implement trauma-informed care.
And how does the saying go? You change the world one mind at a time? We like to think of our newest course in this way.















As always a great article. I thought we had a chance to change the paradigm when Obamacare embraced the model of mental health care being integrated into primary care. In primary care, it might have been possible to skip diagnosis and screen for happiness. Interventions for those deficit in positive moods would consist of yoga, dietary interventions, and support groups. Over at Emory psychiatry, they were even predicting that there would not be much future work for psychiatrists.
I’ve been less than happy with attributing suffering to past trauma. This perspective has resulted in treating everyone as if we were all fragile. Now we announce/warn in our university classes when sensitive topics might be discussed. This has led to criticism from social psychologist, Jonathan Haight.
Anyway, maybe there is hope after the next election for the return of Obamacare and integrating “mental health” into primary care. It’s my hope that we can lose the term “mental health” and all the labels including trauma.
Report comment
That sounds good in theory Jill. But it seems the integration of “mental health” into primary care just means more GP’s handing out SSRI drugs.
Do you think the high numbers of young adults on psych drugs could be a factor in the lack of emotional resiliency on campuses?
Report comment
Dr Jill,
Yoga and support groups, what’s all that about?
Dr Rufus May
https://en.wikipedia.org/wiki/Rufus_May
Advises distressed “schizophrenics” to go out for a walk!
A friend of mine that attends a “support group” said that if you gave a psychologist £50 or £100 and he told you to go home and iron your shirt you’d feel taken advantage off ( – but this is what works).
I came off LAI drugs suitable for “schizophrenia” with straight forward CBT/Buddhist Mindfullness Practice.
If I calculate my 4 grandparents age span years ago in Ireland, on average they lived to their mid eighties with little medical help.
Report comment
“[Rufus May] Advises distressed “schizophrenics” to go out for a walk!”
And those stressed out by constant walking and roaming are advised to go indoors.
So really, we should all be mindful about when we go outdoors and when we remain indoors. And we should, as much as possible, allow life to flow through us, and our thoughts also to flow through us. Because there are only thoughts and impressions. And they flow through us. Or seem to. Given that our being is a sophisticated illusion.
These days most people go out through staying indoors, and experiencing outdoors through screens, in which they explore new worlds. When outdoors they lose themselves in portable screens that enable them to maintain indoors attachments.
Strictly speaking indoors and outdoors are eaxctly the same thing. Much like up and down. And dead and alive. Nothing whatsoever is fundamentally altered, other than perception.
The best discoevered place to get away form it all is likely the moon. It would be interesting to float off the planet one day and venture off aimlessly in a random direction.
Having a mind is burdensome, tiresome. This is why we invented the written word. It’s superior to actual consciousness, which, by the by, is a complete mess.
Report comment
Okay
Report comment
And for those for whom yoga, support groups and a change of diet make little difference?
This perspective is part of the problem in my opinion. Changing from one faulty paradigm to another might result in less harm, but what if there is no universal panacea for human suffering?
It feels to me as though there is an element of winning a competition in this – your perspective is wrong and mine is right. Minds close.
This seems to be mimicking the model of medicine of finding and applying the correct remedy. But medicine relies on theories about the body, what it is, how it works and what goes wrong. Where people have problems with their bodies that don’t fit existing understandings they are blamed and discarded. Will this be how providers of Yoga and dietary interventions respond to those whose suffering is not amenable to their treatments? Isn’t that one of the reasons we collectively choose to warehouse unwanted, and/or problematic people?
Suffering and problems of living encompass every aspect of existence. While adherents and believers, particularly those providing services related to niche markets might be gratified if their understanding and solutions were validated and resourced, no theory or belief system has shown itself to fully understand the questions, let alone provide universally successful solutions.
Report comment
I agree with this thinking 100%. The primary error in the DSM is the assumption that all depressed people are the same, all anxious people are the same, all hallucinating people are the same… these assumptions are absolutely not true, and there is no reason to suspect they would be. Some people who are depressed love meditation! Others find it completely useless or damaging. Same with CBT, regressive therapies, micronutrients, etc. Every person’s needs are different, and what will help is different, too. There is nothing to suggest that all depressed people will be helped by the same approach.
Report comment
The primary error in the DSM is that it exists.
Report comment
You don’t have to be “fragile” to be devastated by childhood sexual abuse or rape or systematic bullying or neglect/abandonment by one’s parents, etc.
Report comment
I agree. You simply have to be human to be affected by these.
And how about instead of suggestive labels like “fragile,” put on those who have been victimized and betrayed (which I know you are not doing here, Steve, I’m saying this in general, it’s unfortunately common to attribute “fragility” to victims of abuse who claim post traumatic stress from abuse), we put the attention on the ones doing the abusing, who are, in reality, the fucked up ones because they are doing harm to others outright, and that’s more than merely a suggestion. It’s a fact.
Report comment
I agree, and that was actually my point. It’s not “fragile” to need and want safety and agency in one’s life. It’s a normal part of being human. What is abnormal and unfortunate is when humans intentionally take away other humans’ safety and agency in order to profit or dominate others. We should, indeed, be focused on stopping abusers instead of accusing their victims of “fragility.”
Report comment
Yes, you say it perfectly! That is the shift in focus needed, entirely, without question. And that would be a community issue, to not enable it, to not agree with it, and to not fear calling it out.
If calling out abuse in the moment were to be unequivocally supported and seen as courageous and strong, and worthy of note as a red flag, then that would indicate a sound, just, safe, and balanced community. As it is now, coming forward to call out abuse, injustice, etc., one risks being shamed as whiney, thin-skinned, and fragile, and I guess lately, “snowflake” would be added to the list.
That’s why they call it courageous, but at the same time, it is the essence of, both, dysfunction and social injustice–one person vs. an entire scapegoating community, all banding together from fear, oppression, and some kind of co-dependent need. That happens when one person’s truth is being highly resisted, to the point of cover up.
Why, I would wonder? What is so threatening about that one person’s truth, who becomes a scapegoat? Maybe because it IS the truth that no one wants to see because it will create too much of a challenge to change on a core, systemic level? I guess there would be a power shift, and that’s too scary to even think about–well, for those in power, at least!
I think, perhaps, these are viable reasons for dysfunction/systemic abuse to be so damn stubborn. It’s easier to think up ways to discredit the truth-speaker, with labels and negative gossip, in all kinds of intentionally sigmatizing ways, but it will not lead to anything good to do so, because it is entirely untrue. A community built on outright lies, as many are, we are discovering more and more–the epitome of corruption and injustice–is a house of cards. It’s only a matter of time before truth comes to light, always.
Report comment
Fragility can come when a young child does not learn to automatically and naturally down-regulate. When a cell-phone alerts us to an incoming call, we answer it and the ringing stops so we can have a conversation. What I find in my fear of flying clients (www.fearofflying.com) is that when their amygdala alerts them via the release of stress hormones, their parasympathetic nervous system does not kick in and override the effects of the stress hormones. Thus, they stay in a state of alert/alarm until the stress hormones burn off. And if stress hormone release continues, as stress hornones are burned off, they are replaced with more.
Fortunately, I stumbled on a way to give my fear of flying clients a way to down-regulate automatically, and as a result, they don’t panic. But the point is, without this automatic down-regulation, a person looks – and in some ways is – emotionally fragile. Continued hyperarousal stands in the way of good cognition, no matter how much CBT they are treated with and no matter how much medication they receive.
Report comment
Would you deny that such “inability to down regulate” is a very common and pernicious result of early childhood abuse and/or neglect?
Report comment
What you say, Tom, I recognize as being caused by kidney-adrenal imbalance, as per Chinese Medicine, which is not only rather common, but it is also not at all complicated or hard to correct.
https://www.empowher.com/holistic-health/content/kidneys-and-adrenals-traditional-chinese-medicine
The psychological issues are generally created when this is treated as though something is dreadfully wrong (and inconvenient) with the child (or adult) and they are, therefore, taken down the wrong and misguided path, potentially causing all kinds of problems, and quite possibly and probably, from being labeled, stigmatized, and marginalized, causing undue suffering.
Coming back into balance from triggers is a practice, and absolutely everyone could benefit from that awareness, being human and all.
Report comment
I’ve been following the most recent research on this topic with complete fascination. Some of you may be interested.
https://www.genengnews.com/news/fight-or-flight-response-shown-to-be-driven-by-bone-hormone-not-adrenaline/
Report comment
That is FASCINATING!!! Everyone interested in REAL science should have a look at this.
Report comment
Thanks for the link, KS, it’s so interesting how these perspectives shift from one thing to another.
What I posted about kidney-adrenal balance does apply to exactly how I healed from chronic stress and anxiety, by addressing this at the root of it all. I was guided to this by a medical intuit (with whom I had a 15 minute session for $45), who gave me the protocol to withdraw from the 9 psych drugs I was on at the time, and how to find my balance again (which had been long lost thanks to these pills and all the toxic mh stuff). I followed this to the letter and it worked, I ended up doing her trainings and internships for the next several years, which is how I healed integrally, trained as medical intuit and holistic healer, and became certified to open my own practice.
Learning to ground and center and to make this practice central to my healing, taking specific herbs to bring balance to kidneys and adrenal glands and also to regenerate other damaged organs (including the brain), along with acupuncture and a variety of energy practices (e.g. Qi Gong) brought all of me back into balance physically and as a result I was finally able to start experiencing the calm of inner peace and a quiet mind again, which had been eluding me for the years that I was on those drugs and yakking with therapists.
Plus, I did tons of healing with my family and relationships, all of that had to be addressed, regardless of anything, if I wanted to get on a new life track.
But on a physical level, what had once been called “Panic or Anxiety disorder” along with even “bipolar disorder” all went away when I addressed the kidney-adrenal system along with all the yin/yang balance of my energy, mind/body/spirit. Now my mind is programmed to bring me back to center without effort, it’s automatic. The body will follow that protocol every time. That would be the nature of my holistic healing and personal transformation.
I no longer require the herbs or any of these practices, other than grounding and cenering, that’s always how I begin and end the day. But the rest was transitional, so I am free from all that now. We can train the body in the direction of self-healing.
I still believe this is universal, it is tried and true ancient wisdom and when you witness it working, it’s like math, very clear logic. But as we say on here often and I believe it’s important, we all go by what makes us each tick, individually. In general, I find Chinese Medicine to be so much more accessible and simple and it gets to the heart of the matter with ease, which makes healing plausible and likely. That’s my personal experience with it and, therefore, my take on the matter.
Report comment
Steve, the science of it all was thrown in my face when I was doing my own healing my way, based on faith, trust, and my personal intution. They were wrong and I was right, what can I say? This is so easy to prove.
These issues are complex and the industry is so misguided and filled with false information, which can be deadly to people and has been, that more than mere science is needed here. We need new vistas and perspectives, and this requires imagination, innovation, and flexible thinking. We are our own scientists and have the capacity to observe the results of our own work.
The professionals who are getting all the grants and doing all the research have failed us miserably. I’d like to see this community being more open to new possibilities and ways of thinking. The “mainstream academic research science” of it all has become stale, it is sooo played!
The mh field is stuck in repetition compulsion and as a result, it is in chronic failure, despite whatever perspective du jour it chooses to adopt, until that one is disproved and dead-ended. Then another theory or modality will come along, and take that same path to nothingness. People spend their entire careers gathering money for no-result research (or worse yet, research that is taken as gospel only to be later disproven, after already wrecking peoples’ lives because it was either mistakenly or deceivingly touted as “scientific reserach” and, therefore, “proof”), and living well despite it–and some live quite well, including even a jet-setting, world-traveling lifestyle. Not that everyone wants this, it’s not exactly a noble and fullfiling goal unto itself, but I believe the implication is clear.
Especially considering that, on the other hand, the research helps no one else to improve the quality of their lives, and people often suffer as a result of believing false research claims, especially when they are desperate and especially vulnerable. I think it’s a travesty of social vampirism, and economics and aggressive class division are at the heart of it.
This has happened for so long, and from where I sit, I believe it is because these “new and exciting theories” are always missing vital information, due to the general closed-mindedness and inherently divisive, hierarchical, and therefore, stigmatizing nature of this field. This is always reflected in whatever theory or modality, seems to be part of the mix always, which undermines any possible truth to be gleaned from the research. This is a grave disservice to society and the public at large, without a doubt.
As far as healing goes, the mh industry is a dead end. I haven’t always thought that way, and when I first came to MiA as a commenter, about 7 years ago, to explore these things further and on a deeper level with others who’d shared at least a version of my experience, this wasn’t my set in stone perspective. Although I was starting to wonder. The issues just went deeper and deeper into rabbit holes, like one void after another.
Overall, however, I was more questioning how to help this field elevate in awareness and do better by its clients. By now, however, I’m deeply convinced that there is no way in hell this will happen. It just stands to reason, at the end of it all, and very easy to intuit at this point in time. I think it’s painfully clear.
Report comment
Alex, the new research implicating osteocalcin in the fight or flight response doesn’t negate previously discovered hormonal responses to stress, it’s just saying that the physical reaction to adrenalin and cortisol doesn’t happen as quickly as they once thought and so they went off looking for other hormones that would explain that rapid response. The adrenals and cortisol depletion are *definitely* still involved and adrenal fatigue is known to be a big factor in all sorts of things but especially ME/CFS type symptoms that so many survivors have to deal with during/after withdrawal.
I think what Steve meant by “real” science was comparing it to psychiatric pseudoscience. 🙂
Report comment
That is exactly what I meant.
Report comment
Thanks for the clarification KS!
Report comment
Excellent article and I think the post that touchs readers’s concerns always rock.
Report comment
It’s interesting to note that the mental health bubble is so important to you. This prevision of “care” that you speak of, is a business, and its a business that knows that something more is involved to it than, your constant criticism, medical attention. Good health, the abstraction, is bad for business. Bad health, the abstraction, is good for business. You’ve got your non-standard practitioners in competition with main-stream practitioners for business. What business? The selling of disease and its treatment. Threaten this system, of course, and there goes some folks bread and butter. When your business is selling ill health, good health is a threat to your survival, and the survival of your family. Of course, these business interests are going to be resistant to change. There is a point at which it becomes too late to, let us say, change careers midstream. Funny thing, the ill health business is booming while the physical fitness business is only doing so so. No gain without pain they say. Business as usual, of course, is not so complicated.
Report comment
Exactly Frank.
I think we all know why a 40 year old is a psychiatrist. There are no other employment opportunities for shrinks. They went into it, not having variable interests to begin with.
Report comment
Stigma against “mental illness” is pervasive in America and is perpetuated by the American Psychiatric Association.
Why is there an anti-psychiatry movement? Because no other branch of medicine has so little regard for the health, well being, or lives of those it “treats.” No other branch can vote illnesses in and out of existence. No other branch claims powers of mind reading and fortune telling. In short, no other branch of medicine has 0 grounding in known science, 0 cures, and premature deaths of all its patients by 25 years.
All other medical branches have patients instead of “consumers” too. This choice of wording on the part of psychiatrists themselves is significant.
If orthopedists acted like psychiatrists they would amputate legs to cure sprained ankles. Pediatricians would euthanize children with head colds. And dermatologists would amputate noses to cure pimples.
Psychiatry has wasted no time in transforming itself from Cinderella to the Wicked Stepmother. They’re very defensive about their origins. And they take it out on the hapless soul whose only crime was trusting a liar with no empathy or conscience.
Report comment
Excellent comment Rachel.
Report comment
Yes Sam I agree. Rachel’s comment nails it!
Report comment
I am regularly reminded of what Avril Levine said about how Lyme Disease patients are treated by the medical system. She said, “They treat you like you’re crazy.” Left unspoken is that she got a taste of how “crazy” people are treated by medical “care” providers. It should be a wake up call to the abuses still shown toward anyone perceived as “crazy”.
Report comment
The question should not be whether it’s possible to “remake” psychiatry, but whether it’s desirable, and to this we should reply with a resounding NO.
The arguments around neurotoxins are actually of secondary relevance. The defining characteristic of psychiatry is its promulgation of the idea of “mental illness,” which is a literal impossibility. Hence all psychiatry is based on a false premise. And, were there not money to be made by both practitioners and “opponents” as a result of everyone turning their heads from this basic absurdity, that would be the end of all this. We can prove forever that this or that new drug is as toxic as all the others, but the most outrageous contradiction is that they are given to people who are NOT SICK. Ergo, psychiatry is a fraudulent and criminal enterprise that needs to be eliminated, not “remade.”
Report comment
I think demaking psychiatric *cough, cough* “care” quite possible. Pull the funding rug out from under the psychiatric pharmaceutical industrial complex, and there you go. The hospital prison, with its torture chambers, and the system associated with it, can go to ruins, and stay there until it crumbles to naught.
Report comment
I’ve seen SmithKline’s headquarters, I can’t visualize trying to pull a rug out from under it. But go for it.
Report comment
Oldhead writes sensibly, and hopefully Whitaker is coming to the realization that Oldhead has been writing sensibly all along. This elephant of psychiatry, to expand the metaphor, doesn’t just need gnats buzzing around its ears. It needs a few rounds from the elephant gun. It needs heavy dose of its own medicine. In any case, what’s the point of remaking a fraudulent, pseudo-scientific system of slavery? Not many people are interested in remaking Nazi prison camps or chattel slave plantations. Why should anyone be interested in remaking psychiatry?
Report comment
Slaying the Elephant of Psychiatry?
Report comment
ONE BITE AT A TIME!!!!
Report comment
The key is written write here, in Robert Whitaker’s own words:
“There are many individual psychiatrists who are championing the need for change in their field and working in new ways. However, psychiatry, as an institution, has not shown much interest in reflecting on the failures cited above.”
This is direct evidence that the purpose of psychiatry, entangled with the courts, law, and behaviour – is a means of social control. The institution has too much invested in the power of social control. How will people “control themselves” without psychiatry to do it for them?
The government needs psychiatry, law enforcement needs psychiatry, corporations need psychiatry, a “well ordered society” needs psychiatry. It’s more than just profit motive, but an entire system of control.
Because psychiatry’s only true function is social control.
Report comment
Great analysis JC.
Report comment
This is dead on Jan
Report comment
Hi Bob,
Thanks for the great blog.
If the objective isn’t to exterminate at least half of the population; to mechanise all production and manufacturing; and to just have good-looking and obedient people serving the rich :- then it might be very possible to completely reform the Mental Health System.
I think we’d have to move on though, and have some type of non judgemental reconciliation procedure. And then to live in peace.
Report comment
But if it couldn’t do all that would would be the point? 🙂
Report comment
I say that it is not possible to remake psychiatric care, and that no one should be trying to do this.
It is all based on exploitation of the patient. Even psychotherapy and the recovery movement are based on this exploitation.
It is about creating and perpetuating an economic underclass of family scapegoats. And it does this by deploying religiously derived concepts, like the Work Ethic and Original Sin.
So rather, people should be steered into progressive political activism.
As it is now, psychiatry, therapy, and recovery are all about forcing people to live without justice, to live without honor.
The strength of R.W.’s books, besides showing how horrid these drugs are, is that never does he say a single word to support therapy or recovery. He does not ever endorse these, though he does not attack them either, as he wants to make his point about the drugs.
It is only on this forum that we see this interest in perpetuating psychiatry, psychotherapy, and recovery.
Report comment
The truly sad part is that the medical/psychiatric community is completely ignoring real illnesses like Lyme Disease that have known neuropsychiatric effects, among them dissociative states, psychosis, and mood lability.
https://www.lymedisease.org/psychiatric-lyme-marke/
There is an epidemic of neuro-Lyme mimicking psychiatric disturbances, and the Infectious Diseases Society of America recommends against testing psychiatric patients for Lyme Disease.
https://www.lymedisease.org/ignoring-psychiatric-lyme/
Additionally, Moderator Steve commented the other day that the medical community generally harms an enormous number of patients. This is true. If medical error were properly accounted for on death certificates and were a reportable condition, it would amount to the third leading cause of death.
https://hub.jhu.edu/2016/05/03/medical-errors-third-leading-cause-of-death/
While this blog was generally well-received, I think you err in your position that it is Psychiatry alone (or primarily) that is doing active (known) harm to its patients while other disciplines are ‘real’ or ‘good’ medicine. There are guild interests going on in virtually all of medicine.
The American Heart Association for example, accepts meat industry funding and has close ties with pharmaceutical companies promoting statins for almost everyone.
https://www.huffpost.com/entry/health-news_b_4398304
The IDSA has close ties to the health insurance industry with enough evidence that a RICO case has been allowed to proceed.
https://www.lymedisease.org/lyme-patients-sue-idsa-insurers
Women are routinely harmed by the entire medical industry.
https://www.harpercollins.com/9780062470805/doing-harm/
The US is the most dangerous developed country in which to give birth.
https://www.propublica.org/article/severe-complications-for-women-during-childbirth-are-skyrocketing-and-could-often-be-prevented
This is just what immediately comes to mind. So I think it’s wise to recognize that medicine does harm, full stop. It is always a gamble when you receive medical care. The privileged get to seek multiple opinions and choose what care they receive. But most don’t have that option with our current capitalist, profit-based and profit-seeking, health care delivery system. Emergency medicine is always a crapshoot. Always. Both in delivery and cost.
Psychiatry does enormous and largely still untold harm. But western medicine is not to be praised at this moment in time. On the whole, the lot of us are sicker and more dependent on chronic pharmaceuticals than ever before. This is not a win and it’s not progress and it’s not limited to psychiatry.
Otherwise, right on!
Report comment
Thanks for the links, a close friend and AP organizer from the “old days” just got a Lyme diagnosis & I’ll forward this. Anything else you’d particularly recommend to someone just beginning to grapple with this?
Report comment
Lymedisease.org is THE authority on Lyme Disease. The membership is worth it to have access to the Lyme Times newsletter. There is also MyLymeData, run by the same org, which is providing the first of its kind, patient-centered data repository for Lyme symptoms and treatments.
Mary Beth Pfeiffer is the Robert Whitaker equivalent in investigative Lyme journalism. Her book is from 2012 but still full of relevant info.
Avril Lavigne released just this year what have quickly become known as the Lyme anthems – Head Above Water and Warrior.
Finally, Steven Jarrod Buhner is an herbalist who came up with what’s known as the “Buhner Protocol”, which many chronic (late diagnosed) Lyme patients find helpful. He has a stack of books on herbal antibiotics and antivirals.
NatCapLyme and Bay Area Lyme are the two largest and best known patient advocacy groups in the US, with lots of free good info, too.
*** Sadly, the Lyme community often pushes traditional psychiatric treatments under the delusion that they’re real medicine. With suicide the number one cause of death for Lyme Disease, desperation drives many of us into the hands of witch doctors; both psychiatrists and a good portion of those claiming to be “Lyme literate” and offering treatments such as IV peroxide infusions. So it’s really a massive mine field to navigate, especially for those without a significant pre-existing medical knowledge base to draw on.
Report comment
Thanks!
Report comment
there is now a growing societal understanding that our current mental health system, from a public health perspective, has failed.
This is too pessimistic. The system works just fine to keep people’s minds and aspirations in shackles and subservient to exploitation by the rich and powerful, which is after all what it’s designed to do.
Report comment
That’s like saying Dr. Fata’s chemo treatments worked. From his perspective they worked fine at making him lots of money.
But a lot of us were told we could live happy, productive lives if we took our “meds.” Even many NAMI parents were fooled. Then when you spend year after year in “day treatment” and still can’t take care of yourself or think straight or watch your 35 year old son forced to live in your basement–so zoned out he can barely make a sandwich or wash dishes unassisted–you ask HOW IS THIS AN IMPROVEMENT?
This is not what we were promised. Not what we signed up for.
So yes it has failed those who needed help. Like Bernie Madoff’s retirement plan.
Psychiatry is NOT help, but exploitation of the sad and lonely.
Psychiatry is anti-help.
Report comment
The question is “working” for whom, and towards what end.
Report comment
It sure doesn’t work at crime prevention either.
Report comment
Psychiatry works wonderfully. It accomplishes exactly what it was designed to do, namely, subjugating, torturing, and annihilating untold numbers of innocent people, including children, the homeless, and the elderly. It accomplishes its goal all too effectively, and it does so while masquerading as a medical profession.
Report comment
Yes. Bernie Madoff accomplished exactly what he designed to do as well.
Report comment
DS what do you consider to be its motivation for all this? What is to be gained by whom?
Report comment
I have my own theory. But it’s too weird to post here.
Report comment
Excellent question, Oldhead.
I mostly agree with Szasz that, in many ways, psychiatry gradually took the place of false religions. It’s more complex than that, but at least he was on to something.
In other words, there are a variety of motivations, power and wealth being among them. But these are characteristics that are common to modern and post-modern political philosophies as well, namely, that the purpose of philosophy is no longer to understand the order of the cosmos or to achieve wisdom, but to remake the world and dominate nature through ideology and technology.
What this means is that there is a connection between what Marx and others were trying to do with philosophy, and what psychiatry has accomplished. Money and power are always motivations for the worst proponents of psychiatry, but it is helpful to keep in mind that many people enter the field of “mental health” under the false belief that they will be helping people.
Psychiatry is doubly pernicious because it accomplishes its evil purposes while masquerading as a medical profession that aims to help and to heal people.
Report comment
Trading wisdom for power?
Interesting and understandable with human nature being what it is. Truth can be mortifying. Power gratifies the ego.
Our society worships the powerful and ignores the wise. This has always been a problem. But it has reached frightening extremes.
Report comment
I meet a person that I feel is cool it’s the inxs need you tonight.
I got to let em know I’m proud of our history and our movement has already transitioned. People get the message.
Here is my studio rendition.
https://youtu.be/4fNPC-Ta6ds
Report comment
Robert:
Psychiatry is a branch of medicine. Medical doctors diagnose disease and dispense medicine – that’s what they do. So suggesting that “psychiatric care” be remade to be non-medical is not only illogical/impossible – it also further legitimizes psychiatry and its disease model.
Lawrence
Report comment
I agree with this. It’s telling that psychiatrists want nothing to do with legitimate brain-effecting illnesses, referring those to neurologists, rheumatologists and infectious disease specialists. The domain of psychiatry is psychiatric drugging of behavior, not curing physical illnesses.
Report comment
“…The burden of mental illness has dramatically increased over the past 35 years, such that “neuropsychiatric disorders are now the leading cause of disability in the United States.” ..”
But once the drugs used to treat the disability are safely removed with some humane support, theres NO more disability! Its like MAGIC!
Report comment
Bingo!
I’m sure OH will agree.
Report comment
Psychiatry is NOT a branch of medicine; it is a tool of social control disguised by the trappings of medicine. It depends on who has the power to define “medicine.”
However Lawrence definitely forces the contradiction into the spotlight.
Report comment
Psychiatry is an illegitimate and pseudoscientific branch of medicine. But it is still a branch of medicine. Also, much of medicine is still not understood and a series of trial and error, which is why promoting any belief that western medicine is actually evidenced based and doctors are authority figures or healers is truly the definition of delusional.
Report comment
It depends on who does the defining of what constitutes “medicine” — people with medical degrees or other vested interests, or people who realize that psychiatry is totally bogus. However one leans semantically it’s clear that psychiatry is not a legitimate branch of medicine.
Report comment
Dr. K was indulging in satire.
Report comment
Psychiatry = medicalization. As Lawrence says, it’s a branch of medicine. Only problem is it sells diagnosis and treatment of bogus disease. What is a psychological illness? What is a psychiatric disorder? Let me answer by posing another question. What is bullshit?
Report comment
Psychiatry is a branch of medicine in the same way as slavery is a branch of productive labor, in the same way as Nazism is a branch of legitimate government, or in the same way as priestcraft is a branch of religion. In other words, psychiatry is a rotten branch that needs to be extirpated from the tree and cast into the ash heap of history.
Report comment
“medical doctors” are among the biggest prescribers. So with the prescription they also are in fact also “diagnosing”, which proves we don’t need psychiatry.
Granted, MD’s usually use words like “psychsomatic”, “depression” and “anxiety”, or they might scribble on their charts that “In my expert opinion, this patient suffers mostly a “psychiatric illness”. Interestingly, they do not need to send you to an “expert” to prescribe. Interestingly if an MD does not want to be bothered or can’t find your illness because of lack of knowledge, since that knowledge does not exist, he resorts to “psycosomatic” which permanently destroys the patient’s credibility of real fair treatment and acknowledgement.
This cop-out practice is why many MD’s no longer enjoy being doctors. Their dismissal, their inability to say “we know very little in the grand scheme of things”, is the cause of misery for client and MD.
Report comment
“Stigma of mental illness is pervasive in American society and is actively perpetuated by a virulent Anti-Psychiatry Movement.” This makes no sense, how are those of us who speak out against the harms of psychiatry, perpetuating stigma? We’re not stigmatizing anyone. It is those who stigmatize others, with the make believe DSM disorders, who are perpetuating and making stigma a pervasive, systemic, societal problem.
“To best serve its patients and the public good, a medical discipline needs to have an open mind regarding the merits of its practices … Unfortunately, American psychiatry—as an institution that sets standards of care—has not demonstrated this openness of mind.” “Is Remaking Psychiatric Care Possible?” I think you answered your own question, Bob. And the answer is no. So long as the foxes are dictating what goes on in the hen house, the hen will not be safe.
https://grammarist.com/usage/fox-guarding-the-hen-house/
Nor will be the sheep. “Beware of false prophets, which come to you in sheep’s clothing, but inwardly they are ravening wolves.” The psychiatrists and psychologists are the “foxes” and “wolves in sheep’s clothing.” Those hypocrites, who first promised to “first and foremost do no harm.” But in reality, do nothing but stigmatize, neurotoxic poison, and in other ways, harm their clients for profit instead.
Report comment
I wouldn’t even waste my breath, Someone.
Report comment
I know, old head, it’s a frustrating battle. People against gigantic industries, or as Whitaker described it “little gnat[s] buzzing around a great big elephant that can be swatted away with a quick flap of the ear.”
I more mention my perspective as an edification of where my work is right now. Since I’m painting a satanic Lutheran psychologist, who came under the guise of an “I want to make you my ‘artist of the year'” and be your “art manager,” as the “wolf in sheep’s clothing” that he actually, unsurprisingly, turned out to be.
The crimes of the psychologists and psychiatrists really know no bounds. They are such corrupt industries, filled with such corrupt individuals. Their crimes, and attempted crimes, need to be pointed out.
Report comment
There’s 2 million Americans in Jail, and 4.5 million Americans on Serious Mental Health Disability; and the
the American Non Mental Health System is also privately managed.
“…. (There are no anti-pediatrics, dermatology or orthopedics movements.) ..” I think one of these might develop some time soon.
Report comment
There is a significant percentage of of people who privately dismiss western medicine as dangerously hubristic and often harmful. When they speak up about other ways of healing, they are summarily dismisses by the masses as anti-science. The propaganda is deep and pervasive. Your doctor is not god.
Ask a doctor how to stay well. They will often say to stay away from doctors. That is very telling all by itself!
Report comment
That’s what they do say!
Report comment
Thanks for this Kindredspirit.
Amongst my friends and family – I am frequently biting my tongue – because I ***know*** how to get them out from under their drug load.
But “I am not a doctor” so – I might say something once (and be dissed, again).
A prophetess is always scorned in her hometown (& family and friends).
And the doctors? They keep doing it. I fear (yes, fear) the time when a condition of mine requires actual treatment by a doctor, whether surgical, procedure, or drugs. At least with drugs, I know how to do the research. Hip replacements? Back surgery? Not so much. Chemotherapy? Radiation? Surgery? This is all scary territory.
I consider a successful interaction with a doctor as “I fended them off.” e.g., I fended off the cardiologists – they don’t want to see me again for 3 years. . . .
Report comment
Just look at the ingredients in the food in the Supermarket!
Report comment
The packaged products in the supermarket aren’t food.
Report comment
A guy on PBS refers to them as “food-like substances.”
Report comment
Somebody told me that a lot of the natural healers were targeted as “witches”, and that we have lost a lot of natural healing as a result.
Report comment
Many natural healers have been disappearing and dying unlikely deaths in recent years, this is well known — especially the ones exposing vaccines.
Report comment
Yes. And most doctors do not die in hospital when their time comes.
Report comment
Bob, I’m glad to be one of the presenters in the upcoming MIA system change webinar. Reading your blog post question about the possibility of remaking psychiatric care, I remembered a conference 7-8 years ago in North Carolina where you spoke after being on the road for months talking about the issues with leading psychiatrists that you raised in your book “Anatomy of an Epidemic.” As I recall, you said you were exhausted and discouraged- that you were possibly reaching the painful conclusion that even the most prominent psychiatrists from some of the most prestigious universities that you’d interacted with, were seemingly not capable of the basic intellectual and ethical honesty necessary to even consider the validity of any serious questioning or challenging of their entrenched belief system.
I must say, I remember I said to myself as you spoke – “I’m sorry Bob had to spend so much time and energy to discover that god-awful reality!”
I’m grateful to you and everyone here who struggles for compassionate caring for all who are suffering within and without of the psychiatric system.
I started my struggle with the psychiatric disease model in the 1970s and at some point realized the only way I could keep it up was to absolutely believe revolutionary change was possible as I’d experienced at Iward, knowing Mosher of Soteria and working with Perry of Diabasis while at the very same time accepting that things would very likely only get worse- but that each day I’d just fight to the best of my ability until they threw dirt in my face.
In solidarity, Michael
Report comment
Michael,
For me, (even beyond compassion) the reality of the situation is that the MH System is “Ineffective” ; and there are other very good ways of overcoming distress most of the time (even today) within the community.
Report comment
to be fair to psychiatry, the medical establishment as a whole is rather authoritarian. i don’t know what goes on in other developed nations, but here in the US, there’s been some research on violence within the medical system–apparently, physical aggression towards people lower on the totem pole is an issue. and…
for all this talk of care and compassion, profit is the name of the game. just look at the rise of ‘concierge medicine.’
but with psychiatry–which is not real medicine, although they do make heavy use of real drugs– I have come to think that the answer is abolition, honestly. the costs, the damage to human beings, the damage to the legal system and even education and religion…
too, too much. I do not think voluntary psychiatry should even be allowed. i do not think the talking guilds that usually work with psychiatry should be allowed to continue, either.
Report comment
It IS the whole medical system. Unless of course people have not been sick enough to experience this. Yet even if they did not experience the shitcrap “care”, it still exists, and it exists as power, not a working relationship.
Report comment
“We are like a little gnat buzzing around a great big elephant that can be swatted away with a quick flap of the ear. But our new 10-session course will at least explore this landscape of “systems change,” with the presenters bringing to this topic a diversity of experience and perspectives. The presenters include psychiatrists, leaders in peer services, former directors of state mental health programs, and trainers experienced in helping providers implement trauma-informed care.”
Respectfully, Bob,
but for as long as I have frequented this website, I have tried to get people to expand your collective vision past those whom the system has wronged. I don’t ever want to demean the experience of those who were caught in the system and abused by it, but the overwhelming majority of Americans haven’t had that experience, and yet they are still touched by this issue. Additionally, no matter how many times I remind this website that the first line of defense in keeping people out of the system is to train people like me, the primary attachment figures, how to help someone in distress, my call seems to be ignored. I had to learn it on my own, but it is possible. What my wife and I went thru, most therapists won’t even touch, but we got thru it together and without any contact with ‘the system.’
But when I look at your list of contributors, there is no one on it who represents my group, those of us in the trenches, 24/7, who deal with the hell that our loved ones are experiencing. Some of us have even figured out how to help them thru it: I’m not the only spouse out there who has walked his loved one thru all the crap that we’ve gone thru.
I like Open Dialogue so much, even though we never had access to it, because it understands the families must be brought into collaboration for the healing journey because we are the ones who get awakened throughout the nights, on the weekends, on vacation, during intimate times and every other situation in life. And so we have to help walk the person thru the night terrors, the panic attacks, the dissociative issues, and so many other issues no matter where they hit life and the relationship that I won’t belabor the point here.
Yours,
Sam
Report comment
Respectfully, there is an entire organization made up of family, friends, and concerned others speaking for and over those labeled as “mentally ill”. It’s called NAMI.
I don’t want families brought in so they can be supported in fixing their broken loved ones. I want systems change to address family dysfunction that is one source of perpetual distress to so many.
Report comment
The nuclear family is inherently “dysfunctional.” It’s a unit of production basically. A mini-factory.
Report comment
Removed for moderation.
Report comment
Removed for moderation.
Report comment
People–and therefore all social groups–are inherently dysfunctional.
Report comment
How say? Sounds like a pretty dim view of humanity.
What are these functions you are referring to?
Guess I’ll never know DS’s views on this (tho he has my email).
Report comment
Opposition to the “nuclear family” is the real dysfunction, and we have Marx, among others, to thank for that dysfunction.
Report comment
Kindred Spirit,
since I specifically mentioned Open Dialogue, why would you bring in NAMI which we all know is generally disrespected on this website as a tool of Big Pharma and Psychiatry. Furthermore, since you just posted a positive comment about Open Dialogue on that thread, why would you try to twist what I say here?
I’m sorry for the things you have shared in the past about your abusive ex, but I am NOT him, and there are a lot of us spouses out there who are in it with our loved ones whether you choose to believe that or not. And until this website can come to some kind of accommodation for both sides, those with abusive families and those with supportive families, I think this movement will continue to falter.
Sam
Report comment
Robert,
There is no other website or any other source that is so dedicated to exposing the many harms being done by psychiatry and fighting so hard to bring about change to prevent these harms from continuing. I am deeply grateful for this entire incredible website and for all your tireless work and advocacy.
In fighting my own battle with a psychiatrist over lasting harm she caused me I came to realize that psychiatrists are untouchable. They are literally ‘top dog’ and answer to no one – not even the College that supposedly governs them. A year ago I was ready to give up on my battle for justice. Then I found your website and was blown away when I realized my story is not an isolated case and any one that sees a psychiatrist for any reason is likely to be harmed instead of “helped”. Finding your site re-energized me to keep fighting and although I have health issues I am trying to be an activist in any way I can.
As you noted, change comes “one mind at a time” and unless, or until people have first-hand experience or hear about the horror stories and the harm, their mind set doesn’t change. I have been forwarding every person I interact with a link to the MIA website (including all mental health professionals in any capacity, as well as my family doctor, heads of mental health organizations, advocacy groups etc). Thank goodness for the mental health professionals on MIA who have a strong moral compass and possess ethics, intelligence and integrity. Hopefully there will be many more who have the courage and integrity to join the fight. I hope every reader of this site tries to pass the information or a link to this site at every opportunity they get and donate whatever they can to keep the fight going.
Please keep up the incredible work and thanks again!
Report comment
I believe that a lot of the increase in the number of adults getting psychiatric disability money is simply the continuing advances in industrial and information technology, reducing the size of the work force, and then the lack of other public support benefits, such as UBI. And then with the Clinton-Gingrich welfare reform, that pretty much means that those on welfare will eventually end up on psychiatric disability of one kind or another.
Need to go to UBI.
Need to terminate the mental health system.
Report comment
Those who would criticize its treatments are often dismissed as being “antipsychiatry,” which is to say that their criticisms are driven by ideology and not any reasonable review of science.
This is SO offensive. I guess you just told AP people here how you really feel — that you consider us “unscientific,” while you consider the “serious” study of the efficacy of toxic drugs for metaphorical diseases to be “scientific.” How “scientific” is not knowing what a metaphor is, and that it cannot have physical qualities such as “disease”?
Elephant in the room, meet MIA; MIA, meet the elephant.
Report comment
And elephant of psychiatry, meet elephant gun… at your service.
Report comment
^^^^^^^ YES!
Report comment
What?? I believe Robert was saying this is the view of psychiatry and not the view of MIA??
Report comment
I agree with that observation.
Report comment
Yeah, he does that all the time. But he respects that view enough for it to make a difference in how he proceeds and what he says, i.e. he waters down what he knows to be true to avoid being attacked by well-financed psychiatric propagandists. He’s also afraid of being called a Scientologist, when such absurd attacks can easily be turned around against those who use them, and THEY can then be exposed. Again, it’s a strategy which accepts psychiatry as a basically legitimate form of “health care,” vs. a strategy based on it being a police force.
Hard to know whether to phrase this in 2nd or 3rd person btw.
Report comment
Reduction ad Absurdium.
“Hitler was a vegan. So if you don’t eat meat you must support genocide like Hitler.”
The stupidity of this “argument” deserves to be called out.
Reductio ad Scientologium.
Report comment
Thank you again Professor Rachel!
Report comment
Oldhead, you know you are deliberately misreading what I wrote. This is how psychiatry, as an institution, responds to criticisms . . . it’s a rhetorical device they use to delegitimize criticism by saying it arises from a biased perspective. It’s a point about how psychiatry avoids dealing with legitimate criticisms.
Beyond that, I am not going to respond. This is such a gross mischaracterization of what I wrote, and you know it to be so. And then, having grossly mischaracterized what I wrote, you then call it offensive.
I am tired of this, I have to say.
Report comment
RW, for what it’s worth, I want to say “Thank you.”
You owed us nothing. But you have risked your own career as a medical journalist to help people like us. The ultimate underdogs of Western society.
And you have given us this site to visit and support each other. Not to mention your books. Got my dad reading Anatomy of an Epidemic. i doubt i could have escaped the system without MIA.
So thank you once again.
And–if someone calls you a Scientologist on social media–remember to call them out on the Reductio ad Absurdium Fallacy.
Report comment
Robert you are avoiding my point. I’m very tired too. The point is that you DO NOT DEFEND anti-psychiatry when it is so “mischaracterized,” you simply declare that you are NOT anti-psychiatry to deflect the attack. Which is a way of invalidating us.
Report comment
Oldhead, you know you are deliberately misreading what I wrote.
This sounds like a personal attack. Why would I “deliberately misread you”? This is what you said:
Those who would criticize its treatments are often dismissed as being “antipsychiatry,” which is to say that their criticisms are driven by ideology and not any reasonable review of science.
This can easily be read to infer that the part about AP being “driven by ideology…” is your definition, which you say it is not, and I have no reason to doubt your clarification. However it is clearly ambiguous.
So if anti-psychiatry thought IS scientific in your book why doesn’t MIA take an overtly anti-psychiatry perspective?
Report comment
Rachel that is a great comment. I wish people would be more grateful for the work, dedication and advocacy of Robert and the MIA site. It is an amazing site with many incredible professional writers and tons of personal stories and it puts out so much new information on a daily basis I can hardly keep up. And there certainly is not money falling from the sky to operate a website of this magnitude. No one has to agree on every aspect but at least show some gratitude and solidarity for the overall mission.
Report comment
Hi Rosalee, you know I have, both, gratitude for MiA and also my criticisms like many do, I’ve been public and transparent about all of it. But I am wondering about asking people, many of whom are on fixed disability incomes and/or living in poverty, to use their very limited financial resources this way. There is a lot of financial disparity in this community alone, and I’m wondering how this is affecting things here.
These are highly contrasting perspectives–having vs. not having financial resources–and at this point, I am not sure they are reconcilable, so solidarity here is a lot to expect because this represents two unequal levels of power in the current paradigm (key phrase), which MiA can only replicate. Is this really the best we can do?
And, indeed, Mr. Whitaker, MiA has been of great value to me, despite our tiffs, and I’ve certainly helped to support it in many ways over the years. But we are eluding core change, which, personally, I believe is the only worthwhile goal at this point as anything else is going to be more of the same, and I am wondering if we’re on the same page about that. I’ll see what unfolds from here. Thank you for these unique opportunities to gain clarity on such complicated and controversial issues!
Report comment
No one has to agree on every aspect but at least show some gratitude and solidarity for the overall mission.
What is that mission in your view? Because people here have differing, even competing “missions.”
In a rush to be “nice,” people are ignoring the points I’m making here. There need be no conflict between being nice and being critical.
Report comment
Alex, you misunderstood my comment. I would never ask anyone on “fixed disability incomes and/or living in poverty” to donate to anything. After a work place accident, then cancer diagnosis and encounter with a psychiatrist I have been on disability and have faced many financial difficulties when living on my own – so I know what it’s like. Of course not every reader is in a position to donate anything but there are thousands of readers and my comment was to say I hope readers pass a link to the website to spread the message and “donate whatever they can to keep the fight going”. Key words – “whatever they can” – if it’s nothing then it’s nothing. No big deal.
You wrote “so solidarity here is a lot to expect”. I was referring to the defintion of “solidarity” as in “Unity of purpose, interest, or sympathy”. The mission of this website as I understood it was to “re-think psychiatry” and by doing so to try to stop the harm being done to so many by psychiatry. I was not linking “solidarity” in any way to donating money.
Report comment
Oldhead, When I found MIA I read the mission is to “re-think psychiatry” and as I continued reading it became clear the mission was also to try stop or prevent the many forms of harm being done to so many by psychiatry. Would I want to see psychiatry abolished, absolutely!! But that is a HUGE goal that will take a very long time and may prove to be impossible. So in the meantime I support re-thinking psychiatry to try stop the ongoing harm and take away the unrestrained power psychiatry currently has. Anything is better than the status quo.
Report comment
Rosalee, I am encouraged that you see the abolition of psychiatry as a goal. Once one reaches that realization the next step is to determine how to get there. That’s a long long conversation.
Most of us who oppose psychiatry see no cause to “rethink” it any further; the only thing left to think about is how to stop it.
“Stopping psychiatry’s unrestrained power” is also the key to ending it completely, as it can’t compete in the marketplace of ideas; it relies on force for its very existence. However until people are educated to the fact that psychiatry is inherently fraudulent and cannot be reformed there will be no demand to restrain it. So the two go together.
Most people who speak of “rethinking” psychiatry do so in the sense of looking for a better way to practice it, which is a dead end. Psychiatry will not end as the result of a steady stream of small reforms but by being relentlessly exposed as a monumental deception, i.e. as the “Empire’s New Clothes,” so to speak.
Report comment
Rosalee, I do know that you are considerate of others this way, I’d never question that. I’m just highlighting the financial disparity within this community, which duplicates the financial disparity in society, and these so called “health systems”–and specifically anything mh related, where I believe this disparity is especially flagrant–which causes such issues of inequality and therefore, marginalization and discrimination. This is social abuse, which, to my mind, is responsible for the ills of society at large, that level of deep division which is crazy-making for people on the wrong end of that.
I wasn’t equating “solidarity” with money, I meant that these different consciousnesses (lack vs. havingness) are hard-pressed to come together in unity due to power imbalance and different immediate needs. These will create divergent mindsets and realities, and are most likely to be in chronic conflict.
Mostly, I was responding to this–
“And there certainly is not money falling from the sky to operate a website of this magnitude.”
When the fuel is money, then we’re going by the old paradigm and there will be no change. That’s my main point of my response. There are other ways to build and create, without being dependent on money. That would be a truly powerful enterprise, built from new ways of thinking. THAT is change.
Report comment
Precisely Rosalee.
I want to abolish psychiatry, but it’s not going to topple all at once.
Too many people believe in it. Those outside believe in the “chemical imbalance” myth.
Those inside rationalize it by saying, “Those people must be innately defective to act weird from grief or trauma or freak out on the mild drug I gave. They’re unfit for polite society and would only be institutionalized without my help.”
Report comment
“I want to abolish psychiatry, but it’s not going to topple all at once.”
I don’t believe that’s necessarily true at this point. I know a lot of people personally and also know of them via internet, who have never been activists nor would know about MiA, etc. (other than with whom I share this info) who already have only negative things to say about psychiatry, and who are aware that it is based on lies, misinformation, and toxic drugs on top of it all. So many people have healed and have gotten their clarity outside of anything having to do with this system and industry, and they are paying it forward successfully.
I think more people than not get that we’ve all been had in many ways, and the mh and social service systems–all based on psychiatry and its “hierarchy of power”–are at the top of that list. The problem is that no one really knows what to do about it. Corrupt systems have been the norm for so long now, hard to know who and what to trust. Communication breakdown is the norm when there is resistance to change. It’s intentional, to ensure status quo. But that can’t go on forever, so it’s really not a sound strategy for survival, which is why the status quo is in trouble.
At this point, however, it only takes one domino to fall so as to kick over the rest. The trick is finding that one domino and tapping it over to start the chain reaction, and more than likely, it’ll be an accident, a matter of convergence along with all the truth coming so quickly to light. There’s no foundation in truth here, we all know this is unequivocal truth, at least I am of that opinion quite firmly. So there is no real foundation here, it’s been exposed a million times. Rapid change can happen this way, under these circumstances. I’m not a historian, but I imagine history holds many examples of this. Stands to reason to my mind, in any event.
And regardless, in this age of information super highway, things happen more quickly than ever. Many previously held in high esteem celebrities of all kinds have seen their careers go down the toilet, along with public respect, in the blink of an eye, thanks to the internet. This can happen to industries and long- established institutions, too. Psychiatry and its ilk are already on shaky ground, I don’t think it’s a secret any longer.
Report comment
I pretty much agree with Alex and support his optimism.
Report comment
Unfortunately, psychiatry is NOT “on shaky ground” at this time. It is more powerful than ever and deeply (and forever) connected to the future of the entire capitalist system.
Those who are NOW overly optimistic about ending psychiatry and their Medical Model, FAIL TO UNDERSTAND THE INTERTWINED CONNECTIONS OF PSYCHIATRY AND MODERN CAPITALISM.
Read Bruce Levine’s blog (currently posted next to RW’s blog) which provides an important response to the provocative question Robert Whitaker raises with his title.
To be optimistic about the fall of psychiatry at this time would have to mean that you are also optimistic that we are now on the verge of a revolution to end the profit based capitalist system.
While a political crisis could develop rapidly and these conditions could change to be more favorable, there is no evidence of this happening at this time.
This is why we must always connect our critique AND organizing efforts against the oppressive Medical Model to also ending the profit based capitalist system.
Richard
Report comment
The Collapse of the American Empire?
Steve Paikin interviews Chris Hedges, Sept 2018
(starting at 10:15, he refers to the opioid crisis, as part of the mix)
https://www.youtube.com/watch?v=tPk9HSLagVg
Report comment
To be optimistic about the fall of psychiatry at this time would have to mean that you are also optimistic that we are now on the verge of a revolution to end the profit based capitalist system.
“At this time” meaning tomorrow, no. But does it matter if we’re talking basically about speeding up the inevitable? If an idea is correct is correct it will remain correct; its correctness cannot be changed by government guns, only its implementation.
I think Alex is saying that the spiritual and material conditions are ripe for a mass epiphany. I’m sure you’re also aware of the “single spark” concept (not that we should count on this).
Optimism is not only necessary to keep jumping back into the struggle, it’s realistic. We can’t put artificial deadlines on anything, it’s a long complicated process.
Report comment
There’s plenty of evidence of BIG change happening, at the core of society. Mostly, at this point in time, it’s that people are waking up more and more, on a daily basis, to their innate personal power, and learning how to transform themselves out of oppressive situations, toward freedom. Some of us have recounted our experience with this on here, and there are countless stories and testimonials about this on YouTube, for starters. We’re in a new era, it’s unfolding currently.
Report comment
Rosalee, that was My impression as well.
Report comment
I agree.
Report comment
Stephen, Steve, KS and Rosalee, please pay attention to my main point — that RW inappropriately considers such views worthy of respect rather than mockery. RW has historically distanced himself and MIA from supporting AP for fear of such attacks by the establishment, rather than pointing out the bankruptcy of such criticisms and defending AP against bogus charges.
Not that I expect more considering the concern expressed in the title is that of “remaking” psychiatry rather than abolishing it.
I’d like RW to restate his position if he considers the above assessment to be inaccurate. The statement I am responding to was rather ambiguous, intentionally or not.
Report comment
RW is like a ‘democrat’…can’t advance social change cuz the republicans are ‘blocking’ him.
Love ya, Robert, but your caution is bogging you down imnsho.
The left is dead. Social change will take a revolution but the tech is in place to make that an impossibility, so here we are, sheep,…begging for the boot on our neck to let up a bit.
Report comment
Yes the true left is very disturbingly dormant at least. In the 70’s the left supported anti-psychiatry in the same breath as they supported Susan Saxe and the FMLN. Now what is called “left” is usually neoliberal identity politics (assuming there’s some other kind).
Report comment
“RW inappropriately considers such views worthy of respect rather than mockery.”
I do not now and never have had the impression that RW considers such views respectable, merely that those arguments are used successfully because of the generally negative view the public holds against Scientology.
Report comment
Not only because of, but in support of the demonization of Scientologists, antipsychiatrists, or anybody who threatens their control of the market. The idea that people who oppose psychiatry are anti-scientific, biased and/or irrational is a PRODUCT that has been SOLD by the psychiatric industry in order to deflect criticism. Robert is quite clear about this in Anatomy, where he outlines how the psych profession collaborated with Time Magazine to do a cover hit piece that established and connected any resistance to psychiatric hegemony to irrationality and self-serving bias. To suggest he doesn’t understand this suggests that perhaps a person might need to reread Anatomy again, because they’re forgetting what RW has said about this very subject.
Report comment
I KNOW he understands this. Nonetheless he publicly denies being anti-psychiatry because he is for some reason afraid of being seen as upholding the conclusions to which his work clearly points.
It’s like saying “I’m not anti-psychiatry because I have a gun being pointed at my head by the psychiatric industry.” But there it is.
ANYONE who exposes this system is targeted for destruction if need be, and no one is immune. We are not obligated to be martyrs. But in the end these are not intellectual debates, they are power struggles. Psychiatry is a police force, not a wayward branch of medicine. There is no moral or intellectual reason not to oppose it.
Report comment
I do not now and never have had the impression that RW considers such views respectable
Then he should pick them apart and mock them.
Report comment
Oldhead says: “Stephen, Steve, KS and Rosalee, please pay attention to my main point …”
No one is going to pay attention, or give much credence to to your “main point,” after you totally mischaracterize some one else’s words and their essential arguments.
And then when you’re called out on this, and rightly criticized for this behavior, you refuse to acknowledge your error and blame RW for being “…ambiguous, intentionally or not.”
This sort of uncivil and unprincipled discourse will NOT lead a higher understanding of these questions.
Richard
Report comment
It was and remains ambiguous, even though RW has since clarified what he meant. If someone is unclear about what they mean it is as least as much their “error” as that of the person reading it.
Report comment
I would add that others agree that this is ambiguous. Had RW intended to diss AP (which he says he doesn’t) he could have phrased the statement exactly the same way. So I don’t need to be lectured, as those familiar with the dispute know what Richard is actually angry about, and it has nothing to do with this article or my response.
I will continue my analysis below based on what RW says he meant. I have no hostility towards Robert, though this doesn’t seem to extend both ways.
Report comment
Further (if correct use of the English language is really the issue), consider the following statement, which contains the same sort of phraseology:
*Those who support stem cell research are often slandered as “cannibals,” which is to say that they consume human tissue.*
Is it “mischaracterizing” whomever might have written this to conclude that they themselves *also* accept the assertion that cannibals “consume human tissue”?
Any English majors here?
Report comment
One can respect the activism and science promoted by those people who are all the way ANTI-PSYCHIATRY, but not YET be ready to advocate for the complete abolition of psychiatry in society.
I would say that this is most likely where RW is coming from. So it is OBVIOUS why he would put some distance between his own views and *anti-psychiatry.*
This is not rocket science!
Report comment
No, it’s called “changing the subject.” 🙂
Report comment
Removed for moderation.
Report comment
Removed for moderation
Report comment
R. Whitaker never adopted an antipsychiatry position. That much was clear from the start. If you are not completely opposed to psychiatry, you are going to be supporting some aspects of it. If you want a vehicle for promoting the antipsychiatry cause, as you apparently do, OldHead, somebody else is going to have to serve as the main impetus for it. In other words, this is all rather do it yourself, and hopefully, do it yourselves, a matter for some sort of unity and solidarity on behalf of those who are true to the cause. Expecting MIA to be an antipsychiatry website, when it explicitly is not an antipsychiatry website, is like trying to drink from a glass that has no bottom. Do you want to do some organizing among those of us who are opposed to psychiatry towards the end of creating a viable vehicle for our position? That’s the place to start.
Report comment
It is immoral and unethical to ever promote any version of Psychiatry, its Drugs, Mental Illness / Mental Health, Psychotherapy, Recovery, Autism/Aspergers/Neurodiversity.
R.W.’s books have never violated this.
For those who want to stop stupid debates with people who take advantage of the marginalized and vulnerable with their ideas about Therapy, Recovery, and Autism, PLEASE JOIN AND BE READY TO ACT:
https://openingoftheway.createaforum.com/
Report comment
A ‘science’ that declares Jeffrey Dahmer sane, but the people he was killing and eating ill, and in need of ECT and chemical castration? People who behave like Ariel Castro and call what they do ‘care’ coz they have a license from the State to do it? Going to come aa day when these people are marched past the corpses of the people they have harmed. It just doesn’t feel like that will be anytime soon. It’s actually worth looking at what the National Socialists who were put on trial at Nuremberg did and said. Don’t admit that what you were doing was wrong etc. The mindset is quite striking when compared to what Mr Whitaker states above.
Report comment
And as we know psychiatry and “National Socialism” were closely intertwined even back then.
Report comment
I saw a brief piece on RTNews today regarding what is being called “Eco-Anxiety”. Might be the latest addition to the DSM? Any child who complains about the destruction of the planet for corporate gain is mentally ill, and will be treated for that illness.
Looks a bit like the trial separation has ended and they’re back from their second honeymoon oldhead lol.
Report comment
They pulled RT from the airwaves where I live. What did the editorial stance seem to be?
Report comment
A good idea to stop these pesky little “activists” and advance the cause of capitalism. I mean who wants their child attending protests about the wholesale destruction of the planet for profit ending up being identified via facial recognition and then ‘selected’ for treatment. Best you go to school today dearie and learn all about the nutritional value of the Big M and Coke.
Nothing that the Russians don’t have experience with though, given heir treatment of political dissidents in the past.
Report comment
As a bit of nostalgia, my very first MIA post was one suggesting RT as a possible venue for anti-psychiatry coverage.
I stumbled upon MIA in 2013 while web-surfing stuff on the mental patients liberation/anti-psychiatry movement after years of absence from the scene, mainly with writing my memoirs in mind, only to discover how far things had regressed. MIA was the only place where I could find some remnants of the movement among the participants.
Report comment
There might have been a time when they may have done that oldhead. And I really don’t know what its like in the US anymore, i was there pre 9/11 but here in Australia the media are in lock step with the government. They are cloaking their propaganda role by claiming they are holding government accountable.
Whistleblowers are in for some serious trouble here these days. And this because the media are handing over their sources willingly, or as a result of raids by Federal Police. Its also the case that human rights have been placed on hold via some rather slick legal tricksters (you know who you are) who claim to have the public interest at heart.
Spying (eavesdropping) on the ‘confessional’ is an old trick, but a good one when people are stupid enough to trust you.
Report comment
In questioning if it is possible to remake psychiatric care, change at the top will only arise when there is a firm demand from the bottom.
The masses of psychiatric consumers who are at the very bottom are without a voice and rely heavily on those who claim to advocate in their best interest.
Unfortunately, mainstream advocacy agendas are part of the well-established pro-psychiatry movement that continues to advance and grow our drug-centered paradigm.
The pro-psychiatry movement deceptively promotes itself as a “national alliance on mental illness”, legitimizes psychiatric abuse, monopolizes the mentality of our lawmakers/court systems involved in issues that impact those who are labeled “mentally ill” and turns a blind eye towards the harmful effects of psychotropic drugs.
The top search engine result for the term “mental illness” is the National Alliance on Mental Illness (NAMI) website.
“NAMI’s top priorities is educating as many people as possible to recognize the warning signs of a mental health condition and to promote early intervention.”
“NAMI Ending the Silence (ETS): Offered in schools at no cost, ETS opens a dialogue for students, families and school staff to help them feel more comfortable talking about mental health, while destigmatizing mental illness and promoting early intervention.”
“NAMI On Campus: NAMI On Campus clubs are available on 57 university campuses and reach college-age students across the country. The program aims to raise mental health awareness and provide peer-to-peer support in educational settings.”
“NAMI Basics OnDemand: A free course for parents and caregivers that provides fundamental information about the signs and symptoms of mental illness, and how to best support a child with a mental health condition.”
The pro-psychiatry movement is comprised mainly of parental/caregiver perspectives who do not dispute the concept of “mental illness”, believe psychiatric treatment is evidence-based and believe psychotropic drugs are safe medicine.
The pro-psychiatry movement is also supported by non-psychiatric medical professionals who liberally prescribed psychotropic drugs to their patients without consideration of the many adverse reactions, including worsening symptoms and long-term chronicity.
Without advocates who will act in the best interest of those labeled “mentally ill”, the drug-centered paradigm of care will continue to expand and profit.
Report comment
People in my position are desperate for help and support: NAMI offers it. I contacted them a long time ago and met with the leader of our local group, but I never ended up going to the meetings. It was only later that I started to frequent this website and realized they had been co-opted by big pharma and psychiatry.
It’s too bad MIA doesn’t have a vision to offer a counter balance to NAMI: it’s a huge need, learning how to deal with all the things that manifest in a distressed loved one and also cope with the hurt and pain those things cause in the relationship. Maybe some day my wife will be in a position to allow me to start something…
Sam
Report comment
What once was the mental hygiene movement, and now refers to itself as the mental health movement, is a movement that is all about medicalization, that is, the provision of medical “care” for people who might be considered to be “in distress”, or in crisis, but who are literally not (i.e. are not physically) sick. NAMI is one of the latest organized manifestations of this movement. The results of this evangelical drive to treat people, and the zealotry behind it, are the almost daily news reports that the numbers of people diagnosed with psychiatric/psychological issues are rising. Another result is the systemic expansion achieved by recruiting patients into its workforce. It should come as no surprise to anyone, that if you wanted the numbers to decline, you’d be working in the opposite direction. that is, towards getting people out of this artificial disability system. Apparently, some folks threw in the towel long, long ago.
Report comment
Are we actually agreeing on something here?
Report comment
We agree on a lot of things I imagine. The problem I have is with this rhetorical “abolish psychiatry”. All psychiatry is not forced psychiatry, all psychiatry is not psychiatric slavery. I’m for abolishing that, that being large-scale institutional coercive psychiatry. I’m not on a vendetta against private practice. When it’s take it or leave it (i.e. consensual and chosen), I’m not for abolishing it, as there are liberty issues involved. Were everybody to leave it, it would be defunct. The abolition of psychiatry would mean the triumph of antipsychiatry, in which event both fields would be reduced to redundancy, however, we’ve got a ways to go before we’re there.
Report comment
“all psychiatry is not forced”
Is a falsehood.
If diagnonsense is a lie, if drugging is based on a lie, if there is coercion from family, schools, etc. (Johnny can’t sit still, see a doctor to see if he has ADHD) – then psychiatry is forced.
Psychiatry which is based on a lie is forced.
Report comment
I tend to agree. There are other forces not obvious to the doctor-patient relationship that act to make it more difficult to avoid psychiatric “treatment” even in the absence of overt force. For instance, doctors are pressured from insurance companies and their own organizations, as are counselors and therapists, potential patients are pressured by friends, family, workplace, schools put pressure on parents to psychiatrically “treat” their kids, the news media makes it seem like people are foolish for not “taking their meds” as prescribed, movies and TV shows dramatize again and again how those who “don’t take their meds” deteriorate and become dangerous, and yet are magically fixed when they are back “on their meds.” Maybe it’s not “force” but “social coercion,” but there are a lot of people on these drugs against their own better judgement, or lacking any kind of informed consent, who were not ordered by the courts to take them. Lying to people can be a form of coercion if the lies create fear that the person will be damaged or do something dangerous if they don’t comply with the doctor’s “suggestions.”
Report comment
Logic, JanCarol.
“all psychiatry is forced”
would be as much of a falsehood. Although “much psychiatry” is forced, certainly “all” of it is not.
Psychiatry that is based upon a lie is based upon deception, however, deception and force are not equivalent. A person can learn the truth, however, in situations where force prevails the truth is irrelevant.
Although it may sound better to the “winners” than it does to the “whiners”, despite the claim that “history is written by the winners”, might doesn’t really make right.
Report comment
We can argue about what constitutes “forced” but there is no argument that it is fraudulent. Often it’s both.
Report comment
I don’t think there is much argument about what constitutes force: involuntary commitment court orders, for instance, leather straps, locked doors, and goons with hypodermic needles. I do, however, think that you are going to get arguments, from true believers among the drug, label, torture and imprisonment gang, that the psychiatric faith is not based upon false premises, that is, that it is sound. As with all religions, and this goes for the “soul healer” religion as well, some of us are going to be skeptics and non-believers.
Report comment
Removed for moderation.
Report comment
NAMI is like one of those bug lights that irresistibly lures millions of insects in, and then zaps them.
Report comment
Sort of like what the Democrats do with idealistic people.
Report comment
I had one of those bug lights at one stage. Bit too much like ECT for my liking, lil bugs being fried. I’m hoping someday to get the updated version that sedates them before zapping them into oblivion. Same result for the bugs, but I feel so much better watching their demise.
RIP Kevin Spratt
Hey I just realised what my wife meant about her and the psychologists plan to spike me with benzos and plant a knife on me ending up being a “suicide by police”. I was lucky I didn’t get shot. Still, everything there for a cover up.
https://www.perthnow.com.au/lifestyle/health-wellbeing/mental-health-plea-after-wa-woman-killed-ng-s-1968548
Ever had police tell you “it might be best I don’t know about that” during an investigation into serious criminal offences? I have.
Report comment
Mental health professionals so desperate to have people forcefully drugged for illnesses people don’t have that they will resort to tactics of spiking and planting knives, and stooging police for referrals.
So what was it that the Senior Constable found it best that he didn’t know? That the psychologist who came up with this plan with my wife had a husband who is a psychiatrist. At the very same hospital where my wife and the psychologist groomed me to attend. Still, by the look on the face of Dr I’m the Boss around here, they weren’t expecting any interference in their back up plan. Not with police turning their backs on the documents I had proving what I was saying to be true. We prefer to slander folk who come in to police stations with evidence as being nutjobs.
Motive? Conspire to stupefy and commit an indictable offence, namely kidnapping. Or “patient”dies from overdose in ED as a result of morphine from an unknown source, in combination with ‘chemical restraint’. He did say “no”.
Yeah, probably best you don’t look Senior Constable.
Report comment
This zapped ex-NAMI member agrees Dr. K.
At least I survived to tell the tale.
Report comment
Its not just a matter of what treatments are better or what heals better. The entire edifice and intent is wrong.
Promoting things to do what Psychiatry does, or which have similar effects, is immoral and unethical.
R.W.’s books have never violated this.
For those who want to stop stupid debates, PLEASE JOIN AND BE READY TO ACT:
https://openingoftheway.createaforum.com/
Report comment
The solution to the terrible oppression of Psychiatry is the same as the solution to the terrible oppression of the Church centuries ago: sever its connection to State power. This also applies to its adjuncts, Big Pharma and the Medical profession generally.
Report comment
Got a strategy?
Report comment
Sure. As I wrote above “sever its connection to State power.”
By which I mean to the regulatory, credentialing, funding, and coercive apparatus of the State that the State-Science-Corporate-Professional-Media Alliance is built on. All of this justified by concern for public safety, all of them in fact undermining it by enabling the power of special interests. Once the broad mechanism is understood the details can be worked out.
Report comment
In my State a psychiatrist need only call police and they will do exactly what they are told. Even if they know they are breaking the law by doing so. Our politicians?
Our treasurer who was given some time in the newspapers for sniffing the chair of our Minister for Mental Health in parliament (her sh&t don’t stink) had to flee the State to obtain treatment for his bipolar disorder after he knew where police were going to take him if they got their hands on him. (He had got drunk and had side swiped a few cars on his way home) I always wondered why he couldn’t obtain adequate mental health services for his illness without getting out of town so quickly. But the police had been knocking on his door wanting a word (and were quite possibly going to drop him at a hospital for an ‘assessment’). I think he was aware of where that was going and fled the State.
If our politiicans are not safe from what are termed “bad faith referrals” and police are basically tools of those who are really pulling the strings, then where do we start?
Our lawmakers don’t even recognise the protections they put in our Acts of Parliament, they rewrite our laws to suit without any amendments being presented to Parliament, and police don’t even have copies of the Criminal Code in their Stations and simply do whatever Doctor orders, despite the claim by our Prime Minister that Australians are a people who value a rule of law. He should spend a day as an Aboriginal.
Report comment
But doesn’t psychiatry exist to preserve state power? Why would we expect the state to undermine its own support system?
Report comment
Closing down Psychiatry or getting rid of the drugs seems to be an all or nothing proposition. Not possible until attitudes change.
But putting some psychotherapist out of business is more of a case by case situation.
I say that the entire enterprise is wrong and amounts to exploitation. But as it is just talk, we can’t outlaw it between consenting adults. All I want is to discredit it and terminate the government licensing.
So you might agree with me that it is all bad. Or you might say that there are good therapists and there are bad therapists.
Doesn’t matter really, all we need to do is get judgments against some of them, that will change the public perception of them. It is quite doable. It starts with an angry client. If we have to pick a particular school, the Richard Schwartz and his Internal Family System’s Therapy.
Perceval and the Red Knight
http://pre15.deviantart.net/25e6/th/pre/f/2011/276/2/a/perceval_and_the_red_knight_by_epictones-d4bqgwu.jpg
Report comment
Mr. Whitaker, did you ever think that societal problems were causing the escalation of mental health problems? Or, the the corporatization of health and mental healthcare were handcuffing psychiatrists so that psychiatrists are burning out at epidemic rates and suiciding at the highest professional rate?
Report comment
Psychiatry claims to be helping with “mental health problems.” We are seeing a VAST increase in the use of psychiatric “treatments” (especially drugs), and yet we’re seeing a steady worsening of the “mental health problems” that these “treatments” are supposed to solve. Isn’t it psychiatry’s job to address these “worsening conditions of society” through their helpful interventions? Doesn’t seem to be working too well, does it?
And this trend is seen to happen again and again in countries where drugs and the “treatments” are introduced – more and more people on disability and unable to participate in normal social interactions and expectations. What exactly is psychiatry claiming to be doing about these societal problems? It seems at best to be drugging the brains and bodies of those harmed by these societal woes, and at the same time denying (through their claims of physical causality) that there is any connection whatsoever between the suffering experienced and the social issues that you have identified. In all likelihood, psychiatry as practiced is not helping, but in fact making those conditions worse by providing a handy way to blame and silence the victims of our post-industrial society’s insanities and adding to that insanity by its stigmatizing labels and “treatments” for “disorders” that are voted into existence by committees.
If mental health problems are caused or exacerbated by social conditions, what exactly does psychiatry propose to do about them, Stevie? Maybe start by discontinuing the blaming of people’s “malfunctioning brains” for their suffering?
Of course, the bitter irony of you blaming psychiatrists’ high suicide rates on social conditions while the profession blames their clients’ genetics is not lost on anyone reading your comment.
Report comment
Well said!
Especially that last paragraph.
Report comment
Exactly Steve! Well stated!
Report comment
Yes to that last paragraph Steve McCrea.
It’s okay Stevie, the redness from the spanking will be gone soon enough. Why is it that like our politicians who are not willing to send their own kids to war, Mental Health professionals seem to not want their own families given the ‘treatments’ that are available? See for example a recent episode of Dateline where a mother who was a mental health professional did everything within her power to ensure her son did not get evaluated by a psychiatrist despite being a serious danger to self or others. Though she did recommend the services for all other members of the community.
Report comment
Alex, yes as you would know from my personal emails I am VERY compassionate and even though I have my own huge struggles I’ve always supported and stood up for anyone less fortunate, facing hard times, the elderly, etc, etc. That is who I am.
I made a simple and well- meaning comment in an effort to support MIA and you turned it into an issue of social abuse?! It’s bad enough psychiatrists twist words and try portray what is said in into something different, let’s not do that to each other. You speak of energy and light for healing but are quick throw shade over a simple comment made to be positive and help grow a website that IS trying to help people and prevent harm.
As far as my comment that money is not falling from the sky – I’m just being realistic. Robert is running a site that takes a lot of time, energy – and money. For that I have deep gratitude and I would hope others do too. That sentence was NOT about donating money – it was about having gratitude for the time, energy and yes – money that IS unfortunately required to run the site. If you or anyone else has a way to build and run a site of this magnitude that doesn’t require money then I say PLEASE do it.
Report comment
Wow, seems we are having a huge misunderstanding here. Not sure how to respond in the moment with respect to the issues, that is secondary to me right now.
What I’m feeling at this point is bad that we have had such a communication glitch. It wasn’t my intention to turn anything around, I was attempting to respond from my own truth, based on where I am in my activism. I thought there was a logic to what I was saying, congruent with and relevant to all we are discussing here. Obviously there are layers of issues and things to process, in light of it all. I’m fine agreeing to disagree. I won’t argue with your truth of the matter, but I do have mine, and I guess they are different, which is fine, why not?
Thanks for your honesty, Rosalee, as well as for being authentic in your heart and emotions, I always appreciate that very much, it is clarity. Although I must admit that I am disappointed that you feel I am twisting your words, which I can honestly tell you is not the case, at least certainly not intentionally, if that’s how it came across. I do not operate this way, I know that I practice integrity and I consider myself to be straightforward and direct in my communication, best I know how, at least, always my intention.
I can’t stand mind games–and you’d know why this is–and do not feel they lend themselves to anything good, much less truth, and I’m most sorry that is not evident to you. I am human, after all, and never make any bones about that. I certainly wasn’t intending any of it to be personal!
Report comment
So to respond to your final statement, there are all kinds of ways to bring truth, light, healing and change using absolutely no money, which can spread far and wide on a physical level, beyond the virtual. I have been creating all kinds of things and helping people for decades, hardly getting back what I put out. I don’t care, as long as it’s helping people. That is really and truly gratifying and fulfilling, which leads to all good things. Ask anyone who does this kind of work, I’m not alone in that. It’s how I know I’m on my path, otherwise it wouldn’t work like this, nor would it feel good to me! I’ve no complaints at all, other than with what is going on in the world, and trying to affect that as positively as I can in a variety of ways, from my vantage point.
Between no-budget films which were labors of love, and a long-time practice working with individuals, families, communities, etc., and just plain old being there for people without asking for anything in return, I think I’ve impacted quite a few folks and it has rippled, from what I’m aware. There was some exchange of money here and there, always by mutual agreement as per services. But my volunteerism greatly outweighs any of this. I’m hardly a for-profit individual, and I don’t lack for anything and to say I am of modest means is an understatement.
I had to learn to create my life this way because my money was stolen from me by the vampirism of psychiatry, is how I guess I’d put it bluntly. To me it’s the absolute truth because it was all so fraudulent and harmful to the point of affecting my income in very direct ways, after my savings from having worked for 20 years was zapped. I know I’m not alone here. I’ve accepted it, there is no justice in this system.
But I wasn’t going to settle for living in lack, so I learned all about the energy of abundance and co-creating with the light—as we’ve discussed often—and I walk my talk, true to my word, and I live the example of this, without question. I’d invite anyone to come to my home and see how this works. It’s impossible to describe in a dialogue such as this and would involve too many personal details which are relevant but which I’m not willing to share here.
But when it comes to putting my “energy” where my mouth is, I am so prepared to do that. But I don’t know how, other than in 3D reality person, where there is no question about what I am saying, and that I am being true to my word in every respect. My partner would not only corroborate it all, he’s an example of what I’m talking about, as well. We’d illustrate by example and tell you all about how we do this, and how it came about through our adversities, to discover this, and how anyone can apply it, who is willing to learn how energy works. It’s the jewel of our journey, and it totally saved our lives.
So hey, you put out a challenge? I’m ready to meet it, head on. I’d be more than willing to give a workshop on how to co-create on any scale desired, large or small, without money 🙂 (or, at least, for extremely minimal money, way less than one would think; but still, there is a lot to be created without money, that would be hard for people to fathom due to programming, but I can change that!)
$$$♥♥♥♥♥♥♥♥♥♥♥
Report comment
Alex, as you noted you have grievances with MIA and you are entitled to your feelings, but it was disappointing and unwarranted to throw shade because I was being supportive of MIA. Let’s not forget MIA is a non-profit organization and has operating costs. There is a donate button at the top of every page – plus at the bottom of every page is a large banner that reads “Help MIA Survive – Click to Donate Now” so I don’t think my comment was at all inappropriate. Like so many on this site my goal and greatest hope is for this movement to keep growing and reach ever more people so the damage psychiatry is doing can finally be stopped. As I said psychiatrists do all sorts of projecting and proclaim there are ‘issues’ where there are none so let’s try refrain from doing that. Solidarity will make for much more progress.
Report comment
My activism is not about MiA. It’s about the world at large. It’s not personal, and in fact, quite the contrary. “Solidarity” can’t be forced, on the one hand, and on the other hand, we’re all One, like it or not.
Report comment
When I belonged to NAMI I made a $3 contribution to the membership every year. Real, “normal” members who ran the show paid $25 as I recall.
I’m now contributing this money to MIA instead.
Report comment
Phraseology aside, the issue remains of WHY psychiatric “care” should be “remade” rather than abolished.
The conflict between reformism and abolitionism remains. This has not been addressed here, not do MIA or its representatives seem to care to address it at all, opting to ignore AP or dismiss it as “fringe.”
RW has actually been more forthcoming about his rationale for “distancing” MIA from the anti-psychiatry movement in past personal communications, if he approves and I can find them perhaps we could engage in a more fruitful discussion of the issues based on this. But this doesn’t seem to be a priority, and people seem to want to make it a personal issue, something in which I have no interest. It’s a shame, really.
Report comment
We’ve got that little problem again. I’m not sure what you mean when you say you’re out to “abolish psychiatry”. I would do what Thomas Szasz consistently campaigned for, that is, abolish involuntary hospitalization. Anything short of that is reformist. Almost two hundred years ago there was all this talk of removing physical restraints, more than two hundred years later the talk is still about removing restraints. That’s reformism for you. Incremental change, reform, has two directions to go in, more tyrannical, more oppressive change, or less so. Get rid of the tyranny, the oppression, entirely, and the degree to which it exists is no longer the issue.
Report comment
Abolish involuntary hospitalization AND false advertising and lies–telling patients they have a “chemical imbalance” the “meds” will fix and claiming it’s the defective patient’s fault if the SSRI drugs drive them nuts.
Using a stethoscope to betray patients’ trust makes consent impossible.
Report comment
Outlaw undue force, sure. Outlaw fooling? I just don’t think it will go over. Practically all advertising is false advertising. People don’t sell products by being honest. Where businesses are concerned, that’s usually the road to bankruptcy court. Simply put, being truthful is not going to stop the competition from lying. There aren’t enough cells to hold all the liars, nor are there enough hospitals to detain all the fools.
Report comment
Charles Ponzi and Bernie Madoff went to prison for fooling people.
So did Farid Fata who has a LOT in common with psychiatrists though his specialty was different.
There are already laws against scams.
If I gave someone rat poison to put in his coffee in place of sugar do you think the courts would buy it if I argued, “But he chose to drink the stuff”?
Report comment
What business has “marketing and advertising” to do with medicine?
This is the core nature of the problem!
Rachel – agree – “He drank the stuff!” because he was told that the rat poison would balance his chemicals. . . lies, coercion, fraud, all of these contribute to the forced nature of psychiatry.
Report comment
Someone poisoned my drink and gave it to me and the police bought that it was ‘medicine’, so they never needed to put anything to the courts about me chosing to drink the stuff. Mind you some of the things they do to people labelled “patients’ is disgusting, but they also know that any complaints never go anywhere. In my instancce it was just unfortunate that they treated me like an animal and then found out I wasn’t really a “patient’. Never mind the power of fraud when you need to change someones status eh?
And yet here we are with penalties for tampering with food being increased by our Federal Government, and police letting the team down with their ‘discretionary powers’ and allowing citizens to be ‘spiked’ with date rape drugs for convenience.Doctors signing prescriptions for the spiking of people they haven’t even met 12 hours after they were spiked. How does that work if someone is harmed? I mean surely the person doing the spiking needs to have more qualifications than being a bus driver? Not exactly a medical degree is it?
Report comment
Charles Ponzi and Bernie Madoff went to prison for stealing money from people. Ditto, Farid Fata.
Psych drugs are a gold mine, or perhaps more aptly, an oil field, of quick cash for researchers and investors seeking to develop the next new “quick fix” and trend in “medical” palliatives.
Deception–something a little education might remedy–is not the same thing as coercion, just as an unfortunate choice in marriage partners does not always mean rape.
Report comment
Educating the public is the real answer.
It’s better to light a single candle than curse the darkness. ~Confucious
Report comment
Abolishing “forced” psychiatry is not abolishing psychiatry. There’s a big difference; one is a civil liberties issue, the other involves a deeper analysis of what psychiatry is.
Report comment
Involuntary treatment is something you abolish. Psychiatry is something you dissuade people from indulging in. There is a difference. On this, OH, you and I disagree. To abolish something you simply outlaw it. As, unlike involuntary treatment, psychiatry is a profession, freely pursued, that is not the way to go with it. Your analysis seems sketchy and flawed to me. All psychiatrists are not the same. Relieve them of this undue power that they have been granted by legislation and courts of law, and they are no longer the problem that they are today. The way you get rid of psychiatry is by boycotting it, and by, working with the market forces for competition that exist, driving it into bankruptcy. Much of its theory is already scientifically bankrupt anyway.
Report comment
I think perhaps you underestimate the power of multi-billion dollar worldwide marketing systems.
Report comment
No, I think people know anti-trust laws are no longer effective, nor enforced, that is to say, that corporate monopolies are the way of our times. I don’t, however, think everybody susceptible to bribery (i.e. corruptible) by corporate interests.
Report comment
Psychiatrists are state licensed medical abusers. We abolish psychiatry by prohibiting our government from licensing it.
Psychotherapy is a bit different, we can still prohibit the government from licensing it, but that will not eradicate it. Still very worth doing.
Life-Coaching is not licensed. But we can still sue when there are abuses, and in general we can educate people so see what is wrong with Self-Improvement.
Report comment
You can fire a life coach at any time.
Most just give you advice on finances or finding a job or time management. Less prone to abuse than others since they aren’t involved with “mental health.” Therefore easier to sue if they take advantage of you.
Some are charlatans who prey on the desperate. Dating coaches are the WORST I hear.
Report comment
Removed for moderation.
Report comment
My biggest complaint about life coaches is how expensive they are. Assuming their advice is good.
Report comment
Mmmm. And what qualifies another human being to coach my life?
Is it a degree? Participation in Amway seminars? “Spiritual” qualifications? WTF?
Now that I am older, I fear I would laugh at some young thing telling me how to organize my life…
Report comment
I’d be apt to hire a financial coach with a degree in accounting.
Usually you read their blog/book and decide to hire them based on that. If it’s practical stuff–making a career change, time management, organizing your house, managing your finances–they have little in common with “therapists.”
Health and fitness coaches or weight loss coaches are just personal trainers like you meet at the gym.
The kind most like psychologists are life coaches who specialize in feeling better and relationships. They aren’t directly in cahoots with shrinks but love to refer people they think may be “mentally ill” to community clinics. So that’s risky if you escaped.
The worst kind of all, IMHO, are the dating coaches.
Report comment
Another term that means nothing in particular. I had a psychoanalyst who was happy to refer to herself as a “life coach” if the client preferred.
Report comment
As long as they don’t force people to attend.
As Szazs (himself a counselor) said, sessions should only occur between consenting adults.
Report comment
LOL I have a degree in accounting. I don’t think that’s the one you want. Our best assets are making sure everything balances, compiling reports and statistics.
FINANCE degrees are about interpreting those stats. There may be some accountants who are wizards about seeing “how things fit together” and may be improved, but LOL I’m not one of them!
Report comment
reformism and abolitionism, yes indeed.
What forced people’s hands was just than any slavery was emboldening the pro-slavery people. So violence broke out in Kansas Territory, and then the slavery people demanded a Slave Code for the West. When they did not get this they walked out of the Democratic Convention.
You see how Psychiatry continues to advance itself, and it does this with Psychotherapy, Recovery, and with this PTMF manual.
Eventually something will happen to force people’s hands, and then abolitionism will win!
Report comment
It’s far more complex than “abolitionists vs. reformists.” We’re aiming for the critical mass needed to make most of these soporific “debates” unnecessary, which can only be done through education of the masses, ultimately accompanied by direct action. But it’s a methodical process, if we “jump the gun” we’ll just end up with more martyrs and still no movement.
Report comment
Sure, OldHead, we could die waiting for the momentum, but…no gun shot…no movement. I get it that strategy is important, but so is spontaneity. I think the movement has to be outside of the system entirely because the system is so deadly. Ever ready, in my view, beats never ready every time.
Report comment
I agree with you 100% oldhead. But as Frank states, it does not seem to be happening.
Pyschotherapy takes people into a land without honor, a land of denial. If you try to restore your honor, you will see how hard it is. But if you don’t even try, then you continue to live in denial. You do not understand what has been done to you. Likely you will end up becoming a therapist yourself.
Shutting down Psychiatry is still way out there. Putting some Psychotherapists out of business is within reach. I believe that if you have a good client who has kept notes, you could probably get a judgment against most of them. As for using that to shut them down and stop them from operating anyplace else, lets say that that is very close to my specialty.
Mostly just have to get to their clients.
Which would you rather say, “I spent the last 20 years in therapy so that I could surface my repressed pain from childhood abuses.”
OR
“I used to believe in Psychotherapy, now I see it as a scam, a con game, so for the last 20 years I’ve been putting psychotherapists out of business and educating the public about them” ?????
Honor is the key! Honor, public honor, is everything.
Perceval and the Red Knight
http://pre15.deviantart.net/25e6/th/pre/f/2011/276/2/a/perceval_and_the_red_knight_by_epictones-d4bqgwu.jpg
Report comment
Things rarely “happen”; they have to be DONE.
Report comment
When they are done, they happen. If you are talking about doing. Way to go! Let’s see more direct action.
Report comment
So while I recognize the work that R.W. and others are doing to get rid of the drugs, I also note that most involved in this work are highly compromised, as they are supporting Psychotherapy and Recovery.
So I say that at this time the new thing to do is to start using lawsuits to shut down some Psychotherapists.
We can use this to show that the whole thing is a con.
This will not eradicate it, but it will be a big improvement, and a big help in still going after psychiatry and the drugs.
So lets make some specific plans for shutting down some psychotherapists, and then we will carry them out.
Report comment
I’m imagining what it is like to shut down a psychotherapist.
“You realise that your methods are harmful?” (like we’ve been saying since Szasz?)
“OMG, really? I will stop right now!”
yeah, right. I like Frank’s perspective that the boycott of all psycho-services is a good place to begin.
Report comment
I am totally supportive of any and all such boycotts and refusals to cooperate.
My issue has been that most on this forum are advocating Psychotherapy, Recovery, and often some version of Psychiatry and belief in the idea of ~Mental Health~. I will have not have collaboration with such people.
I believe that Psychotherapists can be taken down subject to clients who are willing to talk and provide affidavits.
What Freud called Transference is simply the point at which the client realizes that they have been spilling their guts, and investing time and money, into someone who just pretends to accept what they are saying. Rather, they see what has been said as evidence of defect, or of wrong thinking.
Most people, if they can see where the therapy goes, and see how their therapist thinks, I believe that they will abandon therapy. And all the more so if they see some chance of getting compensation money for having been duped and taken advantage of.
Pertaining to this new New York state “Child Victims Act”, the proponents explain how hard it has been to obtain justice, and they say, “That’s why we changed the law.”
This is the way injustice has to be looked at, not as something to find some way to dissociate from, and then say that such is morally superior.
***************
Dr. Thomas Lemke: “Biopolitics: Current Issues and Future Challenges” he teaches at Goethe University, Frankfurt am Main
https://www.youtube.com/watch?v=GPTz0-cWDgs
Report comment
I am totally supportive of any and all such boycotts and refusals to cooperate.
I believe that Psychotherapists can be taken down subject to clients who are willing to talk and provide affidavits.
What Freud called Transference is simply the point at which the client realizes that they have been spilling their guts, and investing time and money, into someone who just pretends to accept what they are saying. Rather, they see what has been said as evidence of defect, or of wrong thinking.
Pertaining to this new New York state “Child Victims Act”, the proponents explain how hard it has been to obtain justice, and they say, “That’s why we changed the law.”
Report comment
Where oh where would one find a lawyer who would take on such a case? I know that the ones I have spoken to have behaved in a manner that could only be described as bordering on criminal negligence. They run folk around in circles for years and then claim its too late to take action.
Good news though, the folk who have finally seen some justice with the institutional abuses have shown the way around the “it was so long ago, and nothing can be done now sucker” bunch. And I dare say if people start getting together and brining action despite the immense difficulties there may be more than a few prepared to squeal on their colleagues. I’d be up for a bit of vigorous questioning given the right circumstances.
Report comment
Just an example of the type of legal represeentation available in my neck of the woods (this is not the worst example, just being used for brevity).
I approach a large law firm and spend time writing out an application for assistance. I attach the documents that I have clearly showing I was spiked with benzos and that police have been lied to in order to unlawfully detain me. My application is rejected because “my doctor authorised the drugging without knowledge with benzos”. I have no prescription for these drugs, and never have.
So I call the law firm concerned and explain the situation again. I ask, “Who is my doctor who authorised this spiking?” To which I receive the reply “We can’t tell you that”. Now that just seemed a little more than strange to me. I have provided them with the documents and they would be aware that I did not have a doctor when the offence occurred. Or if they falsely believed I did then why not name that doctor, surely that can’t be a problem …. unless. Unless of course it would mean that I would knock down their preference for these to not be criminal offences and not start the dominoes falling.
This is the sort of gaslighting one is up against. Doctors who remain in the shadows prescribing drugs to people 12 hours before they even meet their patient. Lawyers appointing doctors to people and not giving anyone the right to respond to their false claims, though I note that they still require payment. I just thought I would have ad the right to know (a) who my doctor is and (b) what types of drugs I can be spiked with and by whom. Not so my government tells me. And lawyers agree. Now maybe if I were a “patient” but these people are fully aware that this was not the case and it was simply a lie told to police to make torture and kidnapping appear lawful. Takes some sort of fool to not see that in the evidence so whats the deal with these legal representatives? Seeking favour with the powers that be? Anyone offended by a government that is kidnapping and torturing citizens? Because I have the proof. And I consider 8 years of obstruction a further breach of the Convention (along with the refoulments already committed eg attempt to kill, threatening my family)
The reason I was drugged without knowledge to be able to plant a knife and some cannabis on me (along with causing an ‘acute stress reaction’ to force me to talk ie torture) was precicely because I did not have a doctor and thus they required a police referral to the Community Nurse. Had I a doctor they would simply have made a referral if they had the power to do so (ie must have seen patient within 48 hours for lawful referral). And what I know is that these people were desperate for me to go to my doctor and GET a referral after this all blew up in their faces. Now if they werent aware that I wasn’t a “patient” why the desperate need for referral? I know one psychiatrist you asked and who said “no”.
Bah, just kill him in the ED and be done with it. A hot shot with someone elses morphine on top of a ‘chemical restraint’ and the Coroner will not be able to identify where the morphine came from. My hands are clean eh Doc? Unfortunate someone noticed really, you could have gone on for years. Oh wait, you did. Took them a little while to catch up huh. Chief Psychiatrist smells a rat when he notices that he didn’t write the poison pen letter. Danger, frauds at work.
Report comment
“….The second-generation story: Prozac and other second-generation antidepressants are understood to provide, at best, a marginal benefit over placebo in the short term. In government-funded studies, the second-generation antipsychotics were not found to be any more effective than the first generation…”
I was placed 1st Generation Trí cyclic antidepressants many years ago and they made no difference whatsoever to my mood:- Going on them, being on them, and coming off them made no difference whatsoever to my mood!
Report comment
I did not read the comments but I see there are many. I attended the first webinar. I noticed that I saw very few familiar names there, which is promising. Many were MH workers of various sorts from Oregon and had a lot of knowledge of Oregon-specific issues. They definitely reacted positively and seemed to be learning!
I also felt that Bob Nikkel’s presentation was realistic because in many ways, their efforts did not succeed. I question how public health officials measure “health.” I took a public health class recently. This was an undergraduate class. These students were likely much younger and less experienced than me. They foolishly measured “health” by “number of doctor visits” and “percentage of people who go get vaccines.” Actually, I suspect this is the prevailing view, pushed by the media. So if I saw a psychiatrist twice a month and a therapist twice a week, I’d be more healthy? If I took a cocktail of blood pressure pills, cholesterol pills, and HRT, I’d be more healthy? I’d likely be dead! It looks like people just don’t get it.
I would not say psychiatry has failed. Psychiatry is a dark shadow in our history, an abomination, an embarrassment.
People wonder why, when the Nazis were rising in power in Germany, the story never reached most of the North American public. The reason is that the media did not publish these stories, or when they did, it was some tiny article in a remote corner of the newspapers. There was growing Antisemitic sentiment shared among the most powerful and richest influencers of the day. Their companies funded the papers through advertising.
This is exactly what is happening now. They squelch our stories. They silence us in any way possible, even using illegal means to keep us out of the mainstream media. We continue to grow in numbers and are more successful at shouting loudly, but are dismissed as nutcases. When I explain to people that I “got better” because I got all MH “care” out of my life, they say, “Oh but you’re an exception.” I’m honestly tired of hearing that. I have known others who have done the same, ditched them all, and what’s cool is that EVENTUALLY, these folks flourish. It takes time to get through the grieving and financial wreckage.
Psychiatry should be abolished. The drugs are only a side issue. Psychiatry is guilty of heavily influencing society on all levels, encouraging eugenics, that is, the separation of the supposedly sane and the supposedly insane. The media supports this idea, that we should be given “care,” which might include incarceration. That we should be put out of work and then, handed an embarrassment of an income from the State. That we should become property of the State, which now controls and monitors our finances and our living situation. We are rounded up and put in ghettos or prisons.
Their “care” should be exposed for what it truly is. The Nazis lied about the showers and psychiatry is lying about what it does, too. We need to inform and enlighten the public so that psychiatric “care” can be stopped. Ended. We need to save our people from the fate we ourselves befell.
A new era should begin, not based on hatred and fear of “other,” but based on love.
Report comment
You are an exception. So am I and many others here.
Most don’t get better. They stay in the system, deteriorate and die. 🙁
We need more exceptions.
Report comment
Psychiatry should be abolished. The drugs are only a side issue.
Touche!
Report comment
Yes, totally abolished, with Crimes Against Humanities prosecution for the Current Practitioners. Following the law, following orders are not an excuse.
Report comment
I hear Albert Pierrepoint is out of work.
Take a leaf out of our current Minister for Healths book (ie calling torture “referral”) and call it neck manipulation and that way Pierrepoint can claim it on Medicare.
Even better news, the ability to overlook human rights abuses? Y’all started it 🙂
Report comment
I like the concept of changing psychiatric care. However, based on my experience as a patient on long-term parenteral nutrition (Nutrition delivered through an IV directly to the bloodstream) I would say that change is only a remote possibility. You are talking about changing healthcare as a whole. If you ask me what frightens me most in the United States it is going to a hospital or doctor’s office. Nutrition Support patients spoke about medical kidnapping behind the scenes at our last Oley conference (a conference geared towards those on nutrition support.) Patients shared their fears of “mental illness” diagnosis. Most of the patients are terrified to see a psychologist because it can be used against us to take control over our lives. I have known patients that have been force fed through a feeding tube begging the nurse to stop. They refuse to end the torture and they ultimately kill the patient. As someone on nutrition support I am abused by the healthcare profession weekly. It is something I am not allowed to speak about because patient abuse is where rape used to be. It must be the patients fault. People the work in healthcare can do no wrong. Unfortunately psychiatry like the other healthcare professions are not about getting people better. People with physical health conditions are misdiagnosed with mental health conditions instead of doctors looking for answers. I fear something drastic must happen to cause change in care. It would require holding doctors and nurses accountable for their behavior and that isn’t going to happen anytime soon.
Report comment
Wow, TooStubbon
You are so right. Not even the same thing but..
I was referred to a specialist, who’s treatment options left a lot to be desired, ie he wants to operate and the stats for successful outcomes are not that great. I declined. The office/practice insists that I must come in for follow up care (?) monthly, 130s mile round trip. I demurred. A few weeks ago I received a letter telling me they are ‘firing’ me as a patient. Huh. There is a possibility that at some point in my aging I will need a specialist of this type so did I screw myself for not following their revenuing plans??
And then there’s the scary thought of being incapacitated and at the mercy of “ModernMedicineTM” I heard horror stories of Advance Directives not being honored.
It is just sickening how money has corrupted every aspect of our lives…
Report comment
Advanced directives are only as good as the doctors who are supposed to abide by them. As a hospital chaplain I saw lots of abuses against advanced directives. Families try to get around them too.
Report comment
One of the problems with our system is that people can self appoint as your power of attorney, and then lawyers and doctors don’t need to inform you that your not speaking for yourself anymore. So for example, the person who spikes me rings the lawyers I approach and claims (falsely) that they have power of attorney for me, and then the lawyers simply state to me that there are things they can not tell me.What is it that they can not tell me? That the person who put drugs into my drink without my knowledge doesn’t want to go to prison and so they want no action taken. I would have thought that lawyers and doctors would need some form of evidence that this person was acting on behalf of another before doing this but ….. I mean imagine how this works with rapists. Vicitm contacts police and then police are contacted by the newly appointed power of attorney and told drop the complaint. And that is what happened to me when I complained about the spiking, FACT. No checking if the person claiming to be my doctor actually was, simply prefer that to be true and so it is. FACT
I would have thought that the admission by my ‘carer’ to attempting to plunge a knife into my chest whilst I was laying on a couch might have been a clue, or the fact she stated she had spiked me with benzos to deprive me of my liberty and make it easy to plant a knife on me but no. Just don’t seem like caring things to do to me, but police obviously see it otherwise. And of course she convinced a Community Nurse to lie to police and that really was the kicker, they were up for beating a mental patient then. Kneejerk action, mental patient get the guns loaded. No checks and when it became apparent during my interrogation that I wasn’t a “patient” the subject was immediately dropped and redirected to me being verballed. Bit like their wrongful convictions, don’t stop when you come up against something that means this person couldn’t have done the criime, just get rid of any inconvenient truth. FACT
This Community Nurse knew at first he was torturing someone he thought was a patient (note to authorities, he has been doing ‘remotes’ for private clinic psychologists FACT), but step it up when he knew he was torturing a citizen and was about to kidnap them. And let me swear this before God, he knew alright. And wasn’t he worried about the police figuring it out. Got a lot of respect for their intelligence huh Mr Community Nurse, And boy did you think quick on your feet, mind you you werent the one who had been spiked with benzos huh.
Report comment
I’m not sure there is such a thing as “medical kidnapping” ToostubborntoDie, its simply kidnapping. (Dr John Kearsley was not doing a breast examination, its actually called sexual assault) Though as a victim of this conduct by someone pretending to have the authority to do it (and who stooged police into helping him) I have found that the embarrassment for our police of being assistants to a kidnapper is just too great for them to want to do anything about it, and so they provide further assistance to compound or conceal evidence of criminal offences, fail to perform their duties, and conspire to pervert the course of justice. All further serious criminal offences but given they are the ones who decide what action is taken against criminals, they decide that none will ever be taken.
It is an assumption made by those with a duty to act against such kidnappings that the criminal was acting in “good faith” that created problems for me. They are good people who are trying to ‘help’. This was nothing of the sort and was a vicious attack on me by a psychologist who did not like some of the things I had to say, and took the opportunity to exploit her position to harm me, and by proxy my family. Still, she is off doing it to many others while I bang my head against a brick wall and attempt to have her enablers do their duty. Though I have begun to realise that these are the same folk who enabled child raping priests for 30 plus years, and we know how thats worked out. “We viewed these assaults as being the result of ‘character flaws’ and not as ‘criminal offences’. Really? Talk about the proverbial blind eye.
I’m sure the police/mental health ‘professionals’ frown on the kidnapper in their midst, but reputation rules so they must provide support to corrupt public officers unfortunately. In fact it can be quite handy to have such a person in your pocket.
Advanced directives are a bit like your human rights, only effective when you don’t need them. I think it was George Carlin who said “think you’ve got human rights? Google Japanese Americans 1940”.
Report comment
So, my point is that in the case of Prof. John Kearsley when he spiked the young womans drink with half the amount of benzodiazepines that I was given and she woke to him sucking on her nipple this was not a “medical sexual assault” but rather simply a “sexual assault”. Now this guy has the right to prescribe these date rape drugs. The people who decided to spike me had no such prescribing rights, and were fully aware that I would not take them even if doctor suggested that I do. Still when one needs to plant items for police, the target being conscious can be a problem so my government tells me they are allowing citizens to spike other citizens with benzos if its in a good cause (ie makes police job easier if the evidence is planted). And any complaints and they slander folk with the “theres no evidence of the drugging therefore this is a paranoid delusion and the nutjoib needs drugging”.
Secondly, this issue of police discretionary powers allows racism to run rampant in our institutions. By being allowed to decide who is and isn’t charged any claim that the numbers of people who are black and in prison is a result of racism can be dismissed easily. Its just a coincidence that black people are charged more often than white folk, and seem to end up with prison sentences for such serious matters as stealing a packet of pencils from Walmart, but a kidnapper can be overlooked because he’s a nice guy and plays on the same football team as me.
When you think about it though police don’t really have a lot of use for pencils. Whereas someone who can arrange spikings with stupefying drugs and kidnappings and make it look like “medicine” might be handy if you wanted to subject someone to an interrogation and thought they wouldn’t talk. And then just exercise your discretionary afterwards. I mean it does violate the Convention against the use of Torture but …. you gunna complain to police about it? The public? Waaahahahaha they tell me they’ll fuking destroy you if you do.
Mental Health can even clean up the ‘mess’ afterwards by chemically restraining the victim and calling the resulting behaviours a mental illness with there slandering and fraud. Seen it done and well, have a set of documents that would be a great training resource for anyone wishing to do it. Policegave up trying to retrieve them when it was realised they hd gone too far. Too many eyes watching to keep committing serious offences against the public. Not a good look threatening psychologists to find out “who else has got the documents”. Can put you in touch with a Clinical Director if fine tuning is required.
Report comment
I’m not sure there is such a thing as “medical kidnapping” ToostubborntoDie, its simply kidnapping.
Good distinction. Or maybe “kidnapping using the trappings of medicine,” to borrow from phraseology sometimes used to describe psychiatry in general.
Report comment
Wow, impressive post!
Report comment
I’m not sure how you reform social control to be anything but another form of social control.
I.e. shit is any form is shit. 🙂
I don’t think we need “professionals” period, as a rule of thumb. So I wouldn’t waste a lot of time trying to figure out how they “should” or “might” think or operate. Great first post though, welcome!
Report comment
I don’t think we’re disagreeing on anything substantial here. We’re talking strategy. The issue is always does change come from the top down or the bottom up, and the answer is often “both” — though if it is ONLY from the top it’s more likely a containment strategy.
Those who find themselves working within the system while in the grips of an epiphany about the true function of psychiatry and the damage it wreaks are in key positions to be allies in the struggle to expose and abolish psychiatry, and if they act as allies and not “reformers” — even if they don’t shout this from the rooftops — they can be of great value to the AP movement, which is to say of people everywhere. 🙂
Report comment
Great followup. Nothing much to add.
Report comment
I will guarantee that anyone at all working in this system is wearing two faces. There is no way to be part of any corrupt system in any capacity without compromising oneself in ways one might not even be aware of. They are lying to themselves and to others, and more than likely without awareness. That is the nature of corruption, and it will touch everyone who is connected to the corrupt system, especially if there is a paycheck involved, or any kind of “reward” for going along with the program (like, keeping your job). That skews everything, and absolutely nothing is clear or trustworthy.
Even if one is feigning loyalty and is, in reality, opposed in principle, they’re still holding up the system by participating day after day. I don’t see how it can be any other way. The truthlessness and irrationality of it all runs so deep, which is seriously dangerous to a society asleep! Waking up is the only way to go, as I see it. Being truthful, and really honest with oneself, is a good place to start, for a change.
Report comment
I wouldn’t expect psychiatrists and professionals on “the inside” to work to destroy “the inside” rather than reform it. I think the only good place to oppose that system, without being complicit, to one degree or another, is outside of it. “Top down” or “bottom up” are irrelevant outside of that system, instead, you’ve got other systems to deal with. Get rid of that system, and it’s kaput. A pin prick is all it takes, conceptually speaking anyway, and *pop* you’ve got no more mental health treatment system bubble.
Report comment
Corruption: Issue Intoxication by deception aka spiking.
You go to police with documents showing that you have been spiked with benzos thinking that they will take a complaint and act. Wrong, they don’t have a copy of the criminal code. Truth is someone claiming to be my doctor had rung them and given instructions not to take a complaint and not accept the documents. And they did what they were told. Now had they taken the documents and looked a little further they would have noticed a conspiracy to kidnap and torture. But they preferred the false “patient” narrative.
Problem: people who have kidnapped and tortured know I have the proof and am going to police with it. “Hi Sgt Im a doctor and you’re going to do as I say” which provides time to arrange a killing in the ED. However another doctor notices and the killing is interupted. Criminals think they have retrieved the documents and all should be sweet, they have used police resources to destroy a “patient”.
I go back to police with documents and they still don’t want to act against the people who are claiming that I am their “patient” and now they tell me that its best they dont know about the attempt to murder me in the ED.
See the thing is that police are really afraid of the organised criminals operating in our hospitals and find it best they do what they are told by them. They are fully aware of what happens legally when you acquire the status of “patient”. I mean they are the ones dishing out the kickings to these said “patients” (shooting the odd one now and then too). You can be killed and not a damn thing the authorities can do about it. This is what is so sinister about the Mental Health Act and the powers given to psychiatrists (and by proxy their psychologist wives).
So I still find myself being misdirected by our current Minister for Health into a complaints process involving doctors. These may be doctors but in this situation they were acting like criminals and as such should be directed to police.
Too late, they are way in over their heads now. A pile of bodies as a result of Sgts negligence and well, criminal conduct in failing to perform his duty.
Anyone here doubt that spiking drinks with intoxicating drugs without knowledge is a medical issue? I get it that its an ugly look for police that they turned me away while the criminals arranged to have me killed in an ED. And still they persist in claiming this is a medical issue. Must use this quite often, for example if a child complains about being drugged and raped by a priest. Call it spreading the love of Jesus (thinking of you Minister) and send them back to the church for referral to Doc (SMO).
Corruption? Most of them have fallen into this as a result of stupidity or plain old laziness, and now find themselves digging a hole deeper that Krakatoa.
Lets start with S.C. McK. I sent you some letters pointing out some facts SC. What happened to them? And I know its best you don’t know about that, but now that you do what did you do? “Insufficient evidence” ? You really expect a Commuunity Nurse who is kidnapping and torturing citizens to document his crimes by completing an Incident Report and having toxicology done on the victim of a spiking? The crimes are there for someone with enough intelligence to solve a 5th grade puzzle SC. He’s been overlooking this for the guys at the football club for years when rape victims turn up for ‘assessment’. Still don’t get off your seat SC your donuts will get cold.
Report comment
Alex speaks of the corrupt system.
This seems to apply to military, police abuses as well.
Where there is a pack of people “following orders” from top down to protect corporate interests.
I know this is paranoid, but I’m beginning to wonder – when we take on the Corporate Masters – what are we in for?
Report comment
Exactly. It is professional sacrifice to not be complicit one way or another. So be it. It’s called courage and integrity to not enable corruption when one awakens to the fact that they are contributing to it as much as they are complaining about it and blaming others for it. Don’t participate, walk away!
Or, speak up and out and expect to get fired, and be damn proud of yourself for speaking and living truth, which really does set us free. People get fired all the time and take new avenues which present themselves. It’s called *INSPIRING CHANGE.* Followed by *being the change,* which is the natural and logical progression from inspiration.
The hope to reform a corrupt system is only upholding corruption. What, suddenly these people will become honest? I think not. It will take a lot of humbling to make that kind of turnaround, if it were to even happen in this lifetime. Making psychiatry obsolete requires abandoning it completely, and ironically, it’s only success has been to make people dependent on it. So there are double binds to face.
And there’s the divide and conquer at work, the civil war among the pawns in this sinister, immoral, and hopelessly self-serving game of “Hey, who has the power here? And how many people do I have to use, split, and bleed dry in order to prove it!”
The phrase, “These are not very nice people” comes to mind.
Report comment
“I know this is paranoid, but I’m beginning to wonder – when we take on the Corporate Masters – what are we in for?”
JanCarol, why paranoid? Sorely needed change is what we’re in for–freedom from oppression and tyranny, as covert as these may seem at times. This is the reality to which people have been awakening for a while now and from which we want to ascend, en masse. The power is in the truth, and when we align with that, we are owning our power.
We know change is unpredictable, but it’s not only needed, it is inevitable at this point, thank God. Embrace the unknown! As we move in present time with moment to moment awareness, we have ample opportunity to create a new future.
Report comment
I was reading in Brave New World today. The chapter where the Savage approaches a bunch of Deltas, clamouring for their allotment of Soma. . .
“It’s poison! You are slaves!” he cries, “Don’t you want to be free?” as he knocks the Soma out of the hands of those distributing it. He throws it out the window, scattering it to the wind –
And chaos ensues, the people want their poison, they want their slavery, and a riot breaks out…the Savage is arrested, and the Riot Police arrive with spray guns of Soma and Tranquilisers to subdue the agitated crowd. The Synthetic Music Box runs “Anti-Riot Speech Number Two (Medium Strength)” which tells the people,
“‘My friends, my friends!’…pathetically, with a note of infinitely tender reproach… ‘What is the meaning of this? Why aren’t you all being happy and good together? Happy and good…At peace, at peace.’ …It sank into a whisper and momentarily expired, ‘Oh, I do want you to be happy,’ it began with a yearning earnestness, ‘I do so want you to be good! Please, please be good and . . . ‘ ”
(paraphrased).
It’s getting close to this. The devices and phones are the box, and Soma is everywhere. . .
Report comment
Fortunately, we have the option of ascending from these played roles and old stories now. I’d say it is an *expanding* new world. Be…whatever! To live in fear or in faith is always choice.
Report comment
Anomie, Wow, another excellent post!
From my own experience with two psychiatrists one relished in her power to punish and “other” me while in cancer treatment but another psychiatrist I saw 10 years earlier at my own request (after my younger brother’s sudden unexplained death on psych drugs, and a workplace accident, etc) was dismayed by what took place. He called it a “horror story” and urged me to fight it. When I told him all this psychiatrist did that was so unethical and unjust he told me I was “preaching to the choir”. But I am well aware that due to the hierarchy he is not at liberty to speak out. The dismantling of psychiatry and its power to abuse can be accelerated when all dissident psychiatrists are driven to speak out. Thankfully there are a few who do speak out on this great website!
You wrote “Psychiatry is like a virus, and it’s spread into the entire medical system.”
YES! “Virus” is a very good description and it has spread into the entire medical system! Psychiatry was used to endlessly punish me because I tried to make my own medical decisions on a questionable cancer “diagnosis” (that was in fact totally OVER diagnosed) Thanks for your thoughtful posts.
Report comment
I agree that psychiatry is a virus – but I would say it has infected more than the medical system.
it has also infected the courts. The schools. The family. The media. It’s a pretty prevalent virus – might even be a retrovirus, that puts its fingers into every system it possibly can.
How do you kill a retrovirus? (hint, you can’t, not yet – we haven’t come that far with stem cells yet) We don’t know how – so all we do is “manage” a retrovirus.
But stop feeding it is a good place to begin.
Report comment
Our current Minister for Health likes to use psychiatry to conceal human rights abuses. He is like the thief who wants his stealing to be an illness called kleptomania. By medicalizing the human rights abuses he knows they can side step all those pesky agreements not to torture and use arbitrary detentions. Mind you who is going to complain about a guy who with a phone call can have you (and your family) fuking destroyed.
So despite knowing full well that I was kidnapped and tortured he simply relabels this as being ‘referral’ and ‘detention’ and misdirects complaints to a medical watchdog with no teeth, and with a whistle slanders the complainant. They say you get what you pay for and this guy is getting a few too many peanuts for some seriously old cons.
Report comment
I call it vampiristic (a virus is, after all, parasitic and depends on a “host” for it to thrive) but either way, yes, it’s insidious, relentless, and dangerous, and certainly behaves as though it has *aversion* to truth and light, whether it’s about healing or justice.
This is worth repeating–
“But stop feeding it is a good place to begin.”
Individuals are, by nature, self-healing and can actively build immunity to viruses so they do not become a host to parasites. The more that do, the more society on the whole becomes immune. Parasites cannot survive without a host, on whom they are completely 100% dependent.
Report comment
I believe that Psychotherapy and Recovery, feed Psychiatry. If people believe in the former two, then they will also believe in the latter for more severe and recalcitrant cases.
Report comment
Anomie you mention New Language:
(sorry, can’t resist)
https://youtu.be/e111qCt4B-Y
Report comment
Dissident psychiatrists are much like many Congressional Republicans. They’re not going to say a damned thing because they themselves want to stay in power.
Report comment
Anomie, much truth and wisdom in what you write. People who are jobless, homeless etc being psychiatrically labelled for their hardships is a heartless and corrupt cover-up of reality.
You wrote: “Being disheveled, sleep deprived, and malnourished will make anyone appear in a way that psychiatry can place a label on.”
Yes, I found that out when during cancer treatment I became very ill and sleep deprived and sent to a psychiatrist for “help with sleep meds”. Among the many effects chemo had was nausea and ravaging my throat membranes so bad I could barely swallow water. All my hair fell out and I became very thin – from the effects of chemo – but the psychiatrist used my appearance against me to support psych labels. It was winter and I bought a head covering for cancer patients (at the cancer hospital) but the psychiatrist wrote “patient appeared with a scarf wrapped around her head” trying to make it sound like it was bizarre behaviour. She also stated I was “very thin” and it was chalked up to “anorexia”. Until it happened to me I had no idea of the blatant lies, betrayals and distortions of reality psychiatry revels in. It’s time for a present-day version of “One Flew Over the Cuckoo’s Nest”.
Report comment
Should have my e-book on Kindle Monday.
Psyched! Five flash fictions about the mental system.
Report comment
Sweet!
Report comment
Anomie, thanks for your comment and the link. Yes I cringe reading cancer patients “should be asked at every visit about anxiety or depression” and patients “should speak up” about these issues. Yep, let’s just keep spreading that virus!
Mine is a twisted saga as I was bullied right from the get-go by an arrogant oncologist. He immediately fear-mongered and said I won’t be alive in 3 years if I only have standard chemo drugs as he wanted me in a clinical trial so he would be an ‘associate’ doctor and earn a big payday from BigPharma. This meant adding a 4th drug to my cocktail and signing off on “side effects” of heart attack, stroke, vision loss, intestinal rupturing etc. I read all the info and told him I felt it was best I decline. He blew up in anger, threw his pen across the desk and with eyes blazing stormed out of the room.
I did start standard chemo and the 1st round flattened me. I was so dizzy and weak I fell, hit my head on the floor and laid unconscious bleeding from a gash to my head. My family doctor stitched up my head and sent me to the ER for a CT scan but the oncologist completely dismissed the incident. The carboplatin in my 1st round triggered vertigo & tinnitus so severe I only managed to walk around the house holding onto walls and furniture. I was due for a 2nd round in 3 weeks but my white cells were so flattened the 2nd round had to be delayed an extra 2 weeks. By then the vertigo had improved by 60%. I asked for dosages of the other drugs to be reduced by 25% and requested to drop carboplatin altogether as it’s known for cumulative and permanent damage to the inner ear. He refused. A 2nd round of carboplatin was forced on me and triggered severe vertigo again. I held my ground and refused a 3rd dose. I was scheduled for 6 rounds but I quit chemo altogether after 4 rounds. Lots of permanent damage and health issues from chemo I didn’t need and years later I’m still alive to talk about my terminal diagnosis. To be sent to a callous psychiatrist whose only goal was to degrade and label me was a double whammy. Lots more to the story but I better quit here. (Btw, the clinical trial was halted because of too many fatal “side effects” occurring.)
Report comment
Thank you for this anomie!
I also wonder about the flip side of the coin: if psych drugs affect metabolism (they do), endocrine (they do), autoimmune functions (they do), the gut (they do) – then do they contribute to cancer forming?
It’s a question which will never be answered, but enquiring minds . . .
Report comment
Here is a numbers model of the symptoms of ‘racing thoughts’ and ‘false beliefs’ observed in many psychosis cases. The model uses true/false information only, without specifying content.
Generally our brains process one unit of input into one unit of contained information. If the thought process switches to a multiple messaging mode then one input can produce multiple units of contained information. What should be considered is that these multiple units will contain high rates of false information (because true information tends to be singular). Not only is the overall amount of processing increasing but the percentage of false information is increasing. A tipping point (onset of psychosis) would be expected if the amount of false information exceeds a normal fact checking ability. For example it may be normal to fact check 20 to 40 items per day but if a person was unaware of this mechanism he/she would not be unable to fact check 200 to 400 items per day.
Using ballpark numbers for normal and psychosis:
Normal
*Normal significant information units processed per day 20000
*Coefficient of true information with normal thought pattern 9980 per 10000 or .9980
*Coefficient of false information with normal thought pattern 20 per 10000 or .0020
*Normal daily true information = .9980 * 20000 = 19960 units of true information
*Normal daily false information = .0020 * 20000 = 40 units of false information, may be corrected
Psychosis
*Psychosis significant information units processed per day 80000
*Coefficient of true information with multiple messaging 9940 per 10000 or .9940
*Coefficient of false information with multiple messaging 60 per 10000 or .0060
*Psychosis daily true information = .9940 * 80000 = 79520 units of true information
*Psychosis daily false information = .0060 * 80000 = 480 units of false information, not corrected
High processing rates combined with relatively tiny coefficients of false information will increase the overall presence of false information to levels that may cause problems.
Notes: This model uses 20000 information units per day as a benchmark for normal thought patterns. The coefficient values are based on observed symptoms and will vary from case to case. This model in no way shows biological failure but shows processes of information mechanics
Report comment
Remake Psychiatry? They tried that with religion. Just more churches, more clubs. Do people have problems? Do people need help? A definite yes. I would say that most need tools, tools take a lifetime of gathering. They need a ton of social support, but not of the saviour kind…. a support system that does not use labels or drugs. Once a week or month visits to a therapist, revisiting ‘trauma’ are not helpful for me. What the majority of people need most is to be thought of and viewed/treated as normal. (whatever the heck that means) wait I think shrinks are the role models.
Report comment
I do know of a whole lot of systems that could weaken psychiatry.
The thing is, psychiatry has already been exposed. The reason they complain about “anti-psychiatry movements”, is to divert attention away from their sham business. Psychiatry is a convenience or has been, to politicians, but I do not see that going on for ever, because it is not sustainable. So far psychiatry has convinced the politicians that everyone is mentally ill and in order to manage these illnesses, they need drugs.
But all that has happened since psychiatry are, more dependent people, more disability, more illness, more crime, more suicides.
Politicians have to be lobbied for alternative schooling, about the dangers of drugs, about human rights regarding children and drugs, and forced drugs and incarcerations.
These changes should be demanded, and the proper truthful reasons of how/why psychiatry has long overstepped the boundaries/autonomy of human beings.
We can’t even, or politicians can’t even argue for it’s usefulness, even as social control. We have to start within the political arena.
Asking Mr shrink to change is not resulting in change. Our therapies are not working on that defensive lot.
Report comment