Thomas Insel’s book Healing: Our Path From Mental Illness to Mental Health is getting a fair amount of media attention, which could be expected given that he was the director of the National Institute for Mental Health for 13 years (2002 – 2015). The book was blurbed by a number of prominent figures, including Rosalynn Carter and Patrick Kennedy, and most reviews have been fairly positive, telling of how “America’s Psychiatrist” has discovered that psychiatry’s somatic therapies—drugs, ECT and such—need to be complemented by social supports that provide “purpose” in life and social connections.
MIA has run two reviews of the book, one by Bruce Levine and the second by Andrew Scull, both of whom offered a more critical assessment. I think it’s fair to say that their reviews reveal how it functions as a work of propaganda.
Personally, I have been mulling over the import of this book ever since it was published. I was focused on a very particular question. Given that Insel opened his book promising to investigate why mental health outcomes in the United States are so poor, would he tell of research, much of which was funded by the NIMH, on the long-term effects of psychiatric drugs?
There was an obvious ethical obligation for him to do so.
There is a basic compact that necessarily exists between any medical discipline and the public. While the public may understand that it is possible for a medical specialty to embrace practices that, at some point in the future, will be found to be harmful, and to do so in good faith, there is the expectation that a medical specialty will be an honest purveyor of scientific findings about the risks and benefits of a medical intervention, and that if its research tells of treatment that is worsening long-term outcomes, then the medical specialty will inform the public of those outcomes and rethink its practices.
For the longest time, psychiatry has failed to fulfill that pact, a failure that Insel had an opportunity to remedy with this book. And I don’t think it is hyperbole to conclude that as he took up his pen, the future of mental health care in the United States—and the narrative that would govern that care—was at stake.
If Insel had decided to direct public attention to the long-term studies, it could have put psychiatry on a new path. Once the public had been informed by “America’s psychiatrist” that there was a history of research that told of how psychiatric drugs worsened long-term outcomes, then our society, with that new narrative in mind, would have been motivated to find alternatives to the drugs as first-line therapies.
But Insel decided to keep the long-term studies hidden, and that means nothing will change, and our society will keep on doing what it has been doing, which has been relying on drugs as our go-to solution for the emotional and mental struggles that may plague us.
Insel Promises to Investigate a Conundrum
I opened my book Anatomy of an Epidemic, which was published in 2010, with this line: “This is the story of a medical puzzle.”
The conventional history of psychiatry tells of how the introduction of antipsychotics in 1955 kicked off a psychopharmacological revolution, a great advance in care. The revolution was then said to take another step forward with the development of a second generation of psychiatric drugs, starting with the marketing of Prozac in 1988. The prescribing of psychiatry drugs soared after that, and as it did, the burden of mental illness in our society, rather than diminishing, noticeably increased. The most visible marker of this could be seen in government disability data. The number of adults receiving a social security payment—either an SSI or SSDI payment—due to a mental disorder rose from around 1.25 million in 1987 to nearly 4 million in 2007, and is now around 6 million, according to Insel’s book.
Usually, a great advance in medicine—and an increase in the number of people treated for the disease—reduces the burden of that illness in society. Here the opposite was true. Why was this so?
This is the question that Insel takes up in his book. In his first chapter, he tells of the worsening of outcomes in this sphere of medicine: rising disability numbers, more suicides, and an increase in mortality, with the mentally ill dying 15 to 30 years earlier than the general population. He then notes how this worsening happened during a period of increased spending on mental health services, with a dramatic jump in people receiving outpatient care and taking psychiatric drugs. He writes:
It’s a pretty safe bet in most of medicine that if you treat more people, death and disability drop. But when it comes to mental illness, there are more people getting more treatment than ever, yet death and disability continue to rise. How can more treatment be associated with worse outcomes?
Now, there may be many factors that have contributed to our society’s worsening mental health. But the correlation between a dramatic increase in treatment and a dramatic increase in disability raises an obvious factor to investigate: What are the long-term effects of psychiatric medications? Do they, in the aggregate, improve long-term outcomes and the functional well-being of those who take them? Or do they, for some reason, have the opposite impact?
This is a question vital to public health, and important to every individual who may consider taking psychiatric drugs. It is central to informed consent, both at the societal and individual level. I sought to answer the question by digging through the research literature, and with each class of drugs, basically followed this methodology:
- What was the clinical course of the specific disorder—e.g. schizophrenia, depression, etc. — before the introduction of psychiatric drugs?
- After the first-generation psychiatric drugs were introduced, did clinicians observe any change in the clinical course of their patients?
- In clinical studies that measured long-term outcomes, did the medicated or unmedicated patients have better outcomes?
- Did modern epidemiological studies find that the disorder now runs a more chronic course than before the introduction of psychiatric drugs?
- In response to findings that indicated the medications were increasing the chronicity of psychiatric disorders, did researchers put forth a biological explanation for why the drugs would have this effect?
I was following a process that reviewed a history of research to see whether the different studies, much like pieces of a puzzle, fit together to tell a coherent story about the long-term impact of psychiatric drugs. The conclusion that emerges from that process is that antipsychotics, antidepressants, and benzodiazepines worsen long-term outcomes, and that bipolar disorder, which is regularly treated with polypharmacy, runs a much more chronic course than manic depressive disorder—the diagnostic precursor to bipolar—once did.
That is an upsetting conclusion, and while there was a great deal of pushback from some prominent American psychiatrists (and defenders of the mainstream narrative), the book did help draw societal—and professional attention—to the issue at hand. How do psychiatric drugs impact people over the long-term?
In March of 2015, filmmaker Kevin Miller interviewed Thomas Insel for a documentary he was making, Letters from Generation RX, and he asked him about the “science of psychiatric drugs” that was presented in Anatomy of an Epidemic. Here is what Insel said at that time:
I will take one piece of what he said to heart—and I think it’s an important one. And his comment is to observe that in spite of this enormous increase in the use of antidepressants, antipsychotics, and other neuroleptic or psychotropic medication, which is that broad class, over the last two to three decades—it’s been difficult to demonstrate a commensurate decrease in morbidity, that is, disability or mortality, measured by suicide. Now, in other areas of medicine, if you increase the use of your medication twofold, threefold, sixfold, you will see—we have seen, reductions in morbidity and mortality. Now, we can argue about whether in those people who get the right medication at the right dose for the right duration, there really have been lives saved and there have been reductions in disability. Every one of us has seen people who have done beautifully, and whose lives have been saved by the use of medication. But at a population level, his observation needs to be taken very seriously.
That’s an honest response. Insel, at that time, was validating the question as of great importance to society, and to our public health.
In 2015, when Kevin Miller told me of his response, I felt a moment of optimism. The possibility for a societal rethinking of psychiatric care loomed large at that moment. Insel didn’t even need to review the full collection of research that I had reported on in Anatomy of an Epidemic. If he simply reviewed the NIMH-funded research that I had cited in the book and made those NIMH findings known to the public, then that would prompt societal thinking about the merits of these drugs to undergo a profound shift.
The future of our societal use of psychiatric drugs was in his hands, and in his first chapter of Healing, he raised the puzzle that I had sought to investigate in Anatomy of an Epidemic. He wrote of how there was a stunning correlation between worsening mental health outcomes and increased treatment, and he was going to examine why that was so.
The long-term impact of psychiatric drugs was about to come under review.
Or so it seemed.
Insel’s Hypothesis
Healing is a book aimed at the general public, with the publisher presenting it as a roadmap for change. And while Insel had stated in 2015 that Anatomy of an Epidemic needed to be taken “very seriously,” he took a very different tack in Healing. After setting forth the conundrum—how is that outcomes are worsening when so many more people are being treated?—he quickly dismissed any worry that psychiatric drugs could be a causative factor for those poor outcomes. He did so in three paragraphs:
Some critics, such as science journalist Robert Whitaker, have blamed the mental health crisis on the treatments. Noting the temporal correlation of increased disability with increased medication use, Whitaker argues that antidepressants and antipsychotics create a “supersensitivity” that makes patients dependent and chronically disabled. With claims that long-term outcomes were better before the “psychopharmacology revolution,” he writes that the psychiatric establishment, in collaboration with the pharmaceutical industry, has conspired to overmedicate and overtreat children and adults with disastrous results.
Not everyone buys this conspiracy theory. Others see the problem as ineffective treatment. They claim current treatments are necessary, but they are not sufficient to cure complex brain disorders. In a call to arms entitled “Revolution Stalled,” Steven Hyman, my predecessor as NIMH director, notes that we need to know much more about the biology of mental illness before we “can illuminate a path across very difficult scientific terrain.” Dr Hyman’s point is that we don’t know enough about the mechanisms or causes of mental illness to develop medications that are as effective as insulin or antibiotics.
There is a third perspective that I think explains the more-care-but-worse-outcomes conundrum. I suspect that clinicians are helping the people they see, that they are seeing more people than ever, and that they are probably more effective today than twenty-five years ago. Why aren’t they bending the curve? The majority of people with mental illness are not in treatment, those in treatment receive little more than medications (which, as Dr. Hyman says, are not adequate), and many of the people receiving medications do not take them . . . so the crisis of care is not just lack of access (to treatment), but lack of engagement [with treatment.]
Those three paragraphs provide the framework for the narrative that is to follow. The idea that psychiatric drugs might worsen long-term outcomes has been dismissed as a conspiracy theory. At the same time, by quoting Hyman, Insel is presenting himself as open-minded about the merits of psychiatric drugs by stating that they are not curative—he is telling readers he will be a sober reviewer of the evidence. Yet, in that same paragraph, he assures readers that such medications are necessary, and in the third paragraph, he ups the ante: clinicians are helping their patients and individual outcomes may be better than 25 years ago. The blame for the poor outcomes, it seems, falls on society for not investing in necessary social supports and on patients who fail to take their drugs and stay engaged in treatment.
There is nothing in that narrative that could be expected to harm psychiatry’s guild interests or pharmaceutical interests. Insel then describes himself as taking on the role of a journalist as he explores humanistic supports that are needed as a complement to drugs and other psychiatric therapies in order to promote lasting recovery.
This is a win-win position to take. Anyone with a heart and common sense is going to welcome societal efforts that provide those struggling with psychiatric difficulties with social support, meaning in life, and a safe place to live. Indeed, critics of psychiatry have been advocating for such efforts for decades, and Insel was now positioning himself as the advocate for this societal response.
In short, his inquiry into the “puzzle”—why have societal mental health outcomes worsened even as more people got treated for psychiatric disorders?—was over before it ever began. His roadmap to “mental health” would not be upsetting to psychiatry’s guild interests; the pharmaceutical companies would have no reason to complain; and nearly all readers could agree that it would be helpful if our society could build a system of care that provided the “mentally ill” with decent housing, a social community, and purpose in life.
And with that framework in place, there would be no place in his 300-page book for research that told of drug treatments that, in the aggregate, worsen long-term outcomes.
The Drug Information Fit To Print
The third chapter in Insel’s book is titled “Treatments Work.” He opens the chapter in this way:
The current state of mental health care is sobering, yes. But there is good news, and it is not just that we can take lessons from the incomplete successes of the past. Perhaps even more important, we also have treatments that work right now. In contrast to so many complex, chronic health problems, here we have solutions. Yes, we have more to learn, and future treatments will likely be even better than what we have today. But crucial to ending America’s crisis of care is understanding that right now we have treatments that can improve outcomes, treatments that help people recover. We can solve so much of the care crisis, because solving the care crisis requires nothing more than a wider application of the best care we can offer.
Psychiatric drugs, ECT, transcranial magnetic stimulation, psychotherapy—all of these current treatments “work.” Antidepressants have an “overall effect size” that is as high and often higher than medications used in other areas of medicine, Insel writes. So too the top-selling antipsychotic, Abilify. Stimulants, benzodiazepines, they all “work.” And in those instances where psychiatric drugs only help people get “better but not well,” then “other forms of treatment, psychological, neurotechnological, or rehabilitative interventions can pave the path to recovery.”
Such was Insel’s inquiry into the merits of psychiatric treatments. His description of the short-term merits of psychiatric drugs could be easily critiqued, but that is not the point of this essay. What is notable is that he didn’t cite a single study that told of psychiatric drugs providing a long-term benefit.
Insel, of course, knows the research literature well. The glaring omission leads to a simple conclusion: the former director of the NIMH, in a chapter titled “Treatment Works,” was unable to find a single study to cite that told of the drugs improving long-term outcomes. And this was after the drugs had been on the market for 65 years.
The Research That Insel Dared Not Mention
There is not enough space in this essay to lay out the full collection of evidence, composed of many different elements, that lead to a conclusion that psychiatric drugs, in the aggregate, worsen long-term outcomes. That took a book-length inquiry. However, it is possible to summarize the highlights of such research findings for antipsychotics and antidepressants, which are the two classes of psychiatric medications that have been most extensively researched. A similar summary of research for stimulants is also provided below.
To a significant extent, this review provides a brief history of NIMH research into the long-term effects of psychiatric medications. Whereas pharmaceutical companies fund the studies that tell of their short-term efficacy, it has been the NIMH, dating back to the 1970s, that funded studies on their long-term effects.
Antipsychotics
After antipsychotics were introduced in the mid 1950s, clinicians began speaking about the “revolving door syndrome” that now appeared in asylum medicine. First-episode patients would be discharged and then return in droves, which led the NIMH, during the 1970s, to fund four studies to assess whether antipsychotics were increasing the chronicity of psychotic disorders.
Here were the results:
Bockoven reported that the rehospitalization rate for discharged patients was higher for patients treated after the arrival of antipsychotics in asylum medicine, and that the medicated patients were also more “socially dependent” than those treated before 1955. Carpenter, Mosher, and Rappaport reported superior outcomes for unmedicated patients at the end of one, two, and three years respectively, which led Carpenter, who had conducted his study at NIMH’s clinical research facility in Bethesda, Maryland, to write that “we raise the possibility that antipsychotic medication may make some schizophrenic patients more vulnerable to future relapse than would be the case in the natural course of the illness.”
By this time, researchers were fleshing out the “adaptive” brain changes stirred by antipsychotics. The drugs block dopamine receptors in the brain, and the brain responds by increasing the density of its dopamine receptors. Two Canadian researchers, after studying their medicated patients, concluded that this drug-induced dopamine supersensitivity “leads to both dyskinetic and psychotic symptoms. An implication is that the tendency toward psychotic relapse in a patient who has developed such a supersensitivity is determined by more than just the normal course of the illness.”
This understanding of how the brain “adapted” to antipsychotic medication provided a biological explanation for why the drug treatment increased the chronicity of psychotic disorders, and thus provided a causal explanation for the research findings reported by Bockoven, Carpenter, Mosher and Rappaport.
More such findings followed.
The World Health Organization, in two studies that compared longer-term outcomes in three “developing countries”—India, Nigeria, and Colombia—with outcomes in the United States and five other developed countries, found that outcomes were much better in the three developing countries, where only 16% of schizophrenia patients were regularly maintained on antipsychotics.
Next, Nancy Andreasen, the long-time editor-in-chief of the American Journal of Psychiatry, in a large MRI study of schizophrenia patients, reported that antipsychotics shrink brain volumes over time, and that this shrinkage is associated with a worsening of negative symptoms, increased functional impairment, and, after five years, cognitive decline.
A Canadian researcher, Philip Seeman, who in the 1970s had helped flesh out how the brain responded to antipsychotics by increasing the density of its dopamine receptors, reported that this adaptive response was why antipsychotics “fail over time.”
Then came the findings reported by Martin Harrow and Thomas Jobe. In the late 1970s, with funding from the NIMH, they had launched a long-term study of 200 patients diagnosed with schizophrenia or other psychotic disorders, most of whom were experiencing a first or second episode of psychosis. All were treated conventionally in the hospital with antipsychotics, and after they were discharged, Harrow and Jobe periodically assessed how they were doing and whether they were using antipsychotics. They found that the outcomes of those who got off the medications by year two began to dramatically diverge from those who stayed on the drugs, and that at the end of 15 years the recovery rate for the off-med patients was eight times higher than for the medication-compliant patients (40% versus 5%). “I conclude that patients with schizophrenia not on antipsychotic medication for a long period of time have significantly better global functioning than those on antipsychotics,” Harrow announced at the 2008 meeting of the American Psychiatric Association.
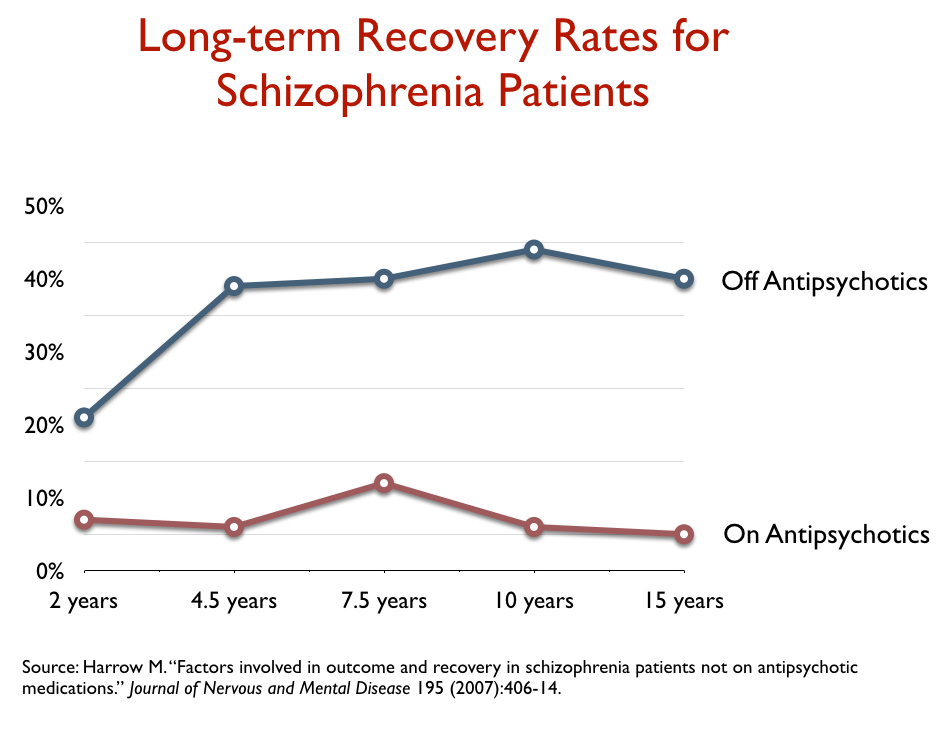
Harrow and Jobe also reported that the medication compliant patients were much more likely to remain psychotic over the long term than those who got off the medication, and it was the off-medication patients who had dropped out of treatment that had the better outcomes. Harrow and Jobe referred to drug-induced dopamine supersensitivity as a likely reason for this difference in outcomes.
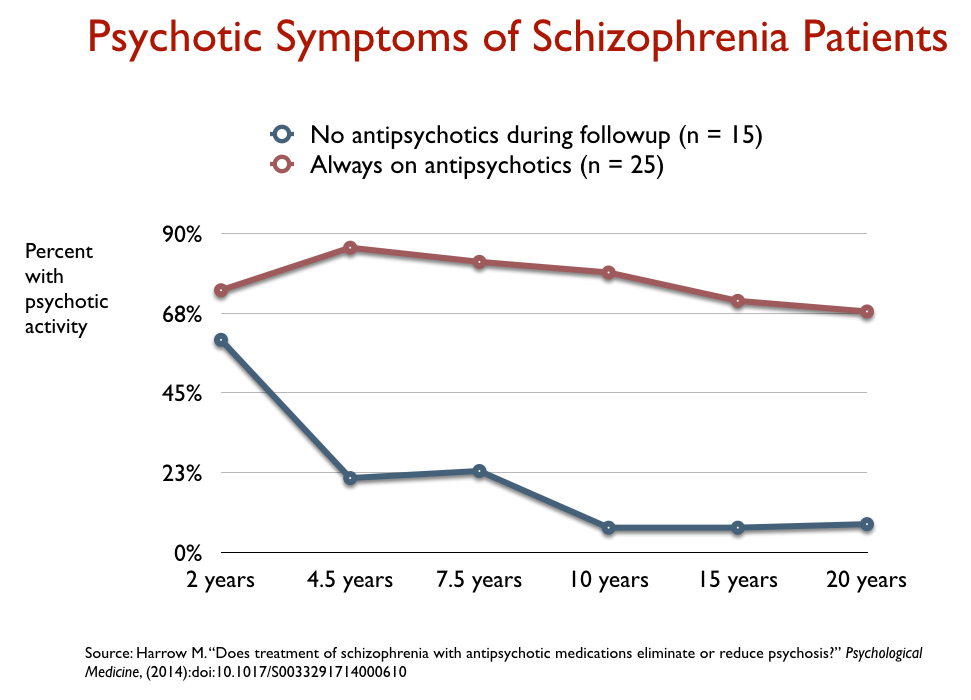
In the past two decades, longer term studies of psychotic patients conducted in the Netherlands, Finland, Australia, Denmark, and Germany all told of higher recovery rates for those off antipsychotic medication. Similarly, users of antipsychotics tell of how these drugs “compromise functional recovery” over the long-term.
Antidepressants
The antidepressant history is much the same. Prior to the introduction of this class of drugs, major depression—and this finding came from studies of hospitalized patients—was understood to be an episodic disorder. Patients could be expected to recover, and perhaps half of patients who suffered a first episode would never be rehospitalized for depression.
However, after the introduction of antidepressants, at least a few clinicians observed that the use of these drugs appeared to be causing a “chronification” of the disorder. In the 1970s, a Dutch researcher, after studying the case histories of 94 depressed patients, some who took antidepressants and some who did not, concluded that “systematic long-term antidepressant medication, with or without ECT, exerts a paradoxical effect on the recurrent nature of vital depression. In other words, this therapeutic approach was associated with an increase in cycle duration.”
In the 1980s, a number of studies found that relapse rates were high for depressed patients treated with antidepressants, so much so that a panel of experts convened by the NIMH concluded that, in contrast to older studies of mood disorders, “new epidemiological studies [have] demonstrated the recurrent and chronic nature of these illnesses.”
Two NIMH studies in “real-world” patients, who were treated in outpatient settings, subsequently confirmed that this was indeed the long-term course for medicated patients. In 2004, Rush and colleagues treated 118 outpatients with a wealth of emotional and clinical support “specifically designed to maximize clinical outcomes,” and only 13% got well and remained well for any length of time. Next, in the NIMH’s STAR*D trial, which was heralded as the largest antidepressant trial ever conducted, only 108 of the 4,041 who entered the trial remitted and stayed well until the end of the one-year follow-up. That’s a 3% recovery rate; the other 97% either failed to remit, or relapsed, or dropped out before the end of one year.
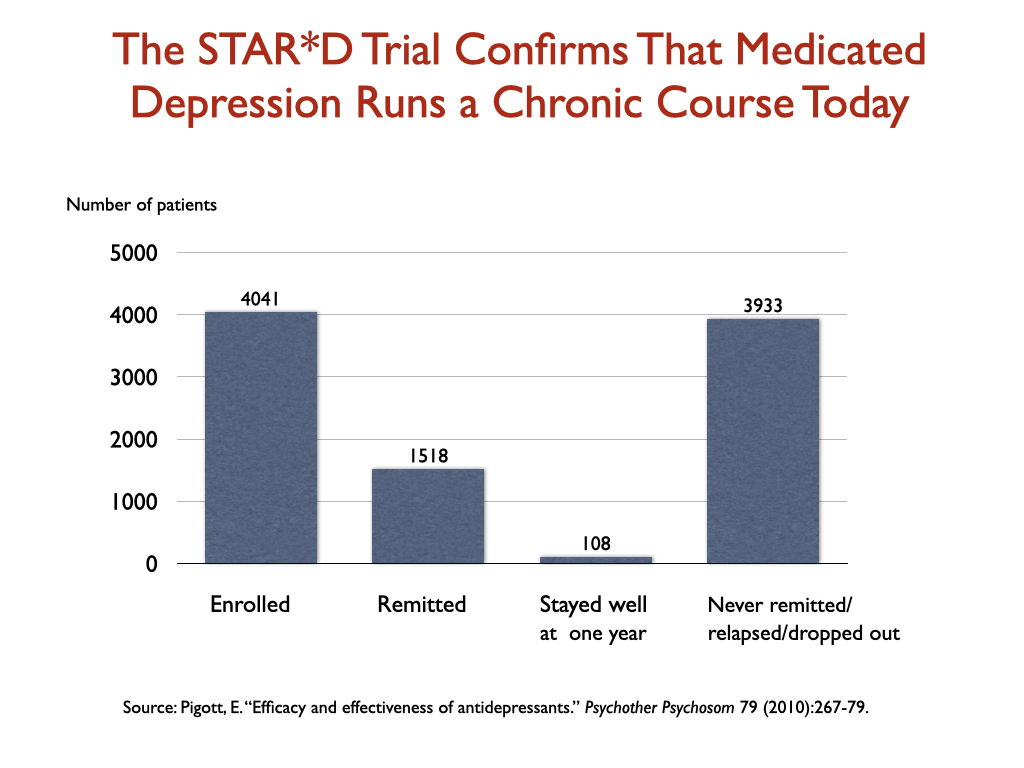
This 3% stay-well rate stood in sharp contrast to the outcome in an NIMH funded trial that sought to identify the longer-term course of untreated depression in modern times. In that study, 85% recovered by the end of one year. “If as many as 85% of depressed individuals who go without somatic treatment spontaneously recover within one year, it would be extremely difficult for any intervention to demonstrate a superior result to this,” the researchers concluded.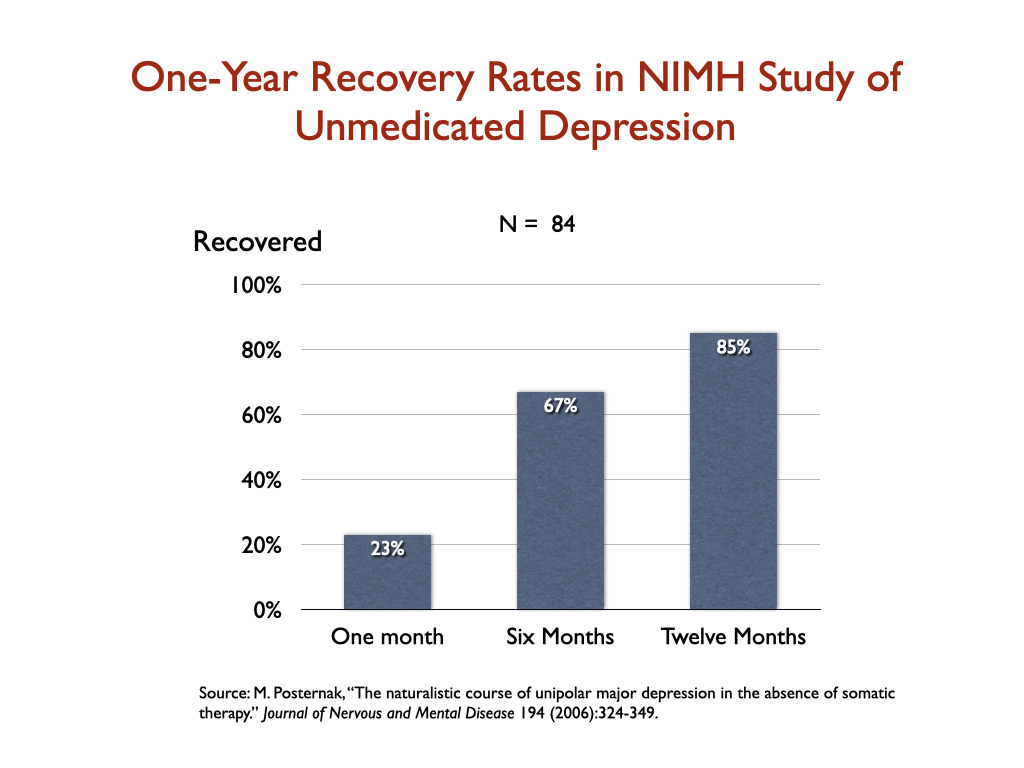
Numerous studies over the past 35 years have compared outcomes for medicated and unmedicated patients over longer periods of time. Here is a quick rundown of these findings:
- In a NIMH study conducted during the 1980s that compared the antidepressant imipramine to two forms of psychotherapy and to placebo, at the end of 18 months the stay-well rate was highest for the cognitive therapy group (30%) and lowest for the imipramine exposed group (19%).
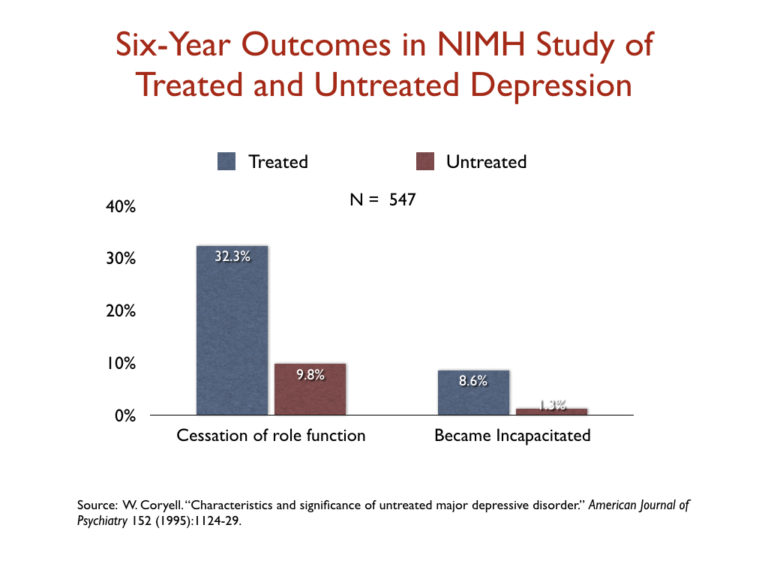
- In a NIMH study that compared six-year outcomes for depressed people who got treated for the disorder and those who eschewed medical treatment, those who were “treated” were three times more likely than the untreated group to suffer a “cessation” of their “principal social role” and nearly seven times more likely to become “incapacitated.”
- A World Health Organization study of depressed patients in 15 cities found that at the end of one year those treated with a psychotropic medication had worse “general health” and were more likely to still be “mentally ill” than those who weren’t exposed to such drugs.
- A Canadian study of 1,281 people who went on short-term disability due to a depressive episode determined that 19% of those who took an antidepressant went on to long-term disability compared to 9% of those who never took such medication.
- In a five-year study of 9,508 depressed patients in Canada, medicated patients were depressed on average 19 weeks a year, versus 11 weeks for those not taking the drugs.
- Two reviews of the long-term outcomes of patients diagnosed with depression found that exposure to an antidepressant was associated with worse outcomes at nine years (U.S. study) and at 30 years (Swiss study).
As these findings have piled up, researchers—led by Italian psychiatrist Giovanni Fava—have pointed to drug changes induced by SSRI antidepressants as a likely explanation for the “bleak long-term outcome of depression.” These drugs may “worsen the progression of the disease in the long term, by increasing the biochemical vulnerability to depression. . . use of antidepressant drugs may propel the illness to a more malignant and treatment unresponsive course,” Fava wrote.
In a 2011 paper, American psychiatrist Rif El-Mallakh observed that 40% percent of depressed patients initially treated with an antidepressant were now ending up in a chronically depressed “treatment resistant” state. “Continued drug treatment may induce processes that are the opposite of what the medication originally produced,” he wrote. This may “cause a worsening of the illness, continue for a period of time after discontinuation of the medication, and may not be reversible.”
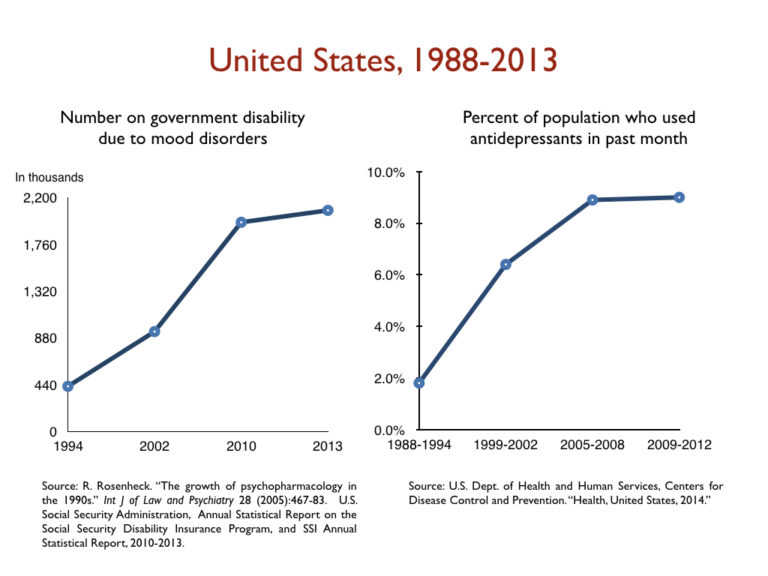
Given this literature, it is no surprise that major depression is now the leading cause of disability in the U.S. for people ages 15 to 44, and that in country after country that has adopted widespread use of SSRIs, the number of people on government disability due to a mood disorder has increased in lockstep with the increased use of those drugs.
Stimulants in Children and Adolescents
In the early 1990s, the NIMH mounted what it called the Multisite Multimodal Treatment Study of children with ADHD (MTA) to assess the longer-term impact of stimulants. At the end of 14 months, youths treated with stimulants by ADHD experts had a greater reduction of ADHD symptoms than those randomized to behavioral therapy (there was no placebo group), which was seen as evidence that stimulants provided a long-term benefit to youth so diagnosed.
However, that was not the end of the study. The NIMH researchers continued to follow the youth, who during this follow-up were free to go on or off stimulant medication if they so chose. At the end of three years, being on a stimulant “was a significant marker not of beneficial outcome, but of deterioration. That is, participants using medication in the 24-to-36 month period actually showed increased symptomatology during that interval relative to those not taking medication.” The medicated youth also had higher delinquency scores at the end of three years, and were shorter and weighed less than their off-med counterparts.
At the end of six to eight years, the results were much the same. Medication use was “associated with worse hyperactivity-impulsivity and oppositional defiant disorder symptoms,” and with great “overall functional impairment.” The medicated youth were also more likely to have been diagnosed with depression or anxiety.
As one of the NIMH investigators later confessed, “We had thought children medicated longer would have better outcomes. That didn’t happen to be the case. There were no beneficial effects, none.”
Longer term ADHD studies in Australia and Quebec have also found worse outcomes for medicated youth than for those treated without stimulants.
A Compact Broken
As can be seen, a review of the research literature tells of how antipsychotics and antidepressants increase the chronicity of the disorders they are used to treat, and it tells too of how at least a few researchers, seeking to explain the poor outcomes, fleshed out a biological explanation for why that would be so. Stimulants as a treatment for ADHD failed the long-term test too. The same is true of benzodiazepines; outcomes for bipolar disorder have similarly worsened in the modern era.
A longer list of studies that tell of these outcomes can be found on MIA resource pages for antipsychotics, antidepressants, benzodiazepines, polypharmacy for bipolar disorder, and stimulants for juvenile ADHD. There are more than 100 journal articles that populate those lists.
But none of this history is found in Insel’s book. This history is also missing from psychiatric textbooks and the NIMH’s website. Search for Martin Harrow on the NIMH website and nothing turns up. Search for STAR*D and you’ll find a press release on short-term results that tells of “particularly good results” with antidepressants that “highlight the effectiveness of high-quality care.” What you will not find on the website is that the documented one-year stay-well rate for patients treated with antidepressants was a dismal 3%. (That information was, in fact, hidden in the journal article that reported one-year outcomes.) Nor does the NIMH website inform parents that in the MTA study, medication use was a marker of “deterioration” by the end of year three, and that at the end of six years those taking stimulants had worse ADHD symptoms and were more functionally impaired.
This is the real source of the poor mental health outcomes in the United States: the psychiatric establishment, which includes the NIMH, is not an honest broker of information related to the merits of psychiatric drugs. Indeed, ever since the American Psychiatric Association adopted a disease model for categorizing psychiatric disorders when it published DSM-III, it has told a story to the public that promotes that model and the prescribing of psychiatric drugs, regardless of whether the elements of that story were grounded in good science. We were told that major psychiatric disorders were caused by chemical imbalances in the brain and that antipsychotics and antidepressants fixed those imbalances, like insulin for diabetes. We were told that the major disorders in the DSM had been validated as discrete diseases, and that those who doubted that were like members of a Flat Earth Society. When the SSRIs and the atypical antipsychotics came to market, we were told they were “breakthrough medications.”
None of this was true, and yet our society organized itself around that false narrative, and the prescribing of psychiatric drugs soared and to all ages, from the young to the elderly. And as that took place, the burden of mental illness in our society dramatically increased.
Today, most elements of that story, at least within psychiatric research circles, have been abandoned. The chemical imbalance story is now derided as a hypothesis that fell out of favor decades ago, with Ronald Pies, former editor in chief of Psychiatric Times, describing it as an “urban legend—never a theory seriously propounded by well-informed psychiatrists.” Allan Frances, who chaired the DSM-IV task force, and other prominent figures in the field, including Insel and his predecessor at the NIMH, Steven Hyman, acknowledge that the disorders in the manual have never been validated as discrete illnesses, and that the diagnostic categories are properly understood to be constructs. In Healing, Insel admits that the second-generation psychiatric drugs are really no better than the first, the notion that they were “breakthrough medications” having been put to rest some time ago.
The narrative that our society organized itself around, starting in the late 1980s, has collapsed. Yet, the prescribing of psychiatric drugs rolls on, with psychiatry touting results from short-term studies of the drugs as evidence of their efficacy, and it is the hiding of the results from long-term studies that now sustains this enterprise. If the scientific narrative that is to be found in the research literature were told to the public, of drugs that don’t fix chemical imbalances but rather induce them, and that researchers have pointed to that drug effect as a likely reason that that the medications increase the risk that a person will become chronically ill and functionally impaired over the long-term, then psychiatry would have to completely reorganize its care.
This is the bridge that psychiatry, as a guild, cannot cross. The prescribing of drugs is psychiatry’s primary therapeutic act, and if its drugs cause long-term harm, then what would the profession do? The profession needs to keep this history out of sight, even to itself, and so it is not presented in psychiatric textbooks, or in continuing medical education seminars. By keeping this history hidden, the field is not just breaking its compact with the public, but with itself—with every prescriber and all those who enter the field.
However, one could have hoped that Insel, writing as the former director of the NIMH, would have dared to cross this bridge of no return. He had the opportunity to turn the profession in a new direction, and while doing so, chart a true roadmap to better “mental health” in our country. His was a bully pulpit, and the NIMH is not subject to the same guild impulses as the American Psychiatric Association.
The NIMH is funded by the public. We funded the Harrow and Jobe study of long-term outcomes for schizophrenia patients; we funded the STAR*D trial; and we funded the MTA study of stimulants. As the funders, we deserve being told the long-term results from those studies, and to have the results widely publicized.
That is what the NIMH—and Thomas Insel—owed to us.
Searching for a Solution
In 2015, Lisa Cosgrove and I published Psychiatry Under the Influence, a book that arose from our time as fellows at the Safra Center for Ethics at Harvard University, in a lab devoted to studying “institutional corruption.” In a democratic society, the expectation is that institutions that serve a public interest—and this is particularly true for medical disciplines—will adhere to ethical standards. We wrote:
Our society thinks of medicine as a noble pursuit, and thus it expects a medical profession to rise above financial influences that might lead it astray. The public expects that medical researchers will be objective in their design of studies and their analysis of the data; that the results will be reported in an accurate and balanced way; and that the medical profession will put the interests of patients first.
In a 2009 essay, Daniel Wikler, a professor of ethics at the Harvard School of Public Health, told of how a medical discipline that fails to adhere to this standard doesn’t deserve to retain its privileged place in society. He wrote:
Erosion of medical integrity is not a mere detail, but rather strikes at the heart of what it is to practice medicine. The basis for medicine’s claim to be a profession rather than a trade, exchanging a degree of self-governance and autonomy to be trusted experts, is the assurance that the trust will not be misplaced.
The erosion of medical integrity is, in this instance, complete. The past is prelude to the future, and psychiatry is not going to alter its behavior in this regard. It is not going to tell the public of research findings that would undermine public confidence in psychiatric drugs. Nor will the NIMH.
This is why Insel’s book makes a case for abolishing psychiatry, or perhaps more aptly stated, for removing psychiatry from its position of authority over this domain of our lives. Our society needs to put its trust and authority into those who will tell of this research, and that means putting its trust and authority into an organization or agency that isn’t moored to psychiatric drugs.
That is the roadmap for moving from “mental illness to mental health” that Insel’s book leaves us with. We need to have leadership that we can trust to tell us the truth about the merits of psychiatric drugs.
***
MIA Reports are supported, in part, by a grant from the Open Society Foundations.
Photo credit: Creative Commons, World Economic Forum





Thank You Bob,
You are right in everything you say about the disadvantages of drug dependent psychiatric treatment.
A person might nearly think that the idea behind Psychiatry was to control and thrash people. We are more or less heading in the Western World for about 30% of the population being somewhat Psychiatric. It can also be clearly seen in society, that all the wealth is going in one direction.
Recovering people through effective Peer Groups needn’t cost anything. I’ve seen lots of people completely recover very quickly in Peer Groups (and remain well).
Do you think this man here is making his story up?
https://youtu.be/YT2ecA6bJ1c
Report comment
Bob, as usual, thorough and acute analysis and was exactly on target. As you know my colleagues David Cohn and Stuart Kirk and I published Mad Science: Psychiatric Coercion, Diagnosis, and Drugs in 2013 regarding most of these issues and the impact of the additional horror of the coercive elements of such “treatments.” The maleficence of both institutional psychiatry and its bureaucratic power will continue as long as the state continues to support its medicalized perspective and supports its unprecedented role as the certified police of deviance of noncriminal although disruptive or disturbing behavior. This is especially so today as central control is more and more supported by the authoritarian elements of our political scene and “mental health” becomes more and more a panchreston of all human travail.
Report comment
I said a comment, comment 103 or comment 110, my comments keep slipping down the landslide of banter, so maybe you need to click on my Diaphanous Weeping name to find that comment faster, but anyway, I am ill with schizophenia as I say. I honour the ideas of this website that are against pushing medications on people. I am also against inacurate diagnosis or misdiagnosis or misdescription being giving to people who do not want that. I am against experts calling people liars when those people say they are not ill. I am against imposing control on peoples choices.
None of this means nobody can air “an opinion”.
If a father drowns his three children because he thinks they were conceived by the devil, I would prefer a gentle psychiatrist to air an opinon that that dad should not collect his fourth child from kindergarten.
I respect what this website stands for. It wants to educate the public or society about faulty education.
But I am NOT the public.
I am me.
And I have a basic human right to say I feel ill. And I have a basic human right to call that illness whatever I choose to. This year it is schizophrenia but next year it might be fizzy atom illness or red poppy disease. It is MY choice to say when I feel ill and since I am NOT THE SOCIETY it is NOT THE SOCIETY’s choice.
I repeat the above for anyone who wants to uphold their basic human right to say they do not have schizophrenia and are not ill.
The “belief” in schizophrenia is like the “belief” in the desert whirlwind that can drive people mad in some cultures. Nobody goes after those people and educates them out of the folly of a belief that brings them comfort. Nobody tells individuals with those views that they are “wrong” now since SOCIETY has decided that the whirlwind is a myth.
What is being trampled on in this era that has EVERYONE FIGHTING EVERYONE over what is BEST for THE world is the aggressive destruction of everyone’s basic human right to have their OWN freedom of choice, to regard themselves and their illness or absence of illness in their own way. Not THE PUBLIC’s way. What does anyone mean by THE PUBLIC?
A person has insomnia over how to SAVE THE WORLD. So they start informing THE SOCIETY of what THEY need to KNOW. What is this push push push to tell strangers what they need to know? The push links to anger and the fight.
But if a person is fighting are they able to listen to multifarious individuals from entirely different tribes who have their own consolling myths?
A person may have utopian vision of how THE WORLD SHOULD BE. Well what if you do not like that utopian vision? What if it looks like it will not respect your freedom to be just you? Is the person going to shun you? If they are is that shunning world one you want to belong to?
Everyone on the internet are fighting, fighting, fighting.
Even dear weary Robert probably feels irked.
It is all going according to plan. By this I mean that humans will only realise the fruitlessness of endless arguements, all pushing to influence individuals freedom of choice, when they mistake THE WORLD for a utopian vision and not see that each individial IS THE WORLD.
Anger ORGANIZES.
Love DISORGANIZES.
Love is the great liberator because it does not try to organize an individual out of their freedom of choice.
Nature is disorganized.
Humans have lost the ability to accept being disorganized. And now humans are fighting, fighting, fighting, in trying to organize THE WORLD that is each other human being.
It is not trauma that breaks you. It is your dreams. The sheer unfairness of them. The unfair difficulty inherent in all dreams to be easily arrived at.
A billion people are going to war over the unfairness of their dreams.
But war is a nightmare that ensures no dreams can even be wept about.
There are no beds left unsplintered to dream them in.
What ceases a war is not the accomplishment of change. It is the successful realization that no accomplishment is worth ruining THE WORLD for.
THE WORLD that is you.
THE WORLD that is me.
ONLY LOVE CAN SET US FREE.
Love is harder to be than war is to do.
Report comment
Hello Robert,
Once Upon A Time, Long Ago, in the beyond, two spirits looked down upon planet Earth and see that everyone is bickering. No one is allowing anyone their “freedom of choice”, their choice to be themselves. Bullying has run amok in all areas of every civilization. So the two spirits hatch a plan. They decide to help bring peace back. The first spirit, let’s call him James, suggests to the second spirit, lets call him Alan, that an enlightened or rather messianic spiritual leader might be good happening on Earth. But Alan says many such figures have been sent already. The bickering has grown worse. So then both James and Alan come up with another idea for making peace everlasting…
War.
It is organized that James will incarnate into human form as a world leader of fine integrity, a matchless hero in a country oppressed by another competing corrupt world leader, Alan.
The two spirits hug each other since they love each other but know they are going to endure the difficult task of incarnating AS rivals. They know their life plan involves the theatre of bringing about war. This is because people who initially “pick a side” in the war are initially motivated by a “logical” sense of being irrefutably “correct”. This may be connected to “rules” such as coastal rules, or maritime rules, or energy pipeline rules, or religious territory rules, or economic rules, any rules. Often it is not the big rules that motivate any army. Often there is just a vague sense of “the others” and they get demonized as “wrong”. That may be all that is required to set two countries at war with each other.
So initially those who “pick a side” can easily find a plethora of “logical reasons” exactly WHY the “others” should be stripped of their “freedom of choice”. The “wrongdoers” get villified as if “they” cause some obstacle to “freedom of choice” and the “feelings” that feed those choices.
The “consensus opinion” of the “others” in one country gets blamed for dismissing the “freedom to be” in another country. But often this “othering” and blaming on both sides is a consequece of the way ANY “consensus opinon”, or group think, in ANY part of the globe can oppress its OWN. What is meant here is that “consensus regulations” make people ILL if their heart and soul and “feelings” are not inspired by such fussy regulations. And since regulations involve “rationalizing” and not “feelings”, people become “feeling deprived” when they nod like puppets on strings for their “consensus opinion” leaders.
The seething ILL resentment at “having to” comply with the ENTITLED demands of “group think” combined with becoming “feelings starved” causes people to become themselves bullies and footsoldiers. As if in a regime they cannot express their real “feelings” in.
But to leave the “group think” would mark them out as a kind of “other” every bit as suspect as the initial “others” who have been designated the title of “them”. The glue that binds “consensus opinion” often thrives on designated another group as “them”, even to the extent that the “them” must constantly have their demon “them” credentials poked and revealed. Every human group does this binding or bonding. It is not bad in itself. Birds of a feather flock together. But when a bird is NOT FREE to BE who it chooses to be it is no longer satisfying to be part of the flock. Yet to leave the group marks it out as a deviant or inexplicable or dreamy or “mad”. It becomes “other”. It may be cautioned against being a “unique individual” since that threatens the “consensus opinion”, like a sinner threatens an established church. Gradually more and more birds in the flock fear leaving and fear speaking as a unique individual. The puppets on strings thing happens more and more. But as this decending into gross bullying by the “consensus opinion” gets worse the pent up anger and ILL sensation at not being “free” to “feel”, without such “feelings” being slammed as being “wrong”, the inner resentment spills outward to the initial “others” in the country that held a separate “consensus opinion”. Ramping up the heckling of those “them” is far easier.
But what is often being heckled is not so much “their” differentness, but living a life of soul destroying “logic” at the expense of being free to “feel”.
What occurs then in a war is two different countries with legitimate grievances but ALSO with enormous displaced rage at “having to” be oppressed by “logic” in general throughout life. A romantic notion of an “improved” way of life beckons. That notion has vague visions of everyone understanding something “logical” and coming together in a new “consensus agreement” about it. So this architects a new paradigm, for a mass salvation, a mass healing.
But the word “mass” should be a clue.
You cannot be “free” to be utterly YOU if you are an insignificant add on bit of a mass. Not even in a mass suicide.
All individuals become well when they have their own “freedom of choice” to want what they want. It is as simple as that. If they do not get this they rapidly become ILL.
Wars are not made by the happy.
Wars are atrocious and grotesque. But what eventually springs out of war is the exhausted obliviousness about anyone’s damn “consensus opinion”. Instead there is a return to realizing that wellness is connected to having the individual “freedom of choice” for almost laughably simple things, such as your OWN comfy bed, your OWN bicycle, your OWN books, your OWN grandparents, your OWN bowl of rice, your OWN preferred kind of herbal medicine, your OWN idea of healing, not everyone else’s “consensus” idea.
The simple “free choices” that make YOU feel better may not make ANYONE else feel better.
Your “choice” as born aloft on the altitude of your “feelings” CANNOT BE WRONG.
This is because “feelings” cannot be wrong or right. The designation of wrong or right are cerebral judgements from bickering rules and arguments.
Feelings, like breathing, and sleeping, just ARE.
If your outward behaviour is not hurting anyone directly and intentionally then YOUR CHOICE to feel how you feel, believe what you believe, decide what you decide, be who you be, is totally innocuous and harmless. Therefore YOU being FREE to feel your OWN feelings and think your OWN thoughts is not a traitor to anything or anyone. And because freedom makes you well, and wellness is healing for all who come into contact with it, in this regard “consensus opinion” can be the demise of wellbeing.
To LOVE can only happen when we are well with our feelings.
Since peace is the essence of love then “freedom of choice” is needed for WORLD PEACE. But weirdly why so many people fight in wars is they are convinced that “their” brand of “consensus opinion” has to be THE ONLY way of finding peace.
When people say wellbeing can only be found by YOU giving up your OWN “feelings” run a mile.
What of James and Alan? They visited Earth and caused a war to help people HATE WAR and HATE HATING and instead value the love lost and value the “freedom” to each individual sleep in their own bed and warm themselves at their own hearth.
When you read of warring leaders in history who argue and sabre rattle perhaps wonder if unbeknownst to their conscious recollection their spirit essences have each already shaken hands in a deal that is not of war but of peace.
To every agonist comes an antagonist. A theatre piece double act. Perhaps an “R” and a “DW”.
Report comment
Damn. That’s a HALL OF FAME-level comment!….makes me GRIN MADLY! LOL!
Report comment
I am not intrested what false medical empiricsm or whatever medical empiricism has to say about psyche. This is evil uzurpation of identity. Everyone who write articles about drugs vs psyche are potential legal murderers. Why this site write about drugs all the time? Because people are paid to do so, because there is a pyramid of corruption, and we are on the bottom. And victims of psychiatry are useless eaters, or always were, to empire of ego cult. To Klaus Schwab – everyone are useless eaters. You, who write about drugs, to people who were almost killed by this poison, you are insane and you should remember about what Schwab promised. I know that this site is some kind of a tube for secret services, not listening to people, at all. Something like – “Och look, we didn’t kill them yet. Let’s find some better drugs”. People are not stupid, you know.
Report comment
“…Everyone are useless eaters..”
It can be seen Right Now how Europe is losing ground – with inflation, recession and impending poverty – yet the World has never been Richer.
Report comment
https://youtu.be/fd5qf4pG-xg
It is not necessary to have “consensus opinion” to back up your own individual “freedom of choice”. In some regards “consensus opinion” is a club for those who cannot brave following the leader that is their honest and true and authentic “feelings”.
A “consensus club” shuns “feelings” in favour of “logic” and uses “logic” as a mode of guilt tripping anyone who has an emotion.
So along comes another group to take down that imposing “consensus opinon”…say psychiatry…but it does so by forming yet another “consensus opinion” club, and it uses the “language” of “logic”….say scientific logic…to kick the achiles heel of imperious “logic”. But this is like an Amazonian tribesman asking the conquistadors to go away by using the “language” that is Spanish. By using the “language” that is not particularly “feeling” to chastise an interloper that is all “logical” what is going on is THE PRESERVATION of the “language” of “logic”, and why this is foolish is because that “language” is the one used to bind a people in a “logical consensus opinion”. A situation of bondage to some authority that supercedes YOUR OWN “freedom of choice”.
In this way antipsychiatry can, from time to time, emulate psychiatry.
If you come accross a “consensus opinion” you do not like or agree with, just “move on”.
No need to grind “the others” group think into dust under the boot heel of yet more hard factual “logic”.
In the medieval era many “thinkers” of “logic” loathed the “feeling” who could not be turned into puppets on strings. Such “thinkers” did not just spar with or mock the “feeling”, they left no trace of them. That’s “thinkers” for you. To have compassion needs access to “feelings”.
I say all this because THIS is the bigger fight of our age, not the details we all get vortexed away on.
You can get rid of the DSM “choice” and the diagnosis “choice” because YOU think it is a rotten choice for everyone else, but in that way this is promoting a “consensus opinion” that not everyone is going to feel well about.
I have NEVER been enamoured with antipsychotics. I think we know too little about the brain to interfere with it. MY CHOICE would be bin all pills. But I KNOW that only other actual diagnosed schizophrenics have ANY understanding of how tormenting living with schizophrenia is. There seems a willful drive at a “consensus opinion” that my feeling ill is my MISINTERPRETATION of my inmost being….as if by antipsychiatry borrowing the “logic” of “consensus opinion” to refute the “consensus opinion” of “logical science” both psychiatry AND antipsychiatry actually KNOWS more about ME than I KNOW ME.
It is THIS “expertise” pontificating that needs to stop.
Instead, all people ought to let adults make up their OWN mind about what is the matter with them and what will best heal them.
I see this as like how many tribes can peacefully coexist in one forest.
You mentioned the refuting of chemical imbalances but I would say that probably someone in menopause “feels” a chemical/hormonal imbalance. They go on HRT and feel a different sort of chemical imbalance, they withdraw from HRT and feel yet more chemical imbalance. It is ALL the experience of chemical imbalance. The original one was a brain thing. I just believe it is petty to do this…prove it prove it prove it prove it. It is so “consensus opinion”.
I am not for medication but I am for people having the “free choice” to see psychiatry as their healer. I am yet to meet a bad doctor or bad psychiatrist or bad psychologist. I have only ever met stressed out imperfect human beings buckling under the strain of working in horrible offices.
I am fine to discover new “consensus opinions” but it does not require bulldozering someone else’s “consensus opinon” to create it. If you want to have a picnic in a park you do not need to obliterate everyone else’s picnic.
I did not want to comment anymore on here…but I was informed that a couple of old comments I had made a week or so ago, that got lost in the spam computer file, had been found. Yesterday I was told those apparently got published, after my ceremonious bon voyage. I realise this would make me look like a bag lady who had left the contents of her bag all over the rear hall. So I have had to come back, say a more exquisite bon voyage, curtsey and stride off. I have not browsed whether anyone has replied to any previous comments I made since I no longer have time to get caught up in doing so. I must let the matter rest.
If anyone has a need to contact me that would be ok.
I really have way too much to do. So I cannot comment anymore.
I am leaving the coast since I believe a global flood is going to obliterate such regions.
Report comment
I will miss your comments. You are free to go. But I will miss your comments. And I really like your evocative name!
Report comment
I am honoured. Indeed I am touched. Though you may not miss my latest comments. Yesterday I was gnawing the gristle of my last supper. I may have said something pitiless.
Report comment
I have been keeping something from you. All of my fans.
I do not have any fans. A month ago the angels and I were chatting and I said rather forlornly…
“People do not seem to hear me on the comments section”.
To which one of the angels replied to me…
“It is because they think you are mentally ill”.
I fell about laughing that a site for antipsychiatry would find me too nutty.
I have been at pains to get people to listen more to the mad than the “logical”. But it seems to have backfired. Or rather gone smoothly and proven my point…that “reason” repeatedly cannot hear “poetry”.
A life without poetry is loveless. Poetry is “feeling”.
That is why Jesus spoke in almost unintelligible poetry.
To which later ediface of The Church replied by burying such “feeling words” under centuries of rational, analytical, rule riddled dogma.
Love thy neighbour.
Forgive thine enemy.
Twenty one centuries later and we still cross examine and pick the words apart so our guts don’t have to “feel” them.
Buddha also.
If the mad are to be heard then they may be believed. The mad who say they are not mad at all would beautifully be accepted in what they believe and what they think of themselves. And the mad who say they are mad would be beautifully accepted in what they believe and regard of themselves.
Madness is like being in touch with your inner child. A child insolently immune to the dictates of oppressive “logical regimes”.
What is a child? A small person who knows entirely what their “free choices” want to be.
An over emphasis on “reason” tries to organize the child to only have particular choices. Right choices.
This horrible lesson about how your inner mad child must get given an ideological lesson in how to make its own choices is a bar to freedom.
So quite why antipsychiatry are in a hurry to erase the mad word is a bit of a mystery. Just because the child is ill treated does not mean getting rid of the child.
Just because the mad are ill treated does not mean getting rid of the mad.
Making them all normal. Whatever that means. It probably is not what your normal is. Your normal free choices for you.
I said I have been keeping something hidden.
It is this…
The human is an animal.
There are no “logical” animals.
There are only “feeling” animals.
Animals do not tell other animals that “have to” call themslves schizophrenic.
Animals do not tell other animals that they SHOULD NOT look mad.
Animals do not tell other animals that they cannot call themselves schizophrenic or pee on streetlights or roll in leaves or guzzle the wrong food or drink muddy water.
Animals treat other animals like children who are FREE to make their OWN CHOICES.
If someone does not treat you like an animal, run screaming for the hills.
Put that in your pipe and smoke it….puff…puff….
Report comment
Beautifully articulated, Mr. Whitaker, many thanks for your honest and important scientific reporting.
Report comment
Thank you Robert for this essay. It’s states the painful truth, which is more than can be said for psychiatry. As you so aptly state, “The erosion of medical integrity is, in this instance, complete” –
But that’s psychiatry in a nutshell, because psychiatry isn’t about integrity – it never was, and never will be. And dear old Tom’s job isn’t about scientific integrity – his job is to promote psychiatry to protect the status quo. To hope or expect anything else from the guy (or psychiatry at large) is a fool’s errand.
I find people like Thomas Insel sickening, but not surprising. And I’ll never understand why the rest of medicine doesn’t take psychiatry to task for its obvious lack of scientific substance. I don’t see how any self-respecting physician can have anything other than contempt for psychiatry’s throw-spaghetti-on-the-wall tactics.
And I don’t think the increase in “psychiatric illness” reflects reality at all. I think the reality is that people have been talked into “illness” by doctors who’ve been trained to hand out drugs at the drop of a hat.
And since when did emotional upset become a physical problem? Since psychiatry figured out it’s a great way rope in patients.
The truth is that people in psychological distress/trauma ought not to look to the medical community, or even the psychotherapeutic community, because all these do is pathologize people’s reactions to stress and trauma. Just look in the DSM!
But good luck to good ol’ Tom. Little does he know he’s looking at a mirage.
Report comment
Robert says,” We need to have leadership that we can trust to tell us the truth about the merits of psychiatric drugs”.
I don’t think psychiatric drugs have ever had any merit, as they don’t heal anything. All they do is mask “symptoms” – and “symptoms” are helpful signs that something is awry in our environment – NOT IN OUR BRAINS –
So a good question to ask might be this – Have psychiatrists ever said ANYTHING scientifically valid?
Yes – but only once – and that was over sixty years ago –
And what was that?
They proudly announced that neuroleptic drugs (a.k.a. Thorazine, etc.) act as chemical lobotomies –
(AS DO ALL PSYCHE DRUGS!)
Now is THAT a merit?
I think NOT –
Report comment
Bob says, “We need to have leadership that we can trust…” –
That would be nice, but I think that cancels out psychiatry.
Report comment
And what do psychiatric drugs do?
They SQUELCH your thought processes –
Define squelch – a circuit that suppresses the output of a radio receiver if the signal strength falls below a certain level –
Report comment
Dear Mr. Whitaker,
Thank you for rebutting Dr. Insel’s insufferably bombastic book in such admirable detail.
Sounds like his book belongs in the Gaslighting genre.
I must confess I get discouraged that people like Insel, “America’s Psychiatrist”, have the bully pulpit. But articles like yours remind me that good minds do still exist –
And though Insel is called “America’s Psychiatrist” (an unenviable position considering psychiatry’s current state of affairs), I see the future optimistically, as playing out – eventually and inevitably – in a much more judicious way, in no small part because there’s people like yourself who care enough to take the time to give integrity its due.
And while Insel may be “America’s Psychiatrist”, I don’t think it a stretch to consider that someday, you and other like-minded folks may be referred to as “Psychiatry’s Copernicus” –
Report comment
Psychiatry’s Copernicus
Report comment
….or Galileo….
Report comment
Thank you, Bradford – that’s even better!
Report comment
True story: One time, I convinced a nurse in theEmergency Room to put in my medical record, that my ONLY “diagnosis” was “iatrogenic neurolepsis”….and she did, and it’s still there…. LOL!
Indeed, my personal experience is that MOST psychiatrists are soul-less, over-educated idiots….
Report comment
Yeah, I guess Galileo did not have a Galileo or Copernicus Giant to compare himself in those days. He was maybe not compared to anyone at all though. Maybe he was snubbed. Maybe the judges of him and the crowds snubbed Galileo and called him Mad or Schizophrenic.
Report comment
The truth is, THERE AIN’T NO TRUTH to “psychiatry” – except that it’s the breeding ground for invented “disease” –
So the next time someone asks you who in the heck “Dr.” Insel is, just tell ‘em good ol’ Tommy Boy’s Head of America’s Iatrogenic Medicine – a.k.a. invented “disease” –
And that’s about as true as it gets –
Report comment
And if anyone asks you what psychiatry is, just say it’s A PRESCRIPTION FOR MISERY –
With the only cure being forced to read “Dr.”Insel’s ego-bloated book, as it’ll have you dying of laughter in no time –
Report comment
What can be learned from reading Dr. Insel’s book?
That mainstream psychiatry is run by BUFFOONS –
Report comment
But wait a minute – I thought iatrogenic meant physician-created disease –
THAT’S EXACTLY WHAT “PSYCHIATRY” IS –
Report comment
What’s it like being a psychiatrist these days?
It’s blowing smoke while chasing lab-created rainbows –
Report comment
After reading Insel’s book, how would you describe mainstream psychiatry?
I think the term “Bad Medicine” fits quite nicely –
Report comment
Iatrogenic Medicine? Why not Rhetorical Medicine?
No…no…wait! How about Hyperbolic Medicine, or Propaganda Medicine!
Naw…you’re both wrong. Gotta keep it simple –
Simple? But that’s something psychiatrists will never be able to do!
That’s true, but I’d still put my money on Pie-In-The-Sky-Medicine – but any of these should keep those Bozos busy for a looong time….
Report comment
The Dr. Insel’s of the world should take note –
Education, accolades, and endless funds at your disposal do not guarantee finding the answers you want or expect.
Just look at Dr. Insel’s decades-long effort at grabbing what he thought would be mainstream psychiatry’s brass ring. He came up empty-handed.
Yet he refuses to give up his vain hopes and delusional dreams of someday discovering a meaningful link between his precious mainstream psychiatry and his incurable infatuation with “neuro-bio-genomic” medicine. He’s foolishly committed to sustaining mainstream psychiatry’s scientific misadventures.
It’s too bad he can’t see that mainstream psychiatry is neither science nor medicine.
And what is mainstream psychiatry?
A deadly serious RIGGED GAME of semantics and drugging –
Report comment
But don’t psychiatrists take The Hippocratic Oath? You know, “To First Do No Harm”?
Yes, but psychiatrists have been known to tweak it to suit themselves (just call it the Hypocritical Oath) –
Report comment
You gotta hand it to science and psychiatry. They never give up searching for their elusive pot of scientific gold –
Science and psychiatry? Somehow these two don’t seem to go together…
And they never will –
Report comment
I think Dr. Insel studied the wrong stuff in college –
Really?
Yep – he shoulda stuck to politics, creative writing and theatre –
Report comment
What’s the important qualities to have as a psychiatrist?
SHOWMANSHIP AND SALESMANSHIP –
Report comment
What do you need these days to be an effective psychiatrist?
SHOWMANSHIP AND SALESMANSHIP –
Report comment
With so much lack of evidence, how could Insel ever write such a fantastical book?
I don’t know. But I guess he must have figured some grown-ups still need to believe in a Santa Claus –
Report comment
Could psychiatry and “mental health” be called oxymorons?
Report comment
Maybe mainstream psychiatry can learn something from Dr. Insel’s book –
Oh yeah? Like what?
That maybe psychiatric medicine is an oxymoron –
Report comment
Insel’s attempts were undoubtedly a noble effort, but a dismal failure. Wouldn’t you agree?
Not completely. I agree with the second half of your statement, but not the first –
How so?
I don’t consider it a noble effort to throw oneself headlong into expensive research in a field whose foundation rests on nothing more than a poorly conceived book of medicalized insults –
Report comment
“Dr.” Insel?
How about “Dr.” INSULT –
Report comment
What’s psychiatry?
It’s INSULTING, more than anything –
And what’s the DSM?
Their bevy of insults –
Report comment
What’s the DSM?
Mainstream psychiatry’s Bucket of Insults –
Report comment
Insel’s book is a prime example of what can happen when someone gets to spend too much time and too much money in academia, a place where people are exposed to everything but everyday reality.
And what can happen? Twenty years and twenty billion dollars down the drain.
And what does genie Insel prescribe? Thirty more years of the same –
Report comment
Insel’s book is a glaring example of what’s wrong with mainstream psychiatry –
Which is???
It lacks wisdom –
Wisdom…hmmm…and where can you find that?
Reading the story of the Six Blind Men and the Elephant is a good place to start –
Report comment
What is mainstream psychiatry?
Marshmallow Medicine –
Marshmallow medicine???
You know, all style, no substance –
Oh – you mean it’s a billion dollar vanity project –
You got it –
Report comment
Insel’s book inadvertently reveals mainstream psychiatry’s true motivations: fame and wealth –
Yep – the guy’s got ‘em all off on that decades-long “neuro-biological” toot.
Someone outta tell the guy the party’s over –
You can’t- he’s convinced psychiatry’s bound for glory –
Report comment
Hey, what’s wrong with you? You look beat –
I am, ‘cause I had a bad dream last night – or maybe it was a nightmare –
Oh yeah? Say more –
Well, I dreamt I was in a roomful of psychiatrists, and they were all excited playing this game –
Game? What game?
A big, huge piñata, in the shape of bottle, and when they busted it, a load a pills spilled out!
Well I wouldn’t call that a dream OR a nightmare –
No? Then what would you call it?
REALITY –
Report comment
removed for moderation
Report comment
Insel’s book inadvertently reveals mainstream psychiatry’s true motivations: fame and wealth –
Yep – the guy’s got ‘em all off on that decades-long “neuro-biological” toot.
Someone outta tell the guy the party’s over –
You can’t – he’s convinced it’s bound for glory –
Report comment
The equation is simple –
MORE PSYCHIATRY = MORE “ILLNESS” –
What in this equation does Insel not get? He says he sees this, but his answer is to just do more of the same.
Which begs the question: Why can’t some people accept defeat?
But apparently, not even he can answer that –
Report comment
If he were a real scientist, he would never view finding out the truth as “defeat!”
Report comment
Thank you Steve!
Yes, it looks like Dr. Insel was more interested in being seen as “right” than doing right, which would have been to acknowledge the truth, but he wasn’t looking for truth, he was in it for the glory –
Report comment
And I’d like to think a scientist goes into something with the attitude that “This may be right, but it might be wrong”. But Insel had other ideas. His mind was made up.
He didn’t practice medicine, he practiced Scientism –
Report comment
Guess what?
What?
I just heard about psychiatry’s latest brain fad –
No kidding? Spill –
Okay – get this – the chemical imbalance theory is now passé –
Oh? So….they must be into the neuro-bio-genomic thing now, huh?
Nope. They gotta whole new thing going on called “brain circuits” –
“Brain circuits”? Jeez…I wouldn’t call it “brain circuits” –
No? Then what would you call it?
Their BRAIN CIRCUS –
Report comment
No one has ever seen a “brain circuit.” But the “brain circus” is on wide display for anyone with his/her eyes open!
Report comment
Dr. Insel’s forays into science have not panned out. He could have saved himself and mainstream psychiatry a lot of trouble had he simply heeded the saying, “Don’t try to be something you’re not” –
But maybe the genomic explosion gave him a bad case of FOMO –
Report comment
How does mainstream psychiatry differ from other branches of medicine?
Most other branches look for more cures, while mainstream psychiatry makes up more “illness” –
Report comment
Too bad Insel couldn’t see what mainstream psychiatry REALLY is, especially before wasting everyone’s time and money –
And what is “mainstream psychiatry REALLY”?
Politics and economics –
Oh. And who said that???
Dr. Szasz –
Report comment
Why is it most psychiatrists get so defensive whenever their views are challenged?
Defensive? Challenged?
You know what I mean – always willing to twist the truth to make themselves look right, no matter who they end up throwing under the bus, and them acting like everyone has flaws but them –
Well, that’s easy to explain: it comes from most of them being deeply insecure, and having a chip on not just one shoulder, BUT TWO –
Report comment
Yes, Steve,
I see psychiatry, psychology and the pharmaceutical industry as a three-ring circus – and I’ve learned it’s best to remain in the audience –
Report comment
It would seem that for all Dr. Insel’s qualifications and efforts, he – as well as most psychiatrists – have forgotten the simple law of cause and effect.
To wit – in his book, Dr. Insel states what he sees as the probable cause behind mainstream psychiatry’s failure to produce a lasting and “meaningful” social nirvana: a lack of social supports and the public’s accompanying “lack of engagement”.
But it seems reasonable to consider that perhaps it’s these lacks (decent housing, a social community, a purpose in life) that are causing these “illnesses” in the first place. And I find it telling that Insel left out that bulwark of social, psychological, and physical support – a decent job. Apparently he hasn’t considered that that might give some people a fighting chance of providing these things for themselves, and in doing so, preserve their sense of dignity. But I guess that’s something he and others with an m.d. have far less occasion to worry about.
And as for the public’s perceived “lack of engagement” – i.e. drug “treatment” and psychotherapy –
If Insel and most of his cohorts had been paying proper attention, they might have been able to see that these two “therapies” don’t work well for more than a few people.
So maybe he and mainstream psychiatry should consider looking at their own “lack of engagement”. After all, spending their days glancing at little more than their text-heavy DSMs and gawking at esoteric genomic sequences would give anyone a bad case of social myopia –
Report comment
More on cause and effect –
There are times when the job itself causes someone’s “mental” distress; indeed, the stress of having to work in a hostile or otherwise toxic environment can take its toll on anyone.
And the same can be said for any environment, be it marriage, family, school, social groups, and even countries – not too mention experiencing unspeakable trauma. And sometimes these difficulties can’t be consciously acknowledged.
But Dr. Insel’s and mainstream psychiatry’s stubborn insistence on finding “neuro/bio/genomic” causes for people’s distress and their continued prescribing of powerful and potentially harmful psychotropic “medications” for their distress is nothing less than a medical travesty.
And what should be done about this medical travesty?
Mr. Whitaker’s suggestion is right on target – get psychiatry out of medicine!
Report comment
Mainstream psychiatry doesn’t deal with tragedy – IT IS the tragedy – an American tragedy in the making. And it will continue being so as long as the Insel’s of the world refuse to read the writing on the wall. And what’s the writing on the wall? That regardless of origin, more diagnoses and more drugs lead to more illness and more disability.
But it’s useless waiting for mainstream psychiatry to change its course because it’s a bureaucracy and bureaucracies don’t change. But sooner or later mainstream psychiatry will have its day of reckoning, because – lo and behold – the medication generation (children from the nineties, aughts and beyond) are now or will be coming of age and WOW – do THEY have their own stories to tell –
Report comment
Mainstream psychiatrists have an incurable disease –
They do? What is it?
WILLFUL IGNORANCE –
Report comment
It’s a pretty dismal and narrow-minded commentary on human beings ability to evolve and adapt to seriously think that what many people may need to be “functional” is contained some or another elaborate pharmaceutical concoction. But that’s the miserable story mainstream psychiatry tells and sells everyone who’ll listen, and even those that won’t. Because it’s essentially all it has to offer – a misleading tale of “you’re sick, take this forever and don’t bother me with questions” –
And what has mainstream psychiatry created? An whole new and ever-expanding subclass of supposedly “sick” people solely and forever dependent on THEIR revolving door services – their captive audience for life – and THAT my friends, is mainstream psychiatry’s America –
Report comment
Seriously, if that’s the problem, why aren’t they working on this with their clients, instead of drugging them into an apathetic state so that they’re less bothered by having their needs go unmet?
Report comment
Steve asks, “…why aren’t they working on this with their clients, instead of drugging them into an apathetic state so that they’re less bothered by having their needs go unmet?” –
I wonder sometimes. I think it’s because psychiatrists and therapists are just like anybody else – they’re off to school and are taught a certain way of thinking and a certain set of answers, which, for the most part, are that people’s psychological problems come from the individual (biology or “character”), not their environment. And in any case, I’ve heard that universities – and medical schools in particular – don’t exactly encourage divergent thinking. And students and residents aren’t in a position to suggest something different; they’ve got to toe the line to get that degree. And doing things differently in private practice could lead to legal troubles as they’re legally obligated to abide by clinical guidelines. And many of them are well-meaning and truly believe in what they’re doing and can only see change as inconvenient and uncertain, and not many people welcome inconvenience and uncertainty. And the status quo is comfortable for them and they’re comfortable in their status, especially after years of strenuous training. And most professionals aren’t looking to change the status quo – they’ve got too much skin in the game. And needless to say, they’re not experiencing their clients problems (for the most part) and most of all aren’t on the receiving end of their “treatments”. And maybe at a certain point they just don’t want to be bothered themselves. And they certainly don’t want to be ostracized for suggesting something different.
People need to stop believing their problems are solved by filling prescriptions or taking part in someone’s idea of “therapy”. But change can be slow because mindsets like this are institutionally created, enabled and promoted and are therefore deeply entrenched.
So change in this area has to come from the ground up – which I believe is possible thanks to websites like this –
Report comment
Any why do they drug people into an apathetic state so that they won’t be so bothered by their unmet needs?
I don’t know, but maybe the answer is in the question – maybe they don’t want to be bothered by people’s unmet needs. Or maybe they don’t know how to help people learn to meet their unmet needs, or maybe they don’t believe their clients are capable of learning to meet their unmet needs. Sometimes people might need something to help them calm down – especially after going through a major trauma – but to be made a chronic zombie isn’t the way to go. But drugging people has gotten way out of hand and people aren’t made enough aware of the drugs potential dangers, and they’re understandably wanting to trust their clinician. But it’s too bad the therapist’s or doctor’s office has become the first stop on the way to drug dependence –
Report comment
It also stops people from looking for better answers. “If my brain’s not working right, there isn’t much I can do about it, is there? Might as well hope the drugs work, because otherwise, I’m screwed.”
Report comment
And why do doctors and psychiatrists drug people into a state of apathy?
Because they’re trained to diagnose and drug. To them that’s “treatment”. It’s as simple as that.
It would be laughable if it weren’t so serious. But that’s their starting point and they’re not about to go much further.
The DSM needs to be scrapped and psychiatric drugging severely curtailed – but that’s not likely to happen any time soon. What’s more likely is a widespread public outcry against psychiatric diagnoses and drugs, but that may be a long way off –
Report comment
Extreme states do exist, (i.e. psychosis, manias, paranoia, catatonic depression, to name a few), and can happen to anyone for any number of reasons. But even these situations deserve to be looked at with an open frame of mind.
But Dr. Insel’s fixation on genes and neurons doesn’t begin to address the real reasons why so many of our homeless are “mentally ill”. And why can’t he see that the changing economy has been good to him and not to others? Psychology 101: tough breaks can break anyone’s mind. And street drugs only add to what has become an increasingly complicated problem.
So I would question Dr. Insel’s and mainstream psychiatry’s grasp on reality before I question anyone else’s –
Report comment
People don’t need any more of psychiatry’s “medications”, and Insel’s incessant genomic theorizing is an expensive and embarrassing pipedream.
People need someplace other than the emergency room to get their bearings when experiencing extreme states.
I once read of a place headed by a psychiatrist where people could go instead of the emergency room. It was a safe place where people could come and go as they pleased, and get “medications” if they asked for them, and rest in cushioned reclining chairs with blankets and pillows.
It sounded like a safe, respectful alternative for people.
Report comment
Steve says, “It also stops people from looking for better answers. “If my brain’s not working right, there isn’t much I can do about it, is there? Might as well hope the drugs work, because otherwise I’m screwed.”
This is exactly the destructive approach I’ve seen growing for years. I see it as a convenient way for detached people – and this includes “mental health professionals” – to deny reality. And it strikes me as especially unhelpful, even cruel, for upset people to be faced with this attitude from “mental health professionals”. And it’s ultimately insulting to have someone suggest that their problems come from their own “inadequacies”.
And on a wider scale, the excessive prescribing of “psychiatric medications” always looked to me like the “bread and circuses” or “let them eat cake” course of action. And this is why I’ve always viewed the majority of “mental health professionals” as exploitative.
Report comment
I just thought of an acronym for Psychiatry –
TSOTWASWIS – “Throw Spaghetti On The Wall And See If It Sticks” –
Report comment
“Throw Spaghetti On The Wall And See If It Sticks” –
TSOTWASIIS
Report comment
Now we can’t be too hard on dear Dr. Insel.
He’s only doing his job –
After all, he knows better than anyone that every group needs it’s scapegoat (a.k.a. psyche “patient”) –
Report comment
So what’s it like seeing a psychiatrist?
It’s like getting addicted to nicotine – only it’s harder to quit psychiatry –
Report comment
What is psychiatry?
The Tobacco Industry of the Mind –
Report comment
What is psychiatry?
The Tobacco Industry of the Soul –
Report comment
Dr. Insel must be spending lots of time in Silicon Valley these days –
Really? You mean the “fake it till you make it” capital of the world?
Yes –
Doesn’t he realize someone got caught in some shenanigans there recently?
Yes, but some people never learn –
Apparently so…
Report comment
What would have been a better title for lnsel’s book?
CONFESSIONS OF A PSYCHIATRIST:
America Should Run For It’s Life (as I don’t know what the heck I’m doing) –
Report comment
How would you describe “psychiatry”?
Big Egos, Big Books, Big Money, Big Mess. –
Report comment
Someday, psychiatry as we know it will be no more. At such time, books may be written about its slow but steady decline.
So here’s a few titles that might be useful:
1. “PSYCHIATRY: The Rise and Fall of Institutionalized Insanity”
2. “PSYCHIATRY: How Freud’s Dreams Theory Went Corporate”
3. “Human Wrongs to Human Rights: Psychiatry’s End in the Twenty-First Century”
4. “From Trauma to Truth: Losing the Lies of Psychiatry”
Report comment
What’s “psychiatry”?
FITYMI Medicine –
Fake-It-Till-You-Make-It-Medicine –
Report comment
Wait – what did you say psychiatry is?
A PRESCRIPTION FOR MISERY –
Report comment
What did you say psychiatry is?
Voodoo Medicine –
I think at this point I’d be better off with voodoo Medicine –
Report comment
Dr. Insel must have spent lot of time writing his book in Silicon Valley –
You mean the “fake-it-till-you-make-it” capitol of the world?
That’s it –
Doesn’t he realize someone got caught pulling some shenanigans up there recently?
Yep – but it just goes to show you – some people just can’t learn –
Apparently so…
Report comment
Just remember these two things when reading Insel’s book:
That science is the VOICE OF REASON –
And psychiatry is the VOICE OF RHETORIC –
Report comment
How could Dr. Insel have written such a fantastical book?
I guess he realized that a truthful book on psychiatry would’ve meant a book full of nothing but empty pages –
Report comment
What does Dr. insel fail to realize?
That being a bio-psychiatrist is like looking for the freckles gene – and just about as meaningless –
Report comment
But they HAVE found the freckles gene!
So what? And just what’s wrong with freckles anyway?
Nothing – but it seems psychiatrists don’t like seeing them on people –
All you’re saying is that freckles are the psychiatrists’ problem –
Yes – but shouldn’t they do something about them?
Yes – look the other way AND MIND THEIR OWN BUSINESS –
Report comment
So why did Dr. Insel write a book?
Because he felt like taking an ego trip –
Define ego trip – an activity done in order to increase one’s sense of self-importance
Report comment
Removed for moderataion.
Report comment
I think Dr. Insel needed to take an ego trip –
Most psychiatrists do – it’s a job requirement –
Report comment
And as for any reported increase in “psychiatric illness” –
I don’t think this reflects reality at all. The reality is that doctors have been trained to hand out diagnoses and drugs at the drop of a hat, with the end result being a nation of people erroneously believing they’re “sick”, but tragically, that’s ONLY AFTER they’ve seen a “psychiatrist” –
Report comment
Will someone please tell me why psychiatrists are so sure of themselves? It seems ridiculous in a field where diagnoses and “treatments” are based entirely on subjectivity and wishful thinking –
And it’s especially odd when you consider how other branches of medicine (which happen to based on objectivity) don’t have this problem –
Report comment
“Treatment, Rickey! Treatment!”
Report comment
Psychiatrists??? To hell with them –
But I heard psychiatrists practice medicine. Isn’t this so?
HELL NO —
Then what DO they practice?
The Power of Suggestion –
Huh???
Just read Insel’s book. You’ll find it clear as day –
Report comment
So what did you learn from reading Dr. Insel’s book?
Well, it sounds like the guy’s gotta serious savior complex going on –
You mean he’s giddy with the prospect of curing the world’s ills?
Bingo!
Report comment
The power of suggestion? What is that? And what does that have to do with Dr. Insel’s book?
All it is is the idea that people will very often live up to – and in mainstream psychiatry’s case – LIVE DOWN to your expectations –
Could you please be more specific?
Yes. It’s how people take ideas given to them and turn those ideas into reality, and in this case, mainstream psychiatry’s “reality” –
Which is???
“Illness”, “illness”, and MORE “illness” –
But what does this have to do with Dr. Insel’s book?
It means he should have spent more time getting to know the people he intends to “treat”, rather than his “research” cronies –
Report comment
Mainstream psychiatry’s “reality” –
Now there’s an oxymoron!
Report comment
Actually, other branches of medicine do have similar problems to psychiatry. In fact, all of science does. I think they call it “scientism.” Psychiatry does not stand alone. Thank you.
Report comment
Thank you rebel for clearing that up for me. And I agree with you – but psychiatrists seem to me to be the most closed-minded –
Report comment
rebel says, “Actually, other branches of medicine do have similar problems to psychiatry. In fact, all of science does. I think they call it “scientism” –
rebel is so right.
And what’s the definition for scientism? “excessive belief in the power of scientific knowledge and techniques” –
Well, there it is, folks! THAT’S the definition of psychiatry –
Report comment
I would define it a bit differently – I see “scientism” as being the believe that Scientists are Authorities and that we peons are too stupid to understand their deep wisdom, so we have to simply believe what Scientists tell us and do as they tell us, even if it makes no sense to us at all. Because Scientists are All Wise, and we mere mortals couldn’t hope to understand the depths of what they are telling us about.
Report comment
What’s wrong with psychiatrists?
They’ve all gotta bad case of scientism –
And what’s “scientism”?
INTELLECTUAL BLOAT –
Report comment
(Duplicate Comment)
Report comment
I know! Have you even heard of somebody who is “anti-cardiology”, or “anti-gynocology”? WHY is psychiatry the ONLY “branch of medicine” that has an “anti”? Auntie Psychiatry has the answer! Google her! LOL!
Report comment
Auntie Psychiatry –
Thanks for the tip, Bradford!
Report comment
Thank you Steve for your more detailed definition of scientism, “…the belief that Scientists are the Authorities and that we peons are too stupid to understand their deep wisdom…” –
This accurately describes the irritatingly pontifical attitude of most psychiatrists.
I’d call it “Psychiatric Scientism” –
Report comment
Is psychiatry a science?
Yes, an illusory science –
And what does that consist of?
RUBBING ALADDIN’S LAMP
Report comment
What is psychiatry?
Drugging people silly while rubbing Aladdin’s Lamp –
Report comment
What is mainstream psychiatry?
Dogmatic Medicine –
Report comment
Why did Insel write his book?
To keep people from seeing mainstream psychiatry for what it is –
And what is it?
IRRELEVANT –
Report comment
Shocked. Told so many times that AP are proven LD-50 tests poison, that talking about damages, long-term effects, etc. just becomes a sell out to readers who don’t get informed that these are not medicine but poison. One more time .. antipsychotics are poison, see for example zyprexa here https://pubchem.ncbi.nlm.nih.gov/compound/Olanzapine . Please inform your readers properly, that have the right to not get misled by organisations that say to be here to better the future for psychiatric patients. It won’t if you keep silent about AP being poison. Thnx !!
Report comment
Most definitely, bthate, The antipsychotics and antidepressants are both anticholinergic drugs. And all doctors are taught in med school that combining the anticholinergic drugs can create “psychosis,” via anticholinergic toxidrome.
So we are looking at staggering amounts of intentional malpractice, that the psychiatric and psychological industries have participated in.
Report comment
“Who controls the past controls the future. Who controls the present controls the past.”
-1984, George Orwell
Report comment
(Duplicate Comment)
Report comment
“…Not everyone buys this conspiracy theory. Others see the problem as ineffective treatment. ..”
“….and many of the people receiving medications do not take them . . . so the crisis of care is not just lack of access (to treatment), but lack of engagement [with treatment.]..”
Once a Professional begins to talk like this it is obvious that they have “sold out”. But maybe Thomas Insel feels that he has no choice. If he rocks the boat he can become a “reject” himself.
Report comment
And as for Thomas Insel’s being called “America’s Psychiatrist” –
I think it more accurate to call him “America’s ASTROLOGIST” –
Astrologist?!! What on earth do you mean?
Well, you know the difference between astrology and astronomy, don’t you?
Yes, yes, I think I do – now let me guess – astronomy is real and astrology is not – now am I right?
You are exactly right –
Report comment
How about “America’s Phrenologist?”
Report comment
Thank you Steve –
I hadn’t thought of that – but I suspect the Phrenology hat will fit Tommy Boy just fine –
Report comment
Medicine and herbalism and sowing all doffed a plumed hat to Astrology. A surgeon barber consulted apothecaries who consulted birthcharts and synastry charts and horology astrology to see the most conducive time for “a treatment”.
Father TIME, the GREAT HEALER, was more respected in the medieval epoch than in our frenetic era. Apothecaries who poured over astrology charts and advised kings of what auspicious hour to pee in piss pots and do battle, often rose to eminence in extraordinary regal turrets.
In many ways because ancient Babylonion astrology is the parent of modern medicine then Big Pharma and maybe also teeny wee pharma came out of astrology. The vast river of humanity’s flirtation with rock solid undeniable certainty.
Comically it is a river of certitude also drowning its bickering opponents.
I prefer to see reality as a mirage. A mirage is chaotic and cannot ever be made all certain.
In a mirage a person experiences reality as completely real. That “reality” has it that two plus two equals four and when you eat a lemon it feels chilly. Real is real “inside” the mirage. But the container of that “realness” is not real at all. That container or background web of light or vibration or frequency is the mirage. We are just too embedded in it to be aware of it. But as soon as you do become aware of how the whole of reality is inside a mirage it makes “logical” analytical correct “real” not something you need take quite so solemnly anymore. You are liberated from having to take life so seriously. The only thing you need take for real are peoples real feelings. And your own feelings of course. It all becomes a kind of heaven. Unfortunately the main force that insists we take reality and life too seriously is “logic”. It runs on adherence to laws and rules but a lot of the time “feelings” are not very amused by those. If you become aware of the way reality cannot be taken too seriously since it fits in a mirage then nothing you want to be exploring can be deemed serious or NOT serious…it transcends such pithy judgements. Therefore to regard astrology as serious or NOT serious is besides the point. The question then becomes….Do you enjoy it?
Does dabbling in starsigns make your “feelings” feel good? Does astrology or anything you are curious about in the gigantic mirage make you “feel better”? If the answer is “yes” then there is nothing “wrong” with your “feeling” about astrology.
By the way mine’s a Gemini. Moon in Pisces. Grand water trine. Everything besides in twelfth house. The asylum of the natal chart.
Report comment
Astrology is actually MORE valid & scientific than psychiatry can EVER BE. You’ve never had your birth chart done by a professional astrologer. Planets & stars are charted with mathematical precision. There is SOME SCIENTIFIC BASIS for astrology. Psychiatry is PURE FRAUD, feeding like a parasite off human suffering & misery….
Report comment
Bradford says, “Astrology is actually MORE valid & scientific than psychiatry can EVER BE”, and,
“Psychiatry is PURE FRAUD, feeding like a parasite off human suffering & misery…”
Bradford speaks the truth.
I have consulted astrologers occasionally in the past, and I’m happy to report that I received more help from them than I ever got from psychiatry or psychotherapy.
It’s interesting how astrologers follow the planets as they travel along the constellations, and astrology’s role in ancient civilizations is truly fascinating. And it’s uncanny how accurate some astrologers can be. They must have an intuitive gift.
I searched astronomy and found it’s classified as a natural science, a branch of science that deals with the physical world, e.g. physics, chemistry, geology and biology. Then I searched the science of psychiatry and it said, “a branch of medicine focused on diagnosing and treating mental health disorders”, followed by, “The term literally means “the medical treatment of the soul”. Now THAT stopped me cold – “medical treatment of the soul”? And just HOW does one “medically treat” the soul? And what does that even mean when the definition of “the soul” is nebulous at best? This proves that all psychiatrists are doing is DRUGGING PEOPLE SILLY and calling it “medicine” – all the while inflicting serious physical and psychological harm with their pharmaceutical and “psychotherapeutic” garbage.
On a more positive note, I think the best part of astrology is that it encourages people to think not only subjectively, but objectively about what’s going on in their lives – without the specter of “illness”.
And I never once left an astrologer feeling humiliated, demoralized, dehumanized, AND demonetized, which is more than I can say for psychiatrists OR psychologists –
Report comment
Bradford,
My apologies if my attempt at humor was off-putting. I consider astrology a valuable interpretive resource and venture.
Report comment
I found these definitions for astronomy and astrology:
Astronomy –
“(from Greek literally meaning the science that studies the laws of the stars) is a natural science that studies celestial objects and phenomena. It uses mathematics, physics and chemistry in order to explain their origin and evolution. Objects of interest include planets, moons, stars, nebulae, galaxies and comets”.
Astrology –
“the study of movements and relative positions of celestial bodies interpreted as having an influence on human affairs and the natural world”.
I think these both serve an important function.
But the same cannot be said for psychiatry, as its claims to either biological OR empirical science are flimsy at best, with the former being tainted with greed and the latter with bias –
Report comment
Relax, Birdsong! Im not off-put at all! I appreciate your views & words very much…Keep speaking your truth. I always welcome it.
Report comment
Thank you, Bradford –
Report comment
And one more thing about psychiatry, astrology and astronomy –
Now, I may be wrong, but it seems to me astrology and astronomy know what they are, and are therefore content to stay in their own lanes. I never had the impression they’re competing with each other.
But psychiatry is another matter, as no one (including psychiatrists) can agree on what they are, what they do, or why they do it. But there are five things you can count on with psychiatry:
1. They’re forever changing their minds, and
2. When one thing doesn’t work, they’re off and running to come up with something else, and
3. You can count on THAT not working either, and
4. They’re always off to someplace even MORE wonderful!
and
5. All they need is more time, more money (of course), and (wink-wink) the public’s gullibility to make their dreams come true –
Report comment
Here’s psychiatry’s theme song (that they sing to each other at their DSM meetings) –
“I’m just wild about psychiatry –
And psychiatry’s wild about me!!
Report comment
Someone once said, “In this world nothing is certain but death and taxes” –
And psychiatry’s ENDLESS ANTICS –
Report comment
You said psychiatrists can’t agree on what they are. What do you mean?
I mean they now call themselves “neuro-bio-psycho-social psychiatrists –
Wow! That’s a mouthful –
You said it -but there’s one thing you can count on –
What’s that?
Next week they’ll come up with something else!
Report comment
“Medically treat the soul”? No one can “medically treat” the soul.The soul cannot and should not be “medically treated”, and no one should even try, as this is where the trouble starts – and it’s called drugging –
I think you mean psychiatry –
Same thing –
Report comment
Now here’s the $64 Question –
What causes mental illness?
PSYCHIATRY –
Report comment
What’s the worst thing about psychiatrists?
They’ve lost sight of what’s important – not that they ever saw it to begin with –
And what’s most important?
Believing in yourself, NOT an “illness” –
Report comment
And mainstream psychiatrists don’t “treat” the soul –
THEY NUMB THE SOUL with their ever-expanding cache of hazardous “medications”/drugs –
Report comment
Removed for moderation.
Report comment
“Neuro-bio-psycho-social” psychiatry – whew! I’m outa breath just saying it –
Yep – the fools can’t make up their minds, that’s for sure. They’re into everything but the kitchen sink –
Yeah…makes me wonder what it’s like being a psychiatrist these days –
Oh I can tell you that –
Oh?
Yep – it’s like constantly playing and losing a game of “Twister” –
Report comment
“Neuro-bio-psycho-social” psychiatry –
Bibbiti Bobbiti Boo!
Report comment
What do psychiatrists do?
SELL SICKNESS –
Report comment
If astrology helped you more than mainstream psychiatry or psychotherapy, then why did you go to psychiatry and psychotherapy?
Because like anyone else, I bought into the “doctors know best” nonsense –
Report comment
And how can people who have no soul (i.e. mainstream psychiatrists) “treat” the soul???
And they don’t “treat” ANYTHING – all they do is DRUG –
Report comment
Ahemmm, cough,
You think the moon in pisces I mentioned was conjecture? Care to discuss the yod and moon’s nodes and placidus versus equal house and conjuctions and trines and sesquisquares and oppositions and the nadir and how uranus causes sudden unheaval whereas pluto causes slow implosions and how neptune is more psychically creative than playful cheerful jupiter and how having venus in twelfth house makes a person find no love in life but in the beyond, so spiritual love?
All cultures discover their own typologies, ways of figuring out what makes us all different. Those typologies may be in soft focus “lore” or “morality tales”, of which each culture bestows its own outlandish imagination, or the typologies may a hint of fussy “logic”, as in Mayan superstitious numeracy and calendars, dates when gods do marvels and dates when specific people ought to. Astrology flirts with “logic” each time a natal chart requires a mathematical compass to assess where in the celestial hemisphere the cosmic bodies were stationed, the sun and mars and so on. The “logic” will tell you who you are, says astrology. Like it or not, people lap that up because everyone wants to be told what they need to know, which is that there is nothing “wrong” with them. They want their being a Taurus or a Capricorn to mean they are loveable. It is refreshing to feel that love is so simple, simple as being a Leo. Thank God, they do not have to try hard anymore. But the “trying hard” often comes intitially from feeling all “wrong”…by being told they are “all wrong”….by some other school of “logic”, or some other typology that pins them as a nutter. Not a Leo.
So what you have in a mixed bag of a civilization is a “merging” of many conflicting tribal typologies all vying with each other as to who has the “right” kind of analytical knowledge of “the standard humanoid”. Whose typology is correct and worthy and “logically right”.
Psychiatry is one such tribe or culture, just like astrology is. Psychiatry saw a virtue in advancing from medieval astrology by making that sort of typology more “practical”, and less astronomically romantic and “feeling”, since astrology still had a lot of charming “feeling” in it. Psychiatry said that although astrology was “logical” with its quasi scientific charts and set squares it tended to be so overly sentimental that it sounded “mad”.
What psychiatry’s typology wanted to do was not sound so “mad”. So it emulated doctorly bone sawing practical medicine. Erradicating emotionality. This was not cruel on the part of psychiatry to become so “logical”. They had seen what hocus pocus superstition had done in the Inquisition and wanted no part in knee jerk cruel witch hunts of the past. They feared going down the sentimental or imaginative path, but some of that fear was coming from the way ANY “logical” way of life becomes “estranged” to inner emotions and forgets what those are. When that occurs “feelings” become the enemy, the “other”.
So inadvertantly psychiatry found half of its professionals rushing to protect people from a “madness” that could get them knotted to the stake, as such those psychiatrists were healers, but half of them were applying cold clinical “logic” out of the fear of “feelings” connected to the chaos and looseness of madness.
Fear creeps into ANY culture. It can take hold in the culture of astrology, in verbose text books on astrology, that use typology to highlight peoples differences, and it can take hold in the culture of psychiatry, in its textbooks that try to explain differences.
There is no harm in ANY culture. No culture is a bully. The ingress of unnecessary fussy punitive “logic” makes some people in that culture or religion or society become A BULLY. A culture will be a safe house for many bullies if it enshrines “logic” more than “love”.
But just because a culture goes through an eruption of bullying does not mean that to stop the bullying you have to erradicate the culture. You just have to ban the bullying.
Which is why I court unpopularity here in feeling that psychiatry as a culture, being as potty as astrology, is harmless. Harm only saturates a culture when it is destabilized by an over emphasis on “reason” rather than “feelings”. But this dynamic can occur in ANY culture, even ballroom dancer culture or yoga culture or priestly culture or even antipsychiatry culture.
It can happen ANYWHERE because of one appalling truth humans like to swerve pondering over. It is this….
WE ARE ALL BULLIES.
Report comment
Robert, Thank you for such meticulous reporting on how psychiatry continues to exploit patients through dishonesty. Somehow psychiatry managed to be considered medicine so most people likely assume such blatant corruption could not be hidden. This industry operates under the guise of providing ‘help’ for the mental well-being of patients therefore making it absolutely repugnant they will unscrupulously harm and sacrifice patients in order to protect their own self-serving interests. Thomas Insel MOST definitely makes a case for psychiatry to be abolished. Many thanks and much respect for your esteemed journalism and extensive humanitarian efforts to expose the truth.
Report comment
Removed for moderation.
Report comment
I’m a phsych patient and not a phsych professional. I’ve been on and off (mostly off) medication for over 25 years. In 2020, I attempted suicide three times in three months. I was on medical leave from work for 7 months. During this period, I was enrolled in phsych educational classes with my insurance company the entire time… Prehospitalization for 6 weeks….. met my personal therapist twice a week….. and finally into a Residential program for six weeks where I lived and breathed mental health.
I was medicated during my leave… heavily medicated for about three months… However, most (and possible all) therapists and phsychiatrists I met informed me that meds were only short term solutions. That we cannot think of medication for psych stuff in the same way we think of other meds like insulin. Meds exist to help interrupt the patterns so that we can work on healing ourselves during the interruption.
It feels like this article assumes phsych meds are supposed to heal and, hey, look at all these studies to prove they do not heal. Yet, the psych professionals who helped me on my journey explicitly told me phsych meds are not for long term use and they do not exist to heal, but to interrupt.
In the end, what truly helped me heal and move past my self hatred and desire to kill myself was the Residential treatment program. It was a combination of intense educational, processing, and group therapies that I believe worked for me. And, honestly, I feel the group aspect was most pivotal. Of course, it was my desire to get better that was the true key to my recovery. For me, it was like what an AA person describes as rock bottom. I had to die or get better. For months, the therapies and drugs failed me…. until the residential program. It took therapies for 7 hours a day, for six weeks before I finally found my hope and desire to live.
It appears to me that psychology based residential treatments are rare and not the norm at all. I was the only resident not going through drug rehab at the same time… and some were court ordered. I’ve had a one-on-one therapist for almost half of my adult life (currently 53) and nothing came close to helping me like the intensive therapy from residential treatment. And CBT has been the most successful for me.
I recognize that this article is not really intended for the lay person like me, but I’m here to tell you that I do believe meds work for the short term, if used along with intensive therapy.
We simply need to shift our thinking away from phsych meds as a cure.
Report comment
Oops. I meant to click on ‘reply’ and clicked on ‘report’ instead, What I intended to say was thanks for sharing MOnkey! I’m glad that you got support that you found useful. Yeah!! I think residential treatment can be useful if it is voluntary. My daughter was forced to live in a residential facility many times and there, her freedoms were always restricted. For some people an ‘open’ facility–a sanctuary populated by people who have the power to come and go as they please, give and receive mutual support, including from humble professionals, may be just the ticket. If the facility is restricted, and residents are court ordered to be there, it can erode trust. Empowerment and choice, even the right to make mistakes must be weighted in favor of the person who is struggling because in the long run, trust is essential for any service to be effective. If a provider lies about a medication or fails to obtain informed consent or later dismisses a side effect or adverse drug reaction, this can erode trust. I agree with you that medications prescribed cautiously for short periods of time can be useful at times, but if the person is forced andor coerced, as my daughter was for many years, and the prescriber or the person administering the drugs by force or coercion uses half truths or downright lies to gain the cooperation of the drugged person, this is gaslighting at its worse. Gaslighting and psychiatric torture can cause a splitting of the self. A person with significant mental or emotional problems can develop far more serious mental or emotional problems if they are exposed, like my daughter was to years and years of forced psychiatry. I consider you to have been very lucky. I hope that eventually my daughter’s luck will turn around and that she will be able to receive appropriate services from so-called ‘professionals’ in a sanctuary-like or homelike, communal environment. But due to her past history of inhumane treatment in the system, some kind of restorative justice is needed as a first step in her regaining trust.
Report comment
Madmom, sounds like your daughter could use the “Inner Fire” type of setting. MiA has an article on it, from Mitzy Sky, on site now, highly recommended…. and, Madmom, you have many friends here, good to see you again!
Report comment
I am surprised your psych professionals said that to you. I’ve almost never seen it. I actually got severely criticized for training our CASA volunteers in exactly this point, by a training coordinator who bought into the medical model.
Report comment
Thank you for being true to you. It is painful to hold contraditory truths and be honest about them. Bless you.
Report comment
I do not believe that it is “simply needing to shift our thinking away from psych meds as a cure” and, in fact, for some people even short term use of psychiatric drugs causes iatrogenic harm. My daughter had an immediate bad reaction to anti-depressants, causing the clinician involved to diagnose her with psychosis and put her on anti-psychotic medication. The result, after three weeks of these medications was her belief that she needed to end her life to stop the horrendous adverse side effects she was experiencing from both these toxic medications. She felt compelled to kill herself in order to stop the extremely painful experience and she almost died in the attempt. Every person is an individual and should not be treated as if these psychiatric drugs are beneficial to all. They can be extremely harmful and life-threatening to self and others. Full facts should be given to everybody so that a choice is available rather than coercion and control of people, as is the case at the moment. Also, the difficulty in withdrawal and reduction from these drugs needs to be told to anybody who decides to take them – whether short-term or long-term.
Report comment
I’m sorry your daughter went through that. I’m glad she has you to stand up for her.
I think all the “antis” – antidepressants, antipsychotics, and antianxiety “drugs” – are on their way to becoming the fentanyl of the future.
Report comment
Ah, but if you recover from psychotic illnesses using unusual means- real medicine, nutrients, dietary avoidance, treating allergies, support groups like SA, etc., then Big Time Psychiatry will rise with righteous fury to tell the world how you’ve let yourself be deceived by scoundrels and are destined to finish your life drooling in the back wards of some institution.
Report comment
There is no need to abolish psychiatry. We simply need to reclassify it as a religion and thereby undermine its false puffery as ‘science’. This article here (on a government server) is compliments of a psych survivor in Finland who I dare not out. I The article really sums up nicely why psychiatry is a religion. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2625374/
Report comment
I second this comment that psychiatry is a religion. Thomas Szasz has said as much if you read between the lines of the writings. Why Szasz did not like “antipsychiatry” the same way you can be anti-christian or anti-jewish. People can choose to worship the holy molecules of psychiatry or not.
Report comment
Found one video of Szasz “Albert Ellis and Thomas Szasz Debate Mental Illness: Primal Scream Therapy” https://youtu.be/l4AwFIVsPE8?t=73
Freedom to worship what you want to worship, but most everyone , lawyers and judges believe the psychiatric drugs are in FACT, medicines.
I blame all the other legitimate (physical science) doctors who go along with psychiatry, but many doctors have severe sadness themselves and seek/take the magical pills of psychiatry.
The planets destruction by the hands of mankind will sort it out one day.
Report comment
I have made a couple of comments but they are slow to appear for some reason so this might sound strange but it wants said, I feel.
I heard of a group called the Aimites, who have built a belief called Aim. That group all live in one huge farmstead and grow their own nourishment. They are profoundly anti-psychiatry. They all share histories of having been abused, either by their absented families or by the education system or by state hospitals or by government regime. They honour holistic ways of healing the broken. They treasure the different. They see every individual as an autonomous human being to be listened to by the heart and respected. They cleave to one another in the spirit of equality and justice. They need nothing from the outside world to which they have abandoned all hope of improving. This reliquishment of having to “fix everything” in “the world” decreases their stress and this reduction in agitation becomes itself a wellspring of healing for the community. They grow in wellness just from that. Outside visitors notice how well the community looks, how joyful and welcoming and healed. This causes visitors to flock to the Aim belief in droves because they feel “the love”.
But at one point a charismatic person joined the faithful little community and told everyone they would have to sort out the whole world. The charismatic person said that millions were dying daily and it was up to the community to “fix” all of “that”.
Soon the once happy community began to experience untold stress and nightmares and pressure from hourly ruminating on statistics. They began to feel upset and distraught and unwell. The charismatic one told them that they felt unwell because “the world” was not “sorted out” yet. The community were told to work harder at rumunating on the depressing statistics. They soon could not sleep at night from thinking about all the little children in the world who were not rescued from familes and education and hospital and government and so on. By getting no rest or peace or sleep over these horror stories the community grew unwell and in such unwellness grew in neediness themselves. They began to burst into tears without any cause and soon the charismatic champion explained that their tears were obviously “for” the millions of desperate people in “the world”, a planet that the community should work night and day to “sort out”.
After a year of this the community members felt like walking wounded. They shuffled exhaustedly into their farmsteading cottages that had been turned into offices and burderned by colossal pointless stress they began to “feel” like “the world” that needs “fixed”. In this regard they ceased healing themselves enough to be healing for anyone. Rather they became more ill than the ill whom they were trying to deliver from evil in “the world”. They stopped looking “welcoming” to outsiders, they stopped sounding interested in equality and justice. They just wanted to talk about how much anguish they felt. Talking like that became a form of therapy but it meant that the only way to feel relief was in talking of desperation. Soon the once lovely little belief called Aim, and its community of faithful visionaries called Aimites, began to “blame the world” for not being an immediately “fixed world”. As if “the world” were an imprisoning blue ball on a chain that prevented them, via obligaltion and duty, from just living and loving and having joyful fun.
It was as if “fixing the world” by “saving everyone in it” had become the new way to pass muster enough to enter the gates of heaven. So that “shirking any responsibility” to “make the world a better place” had become a new type of “cardinal sin”. The much vaunted charismatic person who could not rest in bed until all million people were “fixed” did not realise how miserable by this duty he himself was. No single human being can “fix the world” and yet he had swallowed the devotion of others that said that he could. This meant he could never afford to seem “broken”. It would be “unforgivable”. To fall asleep on the job would seem a luxury only the self indulgent would be delayed by. But if he could not afford to seem broken as he busied himself in “fixing the world” then he would have to choice but to squash all of his exhausted, broken feelings deep down in order to look stoic and invincible and practical.
Soon everyone in the community were doing something similar, bravely ignoring their own brokenness in order to “fix the world” or bursting into tears at the slightest breeze and then “blaming the world” and all its dim sheep-like millions for not being “fixed” fast enough. Either of these reactions grew an unacknowledged resentment “at the world” for “the world” always expecting “super human” levels of stress and compassion and feelingless endurance.
Soon all the visitor was met with was a wall of resentment that the visitor was not “doing more” themselves to “fix the world”. It was as if the visitor was made unwelcome. As if the visitor was a sullen misbehaving “world” that kept flat out refusing to “change” or be “fixed”. A bit like how burnt out and stressed nurses used to see psychiatric patients as “refusing to be fixed”.
The visitors felt “blamed” for something without being able to ever figure out what exactly. Soon the charismatic person chased after the visitors and produced evidence of why the visitors “should change”. If the visitors declined to modify their choices or become one with the stressed community the charismatic person would present fussy “logical” arguements as to why “the world needed fixed”. The visitor might say that the community is the world and that it is easy to mend, by just rediscovering “the love” that was there in its original founding. The planet is made up of billions of such communitites, so much so that if each one focused on healing itself from within this would soon cover the planet like a patchwork quilt, each patch or community all beautifully healed and back to normal and repaired again. And being so full of harmony, rest, joy and love, would be as an oasis in a desert to the millions of miserable.
Gosh! I have just seen how Aim could unintentionally look like MIA spelled backwards. I do think that MIA maybe should become “a belief”. I do not see why not. A belief is a fantastic thing. There are seven thousand on planet Earth. Who would object to squeezing in one more? Have MIA celebrations. Have MIA healing prayers. Have MIA mood healthy diets. Have MIA comfortable bean bags and joyful singing assemblies. Have no discernable leader. Have ten leaders. Have anti-psychiatry be the bonding purpose. Have worship of the sanctity of the holistic body. Have outreach. Have refuges. Have communal get togethers. Have art and crafts. Have a special place of welcome to the unbeliever, the nervous visitor, that equally autonomous individual human being who has a free right to believe in their own way.
There is nothing but fun and joy in building a belief. All beliefs are utterly harmless. They are just specific celebrations of a specific kind of differentness.
Beliefs only descend into bullying when they give themselves egotistically impossible obligations to “fix the world”. It is seldom a belief’s job to “fix the world” but by becoming only one “free choice” in everybody else’s world. By becoming a happy choice and the nextdoor belief becoming a happy choice and the nextdoor belief doing so and the next until all neighbouring beliefs are happy from within, this happiness spreads over the face of the planet.
It requires sort of giving up “logically” or bickeringly or stressfully or bullyingly “fixing the world” and instead it only needs becoming the unutterable peace that the planet is dying for.
Report comment
Wow. You like to write longer comments than I do! I wish there was an easy way we could connect and talk directly. I think an unacknowleged great benefit of MiA, is that some of the VICTIMS of psychiatry can come here, and share their stories. I enjoy your writing, perspective, & thinking.
Report comment
Duplicate comment.
Report comment
Mr. Whitaker, please know your work has sustained me thru the darkness of a diagnoses, decade of ‘woe’, & difficult but brilliant re-entry into MY life.
Thank you for never abandoning me, folks like me, & this topic.
I’m so grateful.
Report comment
Thank you, Mr. Whittaker. The article is very enlightening, as usual. I actually trust no one with credentials from either the NIH or NIMH. It’s sort of like the old phrase, ” I’m from the government and I’m here to help.” Sadly, in many cases, if you do get help, it’s the wrong help and in the end can hurt or harm. But isn’t that psychiatry in a nutshell. I don’t know about abolishing or reforming. I think many people just want to live; just want their lives back. Right now, with their emphasis on drugs and even their therapies at present, people don’t get their lives back. The drugs and even the therapies cause the body and brain to be in a zombie-like, sleep-walking state. So, any real problems or issues or hidden from the patient and of course, the psychiatrist and therapist, but they are uninterested anyway. Drugs and therapies are the easy way out, especially for the psychiatrist. Prescribe a drug, send the patient to therapy and the psychiatrist think he or she has the work, without doing any work at all. And who suffers, the patient and eventually society. I am not sure if we can abolish or reform psychiatry. I am not sure what to do with it. It is like that one child who refuses to learn to listen to him or herself and thus tries to obtain their cues from the outside world. These cues thus become unpredictable and untrustworthy, because the child never learns to look within. I imagine in the end, only SPIRIT can solve this problem. It is probably too large for us mere mortal humans. Thank you.
Report comment
I am the BeliefMaker.
I am a travelling salesman of beliefs. In my raincoat pockets are all sorts of methods for building your own belief.
As I outlined in my previous comment the world has many beliefs. I say a planet can never have enough.
The problem on our planet is there is one dominant belief. It is the religion of “logic”.
It is the worst dogmatic religion to befall humanity.
And just as the inculturating conquistadors imported their belief into lands not of their origin, the religion of “logic” has soaked into the soil of everyone’s fertile imagination.
The absorption of the religion of “logic” has bedded in to the Jesus faith and the Moses faith and the Buddah faith and every simple “emotional” and beautiful, joyful, imaginative, loving faith.
This is because “logic” is at war with “feelings” on this planet and so it cannot let the “feeling of love” win. Instead it has to chaperone feelings and judge feelings and critique feelings and humiliate feelings and bully feelings until whatever sweet belief that the religion of “logic” and its verbose complicated rhetoric seeps into becomes a simple belief turned rigid with impossible “rational laws”.
There are ONLY THREE LAWS any human ought to abide by ethically.
Do not kill, do not abuse children, do not be cruel.
If everyone honoured only those three laws the planet would be at peace.
Instead, the religion of “logic” takes over from “love” in ANY faith and imposes “rational control” over every “free choice”. Until an individual cannot be who they harmlessly choose to be. They get told they are “wrong”. This lifetime of being called “wrong” causes such a wound that in order to heal it there grows a wish to pronounce self “right”. But to do so means finding lots of “others” who are “different” to declare “wrong”….”logically wrong”.
It is the foundation of bickering.
I am right but you are wrong..No I am right but you are wrong..No no I am right but you are wrong. Until a finger hovers over the tomato red nuclear pushbutton.
So lots and lots of screeds of analytical data is presented to argue over who is “wrong” and who is “right”. Often being a puppet on a string and appearing noddingly obedient to “logical” rules offers a person an escape from looking “wrong”. They may want to escape such criticism since often the “wrong” are “logically punished” for failing to abide by hundreds of the religion of “logic’s” laws…laws that have nothing to do with the only three ethical laws humans ever need care about but are instead laws about what you can read or say or not say or eat or write or paint or who you are allowed to talk to or not talk to or which celebrity you must call a liar even though you have never met that fellow human.
The internet is a promoter for the religion of “logic”. It is its loudspeaker, spewing bickering laws at you to stop you being “wrong” in your own “free choices”, as if your “freedom of choice” is a new kind of traitor devilishness. Or love is.
The religion of “logic” is THE WORST THING to ever occur to humanity because it worships certainty more than doubt.
Since all individuals are in a process of evolution in their hour or day or week or year, no spectator can ever say they know that individual. Therefore there should always be a respectful curiousity on approaching any individual, not cast iron “know all” certainty.
To punish an individual requires a hubristic level of “certainty”.
What the religion of “logic” likes best of all is “certainty”.
Human certainty has caused climate change.
The religion of “logic” does not tolerate “feelings” because they are unreliable and ever evolving. But by mistrusting “feelings” what “logic” arrives at is a mistrust of “the feeling” of “love”.
So by the time the religion of “logic” has swept like conquistafors into any faith, any faith at all, or swept into pleasant curious doubting explorative science, or swept into any impassioned campaign that just wants to make “the local area a better place” it has swapped “love” for “laws”.
The religion of “logic” takes a beautiful imaginative “feeling based” response to the environment and turns it into something of a bickering, disdainful, intolerant of difference, humourless, overly serious, diligent, workaholic, rule riddled, miserable nightmare.
That loveless finicky policing nightmare is meant to improve the planet?
That nightmare finds its impressive way into ANY GOOD CAUSE and turns it into a beholden regime with catty laws and regulations and unwelcoming stipulations that see “wrong” in those who do not want “logical” advice but prefer their own ways. The religion of “logic” invents enemies on every street corner. Often those “enemies” are merely the childish or playful or joyful. Anyone of “emotion”. Particularly mothers. The most “feeling” ones.
A mother is an archetypal symbol of someone who says you can be “free” to be who you want to be and all of your “free choices” that are based on your “feelings” need no explanation and all of your growing into your independant choices are a sign of health and wellness and are lovely and delightful.
The religion of “logic” is at war with “feelings”, so it cannot tolerate what your inner mother embraces, the emotions that inspire your “free choices”.
It is not beliefs that are humanity’s problem.
There are many beliefs as I have said in my other comment yet there are billions of humans and NOT ONE HUMAN is the same as any other. They are all unique. So why are there not billions of unique beliefs?
It is because the religion of “logic” entraps people in host religions that those people have not chosen. Some are stuck there because they are afraid of being bickered at for being supposedly “wrong”. Something that the religion of “logic” imposes into ANY science or paradigm or religion as a value more important than “love”.
The more beliefs people choose to make or belong to the merrier. Because ideally a world of nine billion happy beliefs, a belief for each individual’s own preference, would be healing. What this looks like is each person finding their OWN WAY of BEING in life. Which could be an Atheist way or scientism way or a Jesus way or a Buddha way or a Krishna way or a Quaker way or a tossed salad medely of many beliefs.
Some people want the traditional ways, even the psychiatry way. And some individuals want the holistic way.
If it is for you to judge then perhaps you are unwittingly in the religion of “logic”. Knowing what’s best for someone.
There is integrity in allowing space for “doubt” that you truly know anyone at all.
People may champ at the bit and say “leave my free choice to be logical alone!”.
I am not talking about “logic” so much as the religion or global cult of “logic”. You can have it. That is fine. I do not want it.
I prefer my “free choices” to be illogical, mad, and pleasantly schizophrenic.
Report comment
I agree with Bob that psychiatry needs to be abolished and with many of his points along the way. I am uncomfortable with, and disagree with, framing discussion of psychiatric drugs and their effects in terms of treatment for illnesses.
Abolishing psychiatry, even understood as removing it from authority in any domain of life, requires us to acknowledge that there is no reason to medicalize our personalities, thoughts, perceptions or emotions and that psychiatric diagnoses are value judgments in a symbol system that is only way to think about ourselves. Intentional Peer Support training and practice (among many others) rejects the use of diagnosis and mental illness narratives and instead looks for plain language talk about what we’re feeling, seeing, thinking, how we react to someone else’s talk about their thoughts and feelings etc. Diagnosis creates distance and a false claim to an authoritative understanding of someone else’s inner and outer world. Peer support in general and other egalitarian and communitarian practices of support have to be based in mutual respect for each other’s self-knowledge and a perspective of solidarity that allows the supporter to empathize with a person’s needs at the moment and how they understand and go about meeting those needs. (See my book Reimagining Crisis Support also on this, which Irit Shimrat reviewed for MIA recently, the book’s website is https://www.reimaginingcrisissupport.org.)
Two additional points to make on Insel’s duplicity. First, while I get the reason for the headline it’s somewhat misleading and might lead people who don’t actually read this article to think Insel is calling for abolition and promote his book. Not sure what to do with that, but be careful in how you share this article for that reason.
Second, ‘biopsychosocial’ is the latest thing among those critical of psychiatry who don’t want to take an abolitionist stand. I don’t know how many MIA bloggers use it, or where it originated, but I first noticed it in the work of Dainius Puras in his term as UN Special Rapporteur on Health. It was one of his fudges but probably he also simply believed it – wanting to move psychiatry and health practitioners closer to a true social model in line with Convention on the Rights of Persons with Disabilities, but not wanting to give up the medicalization with all that has means – the diagnosis, the unproven and unprovable theory of chemical imbalance, the promotion of medications (drugs) as actual treatment (even if not cure), the authority of psychiatrists as central to any ‘mental health’ team or related supports – while giving more space to ‘psychological’ and ‘social’ or ‘psychosocial’.
It is axiomatic that any human experience has a biological component. To type this I am using the functions of my brain, my hands, heart and lungs and muscle and nerves. But to say that this is a biopsychosocial activity (as anything human would have to be) says nothing about anything being wrong with me and needing to be fixed. The medicalization of thoughts and emotions is not just a claim about human activity having a biological component which can be studied (that is called neurology) but a category error attributing differences in consciousness, communication and behavior to brain biology. It’s not a true hypothesis as it cannot be proven false, so it will come up again and again so long as anyone wants to promote it, there will always be something on the horizon that ‘looks promising’ if that’s what you’re looking for. There’s also inherent cultural, gender, class and personal bias both in aiming for an objectifying view of someone else’s mind and in how others’ minds are judged.
So again, until we’re ready to do true abolition of the authority of psychiatry in all these dimensions – including (which I take as a given but needs to be stated since it’s not yet done anywhere) absolute abolition of the power of involuntary holds/commitment and any treatment, services or support without explicit free and informed consent of the person concerned – everything will be bandaids that maintain the power inequality intact.
Report comment
Duplicate Comment.
Report comment
Dear Mr. Whitaker, You wrote an impressively researched article. Thank you also for publishing my article in MIA in July, 2020 titled, “A Self Help Version of EMDR May Make Healing From Trauma Easier”. When I first developed Se-REM and experienced client’s unprecedented reactions, I knew that this program could change Mental Health Delivery Worldwide. Your article makes a strong case that traditional drug therapies are counterproductive. Se-REM is a totally natural therapy using the brain’s own mechanism to heal. Yet, No One in an establishment position has given it a chance, even experimentally. One client wrote to say it is a “genius creation”, another therapist wrote to say it is “astonishlngly therapuetic”, another wrote to say I should be given an award. Others merely report that it changed their lives. It takes a lot of time and effort to write your extensively researched article that is a justfiable criticism of the system. But, consider being an advocate for something that could change all of mental health. It is the anti-medication model that you might help replace our current system. The following is a telling of a recent experience with the program. Hello David! I’ve been thinking SO much these past weeks in writing back to you and sending my testimonial, so I’m super glad that you’ve reached out to me 🙂
I’m from Argentina, South America, so I speak Spanish but hope my feedback is clear enough (and anyway I believe my English is very good hehe).
So, David, how can I really say THANK YOU from the depths of my heart for what you’ve done. My life is improving in so many ways. Take a cup of coffee or your preferred beverage because I’m going to tell the full story (when we clear trauma, our inner voice starts to speak more and more unapologetically and from love):
I found Se-REM as a result of my internet research on trauma and bilateral stimulation, because I’ve been working with a therapist and see some really good results, and this year I’ve been learning so much on trauma and what actually works, and let me tell you (I know you know), your stuff WORKS.
My situation was (and I’m still working on it): anxiety, had anxiety attacks (or panic) and ptsd. My nervous system tends to dysregulate and I feel extremely sensitive and even psychic or “empath” to the extreme in those moments.
I listened to the full audio one time for the first 4 days, and yes, how important it is to have a GOOD CRY, just me and my inner child being ourselves. I highlight this because it is very good to be able to cry with no one else more than my own awareness and love witnessing.
One of the main things that I’ve been able to develop with your audio is a high awareness of the Conscious and Subconscious minds working together. In the second part (when you instruct us to be there as adults for our inner childs), I feel like the brain starts to integrate so quickly, that I feel my inner child and ME (the conscious mind) melting into ONE. This is one of the greatest gifts and lessons that your work enables to actually DO (that phrase we all know “LOVE YOURSELF” is actually and technically this (again I know you know): the conscious holding all the emotion of the subconscious and letting it unfold the magic behind it, the truth of who we are).
There’s one thing I would like to appreciate too: the specific music you’ve chosen for each part of the process. As a music lover, even though I appreciate classical music but I don’t use to listen to it, your selection is just outstanding, I felt like it speaks about your own loving soul, who you are, and what you know you are meant to do on Earth, this is my particular feeling.
Each time I did a session, I was able to release a lot of stress and integrate my psyche more and more. I did it recalling memories and also just focusing on how I was feeling or a certain recurring thought, in all of the cases it worked wonders. I also added a bit of the tools I have in my personal kit to keep reprocessing (EFT and other forms of bilateral stimulation called “One Eye at a Time”).
I believe deeply David, that your work has to be spread around the world, not only in English but in as many languages as possible. What you’ve done is amazing. I’m already talking about your page when I speak to other people on Facebook groups, I feel like I want to scream to the world “People! This is what you are craving for!!!”.
This work is so needed, so required, there’s so much healing to the nervous system of the collective that needs to be done, that your tool / work could help so much, because this is the foundation where all true wellbeing and creation can be done.
Thank you, thank you, thank you David!
Any other questions, I’m here to collaborate!!!
Julia
From Buenos Aires, Argentina
Report comment
If the scientific narrative that is to be found in the research literature were told to the public, of drugs that don’t fix chemical imbalances but rather induce them, and that researchers have pointed to that drug effect as a likely reason that that the medications increase the risk that a person will become chronically ill and functionally impaired over the long-term, then psychiatry would have to completely reorganize its care.
This is the bridge that psychiatry, as a guild, cannot cross. The prescribing of drugs is psychiatry’s primary therapeutic act, and if its drugs cause long-term harm, then what would the profession do? The profession needs to keep this history out of sight, even to itself, and so it is not presented in psychiatric textbooks, or in continuing medical education seminars. By keeping this history hidden, the field is not just breaking its compact with the public, but with itself—with every prescriber and all those who enter the field.”
I finished reading Adam Stern’s memoir Committed about becoming a Harvard trained psychiatrist. Like Insel in Robert Whitaker’s review, Stern sticks with his guild. Stern is forthright in some regards. He admits that interns screw up generally, though he never admits interns screw up involuntary admissions. He wonders if the whole profession isn’t a sham, but he ends up supporting psychiatry, his ego and his profession. He never takes on the efficacy of drugs. He mentions the harms they cause in one sentence without reflection. In too many places he sounds like he’s trying to land a job writing a television show about the care shown by his field.
Psychiatry won’t be torn down, just like Christianity does not realize that if a character named Jesus showed up with a god story, he would risk being involuntarily detained.
(Psychiatry and Christianity are disastrously related for me, in my story.)
Psych drugs induce chemical imbalance and people do not rise from the dead 33 years after virgin birth. But the truth is outdated, inconvenient. Too many moving parts. Too many people make money and find acclaim.
But those dominant and corrupted will protect their own, even if it means lying and worse. Psychiatry and western religion are likely with us permanently, flawed as they are.
(As a victim of criminal Catholic psychiatry, I’m also finally reading Margaret Atwood’s The Handmaid’s Tale.)
Report comment
Psychiatry is its own religion. It is completely unrelated to any other religion. It has created its own rituals and sacraments. It may have borrowed from other religions here and there. Some have borrowed from Buddhism and tried to manipulate Buddhist principles for alleged therapeutic reasons, but psychiatry is still its own religion. There is no other religion like it on Earth for it denigrates other religions and hides so many truths and facts from people, they suffer. Psychiatry is its own religion. Thank you.
Report comment
Thank you so much for this incisive article – zowie! Well done!
“… one could have hoped that Insel, writing as the former director of the NIMH, would have dared to cross this bridge of no return.”
One could indeed have hoped!
Okay, now it’s time to forward the link to everyone I know 🙂
Report comment
Another study that reveals the inefficacy of medication is the Consumer Reports study that showed that psychotherapy is generally helpful. That study found no difference between psychotherapy with and without medication. If, in fact, medication helps SOME people SOME of the time (which is generally accepted), the only way for there to be no difference between the psychotherapy groups with and without meds is for there to be at least as many people harmed by drugs as helped (so that the averages for the two groups as a whole are the same). See https://www.researchgate.net/publication/247404811_The_effectiveness_of_medication_The_Consumer_Reports_study
Report comment
Amazing! That a study would actually be published in such a “mainstream magazine” as “Consumer Reports” questioning the effectiveness of the “gold standard” of psychiatric treatment. This is especially so as each and every day they step up the noise on the news and other media to promote “mental health/illness” or basically to entice “us” or those we love into the psychiatric office, probably to be compelled to take these drugs. Thank you.
Report comment
“If, in fact, medication helps SOME people SOME of the time (which is generally accepted), the only way for there to be no difference between the psychotherapy groups with and without meds is for there to be at least as many people harmed by drugs as helped (so that the averages for the two groups as a whole are the same).”
This would show up in higher standard deviations of symptom severity in the treatment group vs the placebo one. Now those are rarely given, but from what I’ve seen this is not the case.
Report comment
I could say that mental illness is on the rise because life is less secure than it was. I could say that it is on the rise because in the past people were ashamed of mentioning that they had it. I could say that the lingo and jargon of psychotherapy has seeped into the very cradle as a nursery rhyme we are all brought up with and so to “fit in” we have now bicker in that psychotherapeutic dialect rather than a spiritual one. I could say that bodies are teeming with chemicals and that evolution depends on some of them going awry or imbalanced. I could say that nothing can ever achieve balance without the finicky finessing adjustments brought about by imbalance and that no bodily hormone or chemical is a “fixed” static ornament of accomplishment. Bodies are always both disorganized and organized. Our very spiral galaxy is both diluting into fragmentation and organizing into handome clumps called stars as it spins and spins. Our bodies are perpetually spinning. Ditto our minds. It seems dim to suggest that balance and imbalance at the quantum level can be disentangled. They are bride and groom.
I could argue in this manner from my lowly schizophrenic hearth, shuffle papers by guttering candle light. But what would I be doing? I would simply be trying to make a faith that seems solidified by “logical rhetoric” be even more wearyingly “logical”, and no longer a lovely harmonious faith. A faith is invariably where birds of a feather flock together. There is nothing untoward in that. But when a faith starts telling rare unique individuals that they cannot join unless they “be right” in a “logical” fashion and become “different” or “change” then something else is going on beyond it just being a flock or a faith. I call it bullying.
It occurred in the faith of psychiatry but regrettably it is now occurring in opposing faiths to it.
This is NOT acceptance of the human being’s “freedom of choice” to be who they “feel” they are!
Yes, I have a chemical imbalance and it causes my schizophrenia. This is my individual understanding for “me”. It does not “have to” be obeying anyone else’s “logic”, it can be my from my “free choice” to be “illogical” and preferring to go with the flow of my “feelings” and what “feels” real “to me”. I do not welcome being judged for having the “wrong” or unpopular “feeling”. My “feelings” are entirely “my own”, as are my understandings of “my chemical balances and imbalances”. It is not for any ex-psychiatrist or antipsychistrist to tell me what “my feelings” should be or what my opinions should have been in the past or should now be. A psychiatrist has never had a month of hallucinations such as I have endured for over two decades so how can “any” besuited smart “logical” person quite unaquainted with having in their head my hallucinations say they know all about my schizophrenia? How can that credential lauded person who is not experiencing my exact interior experiences of hallucination torment and who is a stranger to my own feelings ever call my knowing I have schizophenia “wrong”? Data and research and “consensus opinion” have always been bickering and qualifying and quantifying over a hypothetical standard humanoid who IS NOT ME.
Both psychiatry and antipsychiatry hate me because I am “free” of both. Neither owns me with their “consensus opinion” and their argy bargy “reasoning”. My “feelings” are NOT reason. My inner being is “unreasonable” and this helps me feel well. In my “unreasonable” and “unapologetic” knowing for myself that I do have a chemical imbalance and that I am schizophrenic and that I do find it an experience of abject illness…knowing it is a chemical imbalance in me helps “me” feel a bit better.
Whatever makes me “feel better” is what people ought to cheerfully want for me. Even if it is not what makes them feel better. We must all agree on only one thing, to celebrate our each unique individual “free choices” that make us alone “feel better”. But sadly what makes the “reasoners” better is proving that they are “right”. That requires making “the other” obey the assumption based on “logic” that they are “wrong”.
It is how conquistadors imbalance a native population who have their own “freely chosen” way of knowing who they are and how they as unique individuals prefer living.
Such bullying of anyone simply has to stop!
There are no “wrong” feelings. And that includes how I feel about my illness. Or even that my “feelings” conclude it to be an illness. Yet people in both psychiatry and antipsychiatry want to establish power over me and tell me they are “right” about “me”. Me! A person they have never met.
Being “right” is not being “love”.
Being “right” about strangers, as if they are narrow, textbook standard researched humanoids, is the biggest sickness the globe is facing.
So, with weariness of soul I choose to triumphantly have people call me “wrong”…..in my going with the flow of my own “feelings” and my own knowing that I actually DO have a chemical imbalance. I may be one in a billion who believes this. I may be THE ONLY SCHIZOPHRENIC who ever was born. It matters not to me if this turns out to be the case. I have zero wish to have anyone else accompany me in my lowly schizophrenic shepherd hut. I am NOT RESPONSIBLE for the debacle of bad drug treatments. Nor am I responsible for the way society has been lambasting schizophrenics for being “wrong” in a differently predictable way. To most “logic” driven civilizations the “feeling” creatures in the human stock will always be “wrong” simply because they live by their honest gut “feelings” and “intuitions” and have the audacity to believe them.
My “free choice” cannot be controlled.
If your “free choice” is to declare that you do not have a chemical imbalance then I fully and lovingly support your choice for you. I have no wish to change you or your choice since your choice will be dramatically different in how it makes you feel better.
For a century theologians, who were a bit like psychiatrists, could not shake off the “logic” they arrived at that had them pompously and “factually” declaring that female foetuses developed a month or so AFTER male foetuses. You could say that those priests of “reason” had more than “eighty years” to fathom that female foetuses and male foetuses develop in tandem, yet it seems science needs to brush under the carpet all impeding traces of the former emblazoned “facts” of science to surge forward in leaps and bounds. I gather we still do not “factually” know for certain the “cause” of the brain disease of epilepsy. It used to be called “falling down sickness” but just because it was called that did not mean a shrugging off of its real devastating impact. People who felt they had seizures were STILL BELIEVED. God forbid but in those days it would have been a cruel abuse to call them a shivering liar, or a lazy entitled malingerer, or a person of sin avoiding the psychotherapeutic confession box.
I am told by my angels to come away from this website. There is a problem with the Hoover Dam.
Report comment
I support your right to be a schizophrenic who has a chemical imbalance. But I DO HOPE you know about HVN – Hearing Voices Network? It’s 100% peer-driven, and does very good work. And I hope you keep commenting here. You do have a unique voice, which I find refreshing, challenging, & rewarding. Your perspective is valid & needed.
Report comment
Bradford, I may use the word you later in another context but I do not mean specifically you. I just mean generically everyone as eight billion yous.
Bradford, I am impressed by your tolerance of me. I mean it sincerely. I was expecting a flung egg not a warm welcome.
The Hearing Voices Network is, from my own visits to it, a kind of a nice belief.
It is a beautiful accepting belief. I love it limitlessly.
It does what all beliefs ought to do, make you MORE YOU, not less you.
I don’t mean more you as in a textbook idea of what a perfect “fixed” standard humanoid should be like. I mean so very much you that you go home “unchanged”. You go home a complete mess.
But feeling heard.
It is very refreshing when a belief loves you enough to not want to ever change you.
That’s the magic.
Report comment
“DW”, yes, I support your right to believe that you hallucinate, and have schizophrenia. I’m sorry for your distress. While I disbelieve psychiatry, I believe that SOMETHING is going on inside your head. I want to help you be a whole, healthy, haappy person, whether you have schizophrenia, & hallucinate, or NOT. And, it is a process, not an event. Just because you hallucinate & have schizophrenia, so what?, – you still deserve the most whole, healthy, happy life possible. This is my belief. WE, ALL OF US, have some duty to help you, with you in charge of you. You tell US what you need, not the other way around!. I believe that your schizophrenia may be a form of, of part of, a spiritual awakening. Maybe. But I’m still glad you’re here! I find your comments challenging, AND rewarding!….
Report comment
Thanks, and, while he’s at it, ask him to abolish psychology as well.
Report comment
yes, frank, thanks!!!
Report comment
Abolish psychology? THANK YOU!
I second that motion!!!
Report comment
Covid-1984….largest PhRMA marketing & profit-taking campaign ever….
Report comment
We have to thank Robert Whittaker for his article. It is as usual, excellent. But perhaps, Thomas Insel doesn’t deserve such attention. I haven’t check Amazon to see if anyone is reading his book. I am thankful to Robert Whittaker because he hase helped to free so many from psychiatry. I am thankful, especially for his book, “Anatomy of an Epidemic” which virtually fell of the library shelf and into my hands just as I was realizing something was wrong with me and it was not the alleged mental illness, but the psychiatric drugs they had been prescribing me that I dutifully and obediently took; that actually made me sick. But now today, I also realize that if I want to live free and live happy that I must forgive and forget how psychiatry treated me. There is much more to my life story and psychiatry seemed to not want to see that— for a lot of reasons. I have learned, maybe through trial and error that it is much better to light a candle in the darkness than rage until the darkness consumes you. Thank you.
Report comment
Well done Robert.
The word “therapeutic” in psychiatric practice is a misnomer.
People get feeling better by luck, not by the neurotoxins. There is no proof that
the drug had anything to do with someone feeling “better”.
I also have seen many on AD’s and NOT ONE is “better”. And many died early.
Report comment
I am glad Robert wrote his book. I gave up antipsychotics before I ever knew of it. Many do so since the drugs side effects are hard to bear.
I am NOT however in alignment or groupthink with the binning of language. Even the words used in traditional diagnosis are not something I think need to change AS A CHOICE. By this I mean that if a person wants to call their illness by a traditional diagnosis I see no problem with it.
The diagnosis of schizophrenia is one I use FOR ME because it does help ME make sense of MY anguish. Whatever helps me should be fine for other people to permit, if not then they are telling ME how to think.
In a similar light I feel that for me being schizophrenic is part of a unique culture. I believe all cultures HAVE A FREE RIGHT to not be told how to think.
Antipsychiatry has sometimes seemed to me to be a faith or culture, with its own values and innovations.
I believe outsiders can become jealous of any culture and seek to undermine it.
I see this as happening to my culture of schizophrenia or even just any madness.
It is true that there are aspects of being schizophrenic that have had bad treatment, just as native tribal groups have had bad treatment. But if native groups are supposed cease being who they want to be and cease their language and lore in order to stop bad treatment being given to them THEN THAT IS ALSO BAD TREATMENT of their preferred culture.
It is a jealous outsiderish attempt to nullify the expressiveness and language and poetry and art and genious inventiveness and creativity and history of a peoples who through no fault of their own have been victimized again and again and again.
It is not called victimizing but is rather called “normalizing”. And just as the aboriginal children were forced into “normal” clothes to become puppets on strings for the latest politics or paradigm so too is the unashamedly schizophrenic individual argued out of their words and clothes and poems and dreams.
They are told this “normalizing” is “for their own good”. The schizophrenic hears it from psychiatry and antipsychiaty. The missionary and the general.
Schizophrenia is a culture. It keeps an archive all of its own. Van Gogh, Leonora Carrington, Phillip Dick, and the billions of street bards and homeless gurus and philosophers and mathematicians. I know of no person who has not been inspired by meeting a schizophrenic and immersing themselves in that culture.
The schizophrenic has always been the beggar at the banquet. Told what to say. Told how to think. Told what to read. Told to refrain from owning their own schizophrenic “free choices”.
Meanwhile their words and rhymes and poems and visions and wet oil paintings are continuing to be sacked from open windows, carted off in wheel barrows, to decorate the dens of puppets on strings.
I know what it is.
It is cultural vandalism.
It is cultural theft!
Report comment
It’s interesting to me to consider your identification with schizophrenia (diagnosis) as a culture and a personal choice.
It gets complicated when the same words are used in many different ways. I can entirely accept your relating to schizophrenia as a word to describe your anguish. Not sure what I think about your ascribing that label to others like Van Gogh, did he similarly identify with schizophrenia?
Also there is schizophrenia as a diagnosis given by psychiatrists or ascribed by someone else generally (which I’d argue is an act of appropriation in itself) and schizophrenia as a word that people might claim for themselves as a culture. (Like mad.)
BTW, I was given that label once. It has at times interested me to speculate as to what they say in me that might have merited it, but in the end I would rather just tell my story or not, in my own ways. It’s both that ‘schizophrenia’ even as a personal/cultural claim doesn’t work for me, and that ‘schizophrenia’ as a diagnosis is wielded to terrorize and scapegoat.
I appreciate the discussion.
Report comment
Tina, I think the expanding shuffled deck of comments has now put my earlier comment to someone else next to you, as if I am replying in that one. I am not. It gets like speed dating in the comments musical chairs realignment. So,
I entirely beg you to loathe your “schizophrenic” label. Throw it away. Or better yet spit in it like I used to do to my sister’s horse riding boots. I have no wish for you to ever call yourself anything I call myself.
That has always been my position. I am not for anyone having to be like me or like my choices. I just do not like when I meet a chorus of people telling me that I cannot like my choices. And although nobody overtly does, there is occasonally a sneering jibing denigration of my illness which I find ungracious in a website meant to value ALL. But I am not so much riled about that but riled on behalf of anyone who gets told they cannot be who they choose to be. In this regard I echo antipsychiatry. But by this token I am not happy at the way psychiatrists are lambasted for their choice to be who they want to be.
A CHOICE IS HARMLESS.
BULLYING is NOT.
I am all for people denigrating acts of bullying but I am aware that denigrating BY ITSELF can ALSO be a form of bullying. A form known to psychiatry’s murky past. I think antipsychiatry could go down a similar path to psychiatry if it does not let people CHOOSE their own destiny.
I believe MIA could do better if it became a belief. That way it could boldly say at the entrance gates that this is what is believed and this is the type of language used and these are the kinds of healing offered. That clarity would dilineate whose choices for themselves are NOT welcome.
Why that is not happening may be because the belief needs the other to be a source of othering so that group bonding can grow tighter. But this implies there may have been a problem with the bonding before hand, if there is a need to other or unwelcome outsiders. If the “US” cannot “feel” like an “US” without a “THEM” to give its boundary shape then it does not say much for the “US”.
I was just offering my impressions.
But mostly, my main endeavour has been to enjoy the role of scapegoat since I expect we shall ALL feel like one in the future, where for a while at least, nobodies “free choice” will be granted unless it concurs with a new regime.
That dictator regime is on the way.
It will demand that everyone hate everyone or be hated by everyone.
This is why my message has often been that…
ONLY LOVE WILL SET US FREE.
Report comment
Was just a smidgen grumpy when I wrote that.
I get a bit humourless at seeing too many arguments put forward against the illness I have by those who have never had it.
All this hunting for the evidence and then the evidence about the evidence and then the evidence hidden in the evidence and then the evidence that once was and then the evidence that will be soon, as soon as the brain scans plop from the photocopy machine and match the evidence about the liar and then evidence about the truther and all the “right” “wrong” “right” “wrong” “right” “wrong” about my hellish illness that at least once a day has me wanting to turn my brain into a tunnel of light….
it is not helping ME.
I truly do not care that it does not.
I care about my schizophrenic SISTERS and BROTHERS who KNOW that their hallucinations are an illness and they KNOW hallucinations are not mere “trauma”.
For THOSE schizophrenic SISTERS and BROTHERS being ill ought not to immediately mean “treatment”.
It ought to mean love.
By getting rid of the idea of illness in order to get rid of “treatment” may be grand for some, maybe even particular people who want to slip back into “normalcy” in the “consensus opinon” landscape.
But I KNOW schizophrenia is such a horrible illness it cannot be “fixed” just by calling it an “idea” and overturning that idea for a newly championed idea.
It would be like telling any people with a congenital syndrome that it was all in their head.
Report comment
Sorry, “DW”, can’t agree here. Both your schizophrenia, and your halucinations, are subjective, and only provable by your word alone. That is NOT the case with a congenital dsability, which does have objective, physical manifestations. Trauma may be necessary to explain your schizophrenia, but it not sufficient. If the word “schizophrenia” had not been invented, what would you call it? And, have you heard of, or worked with, HVN, – the Hearing Voices Network?
Report comment
I disagree with Bradford. Even the feeling of itching may not be provable by outward, objective, physical manifestation (like a pimple). A person could be faking the feeling of itching by scratching his hand. But that doesn’t tell you whether he’s experiencing the feeling or not.
A person who is hallucinating could be doing a myriad of things. Speaking to a non-existent figure (though people with no hallucinations also do this when they recollect traumatic conversations with people in the past), he could be followings the commands of voices which tell him to drink poison (though a person could actually fake it, which is rare). All sorts of things.
A person can call this schizophrenia or simply state, if they are cognizant of it, that they see and hear things that aren’t there. But dismissing the reality of it in all cases is simply harsh, untrue and invalidates the real pain of what people go through.
Report comment
https://youtu.be/0NiXgKdxezo
This song is my thank you to you Registeredforthis, and to Richard and Rebel and Steve and Tina and Sam and L.e Cox and Bradford and Joshua and everyone everyone everyone. All of ya.
Report comment
I’m NOT “dismissing the reality” of anything, or anyone. I’m simply saying that both an itch, and so-called “schizophrenia”, are SUBJECTIVE experiences. As are hallucinations. Daiphanous Weeping says she has schizophrenia, & hallucinates. I accept her belief as valid for her. I believe that she believes it herself. I accept, and support, BOTH HER, and her belief. If she’s happy, then I’m happy. And if she’s not happy, and wants help to change, I will do what I can to help, if asked. I do not have to believe in so-called “schizophrenia” myself. But, I respect, value, and appreciate DW, AND her subjective experience. Are you so sure you disagree with me?
Report comment
I politely disagree with both Bradford and registerforthissite. I do not think that hallucinations and schizophrenia are subjective as Bradford states. At the very least, psychiatric drugs can cause these to occur and that is not subjective. It is real. Additionally, other drugs and toxic substances can cause this. There may be other causes too, so I do to think they are necessarily subjective. Like all alleged diagnoses of mental illnesses diagnoses, whether or not schizophrenia can and should be debated. I am wondering if many times when a person is diagnosed with schizophrenia, they may actually have another condition which is not addressed. I would be unable to say if every person diagnosed with schizophrenia would fall into this group.
As far as “faking itching.” As someone who has numerous allergies that cause me to itch, you cannot fake itching. Now, sometimes itching can be caused by a stressful situation. Sometimes, drugs and other toxins can cause itching. when I was taking the prescribed psychiatric drugs, I had itching both inside my body and brain and on the skin of my body. My brain also felt raw inside. Now, I am aware that according to those who study the brain, one cannot experience “actual feelings” in the brain. However, I checked with others who were taking similar drugs and they experience similar things. I consider all this as real as the sun that shines every day. Now when I did stop the psychiatric drugs, the raw feeling inside my brain and the itching inside my brain and body stopped. However, since I am prone to other allergic reactions to other things, that type of itching can continue if in contact with something that provokes an allergic reaction and thus has never stopped. And it is not ever faked! Thank you.
Report comment
@rebel: Nothing that I said contradicts anything you said. Of course, there are drugs that cause hallucinations. This happens with psych. drugs sometimes. But we are not talking about drug induced hallucinations.
Also, you can absolutely fake itching. You can do it right now by scratching your hand for no reason and lying to the person beside you that your body is itching a lot.
What you can’t fake is the feeling of being itchy, which is the distinction I made in my earlier post. That is something that lies within your own self. You can’t will your body into thinking “make me feel itchy now” and “fake it” that way.
P.S. There are psych. drugs that also cause the urge to itch.
Report comment
DW
Thank you for that video.
I have now discovered another great singer/songwriter in Ane Brun.
Richard
Report comment
rebel, you’re confused. “Subjective” does NOT mean “not real”. Hallucinations are subjectively real to the person experiencing them, but not objectively real to anybody else….keep thinking. And commenting!
Report comment
And, I say it again; an “itch” is NOT subjective; unless it is used colloquially, such as the proverbial “seven-year itch” or I have an “itch” to do something such as a desire to go visit the Grand Canyon or whatever. An “itch” is real; but then, so is the imagination. One’s imagination (at least for those so pre-disposed is a real as reality-perhaps more real.) The actual problem is that we have some who do not take the imagination seriously or those who have the gift of an imagination seriously. Yes, some are psychiatrists and diagnose people incorrectly based on their imaginations; but they are not necessarily psychiatrists who “diagnose.” Many are just “regular people” who don’t understand and thus judge, criticize and bully. And some do seem to get on that “bandwagon” with the psychiatrists. However, the ITCH is REAL; the IMAGINATION is REAL. Sadly, it only becomes subjective if there might be some type of judgement involved. I doubt this is happening on this site by anyone. But I just wanted to clarify about both itches and the imagination. Thank you.
Report comment
Dear Mr Whitaker,
Thank you very much for fighting a hopeless case. Why can’t your response be published in The New York Times? The Washington Post? (rhetorically angry)Why is this lily livered horrible little careerist toad allowed to whitewash his profession’s gigantic ****-up.
So the ex chief psychiatrist at large has written a book using one of the current wellness buzzwords ‘Healing’ while burying research that shows the damage caused by psychotropic drugs.
He asserts that the ‘drugs work’ while apparently providing no hard evidence for that assertion. This books appears to be written in typical faux wise and faux benign psychiatric patter. I have doubt that it will be widely published across the world. Mr Insel or whatever academic title has been awarded to him will be interviewed I have no doubt on the main media channels.
People who are ignorant of the drugs will continue to be prescribed them voluntarily or not and will continue to have their health destroyed and few will believe them when that happens. It will be a continuation of ‘you had a relapse because you went off your meds you naughty, irresponsible person’.
The information is not getting out about this because of people like Insel. The marketing department at those pharma companies have limitless money to pay lots of social influencers to market their pills to the next generation. What is happening is an insidious, slow and violent assault on unsuspecting and vulnerable people all over the world by an industry that wants power at all costs. It is the very apotheosis of inhumanity and most tragically it’s an institution to which vulnerable people turn when they are looking for humanity because they are suffering.
The words from the Scottish play sum it up for me ‘fair is foul and foul is fair’.
I had hopes that Insel was going to turn but he chose power and having a legacy instead. When he’s dead some Ivy League university will probably have his face cast in bronze and plonked outside some medical faculty. The world does not have a dystopian future – it already exists in the here and now.
Report comment
maedhbh: How can I possibly AGREE MORE WITH YOU?…. PhRMA, and the pseudoscience lies of psychiatry, are 2 Armies attacking America, and the Poeople of Planet Earth, waging a form of CHEMICAL WARFARE against a civilian population. PhRMA & psychiatry are ENEMIES of the PEOPLE. They are inhuman, inhumane, and EVIL. Yes, psychiatry is EVIL. It IS A WAR….
PEOPLE ARE DYING, an average of 25 years sooner than they would otherwise, without PhRMA & psychiatry & psych drugs. I’m not exaggerating here, or being metaphorical. I’m speaking REALITY. WHAT IT IS. PhRMA, & psychiatry, are killing people for profit….
PHRMA & PSYCHIATRY ARE KILLING PEOPLE FOR PROFIT. And schadenfreude.
Go ahead, somebody, anybody? Prove me wrong? You can’t…..
But go ahead and try. I dare you! As for me? MOLON LABBE, Baby, Molon Labbe…..
Report comment
maedhbh says, “The world does not have a dystopian future – it already exists in the here and now.”
This is exactly what Dr. Insel and his mainstream psychiatry has created – a dystopia.
I see Insel’s book as a desperate attempt to continue controlling the narrative, while deflecting attention away from himself and mainstream psychiatry. The book’s an absurd effort at putting a good face on mainstream psychiatry’s categorical failures.
But you gotta hand it to the guy – he’s turned out to be quite the pitchman, as he’s using the bully pulpit for all it’s worth.
Report comment
What is Dr. Insel’s book?
A 336-page ad for the drug companies –
Report comment
Birdsong,
Thanks – ‘desperate attempt to control the narrative’ – I think you’re right there.
People like him don’t get to such exalted heights though without being adept at controlling the narrative.
Maedhbh
Report comment
Thank you maedhbh.
You say, “People like him don’t get to such exalted heights without being adept at controlling the narrative”. How right you are. It’s why I consider mainstream psychiatry to essentially be little more than a con game.
And Insel’s exalted status has certainly gone to his head.
Report comment
maedhbh quotes, “fair is foul and foul is fair” –
Now THAT’S a quote for the ages – AND mainstream psychiatry –
I think these days it’s called “gaslighting” –
maedhbh also says, “…(Insel) chose power and having a legacy instead. When he’s dead some Ivy League university will probably have his face cast in bronze and plonked outside some medical facility”.
No doubt – but in the meantime, he might try heading his own School of Public Relations (with a focus on mainstream psychiatry) –
Report comment
Birdsong, I hope you know the TRUE STORY of Freud’s nephew, Edward Bernays?….
He’s considered to be the “Father of Public Relations”, or some crap like that. Really….
Until you get to a certain level, a lot of stuff really does sound like “conspiracy theory”….
But from DEEP DOWN this bottomless rabbit hole, let me assure you all, that it is instead, CONSPIRACY FACTS. The world is fucked up by design. BY DESIGN….
The super-rich actually WANT the world to be fucked up….
In their sick & twisted minds, that’s how they maintain their power & control.
But, yes, the TRUTH CAN SET YOU FREE….
Insel is nothing more than a puppet, and a mouthpiece, for the Global Ruling Elites, and Global Banksters…. That’s a simple fact. But we all need to understand, if we are to survive….
Report comment
Bradford,
Thank you for informing me, as I didn’t know that Freud’s nephew, Edward Bernays, was the “Father of Public Relations”, but I’m not surprised that he was. It looks as though both were drawn to a similar line of work: the manipulation and distortion of people’s perceptions –
Report comment
The difficulties with the MadInAmerica forum are two fold.
Most of the blog authors are using it to try and legitimate the mental health system. Maybe not Psychitarty, drugs, and lobotomy, but they are still promiting the idea that people need Psychotherapy and that they need to disclose their affairs to a psychotherapist.
Secondly, there is no active component. There should be people standing at the entrances of every county hospital passing our flier that refer people to a web site, denouncing the entire mental health edifice, including psychotherapy and recovery groups.
This kind of protesting should be happening at the offices of psychotherapists, the Austism-Apsergers Doctors, and especially anyone who markets themselves with a Fix My Kid theme.
And most of the time the idea that someone is mentally ill starts in the family. There should be protest in front of every Social Services office.
And people should be told to never ever ingest psych drugs or disclose their affairs to any kind of a therapist, or to cooperate in any way at all.
Joshua
Report comment
I understand why you say what you say, but I definitely disagree. In my personal opinion, I do not necessarily agree that there should be “an active component” to MIA. I think MIA should be a teaching and clearinghouse website. It has helped many as they have tried to free themselves from psychiatry and its drugs. It has been a forum for those who are pro-psychiatry and anti-psychiatry. And this is very good. Whatever side one is on; if one cannot defend and debate it, then it must be reconsidered as to why you think/believe the way you do. I also do not think that MIA should be the catalyst for radicalism against these “establishments.” I, personally, would not feel comfortable standing outside social service offices with leaflets and the like. These kinds of actions sound good on the face; but can backfire in so many different ways. Also, in polite disagreement, I do definitely consider “autism/Asperger’s syndrome” as valid diagnoses. Many parents are dealing with their children who have these issues, and we need to respect their challenges. Finally, I am indebted to Robert Whittaker for the work he has done and providing this site with interesting and as forum in which we can voice our comments. This truly helps all of us heal. Thank you.
Report comment
I agree 100%, rebel….
THANK-YOU, ROBERT WHITAKER!….
20 or30 years ago, could you have imagined the last 20 or 30 years?….
30 years ago, I was still a PSYCH DRUG ZOMBIE!….
Report comment
“I think MIA should be a teaching and clearinghouse website.”
This does not work. Its like trying to tell slave owners that they should be more humane in how they treat their slaves. It is a contradiction in terms. All of us who passively tolerate the machinations of the mental health system are collaborators.
All anyone needs in order to free themselves from Psychiatry and Neurotoxins is the middle-finger.
But on MIA we debate back and forth with people who are using MIA to market their brand of mental health treatment.
Parents deal with issues that they create in their children because they have a need to find in their child the locus of original sin, and because they had children to give themselves an adult social status.
I think the idea that there can be dialog between the pro-mental health and the anti-mental health people is an illusion.
And Gavin Newsom’s Care Courts plan must be resisted by Any Means Necessary, and that starts by reaching out to those who will be targeted.
Joshua
Report comment
Please forgive me, but MIA bears no relation to slaveowners. It is imperfect, yes, as we are imperfect. I am sorry but debating anything is no illusion. And I know an illusion when I see one. Like I have said earlier, if we cannot debate any type of anti-psychiatry stance, then as they say, “we have no leg to stand on.” We must be willing to debate, and we must be willing to forgive those we believe have harmed us and ourselves, too. Otherwise, shallow thinking prevails, and we become the “laughingstock” of the world. We also need to stop making parents scapegoats for the problems of the world. I appreciate the work of MIA and Robert Whittaker. Thank you.
Report comment
Joshua said in his comment above, this: “Parents deal with issues that they create in their children because they have a need to find in their child the locus of original sin, and because they had children to give themselves an adult social status.”
My reply and correction:
First, Joshua, has ANY parent EVER “found the locus of original sin”? Much less in their children? What is the “original” “sin”? What is the copy, or duplicate sin? What is sin? How is it a “locus”, and not a “location”? How did it get there?
But I’m not trying to insult you gratuitously. I am making a point here. Dysfunctional parents raise dysfunctional children. Dysfunctional children grow up to be dysfunctional parents. Who then in turn raise dysfunctional children. Who then grow up to be dysfunctional parents who raise dysfunctional children. It is a generation-after-generation CYCLE of dysfunction. Over-intellectualizing is at best a distraction from the vital work of dismantling the GENOCIDE MACHINE of PhRMA & the pseudoscience of psychiatry.
You know we are on the same page regarding the pseudoscience FRAUD of psychiatry, Joshua, my friend, so thank-you for being so understanding! Parents have children because that is how Natural Biology and human reproduction works. It’s really that simple! That’s the way God, Our Creator, planned it! Or Mother Earth-Mother Nature, if you prefer, ladies.
(BTW, I prefer ladies, but this isn’t THAT kind of website, so I’ll shut up now….) LOL!
KEEP UP the GOOD WORK, Joshua!
Report comment
Rebel, the Mental Health System exists to rob people of their legitimacy. And so it is a situation comparable to people being held in a state of slavery.
So it was posted:
“I think MIA should be a teaching and clearinghouse website.”
Well that is comparable to having discussions with slave owners.
There is no reason that any of us should go along with any pro-psychiatry, pro-psychotherapy, pro-recovery, or pro-salvation seeking stance.
We don’t need to collaborate with the enslavers in anyway, and we should not.
We don’t need to go along with them just to give ourselves some illusory credibility. And IMHO this is the main problem with this MIA Forum, that it tries to gain credibility by collaborating with the abusers.
And the doctrine of forgiveness is one of the main ways the abuse is continued.
We have to be willing to stand up for unpopular minority opinions and not to ever cave in just to seek approval.
The industrial age’s middle-class is probably the first large group of people who have a choice in how they live. And one of the most basic choices is whether or not to have children.
But the middle-class tries to paint itself as being like those in a traditional society, not having such choices, in order to gain approval. The middle-class lives in Bad Faith. And the people who pay the cost of this are the children.
In Robert Whittaker’s books there is nothing whatsoever which endorses the idea of Psychotherapy or Recovery, or any kind of Mental Illness. His books are brave.
Joshua
Report comment
Although, I have been hurt and harmed by the psychiatric system, I would be extremely hesitant to compare it to slavery. People can and still do make choices whether to enter the system or not. Basically, with all due respect, I am completely uncomfortable with what you say in regard to this system. Like I said, I agree that it has harmed and hurt way too many people. I, too, have been harmed and hurt by this system. However, in my personal opinion, what you say in your posts is like adding insult to injury. I strongly believe that the absolute only way to free oneself of such a system is through forgiveness. Not only must we forgive those who we feel harmed us, but ourselves, also. I do realize that most of us have been harmed by those too difficult to forgive, whether in the psychiatric system or not. But, if we do not forgive the psychiatric systems or ourselves for getting involved in it, we will never be free. All of this is a learning experience for SPIRIT as we progress along the path of life. Thank you.
Report comment
Not everyone has a choice whether to participate in the system. But I agree, the analogy to slavery is a bit strained. It’s more like incarceration without cause and without recourse. Which is pretty freakin’ bad!
Report comment
I’ve been reading all the comments here and they’re all very impassioned and well written but I am beginning to wonder really about the point of all this passion. Who reads its? Is it impacting the mainstream? How many people look at the MIA website?
It is pretty clear that very few people are listening. We can write all we want here about the evils of the pharma/psychiatric complex but nothing is changing and the clinicians and scientists (who lets face are the only people that the public will listen to as they won’t listen to ‘mad’ people) who do speak out tend to be cast out.
Dr Peter Gotzsche – kicked out of Cockrane
Dr David Healy – delisted from a prominent academic post because of openly expressed views on SSRI’s.
Dr Terry Lynch – muzzled by lawyers; was part of the Vision for Change in Irish Mental Health Policy; but the government did not fund it and the service is worse than ever now.
Dr Steve Shipko – appears to have given up trying to help people withdraw from their meds as he realises his limitations in only operating out of an office and does not have the resources to help people come off in a hospital setting. I am paraphrasing from a video interview he did on the FB page of either the Medicating Normal page or Inner Compass Initiative last year.
In the UK – the picture is not as bleak – there is Dr Joanna Moncrieff who founded the Critical Psychiatric Network, Dr Sami Timini and Dr Mark Horowitz who seems to have single handedly managed to get the Royal College of Psychiatrists to finally recognise withdrawal.
In Ireland there is only one critical psychiatrist practicing that I am aware of – Dr Pat Bracken. Prof Ivor Browne who fought hard against the existing psychiatric power structure for years and founded the Institute of Psychosocial Medicine is now in his 90’s and retired.
I know there is a body of critical social workers, psychotherapists and psychologists out there many of them who publish on this site like Dr Gabor Maté, Dr John Read and Dr Lucy Johnstone but the psychiatric body look down on them as they’re lower down the medical hierarchy. Witness ex DSM IV editor Frances referring to psychologists such as those behind the Power Threat Meaning Framework as ‘brainless’ in an interview conducted last year with Dr Awais Aftab, a psychiatrist who advertises himself as a critical psychiatrist but is anything but ( I attach the link)
https://www.psychiatrictimes.com/view/moving-beyond-psychiatric-diagnosis-lucy-johnstone-psyd
Then there are the few survivors who have founded non profit organisations or who work alone as therapists – they are too scattered and too underfunded to make much of a difference. I check in on the Medicating Normal site on Facebook and the Inner Compass Initiative. They are fighting a brave battle but they’re not getting the viewers. One of their most charismatic members Angie Peacock recently stepped down from the Medicating Normal outreach team.
The Drop the Disorder Movement have more or less closed their Facebook page and just use it as a bulletin board to advertise niche online plays and their festival at which the same people seem to be invited to speak. I noticed that in the last few months that their Facebook page was active there was an increasing number of therapists from different schools using the FB page to advertise their services which became very depressing. They do invite survivors to participate in their festival but the only survivors that get on are those who have either recovered or are working as therapists or in the mental health area or those who have an artistic talent – they can sing, write poetry or plays. There isn’t much a place created for people who are powerless and stuck in the mental health system who can’t speak out because its’ their only income.
Then there are the sites from people that are coming of psychiatric drugs – these sites are genuinely helpful and supportive to people that are caught in the net of their drugs – Surviving Anti Depressants being as far as I am aware one of the oldest and most notable of those. They attract all types – people who have support in their lives to come off and people who are very alone and do not. The mentors and moderators do their best to help everyone but there are limits to who you can do for someone on a bulletin board. Adele Framer has published an article on what she has learnt in helping people to come off psychiatric drugs. What happens if Adele Framer decides that she and her mods who all work as volunteers can no longer commit to maintaining the board. It is a wonderful site but it has the fragility of all sites that are run by volunteers the same way that MIA relies on donations.
Pharmaceutical companies have bottomless pockets to affect public perceptions along with the psychiatric profession.
I recently attended a summit on Soteria House which I found depressing. Many of the people involved were involved in the original Soteria Houses – most were not funded so they shut. Many of the speakers were elderly. How many Soteria Houses are there in the world? There’s a few scattered throughout Europe and maybe one in Israel? None in the US as they didn’t get the funding. Yes I know all about the wonders of ‘Open Dialogue’ in Finland. Finland seems to be a kind of Shan gri la and thus not comparable to the rest of the world. They rid themselves of their homeless problem by housing everyone even those with severe addiction issues. Would that happen anywhere else in the world? Doubtful.
I wonder really what is the point? I’ve been through all the rage of look what was done to my life by this system but the truth is that no one except the echo chamber of fellow survivors and a few critical clinicians are really listening.
Report comment
I listened.
I am so impressed with your comment. I get sucked in to the wrangling and wrestling with concepts in articles and comments and it becomes to me a type of existence. Like I am one of those subterranian scowling, grunting, plodding, fuzzy grey creatures in the vintage Time Machine movie. Every so often I slam awake to this and ask myself…
“What the f am I doing?”.
It is a refreshing perplexing stepping back from the hypnotic tustling.
I believe humanity are ALL going through this existential question just now. I believe it is important for our species, on the eve of dire climate change, to collectively wonder at how easily we “miss the point”.
But back to the specifics in your comment. I sometimes view out of body narratives. Nearly all have a spread of similar themes. They go through a tunnel. They are accompanied by a couple of loving angel beings or astral figures. They arrive at a landscape of unspeakable peace. They meet an admired spiritual being who exudes endless love. They get to review their life a bit like looking at a love letter before putting it away. I am not sure if all of this happens to everyone. I am not sure if its nonsense or not. But I like the way many of these experiencers speak of being told that in life it is not the big things you do that are important; the planet huge campaigning things, the ambitions to be accomplished or solvent or admired or intellectual or mastermind a better society. It is the times when you gave up your seat for a stranger and YOU DID NOT HAVE TO.
It is the modest bestowing of compassion when you did not have to that gets you the equivallent nobel or oscar award in the hereafter.
So this idea that we ONLY matter if we sort out the mess the world is in is not why we are here. The world is a warzone stage for us to practice love in.
Love has to be a free choice though. Authentic. Or it is not love at all.
So I see the list of brave stellar striving ones in your comment and that is all good. But in some ways the world is the world is the world. Each of us is too tiny to make any vast change on it.
This can come as a disappointment.
Or a relief.
Report comment
Hi Daiphanous Weeping,
I did a reply to your comment a year ago but it wasn’t good enough to publish so I left it and I see you’ve stopped commenting now – great pity to see an original mind like yours leave the comments forum – that’s all I’m saying – the ‘modest bestowing of the compassion you did not get’ – beautifully put – I’m all out of compassion though.
Report comment
In regard of dear Rebel and dear Joshua. I ponder this. And say…
We need no doctrine of forgiveness.
We need no doctrine.
We need forgiveness.
Without it there is no we.
For the puzzled I mean everyone ought to see forgiveness as a personal free choice. Nobody should be telling an individual that they should forgive. Nobody should be telling an individual that they…
should not forgive.
To tell someone that they should forgive can be construed as an imposition. But equally to tell someone they should not forgive…is also an imposition.
You have a basic human right to not forgive someone you do not like.
You have a basic human right to forgive someone you do not like.
Freedom means both possibilities stay open to you.
Let’s always love freedom.
Report comment
Bradford, the quest that some parents have to find the locus of original sin in their child is an unending quest.
What Lloyd deMause wrote is that this is using the child as a poison container, and it goes back 1000s of years. I look specifically to the sacrifices of Isaac and the daughter of Jephthah as the archetypes.
The quest to find defect in one’s child can get quite extreme.
A compelling story too true to be able to even imagine:
https://www.amazon.com/Sickened-True-Story-Lost-Childhood/dp/0553381970
The middle-class is something which arose because of the industrial revolution. One of its characteristics is smaller families. But to be middle-class means to have adopted a reactionary identity. The middle-class is the first large group of people that has choices. But they don’t want choices, they want something to hide behind.
The middle-class does not have to have children. But most do because they want the social approval. They don’t want to have to take responsibility for creating their own values and choices. So they are not living up to their own values. They have children so that they can exploit them. And when you see that their is enmity between parent and child, this is always the reason for it.
What we erroneously call ~mental illness~, is merely the experience of not being at home in the world, or of not having a place in the world.
Specifically pertaining to the facetious mental illness ~schizophenia~, they say that one of its characteristics is a lack of social mapping. The supposedly ill person has not found their place in the world.
Well what you cause this?
For one thing we live in a pretty crazy world. But the more immediate cause is simply of having one’s affairs arranged from the very beginning by exploiters, by people who have been using you, rather than dealing with their own stuff.
So then when this starts to break down, often it is the parents who invoke the white coats, but not always. But the idea that there is something wrong with the child seems to always originate with the parents.
And our society makes redress and public vindication very difficult. All it really offers is an endless array of denial systems.
Thanks Bradford for the encouragement and I consider a discussion like this very constructive.
And Robert Whittaker has been very brave, nothing in his books ever talks about Psychotherapy, Healing, Recovery, Motivationalism, Forgiveness, or Salvation Seeking.
Joshua
Report comment
Joshua, I am sorry what you have written is so sad and so very and tragically wrong. As a child of middle-class parents, I am thankful to have been born and I am thankful for my parents. This is very important as I am the daughter of Vietnam Veteran. I know that they had both my sister and Ioutt of love. Love is the answer because it is rooted in Spirit. And yes, Diaphanous Weeping, no one can make another person forgive or do anything. However, in my opinion, forgiveness is the only true way to healing. But then no one can heal unless they truly want to heal. Thank you.
Report comment
Well said.
Report comment
The analogy to slavery comes simply because people have been continually exploited, and then lied to about it. There is no social support for coming to see this.
People now talk about “Dysfunctional Families”, this obscures the exploitation that is the Middle-Class Family because people are not living authentic lives, but instead have children so that they don’t have to deal with their own stuff.
And those who seem to have have survived with some residual awareness intact are those most likely to end up as fodder for the mental health system. It is like slavery because people are being made to believe that this is the state they deserve. Challenging this without getting into vastly more trouble is extremely difficult.
Joshua
Report comment
By making repeated raids into Maryland, Harriet Tubman was able to liberator over 700 slaves. What she said about this was, “I’d of been able to liberate a lot more if only they’d of known that they were slaves.”
Today the Middle-Class Family tracks people into Drug Use, Prisons, the Mental Health System, Homeless Shelters, Recovery Programs, and Salvation Churches. Most of the people still do not see that their is anything wrong with this.
Joshua
Report comment
With all due respect, if people need to be freed as you claim they do; we must first respect and not intervene in someone else’s life path. Each person must come to his or her own conclusion, shall I say, actually on every little and big thing. Second, if, like you said, people need to be freed, they will need a viable alternative to the above. In my personal opinion, unless the alternative shows people the “wonder of life and SPIRIT,” it will never sell and all those things you list will continue to be the least objectionable alternative to most people. If people are slaves to whatever you claim they are slaves to, they are slaves because of what’s on the inside, rather than the outside. Most people are slaves to themselves, if you choose to use those words. Most people are imprisoned not because of what’s out there, but what’s in there (as in their hearts, their spirits, souls, minds and bodies.) If people want to be freed, they must look within first and make that decision themselves. No one on this Earth can make that decision for them. Thank you.
Report comment
Nice response.
Report comment
Cont…To Maedhbh again, after my reply to you that begins “I listened”. I just want to say that I feel that the world is undergoing a process of rapid changes. Change for the better but for now it is experienced as deeply troubling since the changes bring “uncertainty”. And “uncertainty” agitates the anxious mind, that fragile chandelier that needs a secure holder. Everyone is jittery about the future. This makes tempers snappy which increases the jitters about the future. The changes are right throughout life and society so it feels bombarding and there is no confidence to found in anything or anyone. We are like worried lowing cattle unsure of each threatening unknown. Globally these changes are a good thing. Humanity will rise up out of this mess and chaos. Try to see it like a tea party. All the porcelain crockery is on the table that is bedecked with a fancy traditional tablecloth. A cup and saucer is the MIA campaign. A sugar bowl is the trans rights campaign. A teaspoon is the eco campain. A marmalade jar is the feminist campaign. A teapot is the anti-racism campaign. And so on and so forth. Lots of crucial, important, valuable, planet saving campaigns. They all individually think they are the only ones with the “answer”.
However, what most of them have as their difference is hardly huge. Infact most of the campaigns have IDENTICAL RHETORIC.
It is all about…
.the need for justice.
.the need for care.
.the need to have harms compensated.
.the need to create the world in a more loving way.
.the need to protect children.
.the need to be more environmentally considerate.
.the need to be free.
But the small “difference” comes accross to others as “wrong” or “unacceptable”.
This is the “logical” mind judging what is approved and right and what is beneath contempt.
The “logical” mind is not interested in harmony with “feelings”. To it “feelings” are a problem to be ordered and controlled and bossed.
Each campaign has the same wish list which is full of hopeful “feelings”. But when met with “logical” judgement externally, each campaign grows a veneer or shield of “logic”, like a cold suit of armour. It grows unwelcoming of the judgementally “logical” but does so by being just as “logical” and damning. Soon all the campaigns are both echoing the same wish list yet bickering over who deserves to see it manifest.
All throughout society this vortex of “logical” hateful speech soon ramps up. Then comes a “logical” crackdown on using any speech. Until nobody can speak to eachother.
I won’t make it a long comment but what I believe is going on is not to do with the bitter infighting or shouting between campaigns but rather that the table cloth is being pulled from under ALL campaigns and ALL if humanity. Like a tea party we are collectively just now temporarily experiencing a loss of control. A benefit in this is that we later fear a bit less what a little loss of control is within. I don’t mean we should all emote from dawn to dusk. I just mean the “balance” needs fine tuning between mind and heart. Because a problem for humans is their bullying need to control everything, even themselves. Fear of loss of control strikes at the way emotions are flows that are not always controllable.
Ironically when we feel all of our “feelings” we experience eventual “calm”.
Humanity is taking baby steps in learning where to find the “calm”….a particular depth of peace that comes not from “logic” but from being a big baby. Cleverness is all good and well but when it makes wars and bioviruses and hideous loveless inventions Earth becomes not as it ought to be. A more emotional response to our fellow humans and animals and plants is called for. We think that making posters and holding wooden conferences will do it. But we are too tiny and insignificant in our little enclosed campaigns. So we are given a new campaign from the Source. Our campaign is to love our emotions…
so that they will in turn love
everything else.
Report comment
Rebel,
“not intervene in someone else’s life path.”
Intervene in someone’s life path. Who does that? The Mental Health System, because it is an arm of the state.
And in CA, Governor Newsom is trying to set up special courts for this. We need to oppose this and be ready to resist it.
And of course people come to their own conclusions. But what have they been listening to?
Usually it is the rhetoric of Recovery, Therapy, and Mental Health Treatment. And usually this is coming from the family. This is where the idea of innate moral defect, the modern version of Original Sin, starts.
Viable alternative? Well once people are freed from idol worshiping, they will have the greatest of the human spirit and the wonders of the cosmos before them.
Yes, they are slaves because of what is on the inside. And how did it get there? Most of the time it has come from the family. Drugs, Alcohol, Born Again Christianity, and Psychiatric Medication.
Of course people need to make their own decisions. We need people who will decide and commit to opposing the Psychiatric System, and in general to opposing the idea of Original Sin.
Diaphanous,
Yes the world is changing and for the most part this is better. But there are still some serious problems, and the Mental Health System is one of them.
Various worthy and important campaigns you speak of, but all efforts are sabotaged when people believe in the Mental Health System.
People are tracked into Mental Health, Prison’s, Homeless Shelters, Recovery and Motivational Programs, Psychotherapy, and into Salvation Seeking. Usually this is coming from the family, but it is also highly influenced by the ways that government authority is behind it.
Joshua
Report comment
With all due respect, and very ironically, the more you state what you state, and in the way you state it, the more all those “things” you list seem more and more appealing and more and more the correct answer to all the problems. I am sorry to say this, but sadly, your very arguments basically backfire— if anyone would even have a chance to agree with you, your arguments make this completely impossible. Thank you.
Report comment
Rebel, I am not sure if I am understanding your real meaning. But suffice to say, we need to eradicate the entire mental health system, and we need to be educating people about it so that they do not succumb to it.
https://www.madinamerica.com/2022/04/observation-room/#comment-195987
https://www.madinamerica.com/2022/04/observation-room/#comment-196026
Are you opposing this?
Joshua
Report comment
I hesitate eradicating anything without a viable alternative. Actually, as much as I don’t like the mental health care system, totally eradicating at present is an impossibility. As a nation we have tried to eradicate both Nazism and Communism, but these ideologies still persist. Many people now consider our present mental health care system to be almost like a religion which could be considered an ideology. The word and the concept itself of ideology is basically neutral; however, there are ideologies that are negative and even evil and there are those that are good and wonderful. But, whether good or evil, they are impossible to eradicate. I can guarantee you that if we do eradicate the present mental health system, it will pop up in another form. Sadly, we have no way to discern at this time if it will be more evil than good or the opposite. Right now, like I said, I do not have an answer to this problem, but I do think that eradication of the mental health system will probably and sadly prove to be a total disaster. In my personal opinion, I believe that each one of us would be better to tend our own unique personal gardens that try to be a gardener for the whole world. And slowly, but surely, there will be more gardens of positivity. It has been said it is better to light a candle in the darkness than curse the darkness. Our best bet is to light that candle and let psychiatry, etc. fall on its face in its own due time, which will probably, unfortunately outlast our lifetimes. Sometimes, I don’t necessarily like this way, but it is more workable. My first job out of college was as corrections officer. It worked with individual criminals and will work with psychiatry, too. It is never good to rush headlong into areas where angels fear to tread. Thank you.
Report comment
The viable alternative to the mental health system is the middle finger.
The far right still exists and the mental health system is a core component of it.
“Many people now consider our present mental health care system to be almost like a religion which could be considered an ideology.”
YES! and this is at the core of the problem.
If everyone stops cooperating with the mental health system, then it is eradicated. If we band together we can stop the forced treatments. And if we stop looking to mental health explanations to delegitimate people, then these lose their force.
“better to tend our own unique personal gardens”
This is the standard argument of the Right. The Born Again Movement runs on this, and Psychotherapy, Recovery, and Motivationalism do as well. It was how religion supported slavery in the South East, and it was how they opposed the Civil Rights Movement 100 years later.
But there is no basis for it.
People felt that it was wrong to oppose slavery. People like Stephen Douglas of Illinois said that it would die out on its own because the West had a different soil type than the South East.
The Right is very strong in America today, and in it’s Neoliberal Form, the Mental Heath System is at its core.
CA Governor Gavin Newsom is setting up special courts to force the unhoused into Mental Health treatment. In CA they can already arrest someone who is breaking no law under 5150.
Joshua
Report comment
With all due respect, politically, there is a mixing of political metaphors in your comments, as Gavin Newsome is very liberal and is the nephew of Nancy Pelosi. The right, born again Christians, etc. do not like Pelosi and Newsom and also consider both Pelosi and Newsome too liberal. So, I am confused by the political intonations in your comments. But again, with all due respect, I would like to point out that change never comes from criticism and condemnation, especially lasting change. If we want to change this system, we must practice blessing and loving our world and its myriad of imperfection. This is because perfection only comes from imperfection. Praise is more likely to obtain results than being critical. It is time we concentrate on the good in the world and make it better. I am not here to advocate for drugs or therapy, but I have finally learned that it does me absolutely no good to curse the years I did spend drugged and in therapy. It is better for me to concentrate on the good in my life and why I am really here on this earth. In my opinion, that is the only way any change can be made, even in psychiatry. When I was but a mere child, the mantra was “love is the answer.” Years later, it is still the answer. Thank you.
Report comment
Nancy Pelosi is a centrist Democrat. Newsom is a Neo-Liberal, which is a reactionary cooption of liberalism.
Change does often come from outside criticism and condemnation. It wakes people up, it can get some people to change sides. This is why slavery was ended. But at a minimum it wakes up the opposition. This is why a lot of Democrats were elected to the US House, including some true progressives, in 2018.
The good is that many people completely reject all facets of the mental health system, including Psychotherapy, Recovery, Motivationalism, and Salvation Seeking.
If you have been given psychiatric neurotoxins, then justice demands that you receive restitution. If as an adult you were voluntarily in psychotherapy, what I am calling for is that we prohibit our government from licensing psychotherapy. Such therapy will still go on, but the amount of harm it can do will be minimized.
Joshua
Report comment
Although I don’t necessarily agree with on some points, there is some sense to what you say. In regard to restitution to those who have been given psychiatric neurotoxins, I think many on this site probably think, “Don’t hold your breath.” As far as prohibiting government from licensing psychotherapy, it might have a similar outcome to Prohibition. However, now we do see a strong legal systm committed to preventing the harm of drunk driving. Yet, in my opinion, and others may share a similar opinion is that maybe trusting the government and its buddy, politics to solve the problem may actually cause more problems and trouble. As far as change coming from outside criticism and condemnation, there is change but it is usually only temporary and thus eventually the issue must be revisited again. In your post, you list “Psychotherapy, Recovery, Motivationalism, and Salvation Seeking. I know that many who have posted on this site claim that psychiatry as it is practiced is almost a cult or religion. Perhaps, this is so, but the jury on this one might still be out. However, in many opinions, there is a mixing of metaphors in the list you made. In that list and in my opinion and experience, it is only Psychotherapy that has presented some dangerous qualities. Although, like all things, that could depend on the individual. The other three things you list, that are, in my thinking, quite viable ways to deal with a world that many of us don’t always understand. Like all issues in life, some of this is very gray and even that which is black and white can be very nuanced at times. Although, I personally have been hurt by much of psychiatry, etc. I am still of the opinion, that any action to remedy the situation requires great forethought before taking any action. There are about as many variables as there are people in the world. That is why, I still believe that each one of us must tend to the growing of our own individual gardens first. I think there still remains that plank in the eye thing as mentioned in the Bible. Each one of us is endowed from our Creator to find what answers uniquely and personally work for us. In my opinion, things can only change when we are working to attempt to fulfill our agreements with our Creator. They begin from the ground up, which is in our individual lives and at the right time as appointed by the heavens– things will change accordingly. Thank you.
Report comment
Rebel, remember that a government issued license is at the core of all of this. That puts it all clearly within Nuremberg precedents for Crimes Against Humanity and War Crimes.
Restitution for those given psychiatric neurotoxins is within the same realm as restitution for the Japanese Americans placed into internment camps during WWII.
Prohibition was a law restricting the entire population. It was very unpopular and impossible to enforce.
But prohibiting our government from licensing psychotherapists would be very easy to enforce.
Professional Societies will still certify such therapists, as they do now. And there are at least two such orgs for Philosophical Counselors, and one for Tarot Card Readers, and for lots of other things I am sure. Once you lift the government license, the harm that any of these people can do is seriously truncated.
Well, using a motor vehicle on the public roads has always been interpreted as a privilege, and there has long been a licensing and insurance requirement. And the rules against drunken drivers are very moderate compared to the rules for private aviation. In my opinion drive to bars have to be considered a thing of the past.
The government is there to represent us, and where there are serious problems we need to make it work. The Anti-Government political position is nonsensical.
We were wrong to ever let the government authorize and license the mental health system. It would evaporate tomorrow without the government.
One of the things which keeps the mental health system going, in my opinion, is the fact that so many of its victims do not fight back. They do not respond to the mental health system as a lethal threat. Instead they seek pity and approval. I see all calls to cooperate and decline opposition and conflict as part of this, seeking pity and approval.
Psychotherapy, Recovery, Motivationalism, and Salvation Seeking all work on the premise that people need some sort of re-education because they suffer from some sort of innate moral defect. They deflect people from following their own inclinations. These doctrines are exploitative. I am not suggesting that they ever be prohibited, just that we should completely disregard them and prevent our government from ever supporting them.
We have been subjected to this stuff for at least 100 years now.
To make real change, when faced with power being wielded against you, you always have to focus first and foremost on the splinter in the eye of your neighbor. It was only when people learned this that slavery was ended.
Joshua
Report comment
I disagree with the remedies you seek. I shall no longer discuss this with you. Some of what you say may be correct, but at present, it is, probably, more injurious even to those who have been harmed by the mental health/illness system to speculate. In fact, it might bring up for such harmed things they would like to forget—and forgive. It is always better to light a candle in the darkness than burn the building down. Sometimes bringing harms from the past is more dangerous than anything else. I shall no longer discuss with you. People who have been harmed by this system need love and support above all else not a dredging up of the past in a fight that at least right now is likely to fail. I am at present putting my past behind me so that I may live very peacefully and happily for the rest of my time on Earth. One thing I have learned from my experiences is that each day is precious and despite it all, my life is precious. I don’t need a fight to rip that all apart. Thank you.
Report comment
People continue to be harmed by the mental health system, and all I want to do is to bring an end to it. I am not though will to place legal restrictions on consensual adult behavior, like who they can talk with.
We have channelers, psychic healers, and tarot readers, and we have all manner of preachers. I am not suggesting any restrictions on any of this, only on that kinds of licenses the government can issue. Most of the harm done by the mental health system would be impossible without such licensing.
Many people have made “mental illness” into their identity, rather like name placards on automobiles and the designer labels on clothes.
But what always underlies it is being dissociated from one’s own feelings, and this is what makes it harmful.
Facing harms of the past is always hard, but the way forward still always requires this.
Joshua
Report comment
Removed for moderation.
Report comment